Association between vitamin D hypovitaminosis and severe forms of COVID-19
et al., European Review for Medical and Pharmacological Sciences, doi:10.26355/eurrev_202306_32651, Jun 2023
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
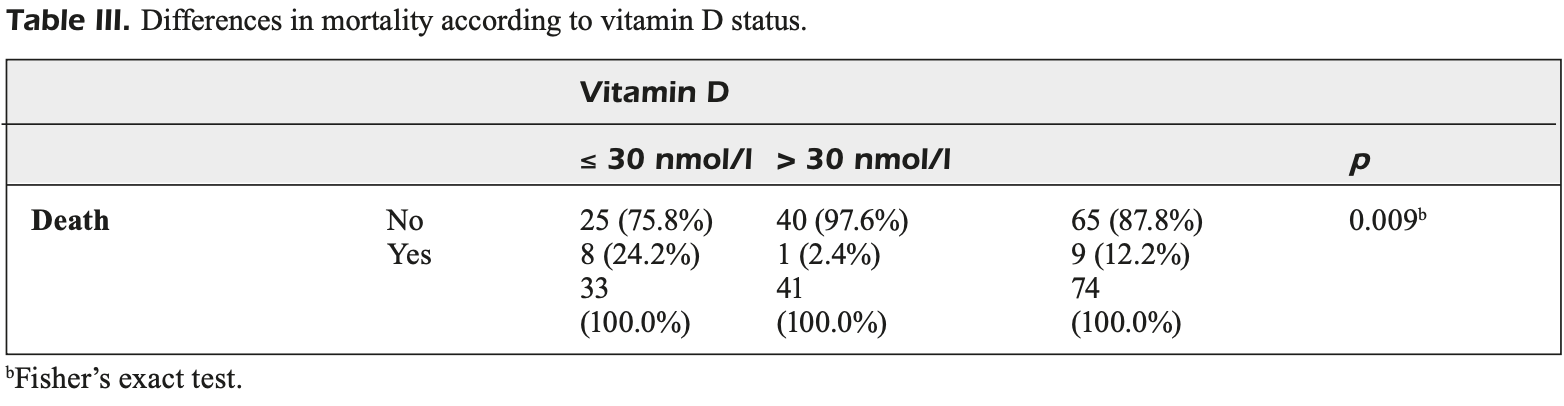
Retrospective 74 COVID-19 patients in Serbia, showing higher mortality with severe vitamin D deficiency in unadjusted results. Patients with severe deficiency were older (63.7 vs. 52.8).
This is the 182nd of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
This study is excluded in the after exclusion results of meta-analysis:
unadjusted differences between groups.
|
risk of death, 89.9% lower, RR 0.10, p = 0.009, high D levels (≥30nmol/l) 1 of 41 (2.4%), low D levels (<30nmol/l) 8 of 33 (24.2%), NNT 4.6.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Manojlovic et al., 15 Jun 2023, retrospective, Serbia, peer-reviewed, mean age 57.6, 11 authors.
Contact: mia.manojlovic@mf.uns.ac.rs.
OBJECTIVE: Hypovitaminosis D may be associated with an increased susceptibility to infection, more severe COVID-19 forms, and a higher risk of death. The objective of this study was to investigate any possible connections between vitamin D status [as measured by serum 25-hydroxyvitamin D (25(OH)D) levels] and COVID-19 severity. PATIENTS AND METHODS: In 2021, a cross-sectional study of consecutive adult COVID-19 patients was conducted. Anthropometric data, comorbidities, hospital setting, length of stay, respiratory support, outcome data, and vitamin D status were all evaluated. RESULTS: The length of hospitalization among participants (n = 74; mean age 57.64 ± 17.83 years, 55.4% male) was 18.58 ± 10 days, the majority of the hospital setting was a medical ward (67.6%), and the respiratory support in the form of mechanical ventilation was represented by 12.2%. Hypertension (54.1%), obesity (64.9%), and overweight (64.9%) were the most common cardiometabolic risk factors. In the study group, 44.6% of participants had severe vitamin D deficiency (< 30 nmol/l), while 8.1% had vitamin D insufficiency (50 -74.9 nmol/l). Furthermore, patients with severe COVID-19 (semi-intensive care unit, intensive care unit) had significantly lower serum 25(OH)D levels (32.9 vs. 20.5 nmol/l; p = 0.007). Participants with severe vitamin D deficiency were older and had more prevalent hypertension, requiring mechanical ventilation; 24.2% experienced a fatal outcome. CONCLUSIONS: Severe vitamin D deficiency may contribute significantly to the influence of other cardiometabolic risk factors in COVID-19.
Conflict of Interest The Authors declare that they have no conflict of interests.
Ethics Approval The study was conducted following the Helsinki Declaration and was approved by the Ethics Committees of the Clinical Center of Vojvodina, Novi Sad, Serbia (approval number: 00-153) and the Faculty of Medicine Novi Sad, Novi Sad, Serbia (approval number: 01-39/94/1).
Informed Consent All subjects provided informed consent.
Authors' Contributions Mia Manojlovic contributed significantly to study conception and design, data acquisition, data interpretation, and manuscript writing; Branislava Ilincic contributed significantly to study conception and design and manuscript writ-
References
Ali, Role of vitamin D in preventing of COVID-19 infection, progression and severity, J Infect Public Health
Amrein, Scherkl, Hoffmann, Neuwersch-Sommeregger, Köstenberger et al., Vitamin D deficiency 2.0: an update on the current status worldwide, Eur J Clin Nutr
Angelidi, Belanger, Lorinsky, Karamanis, Chamorro-Pareja et al., Vitamin D Status Is Associated With In-Hospital Mortality and Mechanical Ventilation: A Cohort of COVID-19 Hospitalized Patients, Mayo Clin Proc
Annweiler, Beaudenon, Gautier, Simon, Dubée et al., CO-VIT-TRIAL study group. COvid-19 and highdose VITamin D supplementation TRIAL in high-risk older patients (COVIT-TRIAL): study protocol for a randomized controlled trial, Trials
Baktash, Hosack, Patel, Shah, Kandiah et al., Vitamin D status and outcomes for hospitalized older patients with COVID-19, Postgrad Med J
Bassatne, Basbous, Chakhtoura, El Zein, Rahme et al., The link between COVID-19 and VItamin D (VIVID): A systematic review and meta-analysis, Metabolism
Castillo, Costa, Barrios, Díaz, Miranda et al., Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study, J Steroid Biochem Mol Biol
Driggin, Madhavan, Gupta, The role of vitamin D in cardiovascular disease and COVID-19, Rev Endocr Metab Disord
Hetta, Muhammad, El-Masry, Taha, Ahmed et al., The interplay between vitamin D and COVID-19: protective or bystander?, Eur Rev Med Pharmacol Sci
Ilie, Stefanescu, Smith, The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality, Aging Clin Exp Res
Ilinčić, Stokić, Stošić, Kojić, Katsiki et al., Vitamin D status and circulating biomarkers of endothelial dysfunction and inflammation in non-diabetic obese individuals: a pilot study, Arch Med Sci
Kotur, Skakic, Klaassen, Gasic, Zukic et al., Association of Vitamin D, Zinc and Selenium Related Genetic Variants With COVID-19 Disease Severity, Front Nutr
Kumar, Rathi, Haq, Wimalawansa, Sharma, Putative roles of vitamin D in modulating immune response and immunopathology associated with COVID-19, Virus Res
Latic, Erben, Vitamin, Disease, with Emphasis on Hypertension, Atherosclerosis, and Heart Failure, Int J Mol Sci
Libby, Lüscher, COVID-19 is, in the end, an endothelial disease, Eur Heart J
Mitchell, Vitamin-D and COVID-19: do deficient risk a poorer outcome?, Lancet Diabetes Endocrinol
Munshi, Hussein, Toraih, Elshazli, Jardak et al., Vitamin D insufficiency as a potential culprit in critical COVID-19 patients, J Med Virol
Ng, Tipih, Makoah, Vermeulen, Goedhals et al., Mahalingam S. Comorbidities in SARS-CoV-2 Patients: a Systematic Review and Meta-Analysis, mBio
Nimer, Khabour, Swedan, Kofahi, The impact of vitamin and mineral supplements usage prior to COVID-19 infection on disease severity and hospitalization, Bosn J of Basic Med Sci
Perna, The enigma of vitamin D supplementation in aging with obesity, Minerva Gastroenterol (Torino)
Pesaresi, Pirani, Tagliabracci, Valsecchi, Procopio et al., SARS-CoV-2 identification in lungs, heart and kidney specimens by transmission and scanning electron microscopy, Eur Rev Med Pharmacol Sci
Petrilli, Jones, Yang, Rajagopalan, Donnell et al., Factors associated with hospital admission and critical illness among 5279 people with coronavirus disease, BMJ
Radujkovic, Hippchen, Tiwari-Heckler, Dreher, Boxberger, Vitamin D Deficiency and Outcome of COVID-19 Patients, Nutrients
Thacher, Evaluating the Evidence in Clinical Studies of Vitamin D in COVID-19, Nutrients
Who, Coronavirus disease (COVID-19)
Zhou, Yu, Du, Fan, Liu et al., Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study, Lancet
DOI record:
{
"DOI": "10.26355/eurrev_202306_32651",
"ISSN": "1128-3602, 2284-0729",
"URL": "https://doi.org/10.26355/eurrev_202306_32651",
"abstract": "OBJECTIVE: Hypovitaminosis D may be associated with an increased susceptibility to infection, more severe COVID-19 forms, and a higher risk of death. The objective of this study was to investigate any possible connections between vitamin D status [as measured by serum 25-hydroxyvitamin D (25(OH)D) levels] and COVID-19 severity. PATIENTS AND METHODS: In 2021, a cross-sectional study of consecutive adult COVID-19 patients was conducted. Anthropometric data, comorbidities, hospital setting, length of stay, respiratory support, outcome data, and vitamin D status were all evaluated. RESULTS: The length of hospitalization among participants (n = 74; mean age 57.64 ± 17.83 years, 55.4% male) was 18.58 ± 10 days, the majority of the hospital setting was a medical ward (67.6%), and the respiratory support in the form of mechanical ventilation was represented by 12.2%. Hypertension (54.1%), obesity (64.9%), and overweight (64.9%) were the most common cardiometabolic risk factors. In the study group, 44.6% of participants had severe vitamin D deficiency (< 30 nmol/l), while 8.1% had vitamin D insufficiency (50 - 74.9 nmol/l). Furthermore, patients with severe COVID-19 (semi-intensive care unit, intensive care unit) had significantly lower serum 25(OH)D levels (32.9 vs. 20.5 nmol/l; p = 0.007). Participants with severe vitamin D deficiency were older and had more prevalent hypertension, requiring mechanical ventilation; 24.2% experienced a fatal outcome. CONCLUSIONS: Severe vitamin D deficiency may contribute significantly to the influence of other cardiometabolic risk factors in COVID-19.",
"author": [
{
"family": "Manojlovic",
"given": "M."
},
{
"family": "Ilincic",
"given": "B."
},
{
"family": "Naglic",
"given": "D.T."
},
{
"family": "Cabarkapa",
"given": "V."
},
{
"family": "Bajkin",
"given": "I."
},
{
"family": "Djuric",
"given": "A.P."
},
{
"family": "Kolarski",
"given": "I."
},
{
"family": "Bojovic",
"given": "M."
},
{
"family": "Urosevic",
"given": "I."
},
{
"family": "Stokic",
"given": "E."
},
{
"family": "Isenovic",
"given": "E.R."
}
],
"container-title": "European Review for Medical and Pharmacological Sciences",
"issue": "11",
"issued": {
"date-parts": [
[
2023,
6
]
]
},
"language": "eng",
"medium": "JB",
"page": "5318-5326",
"page-first": "5318",
"publisher": "Verduci Editore s.r.l.",
"publisher-place": "IT",
"title": "Association between vitamin D hypovitaminosis and severe forms of COVID-19",
"type": "article-journal",
"volume": "27"
}
