Prescription of glucose-lowering therapies and risk of COVID-19 mortality in people with type 2 diabetes: a nationwide observational study in England
et al., The Lancet Diabetes & Endocrinology, doi:10.1016/S2213-8587(21)00050-4, Mar 2021
Metformin for COVID-19
3rd treatment shown to reduce risk in
July 2020, now with p < 0.00000000001 from 111 studies.
Lower risk for mortality, ventilation, ICU, hospitalization, progression, recovery, and viral clearance.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 2,851,465 people with type 2 diabetes in the UK, showing lower mortality with existing metformin use. Results are subject to confounding by indication because metformin is typically used early in the progression of type 2 diabetes.
Standard of Care (SOC) for COVID-19 in the study country,
the United Kingdom, is very poor with very low average efficacy for approved treatments1.
The United Kingdom focused on expensive high-profit treatments, approving only one low-cost early treatment, which required a prescription and had limited adoption. The high-cost prescription treatment strategy reduces the probability of early treatment due to access and cost barriers, and eliminates complementary and synergistic benefits seen with many low-cost treatments.
|
risk of death, 23.0% lower, HR 0.77, p < 0.001, adjusted per study.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Khunti et al., 30 Mar 2021, retrospective, population-based cohort, United Kingdom, peer-reviewed, 15 authors.
Prescription of glucose-lowering therapies and risk of COVID-19 mortality in people with type 2 diabetes: a nationwide observational study in England
Background In patients with type 2 diabetes, hyperglycaemia is an independent risk factor for COVID-19-related mortality. Associations between pre-infection prescription for glucose-lowering drugs and COVID-19-related mortality in people with type 2 diabetes have been postulated but only investigated in small studies and limited to a few agents. We investigated whether there are associations between prescription of different classes of glucose-lowering drugs and risk of COVID-19-related mortality in people with type 2 diabetes.
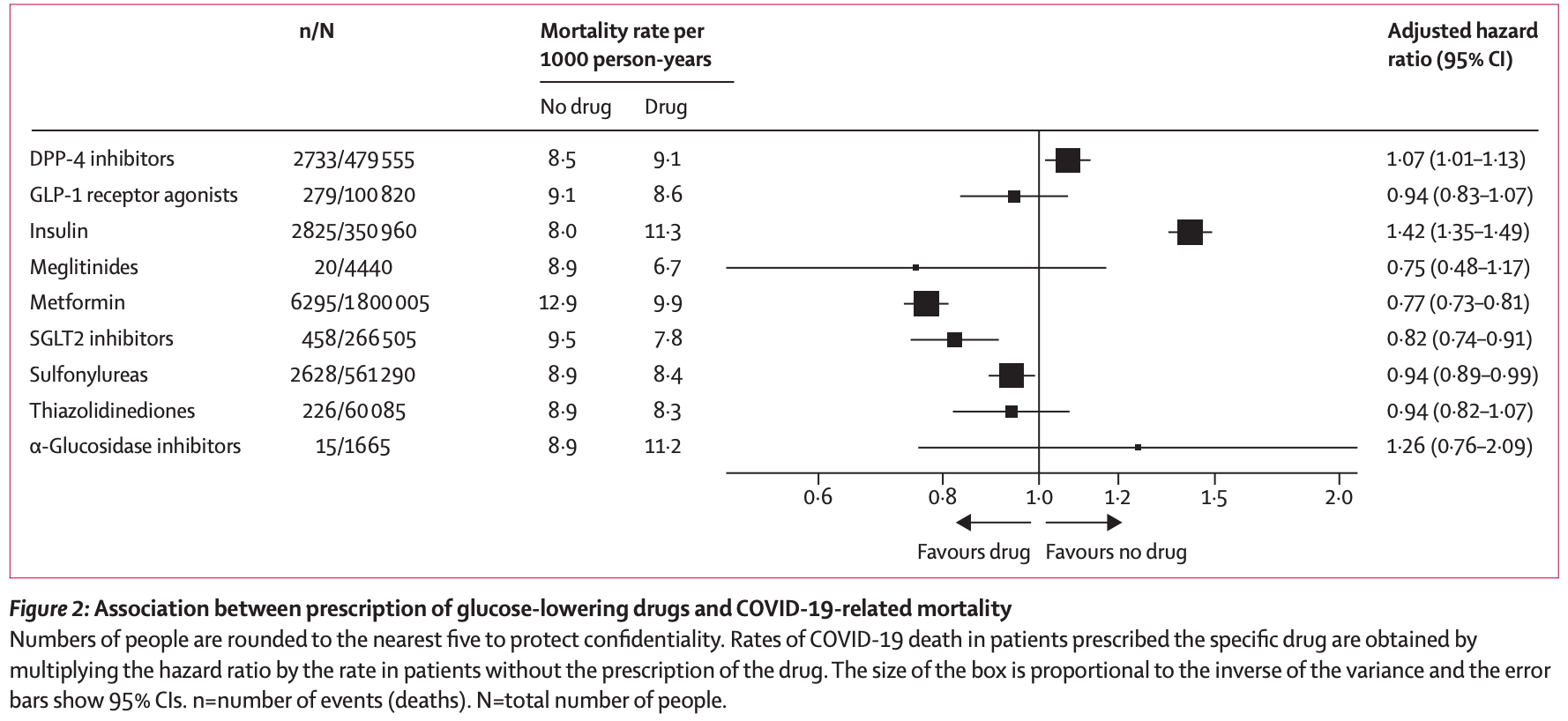
Methods This was a nationwide observational cohort study done with data from the National Diabetes Audit for people with type 2 diabetes and registered with a general practice in England since 2003. Cox regression was used to estimate the hazard ratio (HR) of COVID-19-related mortality in people prescribed each class of glucose-lowering drug, with covariate adjustment with a propensity score to address confounding by demographic, socioeconomic, and clinical factors. Findings Among the 2 851 465 people with type 2 diabetes included in our analyses, 13 479 (0•5%) COVID-19-related deaths occurred during the study period (Feb 16 to Aug 31, 2020), corresponding to a rate of 8•9 per 1000 person-years (95% CI 8•7-9•0). The adjusted HR associated with recorded versus no recorded prescription was 0•77 (95% CI 0•73-0•81) for metformin and 1•42 (1•35-1•49) for insulin. Adjusted HRs for prescription of other individual classes of glucose-lowering treatment were as follows: 0•75 (0•48-1•17) for meglitinides, 0•82 (0•74-0•91) for SGLT2 inhibitors, 0•94 (0•82-1•07) for thiazolidinediones, 0•94 (0•89-0•99) for sulfonylureas, 0•94 (0•83-1•07) for GLP-1 receptor agonists, 1•07 (1•01-1•13) for DPP-4 inhibitors, and 1•26 (0•76-2•09) for α-glucosidase inhibitors. Interpretation Our results provide evidence of associations between prescription of some glucose-lowering drugs and COVID-19-related mortality, although the differences in risk are small and these findings are likely to be due to confounding by indication, in view of the use of different drug classes at different stages of type 2 diabetes disease progression. In the context of the COVID-19 pandemic, there is no clear indication to change prescribing of glucoselowering drugs in people with type 2 diabetes.
References
Anyanwagu, Mamza, Mehta, Donnelly, Idris, Cardiovascular events and all-cause mortality with insulin versus glucagon-like peptide-1 analogue in type 2 diabetes, Heart
Apicella, Campopiano, Mantuano, Mazoni, A, Del Prato S. COVID-19 in people with diabetes: understanding the reasons for worse outcomes
Austin, Stuart, Moving towards best practice when using inverse probability of treatment weighting (IPTW) using the propensity score to estimate causal treatment effects in observational studies, Stat Med
Barron, Bakhai, Kar, Associations of type 1 and type 2 diabetes with COVID-19-related mortality in England: a wholepopulation study, Lancet Diabetes Endocrinol
Bornstein, Rubino, Khunti, Practical recommendations for the management of diabetes in patients with COVID-19, Lancet Diabetes Endocrinol
Bramante, Ingraham, Murray, Metformin and risk of mortality in patients hospitalised with COVID-19: a retrospective cohort analysis, Lancet Healthy Longev
Buse, Wexler, Tsapas, Update to: management of hyperglycemia in type 2 diabetes, 2018. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD), Diabetes Care
Cariou, Hadjadj, Wargny, Phenotypic characteristics and prognosis of inpatients with COVID-19 and diabetes: the CORONADO study, Diabetologia
Cheng, Liu, Li, Metformin is associated with higher incidence of acidosis, but not mortality, in individuals with COVID-19 and pre-existing type 2 diabetes, Cell Metab
Crouse, Grimes, Li, Might, Ovalle et al., Metformin use is associated with reduced mortality in a diverse population with COVID-19 and diabetes, Front Endocrinol
Currie, Poole, Evans, Peters, Morgan, Mortality and other important diabetes-related outcomes with insulin vs other antihyperglycemic therapies in type 2 diabetes, J Clin Endocrinol Metab
Drucker, Coronavirus infections and type 2 diabetes-shared pathways with therapeutic implications, Endocr Rev
Feng, Wang, Ma, Effect of hCMSCs and liraglutide combination in ALI through cAMP/PKAc/β-catenin signaling pathway, Stem Cell Res Ther
Gupta, Ghosh, Singh, Misra, Clinical considerations for patients with diabetes in times of COVID-19 epidemic, Diabetes Metab Syndr
Holman, Knighton, Kar, Risk factors for COVID-19-related mortality in people with type 1 and type 2 diabetes in England: a population-based cohort study, Lancet Diabetes Endocrinol
Kaiser, Mirmira, Stewart, Our response to COVID-19 as endocrinologists and diabetologists, J Clin Endocrinol Metab
Kang, Schafer, Demystifying double robustness: a comparison of alternative strategies for estimating a population mean from incomplete data, Stat Sci
Liang, Ding, Li, Association of preadmission metformin use and mortality in patients with sepsis and diabetes mellitus: a systematic review and meta-analysis of cohort studies, Crit Care
Luo, Qiu, Liu, Metformin treatment was associated with decreased mortality in COVID-19 patients with diabetes in a retrospective analysis, Am J Trop Med Hyg
Monda, Porcellati, Strollo, Gentile, ACE2 and SARS-CoV-2 infection: might GLP-1 receptor agonists play a role?, Diabetes Ther
Monteil, Kwon, Prado, Inhibition of SARS-CoV-2 infections in engineered human tissues using clinical-grade soluble human ACE2, Cell
Pal, Bhadada, Should anti-diabetic medications be reconsidered amid COVID-19 pandemic?, Diabetes Res Clin Pract
Patel, Gupta, Burns, Biochemical urine testing of adherence to cardiovascular medications reveals high rates of nonadherence in people attending their annual review for type 2 diabetes, Diabetes Care
Puig-Domingo, Marazuela, Giustina, COVID-19 and endocrine diseases. A statement from the European Society of Endocrinology, Endocrine
Rosenbaum, Db, The central role of the propensity score in observational studies for causal effects, Biometrika
Sinclair, Dhatariya, Burr, Guidelines for the management of diabetes in care homes during the Covid-19 pandemic, Diabet Med
Singh, Gupta, Ghosh, Misra, Diabetes in COVID-19: prevalence, pathophysiology, prognosis and practical considerations, Diabetes Metab Syndr
Solerte, 'addio, Trevisan, Sitagliptin treatment at the time of hospitalization was associated with reduced mortality in patients with type 2 diabetes and COVID-19: a multicenter, casecontrol, retrospective, observational study, Diabetes Care
Strain, Hope, Green, Kar, Valabhji et al., Type 2 diabetes mellitus in older people: a brief statement of key principles of modern day management including the assessment of frailty. A national collaborative stakeholder initiative, Diabet Med
Vanderweele, Knol, A tutorial on interaction, Epidemiol Methods
Zhu, She, Cheng, Association of blood glucose control and outcomes in patients with COVID-19 and pre-existing type 2 diabetes, Cell Metab
DOI record:
{
"DOI": "10.1016/s2213-8587(21)00050-4",
"ISSN": [
"2213-8587"
],
"URL": "http://dx.doi.org/10.1016/S2213-8587(21)00050-4",
"alternative-id": [
"S2213858721000504"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Prescription of glucose-lowering therapies and risk of COVID-19 mortality in people with type 2 diabetes: a nationwide observational study in England"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "The Lancet Diabetes & Endocrinology"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/S2213-8587(21)00050-4"
},
{
"label": "CrossRef DOI link to the associated document",
"name": "associatedlink",
"value": "https://doi.org/10.1016/S2213-8587(21)00059-0"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2021 Elsevier Ltd. All rights reserved."
}
],
"author": [
{
"affiliation": [],
"family": "Khunti",
"given": "Kamlesh",
"sequence": "first"
},
{
"affiliation": [],
"family": "Knighton",
"given": "Peter",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Zaccardi",
"given": "Francesco",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bakhai",
"given": "Chirag",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Barron",
"given": "Emma",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Holman",
"given": "Naomi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kar",
"given": "Partha",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Meace",
"given": "Claire",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sattar",
"given": "Naveed",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sharp",
"given": "Stephen",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Wareham",
"given": "Nicholas J",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Weaver",
"given": "Andy",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Woch",
"given": "Emilia",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Young",
"given": "Bob",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Valabhji",
"given": "Jonathan",
"sequence": "additional"
}
],
"container-title": "The Lancet Diabetes & Endocrinology",
"container-title-short": "The Lancet Diabetes & Endocrinology",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"clinicalkey.fr",
"clinicalkey.jp",
"clinicalkey.com.au",
"clinicalkey.es",
"clinicalkey.com",
"thelancet.com",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2021,
3,
31
]
],
"date-time": "2021-03-31T01:00:30Z",
"timestamp": 1617152430000
},
"deposited": {
"date-parts": [
[
2023,
5,
2
]
],
"date-time": "2023-05-02T13:50:46Z",
"timestamp": 1683035446000
},
"funder": [
{
"DOI": "10.13039/501100000265",
"award": [
"MC_UU_00006/1"
],
"doi-asserted-by": "publisher",
"name": "Medical Research Council"
},
{
"DOI": "10.13039/501100000272",
"doi-asserted-by": "publisher",
"name": "National Institute for Health Research"
},
{
"DOI": "10.13039/501100018955",
"doi-asserted-by": "publisher",
"name": "Leeds Biomedical Research Centre"
}
],
"indexed": {
"date-parts": [
[
2024,
4,
8
]
],
"date-time": "2024-04-08T17:12:52Z",
"timestamp": 1712596372217
},
"is-referenced-by-count": 137,
"issue": "5",
"issued": {
"date-parts": [
[
2021,
5
]
]
},
"journal-issue": {
"issue": "5",
"published-print": {
"date-parts": [
[
2021,
5
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
1
]
],
"date-time": "2021-05-01T00:00:00Z",
"timestamp": 1619827200000
}
},
{
"URL": "https://doi.org/10.15223/policy-017",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
1
]
],
"date-time": "2021-05-01T00:00:00Z",
"timestamp": 1619827200000
}
},
{
"URL": "https://doi.org/10.15223/policy-037",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
1
]
],
"date-time": "2021-05-01T00:00:00Z",
"timestamp": 1619827200000
}
},
{
"URL": "https://doi.org/10.15223/policy-012",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
1
]
],
"date-time": "2021-05-01T00:00:00Z",
"timestamp": 1619827200000
}
},
{
"URL": "https://doi.org/10.15223/policy-029",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
1
]
],
"date-time": "2021-05-01T00:00:00Z",
"timestamp": 1619827200000
}
},
{
"URL": "https://doi.org/10.15223/policy-004",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
1
]
],
"date-time": "2021-05-01T00:00:00Z",
"timestamp": 1619827200000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S2213858721000504?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S2213858721000504?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "293-303",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2021,
5
]
]
},
"published-print": {
"date-parts": [
[
2021,
5
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1016/S2213-8587(20)30238-2",
"article-title": "COVID-19 in people with diabetes: understanding the reasons for worse outcomes",
"author": "Apicella",
"doi-asserted-by": "crossref",
"first-page": "782",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "10.1016/S2213-8587(21)00050-4_bib1",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(20)30272-2",
"article-title": "Associations of type 1 and type 2 diabetes with COVID-19-related mortality in England: a whole-population study",
"author": "Barron",
"doi-asserted-by": "crossref",
"first-page": "813",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "10.1016/S2213-8587(21)00050-4_bib2",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/j.cmet.2020.04.021",
"article-title": "Association of blood glucose control and outcomes in patients with COVID-19 and pre-existing type 2 diabetes",
"author": "Zhu",
"doi-asserted-by": "crossref",
"first-page": "1068",
"journal-title": "Cell Metab",
"key": "10.1016/S2213-8587(21)00050-4_bib3",
"volume": "31",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(20)30271-0",
"article-title": "Risk factors for COVID-19-related mortality in people with type 1 and type 2 diabetes in England: a population-based cohort study",
"author": "Holman",
"doi-asserted-by": "crossref",
"first-page": "823",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "10.1016/S2213-8587(21)00050-4_bib4",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1210/endrev/bnaa011",
"article-title": "Coronavirus infections and type 2 diabetes—shared pathways with therapeutic implications",
"author": "Drucker",
"doi-asserted-by": "crossref",
"first-page": "457",
"journal-title": "Endocr Rev",
"key": "10.1016/S2213-8587(21)00050-4_bib5",
"volume": "41",
"year": "2020"
},
{
"DOI": "10.1016/j.diabres.2020.108146",
"article-title": "Should anti-diabetic medications be reconsidered amid COVID-19 pandemic?",
"author": "Pal",
"doi-asserted-by": "crossref",
"journal-title": "Diabetes Res Clin Pract",
"key": "10.1016/S2213-8587(21)00050-4_bib6",
"volume": "163",
"year": "2020"
},
{
"DOI": "10.1016/j.cell.2020.04.004",
"article-title": "Inhibition of SARS-CoV-2 infections in engineered human tissues using clinical-grade soluble human ACE2",
"author": "Monteil",
"doi-asserted-by": "crossref",
"first-page": "905",
"journal-title": "Cell",
"key": "10.1016/S2213-8587(21)00050-4_bib7",
"volume": "181",
"year": "2020"
},
{
"DOI": "10.1186/s13287-019-1492-6",
"article-title": "Effect of hCMSCs and liraglutide combination in ALI through cAMP/PKAc/β-catenin signaling pathway",
"author": "Feng",
"doi-asserted-by": "crossref",
"first-page": "2",
"journal-title": "Stem Cell Res Ther",
"key": "10.1016/S2213-8587(21)00050-4_bib8",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1007/s13300-020-00898-8",
"article-title": "ACE2 and SARS-CoV-2 infection: might GLP-1 receptor agonists play a role?",
"author": "Monda",
"doi-asserted-by": "crossref",
"first-page": "1909",
"journal-title": "Diabetes Ther",
"key": "10.1016/S2213-8587(21)00050-4_bib9",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1007/s00125-020-05180-x",
"article-title": "Phenotypic characteristics and prognosis of inpatients with COVID-19 and diabetes: the CORONADO study",
"author": "Cariou",
"doi-asserted-by": "crossref",
"first-page": "1500",
"journal-title": "Diabetologia",
"key": "10.1016/S2213-8587(21)00050-4_bib10",
"volume": "63",
"year": "2020"
},
{
"DOI": "10.2337/dc20-1521",
"article-title": "Sitagliptin treatment at the time of hospitalization was associated with reduced mortality in patients with type 2 diabetes and COVID-19: a multicenter, case-control, retrospective, observational study",
"author": "Solerte",
"doi-asserted-by": "crossref",
"first-page": "2999",
"journal-title": "Diabetes Care",
"key": "10.1016/S2213-8587(21)00050-4_bib11",
"volume": "43",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2020.03.002",
"article-title": "Clinical considerations for patients with diabetes in times of COVID-19 epidemic",
"author": "Gupta",
"doi-asserted-by": "crossref",
"first-page": "211",
"journal-title": "Diabetes Metab Syndr",
"key": "10.1016/S2213-8587(21)00050-4_bib12",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(20)30152-2",
"article-title": "Practical recommendations for the management of diabetes in patients with COVID-19",
"author": "Bornstein",
"doi-asserted-by": "crossref",
"first-page": "546",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "10.1016/S2213-8587(21)00050-4_bib13",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2020.04.004",
"article-title": "Diabetes in COVID-19: prevalence, pathophysiology, prognosis and practical considerations",
"author": "Singh",
"doi-asserted-by": "crossref",
"first-page": "303",
"journal-title": "Diabetes Metab Syndr",
"key": "10.1016/S2213-8587(21)00050-4_bib14",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1111/dme.14317",
"article-title": "Guidelines for the management of diabetes in care homes during the Covid-19 pandemic",
"author": "Sinclair",
"doi-asserted-by": "crossref",
"first-page": "1090",
"journal-title": "Diabet Med",
"key": "10.1016/S2213-8587(21)00050-4_bib15",
"volume": "37",
"year": "2020"
},
{
"DOI": "10.1007/s12020-020-02294-5",
"article-title": "COVID-19 and endocrine diseases. A statement from the European Society of Endocrinology",
"author": "Puig-Domingo",
"doi-asserted-by": "crossref",
"first-page": "2",
"journal-title": "Endocrine",
"key": "10.1016/S2213-8587(21)00050-4_bib16",
"volume": "68",
"year": "2020"
},
{
"DOI": "10.1210/clinem/dgaa148",
"article-title": "Our response to COVID-19 as endocrinologists and diabetologists",
"author": "Kaiser",
"doi-asserted-by": "crossref",
"first-page": "1299",
"journal-title": "J Clin Endocrinol Metab",
"key": "10.1016/S2213-8587(21)00050-4_bib17",
"volume": "105",
"year": "2020"
},
{
"DOI": "10.1016/j.cmet.2020.08.013",
"article-title": "Metformin is associated with higher incidence of acidosis, but not mortality, in individuals with COVID-19 and pre-existing type 2 diabetes",
"author": "Cheng",
"doi-asserted-by": "crossref",
"first-page": "537",
"journal-title": "Cell Metab",
"key": "10.1016/S2213-8587(21)00050-4_bib18",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.2337/dci19-0066",
"article-title": "2019 Update to: management of hyperglycemia in type 2 diabetes, 2018. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD)",
"author": "Buse",
"doi-asserted-by": "crossref",
"first-page": "487",
"journal-title": "Diabetes Care",
"key": "10.1016/S2213-8587(21)00050-4_bib19",
"volume": "43",
"year": "2020"
},
{
"DOI": "10.1002/sim.6607",
"article-title": "Moving towards best practice when using inverse probability of treatment weighting (IPTW) using the propensity score to estimate causal treatment effects in observational studies",
"author": "Austin",
"doi-asserted-by": "crossref",
"first-page": "3661",
"journal-title": "Stat Med",
"key": "10.1016/S2213-8587(21)00050-4_bib22",
"volume": "34",
"year": "2015"
},
{
"DOI": "10.1093/biomet/70.1.41",
"article-title": "The central role of the propensity score in observational studies for causal effects",
"author": "Rosenbaum",
"doi-asserted-by": "crossref",
"first-page": "41",
"journal-title": "Biometrika",
"key": "10.1016/S2213-8587(21)00050-4_bib23",
"volume": "70",
"year": "1983"
},
{
"article-title": "Demystifying double robustness: a comparison of alternative strategies for estimating a population mean from incomplete data",
"author": "Kang",
"first-page": "523",
"journal-title": "Stat Sci",
"key": "10.1016/S2213-8587(21)00050-4_bib24",
"volume": "22",
"year": "2007"
},
{
"DOI": "10.1002/(SICI)1097-0258(19981015)17:19<2265::AID-SIM918>3.0.CO;2-B",
"article-title": "Propensity score methods for bias reduction in the comparison of a treatment to a non-randomized control group",
"author": "D'Agostino",
"doi-asserted-by": "crossref",
"first-page": "2265",
"journal-title": "Stat Med",
"key": "10.1016/S2213-8587(21)00050-4_bib25",
"volume": "17",
"year": "1998"
},
{
"DOI": "10.1111/dme.13644",
"article-title": "Type 2 diabetes mellitus in older people: a brief statement of key principles of modern day management including the assessment of frailty. A national collaborative stakeholder initiative",
"author": "Strain",
"doi-asserted-by": "crossref",
"first-page": "838",
"journal-title": "Diabet Med",
"key": "10.1016/S2213-8587(21)00050-4_bib26",
"volume": "35",
"year": "2018"
},
{
"DOI": "10.1515/em-2013-0005",
"article-title": "A tutorial on interaction",
"author": "VanderWeele",
"doi-asserted-by": "crossref",
"first-page": "33",
"journal-title": "Epidemiol Methods",
"key": "10.1016/S2213-8587(21)00050-4_bib27",
"volume": "3",
"year": "2014"
},
{
"DOI": "10.1210/jc.2012-3042",
"article-title": "Mortality and other important diabetes-related outcomes with insulin vs other antihyperglycemic therapies in type 2 diabetes",
"author": "Currie",
"doi-asserted-by": "crossref",
"first-page": "668",
"journal-title": "J Clin Endocrinol Metab",
"key": "10.1016/S2213-8587(21)00050-4_bib28",
"volume": "98",
"year": "2013"
},
{
"DOI": "10.1136/heartjnl-2015-309164",
"article-title": "Cardiovascular events and all-cause mortality with insulin versus glucagon-like peptide-1 analogue in type 2 diabetes",
"author": "Anyanwagu",
"doi-asserted-by": "crossref",
"first-page": "1581",
"journal-title": "Heart",
"key": "10.1016/S2213-8587(21)00050-4_bib29",
"volume": "102",
"year": "2016"
},
{
"DOI": "10.4269/ajtmh.20-0375",
"article-title": "Metformin treatment was associated with decreased mortality in COVID-19 patients with diabetes in a retrospective analysis",
"author": "Luo",
"doi-asserted-by": "crossref",
"first-page": "69",
"journal-title": "Am J Trop Med Hyg",
"key": "10.1016/S2213-8587(21)00050-4_bib30",
"volume": "103",
"year": "2020"
},
{
"DOI": "10.1016/S2666-7568(20)30033-7",
"article-title": "Metformin and risk of mortality in patients hospitalised with COVID-19: a retrospective cohort analysis",
"author": "Bramante",
"doi-asserted-by": "crossref",
"first-page": "e34",
"journal-title": "Lancet Healthy Longev",
"key": "10.1016/S2213-8587(21)00050-4_bib31",
"volume": "2",
"year": "2021"
},
{
"DOI": "10.3389/fendo.2020.600439",
"article-title": "Metformin use is associated with reduced mortality in a diverse population with COVID-19 and diabetes",
"author": "Crouse",
"doi-asserted-by": "crossref",
"journal-title": "Front Endocrinol",
"key": "10.1016/S2213-8587(21)00050-4_bib32",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.1186/s13054-019-2346-4",
"article-title": "Association of preadmission metformin use and mortality in patients with sepsis and diabetes mellitus: a systematic review and meta-analysis of cohort studies",
"author": "Liang",
"doi-asserted-by": "crossref",
"first-page": "50",
"journal-title": "Crit Care",
"key": "10.1016/S2213-8587(21)00050-4_bib33",
"volume": "23",
"year": "2019"
},
{
"DOI": "10.2337/dc18-1453",
"article-title": "Biochemical urine testing of adherence to cardiovascular medications reveals high rates of nonadherence in people attending their annual review for type 2 diabetes",
"author": "Patel",
"doi-asserted-by": "crossref",
"first-page": "1132",
"journal-title": "Diabetes Care",
"key": "10.1016/S2213-8587(21)00050-4_bib34",
"volume": "42",
"year": "2019"
}
],
"reference-count": 32,
"references-count": 32,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S2213858721000504"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Endocrinology",
"Endocrinology, Diabetes and Metabolism",
"Internal Medicine"
],
"subtitle": [],
"title": "Prescription of glucose-lowering therapies and risk of COVID-19 mortality in people with type 2 diabetes: a nationwide observational study in England",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "9"
}
