Impact of Comorbidities and Glycemia at Admission and Dipeptidyl Peptidase 4 Inhibitors in Patients With Type 2 Diabetes With COVID-19: A Case Series From an Academic Hospital in Lombardy, Italy
et al., Diabetes Care, doi:10.2337/dc20-1340, Oct 2020
Metformin for COVID-19
3rd treatment shown to reduce risk in
July 2020, now with p < 0.00000000001 from 111 studies.
Lower risk for mortality, ventilation, ICU, hospitalization, progression, recovery, and viral clearance.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 90 hospitalized COVID-19 patients with diabetes in Italy, showing lower mortality with metformin use, without statistical significance.
Although the 45% lower mortality is not statistically significant, it is consistent with the significant 36% lower mortality [32‑40%] from meta-analysis of the 74 mortality results to date.
|
risk of death, 45.0% lower, HR 0.55, p = 0.10, treatment 25 of 69 (36.2%), control 13 of 21 (61.9%), NNT 3.9, adjusted per study, Cox proportional hazards.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Mirani et al., 6 Oct 2020, retrospective, Italy, peer-reviewed, median age 66.0, 8 authors, study period 20 February, 2020 - 9 April, 2020.
Contact: mirani@humanitas.it.
Impact of Comorbidities and Glycemia at Admission and Dipeptidyl Peptidase 4 Inhibitors in Patients With Type 2 Diabetes With COVID-19: A Case Series From an Academic Hospital in Lombardy, Italy
doi:10.2337/figshare.12980015.
Diabetes may unfavorably influence the outcome of coronavirus disease 19 , but the determinants of this effect are still poorly understood. In this monocentric study, we aimed at evaluating the impact of type 2 diabetes, comorbidities, plasma glucose levels, and antidiabetes medications on the survival of COVID-19 patients.
RESEARCH DESIGN AND METHODS This was a case series involving 387 COVID-19 patients admitted to a single center in the region of Lombardy, the epicenter of the severe acute respiratory syndrome coronavirus 2 pandemic in Italy, between 20 February and 9 April 2020. Medical history, pharmacological treatments, laboratory findings, and clinical outcomes of patients without diabetes and patients with type 2 diabetes were compared. Cox proportional hazards analysis was applied to investigate risk factors associated with mortality.
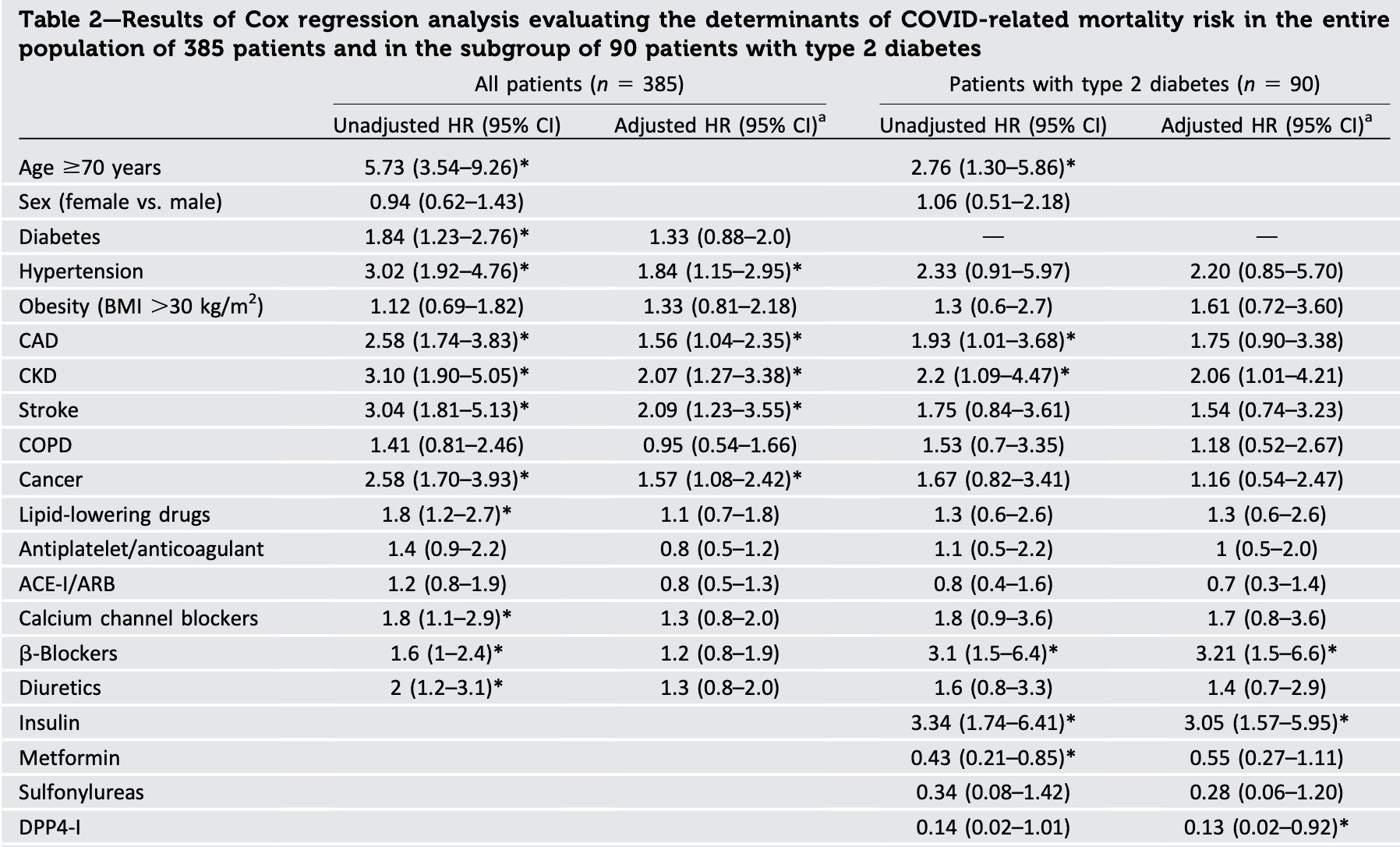
RESULTS Our samples included 90 patients (23.3%) with type 2 diabetes, who displayed double the mortality rate of subjects without diabetes (42.3% vs. 21.7%, P < 0.001). In spite of this, after correction for age and sex, risk of mortality was significantly associated with a history of hypertension (adjusted hazard ratio [aHR] 1.84, 95% CI 1.15-2.95; P 5 0.011), coronary artery disease (aHR 1.56, 95% CI 1.04-2.35; P 5 0.031), chronic kidney disease (aHR 2.07, 95% CI 1.27-3.38; P 5 0.003), stroke (aHR 2.09, 95% CI 1.23-3.55; P 5 0.006), and cancer (aHR 1.57, 95% CI 1.08-2.42; P 5 0.04) but not with type 2 diabetes (P 5 0.170). In patients with diabetes, elevated plasma glucose (aHR 1.22, 95% CI 1.04-1.44, per mmol/L; P 5 0.015) and IL-6 levels at admission (aHR 2.47, 95% CI 1.28-4.78, per 1-SD increase; P 5 0.007) as well as treatment with insulin (aHR 3.05, 95% CI 1.57-5.95; P 5 0.001) and b-blockers (aHR 3.20, 95% CI 1.50-6.60; P 5 0.001) were independently associated with increased mortality, whereas the use of dipeptidyl peptidase 4 inhibitors was significantly and independently associated with a lower risk of mortality (aHR 0.13, 95% CI 0.02-0.92; P 5 0.042).
CONCLUSIONS Plasma glucose levels at admission and antidiabetes drugs may influence the survival of COVID-19 patients affected by type 2 diabetes.
References
Aghemo, Piovani, Parigi, Humanitas COVID-19 Task Force. COVID-19 digestive system involvement and clinical outcomes in a large academic hospital in, Clin Gastroenterol Hepatol
Cecconi, Piovani, Brunetta, Early predictors of clinical deterioration in a cohort of 239 patients hospitalized for covid-19 infection in Lombardy, Italy, J Clin Med
Chen, Yang, Cheng, Clinical characteristics and outcomes of patients with diabetes and COVID-19 in association with glucoselowering medication, Diabetes Care
Chen, Zhou, Dong, Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study, Lancet
Chung, Bernheim, Mei, CT imaging features of 2019 novel coronavirus (2019-nCoV), Radiology
Ciardullo, Zerbini, Perra, Impact of diabetes on COVID-19-related in-hospital mortality: a retrospective study from Northern Italy, J Endocrinol Invest, doi:10.1007/s40618-020-01382-7
Coppelli, Giannarelli, Aragona, Hyperglycemia at hospital admission is associated with severity of the prognosis in patients hospitalized for COVID-19: the Pisa COVID-19 Study, Diabetes Care
Cummings, Baldwin, Abrams, Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: a prospective cohort study, Lancet
Dalan, Is DPP4 inhibition a comrade or adversary in COVID-19 infection, Diabetes Res Clin Pract
Daryabor, Atashzar, Kabelitz, Meri, Kalantar, The effects of type 2 diabetes mellitus on organ metabolism and the immune system, Front Immunol
Fox, Ruddiman, Lo, The relationship between diabetes and clinical outcomes in COVID-19: a single-center retrospective analysis, Acta Diabetol, doi:10.1007/s00592-020-01592-8
Grasselli, Pesenti, Cecconi, Critical care utilization for the COVID-19 outbreak in Lombardy, Italy: early experience and forecast during an emergency response, JAMA
Guo, Li, Dong, Diabetes is a risk factor for the progression and prognosis of COVID-19, Diabetes Metab Res Rev, doi:10.1002/dmrr.3319
Hodgson, Morris, Bridson, Govan, Rush et al., Immunological mechanisms contributing to the double burden of diabetes and intracellular bacterial infections, Immunology
Iaccarino, Grassi, Borghi, Ferri, Salvetti et al., Age and multimorbidity predict death among COVID-19 patients: results of the SARS-RAS study of the Italian Society of Hypertension, Hypertension
Iacobellis, COVID-19 and diabetes: can DPP4 inhibition play a role?, Diabetes Res Clin Pract
Joshi, Caputo, Weitekamp, Karchmer, Infections in patients with diabetes mellitus, N Engl J Med
Kondapally Seshasai, Kaptoge, Thompson, Emerging Risk Factors Collaboration. Diabetes mellitus, fasting glucose, and risk of cause-specific death, N Engl J Med
Kulcsar, Coleman, Beck, Frieman, Comorbid diabetes results in immune dysregulation and enhanced disease severity following MERS-CoV infection, JCI Insight
Lania, Sandri, Cellini, Mirani, Lavezzi et al., Thyrotoxicosis in patients with COVID-19: the THYRCOV study, Eur J Endocrinol
Ling, Cheng, Ge, The efficacy and safety of dipeptidyl peptidase-4 inhibitors for type 2 diabetes: a Bayesian network metaanalysis of 58 randomized controlled trials, Acta Diabetol
Lodigiani, Iapichino, Carenzo, Humanitas COVID-19 Task Force. Venous and arterial thromboembolic complications in COVID-19 patients admitted to an academic hospital in, Thromb Res
Muller, Gorter, Hak, Increased risk of common infections in patients with type 1 and type 2 diabetes mellitus, Clin Infect Dis
Palaiodimos, Kokkinidis, Li, Severe obesity, increasing age and male sex are independently associated with worse in-hospital outcomes, and higher in-hospital mortality, in a cohort of patients with COVID-19 in the Bronx, Metabolism
Richardson, Hirsch, Narasimhan, Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York City area [published correction appears, JAMA
Sardu, Onofrio, Balestrieri, Outcomes in patients with hyperglycemia affected by COVID-19: can we do more on glycemic control?, Diabetes Care
Shi, Zhang, Jiang, Clinical characteristics and risk factors for mortality of COVID-19 patients with diabetes in Wuhan, China: a two-center, retrospective study, Diabetes Care
Suleyman, Fadel, Malette, Clinical characteristics and morbidity associated with coronavirus disease 2019 in a series of patients in metropolitan Detroit, JAMA Netw Open
Trevelin, Carlos, Beretta, Da Silva, Cunha, Diabetes mellitus and sepsis: a challenging association, Shock
Vankadari, Wilce, Emerging WuHan (COVID-19) coronavirus: glycan shield and structure prediction of spike glycoprotein and its interaction with human CD26, Emerg Microbes Infect
Wu, Chen, Cai, Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China, JAMA Intern Med
Xu, Shi, Wang, Pathological findings of COVID-19 associated with acute respiratory distress syndrome, Lancet Respir Med
Yan, Yang, Wang, Clinical characteristics and outcomes of patients with severe covid-19 with diabetes, BMJ Open Diabetes Res Care
Yan, Zhang, Li, Xia, Guo et al., Structural basis for the recognition of SARS-CoV-2 by full-length human ACE2, Science
Yang, Feng, Yuan, Plasma glucose levels and diabetes are independent predictors for mortality and morbidity in patients with SARS, Diabet Med
Zarbock, Gomez, Kellum, Sepsisinduced acute kidney injury revisited: pathophysiology, prevention and future therapies, Curr Opin Crit Care
Zheng, Ley, Hu, Global aetiology and epidemiology of type 2 diabetes mellitus and its complications, Nat Rev Endocrinol
Zhu, She, Cheng, Association of blood glucose control and outcomes in patients with COVID-19 and pre-existing type 2 diabetes, Cell Metab
DOI record:
{
"DOI": "10.2337/dc20-1340",
"ISSN": [
"0149-5992",
"1935-5548"
],
"URL": "http://dx.doi.org/10.2337/dc20-1340",
"abstract": "<jats:sec>\n <jats:title>OBJECTIVE</jats:title>\n <jats:p>Diabetes may unfavorably influence the outcome of coronavirus disease 19 (COVID-19), but the determinants of this effect are still poorly understood. In this monocentric study, we aimed at evaluating the impact of type 2 diabetes, comorbidities, plasma glucose levels, and antidiabetes medications on the survival of COVID-19 patients.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>RESEARCH DESIGN AND METHODS</jats:title>\n <jats:p>This was a case series involving 387 COVID-19 patients admitted to a single center in the region of Lombardy, the epicenter of the severe acute respiratory syndrome coronavirus 2 pandemic in Italy, between 20 February and 9 April 2020. Medical history, pharmacological treatments, laboratory findings, and clinical outcomes of patients without diabetes and patients with type 2 diabetes were compared. Cox proportional hazards analysis was applied to investigate risk factors associated with mortality.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>RESULTS</jats:title>\n <jats:p>Our samples included 90 patients (23.3%) with type 2 diabetes, who displayed double the mortality rate of subjects without diabetes (42.3% vs. 21.7%, P &lt; 0.001). In spite of this, after correction for age and sex, risk of mortality was significantly associated with a history of hypertension (adjusted hazard ratio [aHR] 1.84, 95% CI 1.15–2.95; P = 0.011), coronary artery disease (aHR 1.56, 95% CI 1.04–2.35; P = 0.031), chronic kidney disease (aHR 2.07, 95% CI 1.27–3.38; P = 0.003), stroke (aHR 2.09, 95% CI 1.23–3.55; P = 0.006), and cancer (aHR 1.57, 95% CI 1.08–2.42; P = 0.04) but not with type 2 diabetes (P = 0.170). In patients with diabetes, elevated plasma glucose (aHR 1.22, 95% CI 1.04–1.44, per mmol/L; P = 0.015) and IL-6 levels at admission (aHR 2.47, 95% CI 1.28–4.78, per 1-SD increase; P = 0.007) as well as treatment with insulin (aHR 3.05, 95% CI 1.57–5.95; P = 0.001) and β-blockers (aHR 3.20, 95% CI 1.50–6.60; P = 0.001) were independently associated with increased mortality, whereas the use of dipeptidyl peptidase 4 inhibitors was significantly and independently associated with a lower risk of mortality (aHR 0.13, 95% CI 0.02–0.92; P = 0.042).</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>CONCLUSIONS</jats:title>\n <jats:p>Plasma glucose levels at admission and antidiabetes drugs may influence the survival of COVID-19 patients affected by type 2 diabetes.</jats:p>\n </jats:sec>",
"author": [
{
"affiliation": [
{
"name": "Endocrinology and Diabetology Unit, Humanitas Clinical and Research Center, IRCCS, Milan, Italy"
}
],
"family": "Mirani",
"given": "Marco",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-4187-5378",
"affiliation": [
{
"name": "Endocrinology and Diabetology Unit, Humanitas Clinical and Research Center, IRCCS, Milan, Italy"
}
],
"authenticated-orcid": false,
"family": "Favacchio",
"given": "Giuseppe",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Endocrinology and Diabetology Unit, Humanitas Clinical and Research Center, IRCCS, Milan, Italy"
}
],
"family": "Carrone",
"given": "Flaminia",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Endocrinology and Diabetology Unit, Humanitas Clinical and Research Center, IRCCS, Milan, Italy"
}
],
"family": "Betella",
"given": "Nazarena",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Endocrinology and Diabetology Unit, Humanitas Clinical and Research Center, IRCCS, Milan, Italy"
}
],
"family": "Biamonte",
"given": "Emilia",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Biostatistics Unit, Humanitas Clinical and Research Center, IRCCS, Milan, Italy"
}
],
"family": "Morenghi",
"given": "Emanuela",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Endocrinology and Diabetology Unit, Humanitas Clinical and Research Center, IRCCS, Milan, Italy"
},
{
"name": "Department of Biomedical Sciences, Humanitas University, Milan, Italy"
}
],
"family": "Mazziotti",
"given": "Gherardo",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Endocrinology and Diabetology Unit, Humanitas Clinical and Research Center, IRCCS, Milan, Italy"
},
{
"name": "Department of Biomedical Sciences, Humanitas University, Milan, Italy"
}
],
"family": "Lania",
"given": "Andrea Gerardo",
"sequence": "additional"
}
],
"container-title": "Diabetes Care",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"diabetesjournals.org"
]
},
"created": {
"date-parts": [
[
2020,
10,
7
]
],
"date-time": "2020-10-07T04:00:11Z",
"timestamp": 1602043211000
},
"deposited": {
"date-parts": [
[
2022,
3,
12
]
],
"date-time": "2022-03-12T22:37:56Z",
"timestamp": 1647124676000
},
"indexed": {
"date-parts": [
[
2023,
8,
30
]
],
"date-time": "2023-08-30T14:40:47Z",
"timestamp": 1693406447588
},
"is-referenced-by-count": 106,
"issue": "12",
"issued": {
"date-parts": [
[
2020,
10,
6
]
]
},
"journal-issue": {
"issue": "12",
"published-online": {
"date-parts": [
[
2020,
10,
6
]
]
},
"published-print": {
"date-parts": [
[
2020,
12,
1
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://www.diabetesjournals.org/content/license",
"content-version": "vor",
"delay-in-days": 45,
"start": {
"date-parts": [
[
2020,
11,
20
]
],
"date-time": "2020-11-20T00:00:00Z",
"timestamp": 1605830400000
}
}
],
"link": [
{
"URL": "https://diabetesjournals.org/care/article-pdf/43/12/3042/530950/dc201340.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "syndication"
},
{
"URL": "https://diabetesjournals.org/care/article-pdf/43/12/3042/530950/dc201340.pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1167",
"original-title": [],
"page": "3042-3049",
"prefix": "10.2337",
"published": {
"date-parts": [
[
2020,
10,
6
]
]
},
"published-online": {
"date-parts": [
[
2020,
10,
6
]
]
},
"published-print": {
"date-parts": [
[
2020,
12,
1
]
]
},
"publisher": "American Diabetes Association",
"reference": [
{
"DOI": "10.1016/S0140-6736(20)30211-7",
"article-title": "Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study",
"author": "Chen",
"doi-asserted-by": "crossref",
"first-page": "507",
"journal-title": "Lancet",
"key": "2022031220332739900_B1",
"volume": "395",
"year": "2020"
},
{
"key": "2022031220332739900_B2",
"unstructured": "World Health Organization\n . WHO Director-General's Opening Remarks at the Media Briefing on COVID-19 - 11 March 2020. Accessed 5 May 2020. Available from https://www.who.int/dg/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020."
},
{
"DOI": "10.1001/jama.2020.4031",
"article-title": "Critical care utilization for the COVID-19 outbreak in Lombardy, Italy: early experience and forecast during an emergency response",
"author": "Grasselli",
"doi-asserted-by": "crossref",
"first-page": "1545",
"journal-title": "JAMA",
"key": "2022031220332739900_B3",
"volume": "323",
"year": "2020"
},
{
"key": "2022031220332739900_B4",
"unstructured": "SARS-CoV-2 Surveillance Group\n . Characteristics of COVID-19 patients dying in Italy. Accessed 23 Jul 2020. Available from https://www.epicentro.iss.it/en/coronavirus/sars-cov-2-analysis-of-deaths"
},
{
"article-title": "Diabetes is a risk factor for the progression and prognosis of COVID-19",
"author": "Guo",
"journal-title": "Diabetes Metab Res Rev",
"key": "2022031220332739900_B5"
},
{
"DOI": "10.1136/bmjdrc-2020-001343",
"article-title": "Clinical characteristics and outcomes of patients with severe covid-19 with diabetes",
"author": "Yan",
"doi-asserted-by": "crossref",
"first-page": "e001343",
"journal-title": "BMJ Open Diabetes Res Care",
"key": "2022031220332739900_B6",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1111/j.1464-5491.2006.01861.x",
"article-title": "Plasma glucose levels and diabetes are independent predictors for mortality and morbidity in patients with SARS",
"author": "Yang",
"doi-asserted-by": "crossref",
"first-page": "623",
"journal-title": "Diabet Med",
"key": "2022031220332739900_B7",
"volume": "23",
"year": "2006"
},
{
"DOI": "10.1172/jci.insight.131774",
"article-title": "Comorbid diabetes results in immune dysregulation and enhanced disease severity following MERS-CoV infection",
"author": "Kulcsar",
"doi-asserted-by": "crossref",
"first-page": "e131774",
"journal-title": "JCI Insight",
"key": "2022031220332739900_B8",
"volume": "4",
"year": "2019"
},
{
"DOI": "10.1038/nrendo.2017.151",
"article-title": "Global aetiology and epidemiology of type 2 diabetes mellitus and its complications",
"author": "Zheng",
"doi-asserted-by": "crossref",
"first-page": "88",
"journal-title": "Nat Rev Endocrinol",
"key": "2022031220332739900_B9",
"volume": "14",
"year": "2018"
},
{
"DOI": "10.1086/431587",
"article-title": "Increased risk of common infections in patients with type 1 and type 2 diabetes mellitus",
"author": "Muller",
"doi-asserted-by": "crossref",
"first-page": "281",
"journal-title": "Clin Infect Dis",
"key": "2022031220332739900_B10",
"volume": "41",
"year": "2005"
},
{
"DOI": "10.1056/NEJM199912163412507",
"article-title": "Infections in patients with diabetes mellitus",
"author": "Joshi",
"doi-asserted-by": "crossref",
"first-page": "1906",
"journal-title": "N Engl J Med",
"key": "2022031220332739900_B11",
"volume": "341",
"year": "1999"
},
{
"DOI": "10.1111/imm.12394",
"article-title": "Immunological mechanisms contributing to the double burden of diabetes and intracellular bacterial infections",
"author": "Hodgson",
"doi-asserted-by": "crossref",
"first-page": "171",
"journal-title": "Immunology",
"key": "2022031220332739900_B12",
"volume": "144",
"year": "2015"
},
{
"DOI": "10.1056/NEJMoa1008862",
"article-title": "Diabetes mellitus, fasting glucose, and risk of cause-specific death",
"author": "Rao Kondapally Seshasai",
"doi-asserted-by": "crossref",
"first-page": "829",
"journal-title": "N Engl J Med",
"key": "2022031220332739900_B13",
"volume": "364",
"year": "2011"
},
{
"DOI": "10.2337/dc20-0598",
"article-title": "Clinical characteristics and risk factors for mortality of COVID-19 patients with diabetes in Wuhan, China: a two-center, retrospective study",
"author": "Shi",
"doi-asserted-by": "crossref",
"first-page": "1382",
"journal-title": "Diabetes Care",
"key": "2022031220332739900_B14",
"volume": "43",
"year": "2020"
},
{
"article-title": "Association of blood glucose control and outcomes in patients with COVID-19 and pre-existing type 2 diabetes",
"author": "Zhu",
"first-page": "1068",
"key": "2022031220332739900_B15",
"volume-title": "Cell Metab",
"year": "2020"
},
{
"DOI": "10.2337/dc20-0723",
"article-title": "Outcomes in patients with hyperglycemia affected by COVID-19: can we do more on glycemic control",
"author": "Sardu",
"doi-asserted-by": "crossref",
"first-page": "1408",
"journal-title": "Diabetes Care",
"key": "2022031220332739900_B16",
"volume": "43",
"year": "2020"
},
{
"DOI": "10.2337/dc20-0660",
"article-title": "Clinical characteristics and outcomes of patients with diabetes and COVID-19 in association with glucose-lowering medication",
"author": "Chen",
"doi-asserted-by": "crossref",
"first-page": "1399",
"journal-title": "Diabetes Care",
"key": "2022031220332739900_B17",
"volume": "43",
"year": "2020"
},
{
"DOI": "10.1016/j.metabol.2020.154262",
"article-title": "Severe obesity, increasing age and male sex are independently associated with worse in-hospital outcomes, and higher in-hospital mortality, in a cohort of patients with COVID-19 in the Bronx, New York",
"author": "Palaiodimos",
"doi-asserted-by": "crossref",
"first-page": "154262",
"journal-title": "Metabolism",
"key": "2022031220332739900_B18",
"volume": "108",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)31189-2",
"article-title": "Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: a prospective cohort study",
"author": "Cummings",
"doi-asserted-by": "crossref",
"first-page": "1763",
"journal-title": "Lancet",
"key": "2022031220332739900_B19",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/j.thromres.2020.04.024",
"article-title": "Venous and arterial thromboembolic complications in COVID-19 patients admitted to an academic hospital in Milan, Italy",
"author": "Lodigiani",
"doi-asserted-by": "crossref",
"first-page": "9",
"journal-title": "Thromb Res",
"key": "2022031220332739900_B20",
"volume": "191",
"year": "2020"
},
{
"DOI": "10.3390/jcm9051548",
"article-title": "Early predictors of clinical deterioration in a cohort of 239 patients hospitalized for covid-19 infection in Lombardy, Italy",
"author": "Cecconi",
"doi-asserted-by": "crossref",
"first-page": "1548",
"journal-title": "J Clin Med",
"key": "2022031220332739900_B21",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1530/EJE-20-0335",
"article-title": "Thyrotoxicosis in patients with COVID-19: the THYRCOV study",
"author": "Lania",
"doi-asserted-by": "crossref",
"first-page": "381",
"journal-title": "Eur J Endocrinol",
"key": "2022031220332739900_B22",
"volume": "183",
"year": "2020"
},
{
"DOI": "10.1016/j.cgh.2020.05.011",
"article-title": "COVID-19 digestive system involvement and clinical outcomes in a large academic hospital in Milan, Italy",
"author": "Aghemo",
"doi-asserted-by": "crossref",
"first-page": "2366",
"journal-title": "Clin Gastroenterol Hepatol",
"key": "2022031220332739900_B23",
"volume": "18",
"year": "2020"
},
{
"DOI": "10.1148/radiol.2020200230",
"article-title": "CT imaging features of 2019 novel coronavirus (2019-nCoV)",
"author": "Chung",
"doi-asserted-by": "crossref",
"first-page": "202",
"journal-title": "Radiology",
"key": "2022031220332739900_B24",
"volume": "295",
"year": "2020"
},
{
"article-title": "Vademecum for the treatment of people with COVID-19. Edition 2.0, 13 March 2020",
"author": "Lombardy Section Italian Society Infectious And Tropical Diseases",
"first-page": "143",
"key": "2022031220332739900_B25",
"volume-title": "Infez Med",
"year": "2020"
},
{
"DOI": "10.1007/s00592-018-1222-z",
"article-title": "The efficacy and safety of dipeptidyl peptidase-4 inhibitors for type 2 diabetes: a Bayesian network meta-analysis of 58 randomized controlled trials",
"author": "Ling",
"doi-asserted-by": "crossref",
"first-page": "249",
"journal-title": "Acta Diabetol",
"key": "2022031220332739900_B26",
"volume": "56",
"year": "2019"
},
{
"article-title": "Impact of diabetes on COVID-19-related in-hospital mortality: a retrospective study from Northern Italy",
"author": "Ciardullo",
"journal-title": "J Endocrinol Invest",
"key": "2022031220332739900_B27"
},
{
"DOI": "10.1161/HYPERTENSIONAHA.120.15324",
"article-title": "Age and multimorbidity predict death among COVID-19 patients: results of the SARS-RAS study of the Italian Society of Hypertension",
"author": "Iaccarino",
"doi-asserted-by": "crossref",
"first-page": "366",
"journal-title": "Hypertension",
"key": "2022031220332739900_B28",
"volume": "76",
"year": "2020"
},
{
"DOI": "10.1001/jamanetworkopen.2020.12270",
"article-title": "Clinical characteristics and morbidity associated with coronavirus disease 2019 in a series of patients in metropolitan Detroit",
"author": "Suleyman",
"doi-asserted-by": "crossref",
"first-page": "e2012270",
"journal-title": "JAMA Netw Open",
"key": "2022031220332739900_B29",
"volume": "3",
"year": "2020"
},
{
"article-title": "Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York City area [published correction appears in JAMA 2020;323:2098]",
"author": "Richardson",
"first-page": "2052",
"key": "2022031220332739900_B30",
"volume-title": "JAMA",
"year": "2020"
},
{
"article-title": "The relationship between diabetes and clinical outcomes in COVID-19: a single-center retrospective analysis",
"author": "Fox",
"journal-title": "Acta Diabetol",
"key": "2022031220332739900_B31"
},
{
"DOI": "10.2337/dc20-1380",
"article-title": "Hyperglycemia at hospital admission is associated with severity of the prognosis in patients hospitalized for COVID-19: the Pisa COVID-19 Study",
"author": "Coppelli",
"doi-asserted-by": "crossref",
"first-page": "2345",
"journal-title": "Diabetes Care",
"key": "2022031220332739900_B32",
"volume": "43",
"year": "2020"
},
{
"DOI": "10.1097/SHK.0000000000000778",
"article-title": "Diabetes mellitus and sepsis: a challenging association",
"author": "Trevelin",
"doi-asserted-by": "crossref",
"first-page": "276",
"journal-title": "Shock",
"key": "2022031220332739900_B33",
"volume": "47",
"year": "2017"
},
{
"DOI": "10.1097/MCC.0000000000000153",
"article-title": "Sepsis-induced acute kidney injury revisited: pathophysiology, prevention and future therapies",
"author": "Zarbock",
"doi-asserted-by": "crossref",
"first-page": "588",
"journal-title": "Curr Opin Crit Care",
"key": "2022031220332739900_B34",
"volume": "20",
"year": "2014"
},
{
"DOI": "10.3389/fimmu.2020.01582",
"article-title": "The effects of type 2 diabetes mellitus on organ metabolism and the immune system",
"author": "Daryabor",
"doi-asserted-by": "crossref",
"first-page": "1582",
"journal-title": "Front Immunol",
"key": "2022031220332739900_B35",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1001/jamainternmed.2020.0994",
"article-title": "Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China",
"author": "Wu",
"doi-asserted-by": "crossref",
"first-page": "934",
"journal-title": "JAMA Intern Med",
"key": "2022031220332739900_B36",
"volume": "180",
"year": "2020"
},
{
"DOI": "10.1016/S2213-2600(20)30076-X",
"article-title": "Pathological findings of COVID-19 associated with acute respiratory distress syndrome",
"author": "Xu",
"doi-asserted-by": "crossref",
"first-page": "420",
"journal-title": "Lancet Respir Med",
"key": "2022031220332739900_B37",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.2337/dc20-S009",
"article-title": "9. Pharmacologic approaches to glycemic treatment: Standards of Medical Care in Diabetes—2020",
"author": "American Diabetes Association",
"doi-asserted-by": "crossref",
"first-page": "S98",
"journal-title": "Diabetes Care",
"key": "2022031220332739900_B38",
"volume": "43",
"year": "2020"
},
{
"DOI": "10.1080/22221751.2020.1739565",
"article-title": "Emerging WuHan (COVID-19) coronavirus: glycan shield and structure prediction of spike glycoprotein and its interaction with human CD26",
"author": "Vankadari",
"doi-asserted-by": "crossref",
"first-page": "601",
"journal-title": "Emerg Microbes Infect",
"key": "2022031220332739900_B39",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1126/science.abb2762",
"article-title": "Structural basis for the recognition of SARS-CoV-2 by full-length human ACE2",
"author": "Yan",
"doi-asserted-by": "crossref",
"first-page": "1444",
"journal-title": "Science",
"key": "2022031220332739900_B40",
"volume": "367",
"year": "2020"
},
{
"DOI": "10.1016/j.diabres.2020.108125",
"article-title": "COVID-19 and diabetes: can DPP4 inhibition play a role",
"author": "Iacobellis",
"doi-asserted-by": "crossref",
"first-page": "108125",
"journal-title": "Diabetes Res Clin Pract",
"key": "2022031220332739900_B41",
"volume": "162",
"year": "2020"
},
{
"DOI": "10.1016/j.diabres.2020.108216",
"article-title": "Is DPP4 inhibition a comrade or adversary in COVID-19 infection",
"author": "Dalan",
"doi-asserted-by": "crossref",
"first-page": "108216",
"journal-title": "Diabetes Res Clin Pract",
"key": "2022031220332739900_B42",
"volume": "164",
"year": "2020"
}
],
"reference-count": 42,
"references-count": 42,
"relation": {},
"resource": {
"primary": {
"URL": "https://diabetesjournals.org/care/article/43/12/3042/30894/Impact-of-Comorbidities-and-Glycemia-at-Admission"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Advanced and Specialized Nursing",
"Endocrinology, Diabetes and Metabolism",
"Internal Medicine"
],
"subtitle": [],
"title": "Impact of Comorbidities and Glycemia at Admission and Dipeptidyl Peptidase 4 Inhibitors in Patients With Type 2 Diabetes With COVID-19: A Case Series From an Academic Hospital in Lombardy, Italy",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.2337/ada-journal-policies",
"volume": "43"
}
