Coronavirus in HIP Fractures CHIP 2: Is Vitamin D Deficiency Associated with Increased Mortality from COVID-19 Infections in A Hip Fracture Population?
et al., European Journal of Medical and Health Sciences, doi:10.24018/ejmed.2021.3.6.1159, Dec 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 517 hip fracture patients in the UK with vitamin D levels measured during COVID-19 admission, not showing significant differences in mortality for supplementation in unadjusted analysis with no group details and subject to confounding by indication. There was also no significant effect based on deficiency.
This is the 63rd of 137 COVID-19 controlled studies for vitamin D, which collectively show efficacy with p<0.0000000001.
41 studies are RCTs, which show efficacy with p=0.00000049.
Standard of Care (SOC) for COVID-19 in the study country,
the United Kingdom, is very poor with very low average efficacy for approved treatments1.
The United Kingdom focused on expensive high-profit treatments, approving only one low-cost early treatment, which required a prescription and had limited adoption. The high-cost prescription treatment strategy reduces the probability of early treatment due to access and cost barriers, and eliminates complementary and synergistic benefits seen with many low-cost treatments.
This may explain in part the very high mortality seen in this study.
Results may differ in countries with improved SOC.
This study is excluded in the after exclusion results of meta-analysis:
unadjusted results with no group details; substantial unadjusted confounding by indication likely.
|
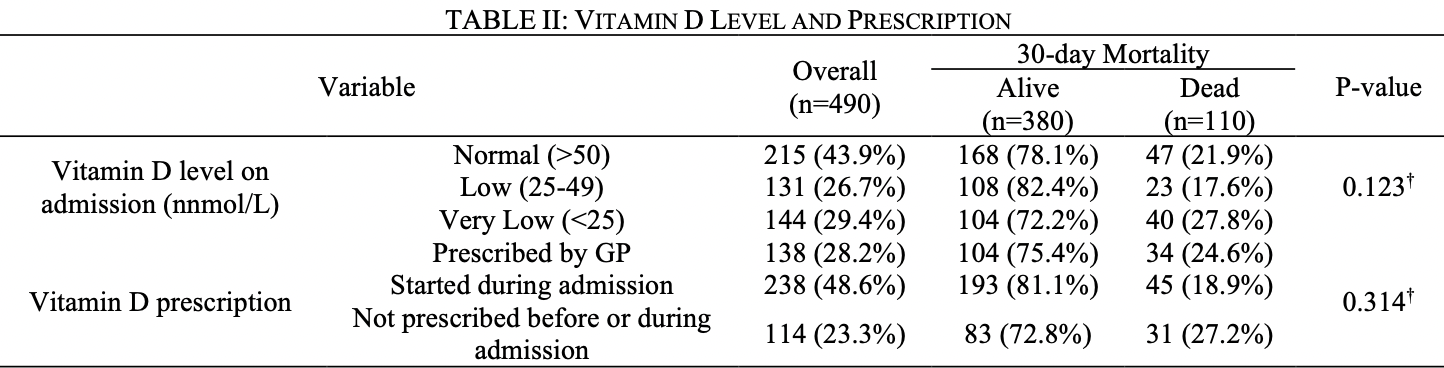
risk of death, 9.4% lower, RR 0.91, p = 0.67, treatment 34 of 138 (24.6%), control 31 of 114 (27.2%), NNT 39, prescribed by GP.
|
|
risk of death, 30.5% lower, RR 0.70, p = 0.10, treatment 45 of 238 (18.9%), control 31 of 114 (27.2%), NNT 12, started after admission, late treatment result.
|
|
risk of death, 12.5% lower, RR 0.87, p = 0.51, high D levels (≥25nmol/L) 70 of 346 (20.2%), low D levels (<25nmol/L) 40 of 144 (27.8%), adjusted per study, inverted to make RR<1 favor high D levels (≥25nmol/L), odds ratio converted to relative risk, outcome based on serum levels.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Mahmood et al., 29 Dec 2021, retrospective, United Kingdom, peer-reviewed, 4 authors, study period 23 March, 2020 - 31 December, 2020, dosage varies.
Coronavirus in HIP Fractures CHIP 2: Is Vitamin D Deficiency Associated with Increased Mortality from COVID-19 Infections in A Hip Fracture Population?
European Journal of Medical and Health Sciences, doi:10.24018/ejmed.2021.3.6.1159
Purpose: There is controversy as to whether vitamin D deficiency is associated with increased mortality from coronavirus infection. The aim of the study was to assess the relationship between vitamin D levels and 30day mortality in hip fracture patients co-infected with COVID-19.
Methods : This was a national observational audit conducted between 23 March 2020 (start of UK lockdown) and 31 st December 2020. The cohort consisted of patients aged >60 years presenting with a hip fracture. Patients were included if they had a vitamin D level done during the admission episode, diagnosis of COVID-19 infection via a viral reverse transcriptase PCR swab, and a hip fracture. There were 517 patients included in the study from 43 different hospital trusts. The primary outcome measure was 30-day mortality. Secondary outcomes were the percentage of patients who had vitamin D deficiency, the percentage of patients who were prescribed Vitamin D, and the impact of vitamin D prescribing on mortality Results: Vitamin D deficiency was not associated with a higher 30-day mortality. Low serum vitamin D was observed in 56% of the patients on admission. Vitamin D was prescribed prior to admission in 28% and during admission in a further 49%. Pre-hospital vitamin D therapy reduced the chance of vitamin D deficiency. Starting vitamin D before or on admission did not affect the mortality rates. Conclusion: Vitamin D deficiency was common, but not associated with a higher 30-day mortality in the hip fracture population co-infected with COVID-19.
CONFLICT OF INTEREST All named authors hereby declare that they have no conflicts of interest to disclose.
References
Baktash, Hosack, Patel, Shah, Kandiah et al., Vitamin D status and outcomes for hospitalised older patients with COVID-19, Postgrad Med J
Beresford, Sexton, Nebhani, Liverpool University Foundation Trust
Boban, Novel coronavirus disease (COVID-19) update on epidemiology, pathogenicity, clinical course and treatments, Int J Clin Pract
Castillo, Costa, Barrios, Díaz, Miranda et al., Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study, J Steroid Biochem Mol Biol
Craveiro, Cabral, Araújo, Falcão, Guimarães et al., Association of Serum 25-Hydroxyvitamin D Concentration with Pulmonary Function in Young Adults, Nutrients
Ginde, Mansbach, Camargo, Association between serum 25-hydroxyvitamin D level and upper respiratory tract infection in the Third National Health and Nutrition Examination Survey, Arch Intern Med
Grant, Lahore, Mcdonnell, Baggerly, French et al., Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths, Nutrients
Hastie, Pell, Sattar, Vitamin D and COVID-19 infection and mortality in UK Biobank, Eur J Nutr
Ilie, Stefanescu, Smith, The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality, Aging Clin Exp Res
Kaufman, Niles, Kroll, Bi, Holick, SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels, PLoS One
Laird, Rhodes, Kenny, Vitamin D and Inflammation: Potential Implications for Severity of Covid-19, Ir Med J
Liu, Sun, Wang, Zhang, Zhao et al., Low vitamin D status is associated with coronavirus disease 2019 outcomes: a systematic review and meta-analysis, Int J Infect Dis
Mahmood, Rashid, Limb, Cash, Nagy et al., Coronavirus infection in hip fractures (CHIP) study, Bone Joint J
Martineau, Jolliffe, Hooper, Greenberg, Aloia et al., Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data, BMJ
Marufu, White, Griffiths, Moonesinghe, Moppett, Prediction of 30-day mortality after hip fracture surgery by the Nottingham Hip Fracture Score and the Surgical Outcome Risk Tool, Anaesthesia
Mccartney, Byrne, Optimisation of Vitamin D Status for Enhanced Immuno-protection Against Covid-19, Ir Med J
Meltzer, Best, Zhang, Vokes, Arora et al., Association of Vitamin D Status and Other Clinical Characteristics With COVID-19 Test Results, JAMA Netw Open
Mitchell, Vitamin-D and COVID-19: do deficient risk a poorer outcome?, Lancet Diabetes Endocrinol
Murai, Fernandes, Sales, Pinto, Goessler et al., Effect of a Single High Dose of Vitamin D3 on Hospital Length of Stay in Patients with Moderate to Severe COVID-19: A Randomized Clinical Trial, JAMA
Panagiotou, Tee, Ihsan, Athar, Marchitelli et al., Low serum 25-hydroxyvitamin D (25[OH]D) levels in patients hospitalized with COVID-19 are associated with greater disease severity, Clin Endocrinol (Oxf)
Pizzini, Aichner, Sahanic, Böhm, Egger et al., Impact of Vitamin D Deficiency on COVID-19-A Prospective Analysis from the CovILD Registry, Nutrients
DOI record:
{
"DOI": "10.24018/ejmed.2021.3.6.1159",
"ISSN": [
"2593-8339"
],
"URL": "http://dx.doi.org/10.24018/ejmed.2021.3.6.1159",
"abstract": "<jats:p>Purpose: There is controversy as to whether vitamin D deficiency is associated with increased mortality from coronavirus infection. The aim of the study was to assess the relationship between vitamin D levels and 30-day mortality in hip fracture patients co-infected with COVID-19.\nMethods: This was a national observational audit conducted between 23 March 2020 (start of UK lockdown) and 31st December 2020. The cohort consisted of patients aged >60 years presenting with a hip fracture. Patients were included if they had a vitamin D level done during the admission episode, diagnosis of COVID-19 infection via a viral reverse transcriptase PCR swab, and a hip fracture. There were 517 patients included in the study from 43 different hospital trusts. The primary outcome measure was 30-day mortality. Secondary outcomes were the percentage of patients who had vitamin D deficiency, the percentage of patients who were prescribed Vitamin D, and the impact of vitamin D prescribing on mortality\nResults: Vitamin D deficiency was not associated with a higher 30-day mortality. Low serum vitamin D was observed in 56% of the patients on admission. Vitamin D was prescribed prior to admission in 28% and during admission in a further 49%. Pre-hospital vitamin D therapy reduced the chance of vitamin D deficiency. Starting vitamin D before or on admission did not affect the mortality rates.\nConclusion: Vitamin D deficiency was common, but not associated with a higher 30-day mortality in the hip fracture population co-infected with COVID-19.</jats:p>",
"author": [
{
"affiliation": [],
"family": "Mahmood",
"given": "A.",
"sequence": "first"
},
{
"affiliation": [],
"family": "Rashid",
"given": "F.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Hawkes",
"given": "D.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Harrison",
"given": "W. J.",
"sequence": "additional"
}
],
"container-title": [
"European Journal of Medical and Health Sciences"
],
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2022,
1,
6
]
],
"date-time": "2022-01-06T13:59:27Z",
"timestamp": 1641477567000
},
"deposited": {
"date-parts": [
[
2022,
1,
6
]
],
"date-time": "2022-01-06T13:59:47Z",
"timestamp": 1641477587000
},
"indexed": {
"date-parts": [
[
2022,
1,
21
]
],
"date-time": "2022-01-21T07:29:51Z",
"timestamp": 1642750191579
},
"is-referenced-by-count": 1,
"issn-type": [
{
"type": "electronic",
"value": "2593-8339"
}
],
"issue": "6",
"issued": {
"date-parts": [
[
2021,
12,
29
]
]
},
"journal-issue": {
"issue": "6",
"published-online": {
"date-parts": [
[
2021,
11,
1
]
]
}
},
"license": [
{
"URL": "http://creativecommons.org/licenses/by/4.0",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
12,
29
]
],
"date-time": "2021-12-29T00:00:00Z",
"timestamp": 1640736000000
}
}
],
"link": [
{
"URL": "https://www.ej-med.org/index.php/ejmed/article/download/1159/699",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://www.ej-med.org/index.php/ejmed/article/download/1159/699",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "10105",
"original-title": [],
"page": "111-116",
"prefix": "10.24018",
"published": {
"date-parts": [
[
2021,
12,
29
]
]
},
"published-online": {
"date-parts": [
[
2021,
12,
29
]
]
},
"publisher": "European Open Science Publishing",
"reference-count": 24,
"references-count": 24,
"relation": {},
"score": 1,
"short-container-title": [
"EJMED"
],
"short-title": [],
"source": "Crossref",
"subtitle": [],
"title": [
"Coronavirus in HIP Fractures CHIP 2: Is Vitamin D Deficiency Associated with Increased Mortality from COVID-19 Infections in A Hip Fracture Population?"
],
"type": "journal-article",
"volume": "3"
}
