Running behavior and symptoms of respiratory tract infection during the COVID-19 pandemic
et al., Journal of Science and Medicine in Sport, doi:10.1016/j.jsams.2020.10.009, Oct 2020
Exercise for COVID-19
9th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 68 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
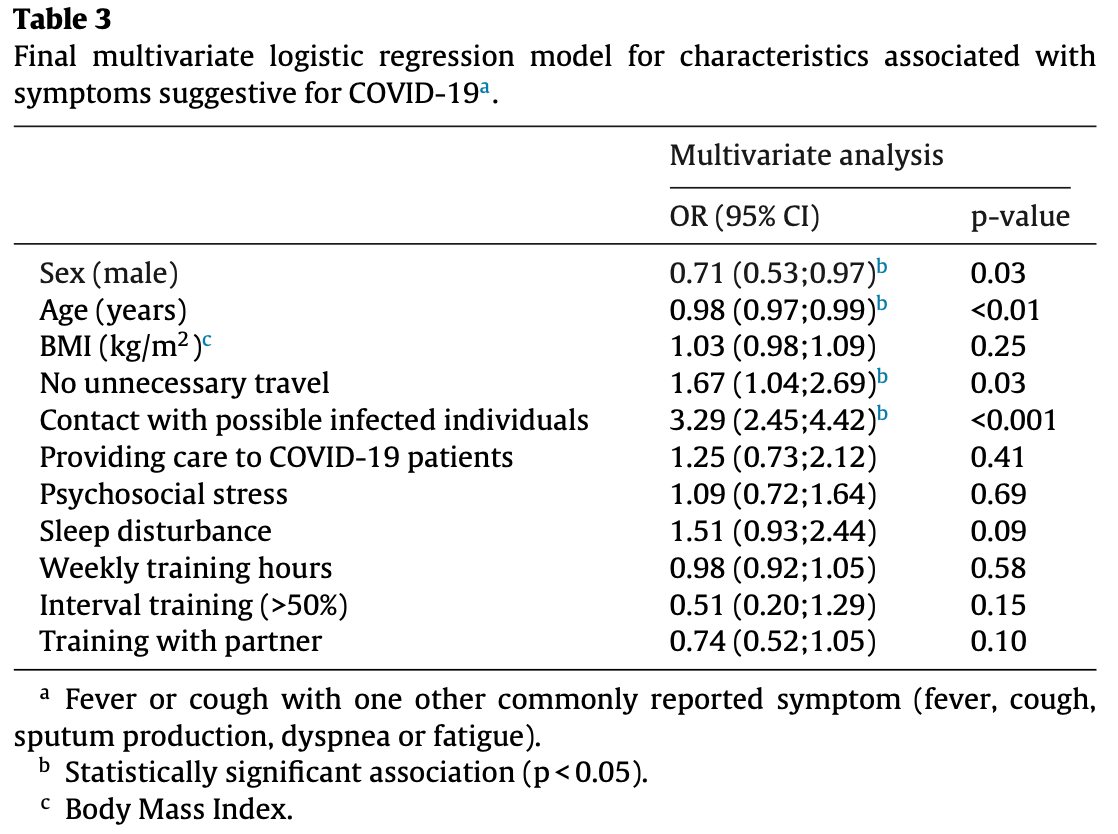
Analysis of 2,586 participants of a running injury prevention RCT in the Netherlands, showing lower risk of COVID-19 symptoms with interval training and increased training hours, without statistical significance.
Study covers exercise and sleep.
Cloosterman et al., 21 Oct 2020, retrospective, Netherlands, peer-reviewed, 4 authors.
Contact: k.cloosterman@erasmusmc.nl.
Running behavior and symptoms of respiratory tract infection during the COVID-19 pandemic
Journal of Science and Medicine in Sport, doi:10.1016/j.jsams.2020.10.009
Objectives: To explore changes in running behavior due to the Coronavirus Disease 2019 (COVID-19) pandemic, assess presence of symptoms suggestive for COVID-19 and identify whether there is an association between running behavior and COVID-19. Design: Prospective cohort study. Methods: For this study we used a cohort of runners participating in an ongoing randomized controlled trial on running injury prevention among recreational runners. At baseline, demographic and training variables were collected. Seven weeks after starting the lockdown, information on running behavior (interval training, training with partner and physical distancing during training) and running habits (training frequency, duration, distance and speed) were obtained. Furthermore, healthcare utilization and symptoms suggestive for COVID-19 were assessed. To determine the association between running and symptoms suggestive for COVID-19, univariate and multivariate logistic regression analyses were performed. Results: Of the 2586 included participants, 2427 (93.9%) participants continued running during lockdown with no significant changes in mean weekly training variables. A total of 253 participants (9.8%) experienced symptoms suggestive for COVID-19 and 10 participants tested positive for COVID-19. Two participants were admitted to hospital due to COVID-19 with both one day of admission. Running behavior and running habits were not associated with the onset of symptoms suggestive for COVID-19. Conclusions: The large majority of runners in the Netherlands did not change their running habits during lockdown. No association between running behavior or running habits and onset of symptoms suggestive for COVID-19 was identified. This implicates that running outdoor during lockdown does not negatively affect health of runners.
Research and Development (ZonMW), grant number 50-53600-98-104.
Appendix A. Supplementary data Supplementary material related to this article can be found, in the online version, at doi:https://doi.org/10.1016/j.jsams.2020.10. 009.
References
Ali, COVID-19: are we ready for the second wave?, Disaster Med Public Health Prep
Blocken, Malizia, Van Druenen, Towards aerodynamically equivalent COVID-19 1.5 m social distancing for walking and running
Chen, Mao, Nassis, Coronavirus disease (COVID-19): the need to maintain regular physical activity while taking precautions, J Sport Health Sci
Chen, Zhou, Dong, Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study, Lancet
Fokkema, De Vos, Van Ochten, Preventing running-related injuries using evidence-based online advice: the design of a randomised-controlled trial, BMJ Open Sport Exerc Med
Guan, Ni, Hu, Clinical characteristics of coronavirus disease 2019 in China, N Engl J Med
Huang, Wang, Li, Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, Lancet
Hull, Loosemore, Schwellnus, Respiratory health in athletes: facing the COVID-19 challenge, Lancet Respir Med
Khammassi, Ouerghi, Said, Continuous moderate-intensity but not high-intensity interval training improves immune function biomarkers in healthy young men, J Strength Cond Res
Simpson, Campbell, Gleeson, Can exercise affect immune function to increase susceptibility to infection?, Exerc Immunol Rev
Sjodin, Wilder-Smith, Osman, Only strict quarantine measures can curb the coronavirus disease (COVID-19) outbreak in Italy, Euro Surveill
Veiligheid, Hardloopblessures Blessurecijfers 2014
Walsh, Recommendations to maintain immune health in athletes, Eur J Sport Sci
Wang, Fang, Zhu, Clinical characteristics of non-critically ill patients with novel coronavirus infection (COVID -19) in a Fangcang Hospital, Clin Microbiol Infect
Wang, Hu, Hu, Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China, JAMA
Zhang, Wang, Rauch, Unprecedented disruption of lives and work: health, distress and life satisfaction of working adults in China one month into the COVID-19 outbreak, Psychiatry Res
DOI record:
{
"DOI": "10.1016/j.jsams.2020.10.009",
"ISSN": [
"1440-2440"
],
"URL": "http://dx.doi.org/10.1016/j.jsams.2020.10.009",
"alternative-id": [
"S144024402030788X"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Running behavior and symptoms of respiratory tract infection during the COVID-19 pandemic"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "Journal of Science and Medicine in Sport"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.jsams.2020.10.009"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2020 The Authors. Published by Elsevier Ltd on behalf of Sports Medicine Australia."
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-3926-4025",
"affiliation": [],
"authenticated-orcid": false,
"family": "Cloosterman",
"given": "Kyra L.A.",
"sequence": "first"
},
{
"affiliation": [],
"family": "van Middelkoop",
"given": "Marienke",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-5609-9471",
"affiliation": [],
"authenticated-orcid": false,
"family": "Krastman",
"given": "Patrick",
"sequence": "additional"
},
{
"affiliation": [],
"family": "de Vos",
"given": "Robert-Jan",
"sequence": "additional"
}
],
"container-title": "Journal of Science and Medicine in Sport",
"container-title-short": "Journal of Science and Medicine in Sport",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"jsams.org",
"clinicalkey.jp",
"clinicalkey.com",
"clinicalkey.es",
"clinicalkey.fr",
"clinicalkey.com.au",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2020,
10,
21
]
],
"date-time": "2020-10-21T02:43:47Z",
"timestamp": 1603248227000
},
"deposited": {
"date-parts": [
[
2022,
2,
12
]
],
"date-time": "2022-02-12T11:22:10Z",
"timestamp": 1644664930000
},
"funder": [
{
"DOI": "10.13039/501100001826",
"doi-asserted-by": "publisher",
"name": "ZonMw"
}
],
"indexed": {
"date-parts": [
[
2022,
9,
23
]
],
"date-time": "2022-09-23T19:13:11Z",
"timestamp": 1663960391796
},
"is-referenced-by-count": 3,
"issue": "4",
"issued": {
"date-parts": [
[
2021,
4
]
]
},
"journal-issue": {
"issue": "4",
"published-print": {
"date-parts": [
[
2021,
4
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
4,
1
]
],
"date-time": "2021-04-01T00:00:00Z",
"timestamp": 1617235200000
}
},
{
"URL": "http://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2020,
10,
28
]
],
"date-time": "2020-10-28T00:00:00Z",
"timestamp": 1603843200000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S144024402030788X?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S144024402030788X?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "332-337",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2021,
4
]
]
},
"published-print": {
"date-parts": [
[
2021,
4
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"author": "World Health Organization (WHO)",
"key": "10.1016/j.jsams.2020.10.009_bib0005",
"series-title": "Coronavirus Disease (COVID-19) Pandemic",
"year": "2020"
},
{
"DOI": "10.1016/j.jshs.2020.02.001",
"article-title": "Coronavirus disease (COVID-19): the need to maintain regular physical activity while taking precautions",
"author": "Chen",
"doi-asserted-by": "crossref",
"first-page": "103",
"issue": "2",
"journal-title": "J Sport Health Sci",
"key": "10.1016/j.jsams.2020.10.009_bib0010",
"volume": "9",
"year": "2020"
},
{
"author": "Veiligheid",
"key": "10.1016/j.jsams.2020.10.009_bib0015",
"series-title": "Hardloopblessures Blessurecijfers 2014",
"year": "2016"
},
{
"DOI": "10.1519/JSC.0000000000002737",
"article-title": "Continuous moderate-intensity but not high-intensity interval training improves immune function biomarkers in healthy young men",
"author": "Khammassi",
"doi-asserted-by": "crossref",
"first-page": "249",
"issue": "1",
"journal-title": "J Strength Cond Res",
"key": "10.1016/j.jsams.2020.10.009_bib0020",
"volume": "34",
"year": "2020"
},
{
"DOI": "10.1080/17461391.2018.1449895",
"article-title": "Recommendations to maintain immune health in athletes",
"author": "Walsh",
"doi-asserted-by": "crossref",
"first-page": "820",
"issue": "6",
"journal-title": "Eur J Sport Sci",
"key": "10.1016/j.jsams.2020.10.009_bib0025",
"volume": "18",
"year": "2018"
},
{
"DOI": "10.2807/1560-7917.ES.2020.25.13.2000280",
"article-title": "Only strict quarantine measures can curb the coronavirus disease (COVID-19) outbreak in Italy, 2020",
"author": "Sjodin",
"doi-asserted-by": "crossref",
"issue": "13",
"journal-title": "Euro Surveill",
"key": "10.1016/j.jsams.2020.10.009_bib0030",
"volume": "25",
"year": "2020"
},
{
"key": "10.1016/j.jsams.2020.10.009_bib0035",
"unstructured": "Blocken B., Malizia F., van Druenen T., et al., Towards aerodynamically equivalent COVID-19 1.5 m social distancing for walking and running. Unpublished results. Available at: http://www.urbanphysics.net/COVID19_Aero_Paper.pdf."
},
{
"DOI": "10.1016/S2213-2600(20)30175-2",
"article-title": "Respiratory health in athletes: facing the COVID-19 challenge",
"author": "Hull",
"doi-asserted-by": "crossref",
"first-page": "557",
"issue": "6",
"journal-title": "Lancet Respir Med",
"key": "10.1016/j.jsams.2020.10.009_bib0040",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/j.psychres.2020.112958",
"article-title": "Unprecedented disruption of lives and work: health, distress and life satisfaction of working adults in China one month into the COVID-19 outbreak",
"author": "Zhang",
"doi-asserted-by": "crossref",
"first-page": "112958",
"journal-title": "Psychiatry Res",
"key": "10.1016/j.jsams.2020.10.009_bib0045",
"volume": "288",
"year": "2020"
},
{
"DOI": "10.1136/bmjsem-2017-000265",
"article-title": "Preventing running-related injuries using evidence-based online advice: the design of a randomised-controlled trial",
"author": "Fokkema",
"doi-asserted-by": "crossref",
"issue": "1",
"journal-title": "BMJ Open Sport Exerc Med",
"key": "10.1016/j.jsams.2020.10.009_bib0050",
"volume": "3",
"year": "2017"
},
{
"DOI": "10.1001/jama.2020.1585",
"article-title": "Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China",
"author": "Wang",
"doi-asserted-by": "crossref",
"first-page": "1061",
"issue": "11",
"journal-title": "JAMA",
"key": "10.1016/j.jsams.2020.10.009_bib0055",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"article-title": "Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China",
"author": "Huang",
"doi-asserted-by": "crossref",
"first-page": "497",
"issue": "10223",
"journal-title": "Lancet",
"key": "10.1016/j.jsams.2020.10.009_bib0060",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30211-7",
"article-title": "Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study",
"author": "Chen",
"doi-asserted-by": "crossref",
"first-page": "507",
"issue": "10223",
"journal-title": "Lancet",
"key": "10.1016/j.jsams.2020.10.009_bib0065",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1056/NEJMoa2002032",
"article-title": "Clinical characteristics of coronavirus disease 2019 in China",
"author": "Guan",
"doi-asserted-by": "crossref",
"first-page": "1708",
"issue": "18",
"journal-title": "N Engl J Med",
"key": "10.1016/j.jsams.2020.10.009_bib0070",
"volume": "382",
"year": "2020"
},
{
"DOI": "10.1016/j.cmi.2020.03.032",
"article-title": "Clinical characteristics of non-critically ill patients with novel coronavirus infection (COVID -19) in a Fangcang Hospital",
"author": "Wang",
"doi-asserted-by": "crossref",
"first-page": "1063",
"issue": "8",
"journal-title": "Clin Microbiol Infect",
"key": "10.1016/j.jsams.2020.10.009_bib0075",
"volume": "26",
"year": "2020"
},
{
"article-title": "Can exercise affect immune function to increase susceptibility to infection?",
"author": "Simpson",
"first-page": "8",
"journal-title": "Exerc Immunol Rev",
"key": "10.1016/j.jsams.2020.10.009_bib0080",
"volume": "26",
"year": "2020"
},
{
"article-title": "COVID-19: are we ready for the second wave?",
"author": "Ali",
"first-page": "1",
"journal-title": "Disaster Med Public Health Prep",
"key": "10.1016/j.jsams.2020.10.009_bib0085",
"year": "2020"
}
],
"reference-count": 17,
"references-count": 17,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S144024402030788X"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Physical Therapy, Sports Therapy and Rehabilitation",
"Orthopedics and Sports Medicine"
],
"subtitle": [],
"title": "Running behavior and symptoms of respiratory tract infection during the COVID-19 pandemic",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "24"
}
