Association of dietary inflammatory index and the SARS-CoV-2 infection incidence, severity and mortality of COVID-19: a systematic review and dose-response meta-analysis
et al., Nutrition Journal, doi:10.1186/s12937-024-00927-3, PROSPERO CRD42023407410, Feb 2024
Diet for COVID-19
26th treatment shown to reduce risk in
June 2021, now with p < 0.00000000001 from 30 studies, recognized in 4 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Systematic review and dose-response meta-analysis of 5 studies with 197,929 participants showing higher SARS-CoV-2 infection risk and COVID-19 severity with higher Dietary Inflammatory Index (DII) scores. The odds of COVID-19 increased 31% per 1-point rise in E-DII.
2 meta-analyses show significant improvements with diet for hospitalization1,
severity2, and
cases1,2.
Currently there are 30 diet for COVID-19 studies, showing 20% lower mortality [-15‑44%], 99% lower ICU admission [79‑100%], 73% lower hospitalization [60‑82%], and 35% fewer cases [26‑43%].
Hao et al., 20 Feb 2024, peer-reviewed, 6 authors, trial PROSPERO CRD42023407410.
Contact: dyli@sj-hospital.org.
Association of dietary inflammatory index and the SARS-CoV-2 infection incidence, severity and mortality of COVID-19: a systematic review and dose-response meta-analysis
Nutrition Journal, doi:10.1186/s12937-024-00927-3
Background Several studies have reported the association between dietary inflammatory index (DII) and the SARS-CoV-2 infection risk, severity or mortality of COVID-19, however, the outcomes remain controversial. Objective We sought to examine whether a dose-response association of DII and SARS-CoV-2 infection exists. Design A dose-response meta-analysis was performed to investigate the association of DII and SARS-CoV-2 infection. We conducted a systematic search of PubMed, Embase and Web of Science up to March 15th, 2023. The odds ratios (OR) of DII and COVID-19 risk and severity were computed.
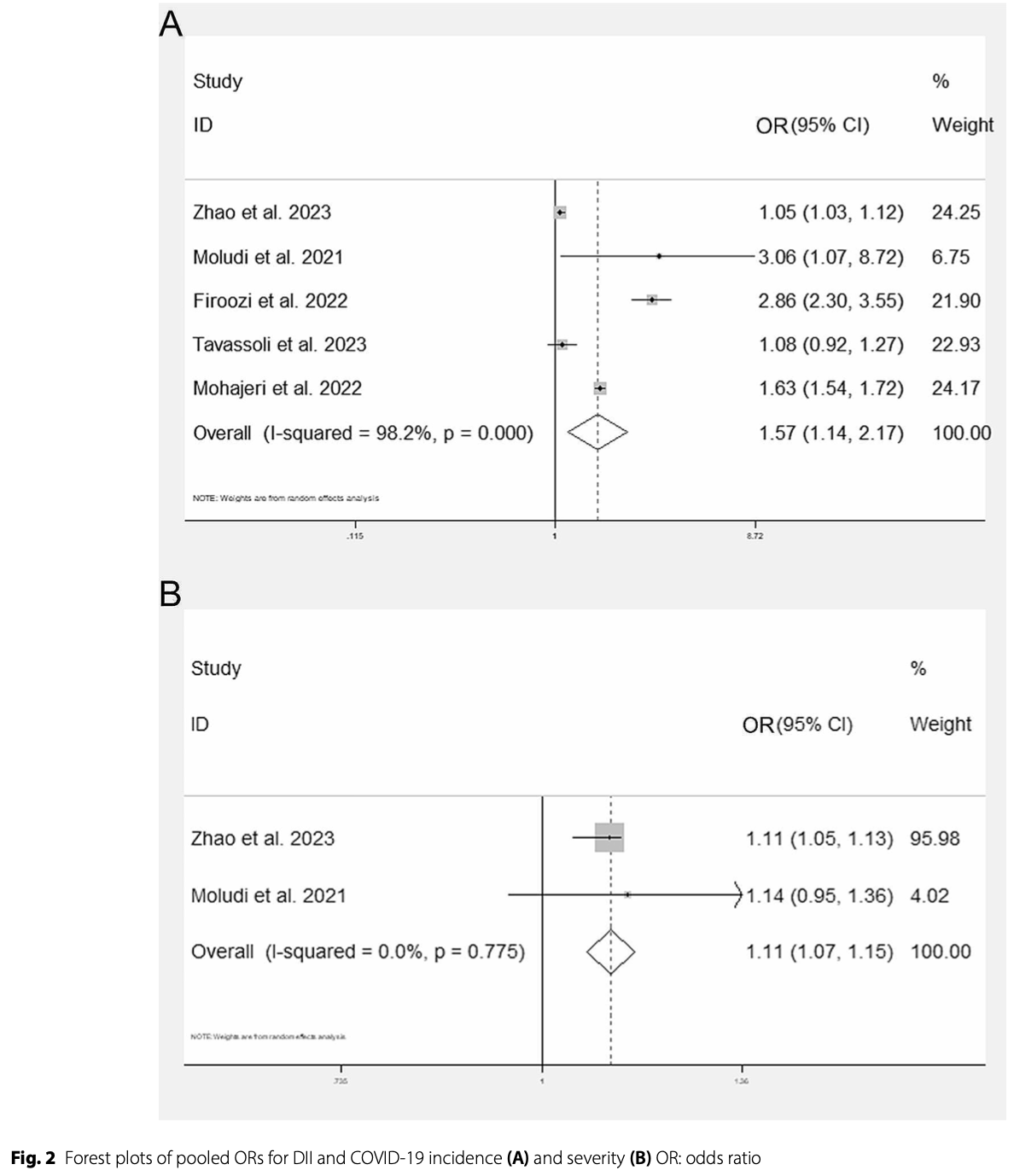
Results Totally, 5 studies were included (1 from UK and 4 from Iran), consisting of 197,929 participants with 12,081 COVID-19 cases. Although there was heterogeneity among studies, the results indicated that higher DII was independently related to higher SARS-CoV-2 infection incidence (OR = 1.57, 95% CI: 1.14, 2.17) and COVID-19 severity (OR = 1.11, 95% CI: 1.07, 1.15) but not COVID-19 mortality (risk ratio = 1.13, 95% CI: 1.00, 1.27). The incidence of SARS-CoV-2 infection increased by 31% for each 1-point increase in the E-DII (OR = 1.31, 95% CI: 1.20, 1.43).
Conclusions This meta-analysis suggests that an elevated DII score is associated with increased SARS-CoV-2 infectious risk and severity of COVID-19. There were not enough studies on COVID-19 mortality. Further large prospective studies in different countries are warranted to validate our results.
Supplementary Information The online version contains supplementary material available at https://doi. org/10.1186/s12937-024-00927-3.
Supplementary Material 1
Declarations Ethical approval Not applicable.
Consent to publication Not applicable.
Competing interests The authors declare no competing interests.
Publisher's Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Aune, Greenwood, Chan, Body mass index, abdominal fatness and pancreatic cancer risk: a systematic review and non-linear dose-response meta-analysis of prospective studies, Annals Oncology: Official J Eur Soc Med Oncol
Bagnardi, Zambon, Quatto, Corrao, Flexible meta-regression functions for modeling aggregate dose-response data, with an application to alcohol and mortality, Am J Epidemiol
Begg, Mazumdar, Operating characteristics of a rank correlation test for publication bias, Biometrics
Boaz, Kaufman-Shriqui, Systematic review and Meta-analysis: Malnutrition and In-Hospital death in adults hospitalized with COVID-19, Nutrients
Butler, Barrientos, The impact of nutrition on COVID-19 susceptibility and long-term consequences, Brain Behav Immun
Calder, Ahluwalia, Brouns, Dietary factors and low-grade inflammation in relation to overweight and obesity, Br J Nutr
Da, Santos, De Mattos Pimenta, Nobre, The PICO strategy for the research question construction and evidence search, Rev Latinoam Enferm
Firoozi, Masoumi, The Association between Energy-Adjusted Dietary Inflammatory Index, body composition, and Anthropometric indices in COVID-19-Infected patients: a case-control study in Shiraz, Iran, Int J Clin Pract
Gobbi, Brunani, Arreghini, Nutritional status in post SARS-Cov2 rehabilitation patients, Clin Nutr
Guenther, Reedy, Krebs-Smith, Development of the healthy eating Index-2005, J Am Diet Assoc
Jiang, Yin, Liu, Liu, Ma et al., Dietary inflammatory index and depression risk in patients with chronic diseases and comorbidity, J Affect Disord
Khoury, Julien, Inverse Association between the Mediterranean Diet and COVID-19 risk in Lebanon: a case-control study, Front Nutr
Kunnumakkara, Rana, Parama, COVID-19, cytokines, inflammation, and spices: how are they related?, Life Sci
Kwok, Kontopantelis, Kuligowski, Self-reported Sleep Duration and Quality and Cardiovascular Disease and Mortality: a dose-response Metaanalysis, J Am Heart Association
Lee, Cohet, Yang, Stayner, Hashibe et al., Meta-analysis of epidemiologic studies on cigarette smoking and liver cancer, Int J Epidemiol
Li, Hao, Li, Dose-response relation between dietary inflammatory index and human cancer risk: evidence from 44 epidemiologic studies involving 1,082,092 participants, Am J Clin Nutr
Li, Lai, The emergence, genomic diversity and global spread of SARS-CoV-2, Nature
Li, Xu, Yu, Risk factors for severity and mortality in adult COVID-19 inpatients in Wuhan, J Allergy Clin Immunol
Mcintyre, Aggarwal, Jani, COVID-19 vaccine strategies must focus on severe disease and global equity, Lancet
Milton-Laskibar, Trepiana, Potential usefulness of Mediterranean diet polyphenols against COVID-19-induced inflammation: a review of the current knowledge, J Physiol Biochem
Mohajeri, Mohajery, Nemati, Pourfarzi, The difference in the dietary inflammatory index, functional food, and antioxidants intake between COVID -19 patients and healthy persons, Mediterranean J Nutr Metabolism
Moher, Liberati, Tetzlaff, Altman, Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement, BMJ (Clinical Res ed)
Moludi, Qaisar, Alizadeh, The relationship between Dietary Inflammatory Index and disease severity and inflammatory status: a casecontrol study of COVID-19 patients, Br J Nutr
Montero López, Urda, Changes in eating behaviors during the COVID-19 Lockdown and the impact on the potential Inflammatory effects of Diet, Int J Environ Res Public Health
Morais, Aquino, Nutritional status, diet and viral respiratory infections: perspectives for severe acute respiratory syndrome coronavirus 2, Br J Nutr
Olczak-Pruc, Swieczkowski, Vitamin C supplementation for the treatment of COVID-19: a systematic review and Meta-analysis, Nutrients
Orsini, Li, Wolk, Khudyakov, Spiegelman, Meta-analysis for linear and nonlinear dose-response relations: examples, an evaluation of approximations, and software, Am J Epidemiol
Petrelli, Oldani, Borgonovo, Vitamin D3 and COVID-19 outcomes: an Umbrella Review of systematic reviews and Meta-analyses
Ponzo, Pellegrini, Eusebio, Bioletto, Goitre et al., Mediterranean Diet and SARS-COV-2 infection: is there any Association? A proof-of-Concept Study, Nutrients
Rahmati, Fatemi, Yon, The effect of adherence to high-quality dietary pattern on COVID-19 outcomes: a systematic review and meta-analysis, J Med Virol
Schwingshackl, Bogensberger, Hoffmann, Diet Quality as assessed by the healthy eating index, alternate healthy eating Index, Dietary approaches to stop hypertension score, and Health outcomes: an updated systematic review and Meta-analysis of Cohort studies, J Acad Nutr Dietetics
Shivappa, Godos, Hébert, Dietary Inflammatory Index and Cardiovascular Risk and Mortality-A Meta-Analysis, Nutrients
Shivappa, Steck, Hurley, A population-based dietary inflammatory index predicts levels of C-reactive protein in the Seasonal variation of blood cholesterol study (SEASONS), Public Health Nutr
Shivappa, Steck, Hurley, Hussey, Hébert, Designing and developing a literature-derived, population-based dietary inflammatory index, Public Health Nutr
Skrajnowska, Brumer, Kankowska, Matysek, Miazio et al., Covid 19: Diet Composition and Health, Nutrients
Tavassoli, Askar, Hadi, The Association between Dietary Inflammatory Index with risk of coronavirus infection and severity: a case-control study, Int J Prev Med
Tay, Poh, Rénia, The trinity of COVID-19: immunity, inflammation and intervention, Nat Rev Immunol
Toor, Saleh, T-cell responses and therapies against SARS-CoV-2 infection, Immunology
Vj, Bustamante-Sanchez, Inflammation in COVID-19 and the effects of non-pharmacological interventions during the pandemic: a review, Int J Mol Sci
Wang, Perlman, COVID-19: Inflammatory Profile, Annu Rev Med
Wouters, Shadlen, Salcher-Konrad, Challenges in ensuring global access to COVID-19 vaccines: production, affordability, allocation, and deployment, Lancet
Yang, Yu, Xu, Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study, Lancet Respiratory Med
Zabetakis, Lordan, COVID-19: the inflammation link and the role of Nutrition in potential mitigation, Nutrients
Zeng, Zhang, Kwong, The methodological quality assessment tools for preclinical and clinical studies, systematic review and meta-analysis, and clinical practice guideline: a systematic review, J evidence-based Med
Zhao, Wirth, Petermann-Rocha, Diet-Related Inflammation Is Associated with Worse COVID-19 Outcomes in the UK Biobank Cohort, Nutrients
DOI record:
{
"DOI": "10.1186/s12937-024-00927-3",
"ISSN": [
"1475-2891"
],
"URL": "http://dx.doi.org/10.1186/s12937-024-00927-3",
"abstract": "<jats:title>Abstract</jats:title><jats:sec>\n <jats:title>Background</jats:title>\n <jats:p>Several studies have reported the association between dietary inflammatory index (DII) and the SARS-CoV-2 infection risk, severity or mortality of COVID-19, however, the outcomes remain controversial.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Objective</jats:title>\n <jats:p>We sought to examine whether a dose-response association of DII and SARS-CoV-2 infection exists.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Design</jats:title>\n <jats:p>A dose-response meta-analysis was performed to investigate the association of DII and SARS-CoV-2 infection. We conducted a systematic search of PubMed, Embase and Web of Science up to March 15th, 2023. The odds ratios (OR) of DII and COVID-19 risk and severity were computed.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Results</jats:title>\n <jats:p>Totally, 5 studies were included (1 from UK and 4 from Iran), consisting of 197,929 participants with 12,081 COVID-19 cases. Although there was heterogeneity among studies, the results indicated that higher DII was independently related to higher SARS-CoV-2 infection incidence (OR = 1.57, 95% CI: 1.14, 2.17) and COVID-19 severity (OR = 1.11, 95% CI: 1.07, 1.15) but not COVID-19 mortality (risk ratio = 1.13, 95% CI: 1.00, 1.27). The incidence of SARS-CoV-2 infection increased by 31% for each 1-point increase in the E-DII (OR = 1.31, 95% CI: 1.20, 1.43).</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Conclusions</jats:title>\n <jats:p>This meta-analysis suggests that an elevated DII score is associated with increased SARS-CoV-2 infectious risk and severity of COVID-19. There were not enough studies on COVID-19 mortality. Further large prospective studies in different countries are warranted to validate our results.</jats:p>\n </jats:sec>",
"alternative-id": [
"927"
],
"article-number": "21",
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "2 September 2023"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "15 February 2024"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "20 February 2024"
},
{
"group": {
"label": "Declarations",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Ethical approval",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "Not applicable."
},
{
"group": {
"label": "Consent to publication",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "Not applicable."
},
{
"group": {
"label": "Competing interests",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 4,
"value": "The authors declare no competing interests."
},
{
"group": {
"label": "Source of support",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 5,
"value": "This study didn?t receive any external funding."
},
{
"group": {
"label": "PROSPERO Registry number and websites",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 6,
"value": "PROSPERO :<b>CRD42023407410</b> Available from: ExternalRef removed"
}
],
"author": [
{
"affiliation": [],
"family": "Hao",
"given": "Xuanyu",
"sequence": "first"
},
{
"affiliation": [],
"family": "Li",
"given": "Shiwen",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Yang",
"given": "Yanmin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Dai",
"given": "Huixu",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Yan",
"given": "Yumeng",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Li",
"given": "Dongyang",
"sequence": "additional"
}
],
"container-title": "Nutrition Journal",
"container-title-short": "Nutr J",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2024,
2,
20
]
],
"date-time": "2024-02-20T03:02:24Z",
"timestamp": 1708398144000
},
"deposited": {
"date-parts": [
[
2024,
2,
20
]
],
"date-time": "2024-02-20T03:03:44Z",
"timestamp": 1708398224000
},
"indexed": {
"date-parts": [
[
2024,
2,
21
]
],
"date-time": "2024-02-21T00:28:25Z",
"timestamp": 1708475305150
},
"is-referenced-by-count": 0,
"issue": "1",
"issued": {
"date-parts": [
[
2024,
2,
20
]
]
},
"journal-issue": {
"issue": "1",
"published-online": {
"date-parts": [
[
2024,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2024,
2,
20
]
],
"date-time": "2024-02-20T00:00:00Z",
"timestamp": 1708387200000
}
},
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2024,
2,
20
]
],
"date-time": "2024-02-20T00:00:00Z",
"timestamp": 1708387200000
}
}
],
"link": [
{
"URL": "https://link.springer.com/content/pdf/10.1186/s12937-024-00927-3.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/article/10.1186/s12937-024-00927-3/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/content/pdf/10.1186/s12937-024-00927-3.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"prefix": "10.1186",
"published": {
"date-parts": [
[
2024,
2,
20
]
]
},
"published-online": {
"date-parts": [
[
2024,
2,
20
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.1038/s41586-021-04188-6",
"author": "J Li",
"doi-asserted-by": "publisher",
"first-page": "408",
"journal-title": "Nature",
"key": "927_CR1",
"unstructured": "Li J, Lai S. The emergence, genomic diversity and global spread of SARS-CoV-2. Nature. 2021;600:408–18.",
"volume": "600",
"year": "2021"
},
{
"DOI": "10.1016/S0140-6736(21)02835-X",
"author": "PB McIntyre",
"doi-asserted-by": "publisher",
"first-page": "406",
"journal-title": "Lancet (London England)",
"key": "927_CR2",
"unstructured": "McIntyre PB, Aggarwal R, Jani I, et al. COVID-19 vaccine strategies must focus on severe disease and global equity. Lancet (London England). 2022;399:406–10.",
"volume": "399",
"year": "2022"
},
{
"DOI": "10.1016/S0140-6736(21)00306-8",
"author": "OJ Wouters",
"doi-asserted-by": "publisher",
"first-page": "1023",
"journal-title": "Lancet (London England)",
"key": "927_CR3",
"unstructured": "Wouters OJ, Shadlen KC, Salcher-Konrad M, et al. Challenges in ensuring global access to COVID-19 vaccines: production, affordability, allocation, and deployment. Lancet (London England). 2021;397:1023–34.",
"volume": "397",
"year": "2021"
},
{
"DOI": "10.1016/j.lfs.2021.119201",
"author": "AB Kunnumakkara",
"doi-asserted-by": "publisher",
"first-page": "119201",
"journal-title": "Life Sci",
"key": "927_CR4",
"unstructured": "Kunnumakkara AB, Rana V, Parama D, et al. COVID-19, cytokines, inflammation, and spices: how are they related? Life Sci. 2021;284:119201.",
"volume": "284",
"year": "2021"
},
{
"DOI": "10.1038/s41577-020-0311-8",
"author": "MZ Tay",
"doi-asserted-by": "publisher",
"first-page": "363",
"journal-title": "Nat Rev Immunol",
"key": "927_CR5",
"unstructured": "Tay MZ, Poh CM, Rénia L. The trinity of COVID-19: immunity, inflammation and intervention. Nat Rev Immunol. 2020;20:363–74.",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.1002/jmv.28298",
"author": "M Rahmati",
"doi-asserted-by": "publisher",
"first-page": "e28298",
"journal-title": "J Med Virol",
"key": "927_CR6",
"unstructured": "Rahmati M, Fatemi R, Yon DK. The effect of adherence to high-quality dietary pattern on COVID-19 outcomes: a systematic review and meta-analysis. J Med Virol. 2023;95:e28298.",
"volume": "95",
"year": "2023"
},
{
"DOI": "10.3390/nu15051298",
"doi-asserted-by": "crossref",
"key": "927_CR7",
"unstructured": "Boaz M, Kaufman-Shriqui V. Systematic review and Meta-analysis: Malnutrition and In-Hospital death in adults hospitalized with COVID-19. Nutrients. 2023;15."
},
{
"DOI": "10.3389/fnut.2021.707359",
"author": "CN El Khoury",
"doi-asserted-by": "publisher",
"first-page": "707359",
"journal-title": "Front Nutr",
"key": "927_CR8",
"unstructured": "El Khoury CN, Julien SG. Inverse Association between the Mediterranean Diet and COVID-19 risk in Lebanon: a case-control study. Front Nutr. 2021;8:707359.",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.1007/s13105-022-00926-0",
"doi-asserted-by": "crossref",
"key": "927_CR9",
"unstructured": "Milton-Laskibar I, Trepiana J. Potential usefulness of Mediterranean diet polyphenols against COVID-19-induced inflammation: a review of the current knowledge. J Physiol Biochem. 2022:1–12."
},
{
"DOI": "10.3390/nu14194217",
"doi-asserted-by": "crossref",
"key": "927_CR10",
"unstructured": "Olczak-Pruc M, Swieczkowski D. Vitamin C supplementation for the treatment of COVID-19: a systematic review and Meta-analysis. Nutrients. 2022;14."
},
{
"DOI": "10.3390/antiox12020247",
"doi-asserted-by": "crossref",
"key": "927_CR11",
"unstructured": "Petrelli F, Oldani S, Borgonovo K et al. Vitamin D3 and COVID-19 outcomes: an Umbrella Review of systematic reviews and Meta-analyses. Antioxidants (Basel, Switzerland). 2023;12."
},
{
"DOI": "10.1017/S0007114520003311",
"author": "AHA Morais",
"doi-asserted-by": "publisher",
"first-page": "851",
"journal-title": "Br J Nutr",
"key": "927_CR12",
"unstructured": "Morais AHA, Aquino JS. Nutritional status, diet and viral respiratory infections: perspectives for severe acute respiratory syndrome coronavirus 2. Br J Nutr. 2021;125:851–62.",
"volume": "125",
"year": "2021"
},
{
"DOI": "10.1017/S1368980013002115",
"author": "N Shivappa",
"doi-asserted-by": "publisher",
"first-page": "1689",
"journal-title": "Public Health Nutr",
"key": "927_CR13",
"unstructured": "Shivappa N, Steck SE, Hurley TG, Hussey JR, Hébert JR. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014;17:1689–96.",
"volume": "17",
"year": "2014"
},
{
"DOI": "10.1017/S1368980013002565",
"author": "N Shivappa",
"doi-asserted-by": "publisher",
"first-page": "1825",
"journal-title": "Public Health Nutr",
"key": "927_CR14",
"unstructured": "Shivappa N, Steck SE, Hurley TG, et al. A population-based dietary inflammatory index predicts levels of C-reactive protein in the Seasonal variation of blood cholesterol study (SEASONS). Public Health Nutr. 2014;17:1825–33.",
"volume": "17",
"year": "2014"
},
{
"DOI": "10.3390/nu10020200",
"doi-asserted-by": "crossref",
"key": "927_CR15",
"unstructured": "Shivappa N, Godos J, Hébert JR et al. Dietary Inflammatory Index and Cardiovascular Risk and Mortality-A Meta-Analysis. Nutrients. 2018;10."
},
{
"DOI": "10.1016/j.jad.2022.01.008",
"author": "C Jiang",
"doi-asserted-by": "publisher",
"first-page": "307",
"journal-title": "J Affect Disord",
"key": "927_CR16",
"unstructured": "Jiang C, Yin H, Liu A, Liu Q, Ma H, Geng Q. Dietary inflammatory index and depression risk in patients with chronic diseases and comorbidity. J Affect Disord. 2022;301:307–14.",
"volume": "301",
"year": "2022"
},
{
"DOI": "10.1093/ajcn/nqx064",
"author": "D Li",
"doi-asserted-by": "publisher",
"first-page": "371",
"journal-title": "Am J Clin Nutr",
"key": "927_CR17",
"unstructured": "Li D, Hao X, Li J, et al. Dose-response relation between dietary inflammatory index and human cancer risk: evidence from 44 epidemiologic studies involving 1,082,092 participants. Am J Clin Nutr. 2018;107:371–88.",
"volume": "107",
"year": "2018"
},
{
"DOI": "10.1017/S0007114511005460",
"author": "PC Calder",
"doi-asserted-by": "publisher",
"first-page": "5",
"issue": "Suppl 3",
"journal-title": "Br J Nutr",
"key": "927_CR18",
"unstructured": "Calder PC, Ahluwalia N, Brouns F, et al. Dietary factors and low-grade inflammation in relation to overweight and obesity. Br J Nutr. 2011;106(Suppl 3):5–78.",
"volume": "106",
"year": "2011"
},
{
"DOI": "10.3390/nu13051721",
"doi-asserted-by": "crossref",
"key": "927_CR19",
"unstructured": "Ponzo V, Pellegrini M, D’Eusebio C, Bioletto F, Goitre I, Buscemi S. Mediterranean Diet and SARS-COV-2 infection: is there any Association? A proof-of-Concept Study. Nutrients. 2021;13."
},
{
"DOI": "10.3390/nu13092980",
"doi-asserted-by": "crossref",
"key": "927_CR20",
"unstructured": "Skrajnowska D, Brumer M, Kankowska S, Matysek M, Miazio N, Bobrowska-Korczak B. Covid 19: Diet Composition and Health. Nutrients. 2021;13."
},
{
"DOI": "10.1016/j.jaci.2020.04.006",
"author": "X Li",
"doi-asserted-by": "publisher",
"first-page": "110",
"journal-title": "J Allergy Clin Immunol",
"key": "927_CR21",
"unstructured": "Li X, Xu S, Yu M, et al. Risk factors for severity and mortality in adult COVID-19 inpatients in Wuhan. J Allergy Clin Immunol. 2020;146:110–8.",
"volume": "146",
"year": "2020"
},
{
"DOI": "10.3390/nu12051466",
"doi-asserted-by": "crossref",
"key": "927_CR22",
"unstructured": "Zabetakis I, Lordan R. COVID-19: the inflammation link and the role of Nutrition in potential mitigation. Nutrients. 2020;12."
},
{
"DOI": "10.1016/j.bbi.2020.04.040",
"author": "MJ Butler",
"doi-asserted-by": "publisher",
"first-page": "53",
"journal-title": "Brain Behav Immun",
"key": "927_CR23",
"unstructured": "Butler MJ, Barrientos RM. The impact of nutrition on COVID-19 susceptibility and long-term consequences. Brain Behav Immun. 2020;87:53–4.",
"volume": "87",
"year": "2020"
},
{
"DOI": "10.1016/j.jada.2008.08.016",
"author": "PM Guenther",
"doi-asserted-by": "publisher",
"first-page": "1896",
"journal-title": "J Am Diet Assoc",
"key": "927_CR24",
"unstructured": "Guenther PM, Reedy J, Krebs-Smith SM. Development of the healthy eating Index-2005. J Am Diet Assoc. 2008;108:1896–901.",
"volume": "108",
"year": "2008"
},
{
"DOI": "10.1016/j.jand.2017.08.024",
"author": "L Schwingshackl",
"doi-asserted-by": "publisher",
"first-page": "74",
"journal-title": "J Acad Nutr Dietetics",
"key": "927_CR25",
"unstructured": "Schwingshackl L, Bogensberger B, Hoffmann G. Diet Quality as assessed by the healthy eating index, alternate healthy eating Index, Dietary approaches to stop hypertension score, and Health outcomes: an updated systematic review and Meta-analysis of Cohort studies. J Acad Nutr Dietetics. 2018;118:74–100e111.",
"volume": "118",
"year": "2018"
},
{
"DOI": "10.1016/j.clnu.2021.04.013",
"author": "M Gobbi",
"doi-asserted-by": "publisher",
"first-page": "3055",
"journal-title": "Clin Nutr",
"key": "927_CR26",
"unstructured": "Gobbi M, Brunani A, Arreghini M, et al. Nutritional status in post SARS-Cov2 rehabilitation patients. Clin Nutr. 2022;41:3055–60.",
"volume": "41",
"year": "2022"
},
{
"DOI": "10.3390/nu15040884",
"doi-asserted-by": "crossref",
"key": "927_CR27",
"unstructured": "Zhao L, Wirth MD, Petermann-Rocha F. Diet-Related Inflammation Is Associated with Worse COVID-19 Outcomes in the UK Biobank Cohort. Nutrients. 2023;15."
},
{
"author": "M Tavassoli",
"first-page": "14",
"journal-title": "Int J Prev Med",
"key": "927_CR28",
"unstructured": "Tavassoli M, Askar G, Hadi V, et al. The Association between Dietary Inflammatory Index with risk of coronavirus infection and severity: a case–control study. Int J Prev Med. 2023;14:14.",
"volume": "14",
"year": "2023"
},
{
"DOI": "10.1136/bmj.b2535",
"author": "D Moher",
"doi-asserted-by": "publisher",
"first-page": "b2535",
"journal-title": "BMJ (Clinical Res ed)",
"key": "927_CR29",
"unstructured": "Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ (Clinical Res ed). 2009;339:b2535.",
"volume": "339",
"year": "2009"
},
{
"DOI": "10.1590/S0104-11692007000300023",
"author": "CM da Costa Santos",
"doi-asserted-by": "publisher",
"first-page": "508",
"journal-title": "Rev Latinoam Enferm",
"key": "927_CR30",
"unstructured": "da Costa Santos CM, de Mattos Pimenta CA, Nobre MR. The PICO strategy for the research question construction and evidence search. Rev Latinoam Enferm. 2007;15:508–11.",
"volume": "15",
"year": "2007"
},
{
"DOI": "10.1111/jebm.12141",
"author": "X Zeng",
"doi-asserted-by": "publisher",
"first-page": "2",
"journal-title": "J evidence-based Med",
"key": "927_CR31",
"unstructured": "Zeng X, Zhang Y, Kwong JS, et al. The methodological quality assessment tools for preclinical and clinical studies, systematic review and meta-analysis, and clinical practice guideline: a systematic review. J evidence-based Med. 2015;8:2–10.",
"volume": "8",
"year": "2015"
},
{
"DOI": "10.1161/JAHA.118.008552",
"author": "CS Kwok",
"doi-asserted-by": "publisher",
"first-page": "e008552",
"journal-title": "J Am Heart Association",
"key": "927_CR32",
"unstructured": "Kwok CS, Kontopantelis E, Kuligowski G, et al. Self-reported Sleep Duration and Quality and Cardiovascular Disease and Mortality: a dose-response Meta-analysis. J Am Heart Association. 2018;7:e008552.",
"volume": "7",
"year": "2018"
},
{
"DOI": "10.1093/ije/dyp280",
"author": "YC Lee",
"doi-asserted-by": "publisher",
"first-page": "1497",
"journal-title": "Int J Epidemiol",
"key": "927_CR33",
"unstructured": "Lee YC, Cohet C, Yang YC, Stayner L, Hashibe M, Straif K. Meta-analysis of epidemiologic studies on cigarette smoking and liver cancer. Int J Epidemiol. 2009;38:1497–511.",
"volume": "38",
"year": "2009"
},
{
"DOI": "10.1093/aje/kwh142",
"author": "V Bagnardi",
"doi-asserted-by": "publisher",
"first-page": "1077",
"journal-title": "Am J Epidemiol",
"key": "927_CR34",
"unstructured": "Bagnardi V, Zambon A, Quatto P, Corrao G. Flexible meta-regression functions for modeling aggregate dose-response data, with an application to alcohol and mortality. Am J Epidemiol. 2004;159:1077–86.",
"volume": "159",
"year": "2004"
},
{
"DOI": "10.1093/annonc/mdr398",
"author": "D Aune",
"doi-asserted-by": "publisher",
"first-page": "843",
"journal-title": "Annals Oncology: Official J Eur Soc Med Oncol",
"key": "927_CR35",
"unstructured": "Aune D, Greenwood DC, Chan DS, et al. Body mass index, abdominal fatness and pancreatic cancer risk: a systematic review and non-linear dose-response meta-analysis of prospective studies. Annals Oncology: Official J Eur Soc Med Oncol. 2012;23:843–52.",
"volume": "23",
"year": "2012"
},
{
"DOI": "10.1093/aje/kwr265",
"author": "N Orsini",
"doi-asserted-by": "publisher",
"first-page": "66",
"journal-title": "Am J Epidemiol",
"key": "927_CR36",
"unstructured": "Orsini N, Li R, Wolk A, Khudyakov P, Spiegelman D. Meta-analysis for linear and nonlinear dose-response relations: examples, an evaluation of approximations, and software. Am J Epidemiol. 2012;175:66–73.",
"volume": "175",
"year": "2012"
},
{
"DOI": "10.2307/2533446",
"author": "CB Begg",
"doi-asserted-by": "publisher",
"first-page": "1088",
"journal-title": "Biometrics",
"key": "927_CR37",
"unstructured": "Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics. 1994;50:1088–101.",
"volume": "50",
"year": "1994"
},
{
"DOI": "10.1017/S0007114521003214",
"author": "J Moludi",
"doi-asserted-by": "publisher",
"first-page": "773",
"journal-title": "Br J Nutr",
"key": "927_CR38",
"unstructured": "Moludi J, Qaisar SA, Alizadeh M, et al. The relationship between Dietary Inflammatory Index and disease severity and inflammatory status: a case-control study of COVID-19 patients. Br J Nutr. 2022;127:773–81.",
"volume": "127",
"year": "2022"
},
{
"DOI": "10.3233/MNM-211521",
"author": "M Mohajeri",
"doi-asserted-by": "publisher",
"first-page": "219",
"journal-title": "Mediterranean J Nutr Metabolism",
"key": "927_CR39",
"unstructured": "Mohajeri M, Mohajery R, Nemati A, Pourfarzi F. The difference in the dietary inflammatory index, functional food, and antioxidants intake between COVID – 19 patients and healthy persons. Mediterranean J Nutr Metabolism. 2022;15:219–27.",
"volume": "15",
"year": "2022"
},
{
"DOI": "10.1155/2022/5452488",
"author": "D Firoozi",
"doi-asserted-by": "publisher",
"first-page": "5452488",
"journal-title": "Int J Clin Pract",
"key": "927_CR40",
"unstructured": "Firoozi D, Masoumi SJ. The Association between Energy-Adjusted Dietary Inflammatory Index, body composition, and Anthropometric indices in COVID-19-Infected patients: a case-control study in Shiraz, Iran. Int J Clin Pract. 2022;2022:5452488.",
"volume": "2022",
"year": "2022"
},
{
"DOI": "10.3390/ijms232415584",
"doi-asserted-by": "crossref",
"key": "927_CR41",
"unstructured": "Clemente-Suárez VJ, Bustamante-Sanchez Á. Inflammation in COVID-19 and the effects of non-pharmacological interventions during the pandemic: a review. Int J Mol Sci. 2022;23."
},
{
"DOI": "10.1016/S2213-2600(20)30079-5",
"author": "X Yang",
"doi-asserted-by": "publisher",
"first-page": "475",
"journal-title": "Lancet Respiratory Med",
"key": "927_CR42",
"unstructured": "Yang X, Yu Y, Xu J, et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respiratory Med. 2020;8:475–81.",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1146/annurev-med-042220-012417",
"author": "Y Wang",
"doi-asserted-by": "publisher",
"first-page": "65",
"journal-title": "Annu Rev Med",
"key": "927_CR43",
"unstructured": "Wang Y, Perlman S. COVID-19: Inflammatory Profile. Annu Rev Med. 2022;73:65–80.",
"volume": "73",
"year": "2022"
},
{
"DOI": "10.1111/imm.13262",
"author": "SM Toor",
"doi-asserted-by": "publisher",
"first-page": "30",
"journal-title": "Immunology",
"key": "927_CR44",
"unstructured": "Toor SM, Saleh R. T-cell responses and therapies against SARS-CoV-2 infection. Immunology. 2021;162:30–43.",
"volume": "162",
"year": "2021"
},
{
"DOI": "10.3390/ijerph19159079",
"doi-asserted-by": "crossref",
"key": "927_CR45",
"unstructured": "Montero López MDP, Mora Urda AI. Changes in eating behaviors during the COVID-19 Lockdown and the impact on the potential Inflammatory effects of Diet. Int J Environ Res Public Health. 2022;19."
}
],
"reference-count": 45,
"references-count": 45,
"relation": {},
"resource": {
"primary": {
"URL": "https://nutritionj.biomedcentral.com/articles/10.1186/s12937-024-00927-3"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Nutrition and Dietetics",
"Medicine (miscellaneous)"
],
"subtitle": [],
"title": "Association of dietary inflammatory index and the SARS-CoV-2 infection incidence, severity and mortality of COVID-19: a systematic review and dose-response meta-analysis",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "23"
}
