Metformin is Associated with Reduced COVID-19 Severity in Patients with Prediabetes
et al., medRxiv, doi:10.1101/2022.08.29.22279355, Aug 2022
Metformin for COVID-19
3rd treatment shown to reduce risk in
July 2020, now with p < 0.00000000001 from 111 studies.
Lower risk for mortality, ventilation, ICU, hospitalization, progression, recovery, and viral clearance.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 3,136 patients with prediabetes and 282 with PCOS, showing metformin associated with reduced COVID-19 severity.
Standard of Care (SOC) for COVID-19 in the study country,
the USA, is very poor with very low average efficacy for approved treatments1.
Only expensive, high-profit treatments were approved for early treatment. Low-cost treatments were excluded, reducing the probability of early treatment due to access and cost barriers, and eliminating complementary and synergistic benefits seen with many low-cost treatments.
|
risk of death, 58.6% lower, OR 0.41, p = 0.66, treatment 400, control 2,736, adjusted per study, mortality/hospice, multivariable, prediabeties, RR approximated with OR.
|
|
risk of severe case, 54.1% lower, OR 0.46, p = 0.37, treatment 400, control 2,736, adjusted per study, multivariable, prediabeties, RR approximated with OR.
|
|
risk of progression, 42.4% lower, RR 0.58, p = 0.37, treatment 51 of 400 (12.8%), control 798 of 2,736 (29.2%), NNT 6.1, adjusted per study, odds ratio converted to relative risk, moderate, multivariable, prediabeties.
|
|
risk of progression, 37.0% lower, OR 0.63, p = 0.37, treatment 400, control 2,736, adjusted per study, mild ER, multivariable, prediabeties, RR approximated with OR.
|
|
risk of progression, 40.7% lower, OR 0.59, p = 0.22, treatment 196, control 86, adjusted per study, moderate, multivariable, PCOS, RR approximated with OR.
|
|
risk of progression, 34.5% lower, OR 0.66, p = 0.20, treatment 196, control 86, adjusted per study, mild ER, multivariable, PCOS, RR approximated with OR.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Chan et al., 30 Aug 2022, retrospective, USA, preprint, 15 authors.
Contact: justinreese@lbl.gov.
Metformin is Associated with Reduced COVID-19 Severity in Patients with Prediabetes
doi:10.1101/2022.08.29.22279355
Background: With the continuing COVID-19 pandemic, identifying medications that improve COVID-19 outcomes is crucial. Studies suggest that use of metformin, an oral antihyperglycemic, is associated with reduced COVID-19 severity in individuals with diabetes compared to other antihyperglycemic medications. Some patients without diabetes, including those with polycystic ovary syndrome (PCOS) and prediabetes, are prescribed metformin for off-label use, which provides an opportunity to further investigate the effect of metformin on COVID-19.
Participants: In this observational, retrospective analysis, we leveraged the harmonized electronic health record data from 53 hospitals to construct cohorts of COVID-19 positive, metformin users without diabetes and propensity-weighted control users of levothyroxine (a medication for hypothyroidism that is not known to affect COVID-19 outcome) who had either PCOS (n = 282) or prediabetes (n = 3136). The primary outcome of interest was COVID-19 severity, which was classified as: mild, mild ED (emergency department), moderate, severe, or mortality/hospice.
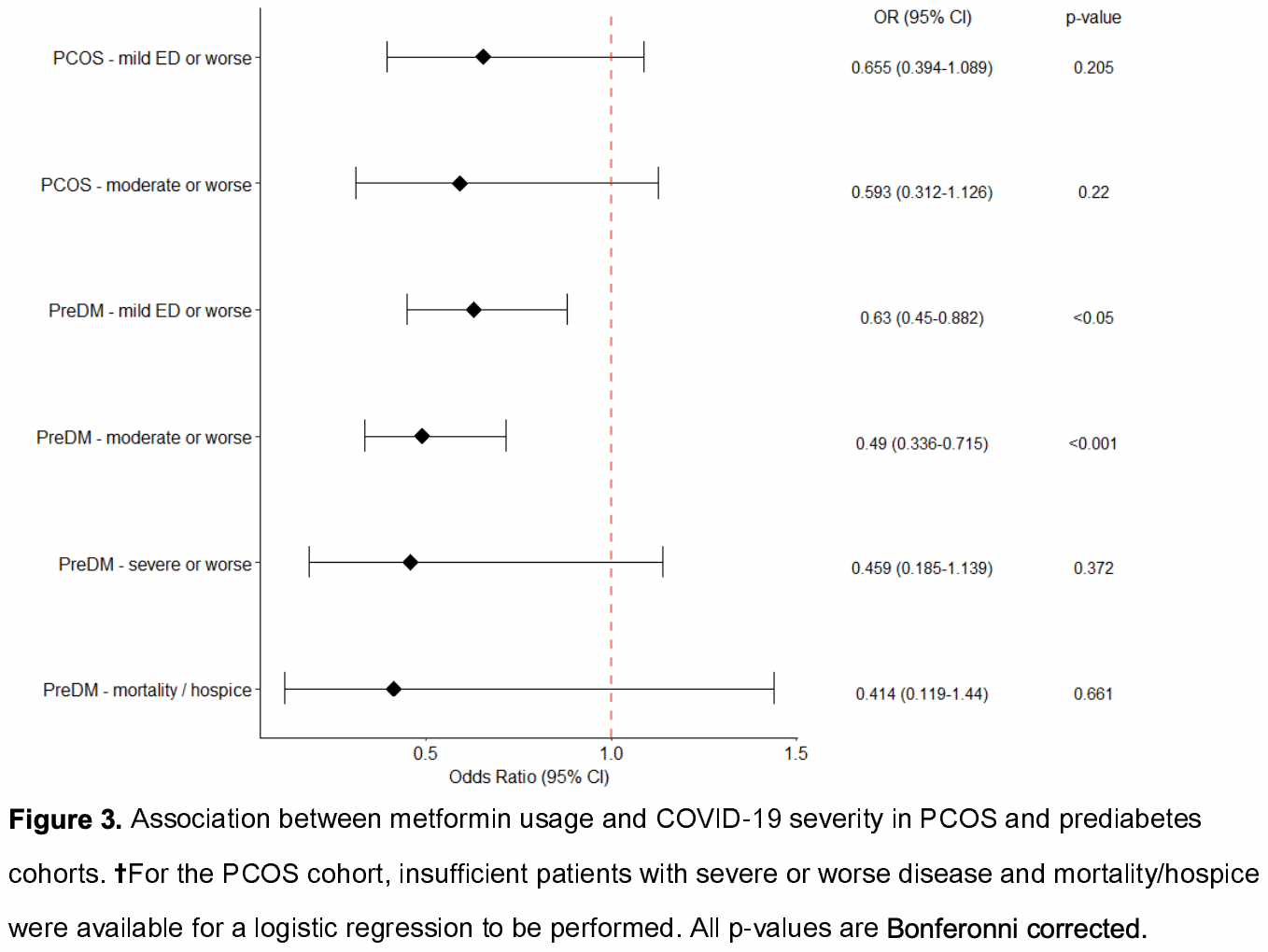
Results: In the prediabetes cohort, metformin use was associated with a lower rate of COVID-19 with severity of mild ED or worse (OR: 0.630, 95% CI 0.450 -0.882, p < 0.05) and a lower rate of COVID-19 with severity of moderate or worse (OR: 0.490, 95% CI 0.336 -0.715, p < 0.001). In for use under a CC0 license.
Conflict of Interest The authors declare no conflicts of interest. Supplementary Figure S2 . Forest plots for the prediabetes cohort. A: Mild, mild ED, and moderate vs severe and worse, B: Mild, mild ED, moderate, and severe vs death with COVID-19 Supplementary Figure S3 . Forest Plots for univariate odds ratios computed to assess the non-collapsibility effect for chronic respiratory disease. According to Schuster et al., 50 noncollapsibility effects on a covariate can be estimated by comparing the OR obtained by univariate LR on the variable and the OR obtained in the multivariate analysis. To check whether the OR for chronic-respiratory disease is affected by the non-collapsibility effect we therefore run an univariate LR for each outcome. The forest plot reports the results obtained when univariate LRs were applied to either drug usage ("on metformin") or chronic respiratory disease; the ORs for drug usage are comparable to those obtained by multivariate LR (Fig. 4a, 4b ) showing the reliability of the estimate. On the other hand, the remarkable difference in the ORs estimated for chronic respiratory disease confirm the non-collapsibility effect for this variable. e , for use under a CC0 license.
References
Adam ; Wilcox, Lee, Graves, Jerrod) Anzalone, Manna et al., Details of contributions available at covid
Azziz, Chen, Polycystic ovary syndrome, Nat Rev Dis Primers
Bailey, Gwilt, Diabetes, Metformin and the Clinical Course of Covid-19: Outcomes, Mechanisms and Suggestions on the Therapeutic Use of Metformin, Front Pharmacol
Batandier, Guigas, Detaille, The ROS production induced by a reverse-electron flux at respiratory-chain complex 1 is hampered by metformin, J Bioenerg Biomembr
Bennett, Moffitt, Hajagos, The National COVID Cohort Collaborative: Clinical Characterization and Early Severity Prediction, doi:10.1101/2021.01.12.21249511
Boelaert, Visser, Taylor, Moran, Léger et al., ENDOCRINOLOGY IN THE TIME OF COVID-19: Management of hyperthyroidism and hypothyroidism, Eur J Endocrinol
Bozdag, Mumusoglu, Zengin, Karabulut, Yildiz, The prevalence and phenotypic features of polycystic ovary syndrome: a systematic review and meta-analysis, Hum Reprod
Bramante, Buse, Tamaritz, Outpatient metformin use is associated with reduced severity of COVID-19 disease in adults with overweight or obesity, J Med Virol
Casiraghi, Wong, Hall, A Methodological Framework for the Comparative Evaluation of Multiple Imputation Methods: Multiple
Charlson, Pompei, Ales, Mackenzie, A new method of classifying prognostic comorbidity in longitudinal studies: development and validation, J Chronic Dis
Chen, Guo, Qiu, Zhang, Deng et al., Immunomodulatory and Antiviral Activity of Metformin and Its Potential Implications in Treating Coronavirus Disease 2019 and Lung Injury, Front Immunol
D'arcy, Stürmer, Lund, The importance and implications of comparator selection in pharmacoepidemiologic research, Curr Epidemiol Rep
Daniel, Zhang, Farewell, Making apples from oranges: Comparing noncollapsible effect estimators and their standard errors after adjustment for different covariate sets, Biom J
De Medeiros, Yamamoto, De Medeiros, Yamamoto, Barbosa, Polycystic ovary syndrome and risks for COVID-19 infection: A comprehensive review, Rev Endocr Metab Disord
Diabetes, Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes-2021, Diabetes Care
Diabetes, Diagnosis and classification of diabetes mellitus, Diabetes Care
Diamanti-Kandarakis, Insulin resistance in PCOS, Endocrine
Dotolo, Marabotti, Facchiano, Tagliaferri, A review on drug repurposing applicable to COVID-19, Brief Bioinform
Dunaif, Segal, Futterweit, Dobrjansky, Profound peripheral insulin resistance, independent of obesity, in polycystic ovary syndrome, Diabetes
Echouffo-Tcheugui, Selvin, Prediabetes and What It Means: The Epidemiological Evidence, Annu Rev Public Health
Eghtedari, Correa, Levothyroxine
Fischer, Eron, Holman, an Oral Antiviral Treatment for COVID-19, doi:10.1101/2021.06.17.21258639
Foretz, Hébrard, Leclerc, Metformin inhibits hepatic gluconeogenesis in mice independently of the LKB1/AMPK pathway via a decrease in hepatic energy state, J Clin Invest
Fox, Applied regression analysis, linear models, and related methods
Fox, Monette, Generalized Collinearity Diagnostics, J Am Stat Assoc
Ghany, Palacio, Dawkins, Metformin is associated with lower hospitalizations, mortality and severe coronavirus infection among elderly medicare minority patients in 8 states in USA, Diabetes Metab Syndr
Haendel, Chute, Bennett, The National COVID Cohort Collaborative (N3C): Rationale, design, infrastructure, and deployment, J Am Med Inform Assoc
Hajjar, Habra, Naing, Metformin: an old drug with new potential, Expert Opin Investig Drugs
Hariyanto, Kurniawan, Metformin use is associated with reduced mortality rate from coronavirus disease 2019 (COVID-19) infection, Obes Med
Hariyanto, Kurniawan, Thyroid disease is associated with severe coronavirus disease 2019 (COVID-19) infection, Diabetes Metab Syndr
Hripcsak, Duke, Shah, Observational Health Data Sciences and Informatics for use under a CC0 license
Kim, Yoo, Choi, The Effects of Previous Thyroid Disease on the Susceptibility to, Morbidity of, and Mortality Due to COVID-19: A Nationwide Cohort Study in South Korea, J Clin Med Res, doi:10.3390/jcm10163522foruseunderaCC0license
Knowler, Fowler, 10-year follow-up of diabetes incidence and weight loss in the Diabetes Prevention Program Outcomes Study, Lancet
Kyritsi, Dimitriadis, Kyrou, Kaltsas, Randeva, PCOS remains a diagnosis of exclusion: a concise review of key endocrinopathies to exclude, Clin Endocrinol
Kyrou, Karteris, Robbins, Chatha, Drenos et al., Polycystic ovary syndrome (PCOS) and COVID-19: an overlooked female patient population at potentially higher risk during the COVID-19 pandemic, BMC Med
Legro, Arslanian, Ehrmann, Diagnosis and treatment of polycystic ovary syndrome: an Endocrine Society clinical practice guideline, J Clin Endocrinol Metab
Li, Little's Test of Missing Completely at Random, Stata J
Maier, Kapsner, Mate, Prokosch, Kraus, Patient Cohort Identification on Time Series Data Using the OMOP Common Data Model, Appl Clin Inform
Mayer, Fast Imputation of Missing Values [R package missRanger version 2
Morales, Laughlin, Bützow, Maheshwari, Baumann et al., Insulin, somatotropic, and luteinizing hormone axes in lean and obese women with polycystic ovary syndrome: common and distinct features, J Clin Endocrinol Metab
Muniyappa, Gubbi, COVID-19 pandemic, coronaviruses, and diabetes mellitus, Am J Physiol Endocrinol Metab
Nagy, Perros, Papini, Katko, Hegedüs, New Formulations of Levothyroxine in the Treatment of Hypothyroidism: Trick or Treat?, Thyroid
Ohdsi, Opportunities for Observational Researchers, Stud Health Technol Inform
Palladino, Tabak, Khunti, Association between pre-diabetes and microvascular and macrovascular disease in newly diagnosed type 2 diabetes, BMJ Open Diabetes Res Care, doi:10.1136/bmjdrc-2019-001061
Permana, Soeriadi, Damara, Soetedjo, The prognostic values of thyroid disorders in predicting COVID-19 composite poor outcomes: A systematic review and meta-analysis, Diabetes Metab Syndr
Pishgar, Greifer, Leyrat, Stuart, MatchThem:: Matching and weighting after multiple imputation, R J
Rubin, Multiple imputation for nonresponse in surveys
Samuel, Varghese, Büsselberg, Therapeutic Potential of Metformin in COVID-19: Reasoning for Its Protective Role, Trends Microbiol
Schuster, Twisk, Riet, Heymans, Rijnhart, Noncollapsibility and its role in quantifying confounding bias in logistic regression, BMC Med Res Methodol
Sharma, Ray, Sadasivam, Metformin in COVID-19: A possible role beyond diabetes, Diabetes Res Clin Pract
Singh, Parida, Lingaraju, Kesavan, Kumar et al., Drug repurposing approach to fight COVID-19, Pharmacol Rep
Sosibo, Khathi, Pre-diabetes and COVID-19, could we be missing the silent killer?, Exp Biol Med
Stekhoven, Bühlmann, MissForest--non-parametric missing value imputation for mixed-type data, Bioinformatics
Subramanian, Anand, Adderley, Increased COVID-19 infections in women with polycystic ovary syndrome: a population-based study, Eur J Endocrinol
Tabák, Herder, Rathmann, Brunner, Kivimäki, Prediabetes: a high-risk state for diabetes development, Lancet
Van Buuren, Flexible Imputation of Missing Data
Vanderweele, Ding, Sensitivity Analysis in Observational Research: Introducing the E-Value, Ann Intern Med
Vitek, Alur, Hoeger, Off-label drug use in the treatment of polycystic ovary syndrome, Fertil Steril
Voss, Makadia, Matcho, Feasibility and utility of applications of the common data model to multiple, disparate observational health databases, J Am Med Inform Assoc
Zhong, Tang, Ye, Dong, The immunology of COVID-19: is immune modulation an option for treatment?, Lancet Rheumatol
Zhou, Myers, Li, Role of AMP-activated protein kinase in mechanism of metformin action, J Clin Invest
DOI record:
{
"DOI": "10.1101/2022.08.29.22279355",
"URL": "http://dx.doi.org/10.1101/2022.08.29.22279355",
"abstract": "<jats:title>Abstract</jats:title><jats:sec><jats:title>Background</jats:title><jats:p>With the continuing COVID-19 pandemic, identifying medications that improve COVID-19 outcomes is crucial. Studies suggest that use of metformin, an oral antihyperglycemic, is associated with reduced COVID-19 severity in individuals with diabetes compared to other antihyperglycemic medications. Some patients without diabetes, including those with polycystic ovary syndrome (PCOS) and prediabetes, are prescribed metformin for off-label use, which provides an opportunity to further investigate the effect of metformin on COVID-19.</jats:p></jats:sec><jats:sec><jats:title>Participants</jats:title><jats:p>In this observational, retrospective analysis, we leveraged the harmonized electronic health record data from 53 hospitals to construct cohorts of COVID-19 positive, metformin users without diabetes and propensity-weighted control users of levothyroxine (a medication for hypothyroidism that is not known to affect COVID-19 outcome) who had either PCOS (n = 282) or prediabetes (n = 3136). The primary outcome of interest was COVID-19 severity, which was classified as: mild, mild ED (emergency department), moderate, severe, or mortality/hospice.</jats:p></jats:sec><jats:sec><jats:title>Results</jats:title><jats:p>In the prediabetes cohort, metformin use was associated with a lower rate of COVID-19 with severity of mild ED or worse (OR: 0.630, 95% CI 0.450 - 0.882, p < 0.05) and a lower rate of COVID-19 with severity of moderate or worse (OR: 0.490, 95% CI 0.336 - 0.715, p < 0.001). In patients with PCOS, we found no significant association between metformin use and COVID-19 severity, although the number of patients was relatively small.</jats:p></jats:sec><jats:sec><jats:title>Conclusions</jats:title><jats:p>Metformin was associated with less severe COVID-19 in patients with prediabetes, as seen in previous studies of patients with diabetes. This is an important finding, since prediabetes affects between 19 and 38% of the US population, and COVID-19 is an ongoing public health emergency. Further observational and prospective studies will clarify the relationship between metformin and COVID-19 severity in patients with prediabetes, and whether metformin usage may reduce COVID-19 severity.</jats:p></jats:sec>",
"accepted": {
"date-parts": [
[
2022,
8,
30
]
]
},
"author": [
{
"ORCID": "http://orcid.org/0000-0002-7463-6306",
"affiliation": [],
"authenticated-orcid": false,
"family": "Chan",
"given": "Lauren E.",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0003-2024-7572",
"affiliation": [],
"authenticated-orcid": false,
"family": "Casiraghi",
"given": "Elena",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-0450-7074",
"affiliation": [],
"authenticated-orcid": false,
"family": "Laraway",
"given": "Bryan",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-4422-1708",
"affiliation": [],
"authenticated-orcid": false,
"family": "Coleman",
"given": "Ben",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-4557-5492",
"affiliation": [],
"authenticated-orcid": false,
"family": "Blau",
"given": "Hannah",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-6884-7748",
"affiliation": [],
"authenticated-orcid": false,
"family": "Zaman",
"given": "Adnin",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-6315-3707",
"affiliation": [],
"authenticated-orcid": false,
"family": "Harris",
"given": "Nomi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Wilkins",
"given": "Kenneth",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Gargano",
"given": "Michael",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-5694-3919",
"affiliation": [],
"authenticated-orcid": false,
"family": "Valentini",
"given": "Giorgio",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-4616-1171",
"affiliation": [],
"authenticated-orcid": false,
"family": "Sahner",
"given": "David",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-9114-8737",
"affiliation": [],
"authenticated-orcid": false,
"family": "Haendel",
"given": "Melissa",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-0736-9199",
"affiliation": [],
"authenticated-orcid": false,
"family": "Robinson",
"given": "Peter N.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-5858-2080",
"affiliation": [],
"authenticated-orcid": false,
"family": "Bramante",
"given": "Carolyn",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-2170-2250",
"affiliation": [],
"authenticated-orcid": false,
"family": "Reese",
"given": "Justin",
"sequence": "additional"
}
],
"container-title": [],
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2022,
9,
1
]
],
"date-time": "2022-09-01T19:40:29Z",
"timestamp": 1662061229000
},
"deposited": {
"date-parts": [
[
2022,
9,
1
]
],
"date-time": "2022-09-01T19:41:10Z",
"timestamp": 1662061270000
},
"group-title": "Infectious Diseases (except HIV/AIDS)",
"indexed": {
"date-parts": [
[
2022,
9,
2
]
],
"date-time": "2022-09-02T04:10:07Z",
"timestamp": 1662091807820
},
"institution": [
{
"name": "medRxiv"
}
],
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2022,
8,
30
]
]
},
"link": [
{
"URL": "https://syndication.highwire.org/content/doi/10.1101/2022.08.29.22279355",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "246",
"original-title": [],
"posted": {
"date-parts": [
[
2022,
8,
30
]
]
},
"prefix": "10.1101",
"published": {
"date-parts": [
[
2022,
8,
30
]
]
},
"publisher": "Cold Spring Harbor Laboratory",
"reference": [
{
"DOI": "10.1101/2021.06.17.21258639",
"doi-asserted-by": "crossref",
"key": "2022090112402186000_2022.08.29.22279355v1.1",
"unstructured": "Fischer W , Eron JJ , Holman W , et al. Molnupiravir, an Oral Antiviral Treatment for COVID-19. medRxiv [Internet] 2021;Available from: http://dx.doi.org/10.1101/2021.06.17.21258639"
},
{
"DOI": "10.1016/S2665-9913(20)30120-X",
"article-title": "The immunology of COVID-19: is immune modulation an option for treatment?",
"doi-asserted-by": "crossref",
"first-page": "e428",
"issue": "7",
"journal-title": "Lancet Rheumatol",
"key": "2022090112402186000_2022.08.29.22279355v1.2",
"volume": "2",
"year": "2020"
},
{
"DOI": "10.1007/s43440-020-00155-6",
"article-title": "Drug repurposing approach to fight COVID-19",
"doi-asserted-by": "crossref",
"first-page": "1479",
"issue": "6",
"journal-title": "Pharmacol Rep",
"key": "2022090112402186000_2022.08.29.22279355v1.3",
"volume": "72",
"year": "2020"
},
{
"DOI": "10.1093/bib/bbaa288",
"article-title": "A review on drug repurposing applicable to COVID-19",
"doi-asserted-by": "crossref",
"first-page": "726",
"issue": "2",
"journal-title": "Brief Bioinform",
"key": "2022090112402186000_2022.08.29.22279355v1.4",
"volume": "22",
"year": "2021"
},
{
"DOI": "10.1016/j.dsx.2021.02.022",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.5"
},
{
"DOI": "10.1002/jmv.26873",
"article-title": "Outpatient metformin use is associated with reduced severity of COVID-19 disease in adults with overweight or obesity",
"doi-asserted-by": "crossref",
"first-page": "4273",
"issue": "7",
"journal-title": "J Med Virol",
"key": "2022090112402186000_2022.08.29.22279355v1.6",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.3389/fphar.2022.784459",
"article-title": "Diabetes, Metformin and the Clinical Course of Covid-19: Outcomes, Mechanisms and Suggestions on the Therapeutic Use of Metformin",
"doi-asserted-by": "crossref",
"first-page": "784459",
"journal-title": "Front Pharmacol",
"key": "2022090112402186000_2022.08.29.22279355v1.7",
"volume": "13",
"year": "2022"
},
{
"DOI": "10.3389/fimmu.2020.02056",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.8"
},
{
"DOI": "10.1517/13543784.2013.833604",
"article-title": "Metformin: an old drug with new potential",
"doi-asserted-by": "crossref",
"first-page": "1511",
"issue": "12",
"journal-title": "Expert Opin Investig Drugs",
"key": "2022090112402186000_2022.08.29.22279355v1.9",
"volume": "22",
"year": "2013"
},
{
"DOI": "10.1172/JCI200113505",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.10"
},
{
"DOI": "10.1172/JCI40671",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.11"
},
{
"DOI": "10.1007/s10863-006-9003-8",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.12"
},
{
"DOI": "10.1016/j.tim.2021.03.004",
"article-title": "Therapeutic Potential of Metformin in COVID-19: Reasoning for Its Protective Role",
"doi-asserted-by": "crossref",
"first-page": "894",
"issue": "10",
"journal-title": "Trends Microbiol",
"key": "2022090112402186000_2022.08.29.22279355v1.13",
"volume": "29",
"year": "2021"
},
{
"DOI": "10.1016/j.diabres.2020.108183",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.14"
},
{
"DOI": "10.1152/ajpendo.00124.2020",
"article-title": "COVID-19 pandemic, coronaviruses, and diabetes mellitus",
"doi-asserted-by": "crossref",
"first-page": "E736",
"issue": "5",
"journal-title": "Am J Physiol Endocrinol Metab",
"key": "2022090112402186000_2022.08.29.22279355v1.15",
"volume": "318",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(12)60283-9",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.16"
},
{
"DOI": "10.2337/dc21-S002",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.17"
},
{
"DOI": "10.1146/annurev-publhealth-090419-102644",
"article-title": "Prediabetes and What It Means: The Epidemiological Evidence",
"doi-asserted-by": "crossref",
"first-page": "59",
"journal-title": "Annu Rev Public Health",
"key": "2022090112402186000_2022.08.29.22279355v1.18",
"volume": "42",
"year": "2021"
},
{
"DOI": "10.1016/S0140-6736(09)61457-4",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.19"
},
{
"DOI": "10.1038/nrdp.2016.57",
"article-title": "Polycystic ovary syndrome",
"doi-asserted-by": "crossref",
"first-page": "16057",
"journal-title": "Nat Rev Dis Primers",
"key": "2022090112402186000_2022.08.29.22279355v1.20",
"volume": "2",
"year": "2016"
},
{
"DOI": "10.1093/humrep/dew218",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.21"
},
{
"DOI": "10.1111/cen.13245",
"article-title": "PCOS remains a diagnosis of exclusion: a concise review of key endocrinopathies to exclude",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "Clin Endocrinol",
"key": "2022090112402186000_2022.08.29.22279355v1.22",
"volume": "86",
"year": "2017"
},
{
"DOI": "10.1016/j.fertnstert.2015.01.019",
"article-title": "Off-label drug use in the treatment of polycystic ovary syndrome",
"doi-asserted-by": "crossref",
"first-page": "605",
"issue": "3",
"journal-title": "Fertil Steril",
"key": "2022090112402186000_2022.08.29.22279355v1.23",
"volume": "103",
"year": "2015"
},
{
"DOI": "10.1385/ENDO:30:1:13",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.24"
},
{
"DOI": "10.2337/diab.38.9.1165",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.25"
},
{
"DOI": "10.1210/jc.81.8.2854",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.26"
},
{
"DOI": "10.1210/jc.2013-2350",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.27"
},
{
"DOI": "10.1093/jamia/ocu023",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.28"
},
{
"DOI": "10.1093/jamia/ocaa196",
"article-title": "The National COVID Cohort Collaborative (N3C): Rationale, design, infrastructure, and deployment",
"doi-asserted-by": "crossref",
"first-page": "427",
"issue": "3",
"journal-title": "J Am Med Inform Assoc",
"key": "2022090112402186000_2022.08.29.22279355v1.29",
"volume": "28",
"year": "2021"
},
{
"DOI": "10.1101/2021.01.12.21249511",
"doi-asserted-by": "crossref",
"key": "2022090112402186000_2022.08.29.22279355v1.30",
"unstructured": "Bennett TD , Moffitt RA , Hajagos JG , et al. The National COVID Cohort Collaborative: Clinical Characterization and Early Severity Prediction. medRxiv [Internet] 2021;Available from: http://dx.doi.org/10.1101/2021.01.12.21249511"
},
{
"article-title": "Observational Health Data Sciences and Informatics (OHDSI): Opportunities for Observational Researchers",
"first-page": "574",
"journal-title": "Stud Health Technol Inform",
"key": "2022090112402186000_2022.08.29.22279355v1.31",
"volume": "216",
"year": "2015"
},
{
"DOI": "10.2337/dc10-S062",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.32"
},
{
"DOI": "10.1055/s-0040-1721481",
"article-title": "Patient Cohort Identification on Time Series Data Using the OMOP Common Data Model",
"doi-asserted-by": "crossref",
"first-page": "57",
"issue": "1",
"journal-title": "Appl Clin Inform",
"key": "2022090112402186000_2022.08.29.22279355v1.33",
"volume": "12",
"year": "2021"
},
{
"key": "2022090112402186000_2022.08.29.22279355v1.34",
"unstructured": "Fox J. Applied regression analysis, linear models, and related methods. 1997;597. Available from: https://psycnet.apa.org/fulltext/1997-08857-000.pdf"
},
{
"DOI": "10.2307/2290467",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.35"
},
{
"DOI": "10.1016/0021-9681(87)90171-8",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.36"
},
{
"DOI": "10.1093/bioinformatics/btr597",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.37"
},
{
"key": "2022090112402186000_2022.08.29.22279355v1.38",
"unstructured": "Mayer M. Fast Imputation of Missing Values [R package missRanger version 2.1.3]. 2021 [cited 2022 Jun 14];Available from: https://CRAN.R-project.org/package=missRanger"
},
{
"DOI": "10.1201/9780429492259",
"doi-asserted-by": "crossref",
"key": "2022090112402186000_2022.08.29.22279355v1.39",
"unstructured": "van Buuren S. Flexible Imputation of Missing Data, Second Edition. CRC Press; 2018."
},
{
"key": "2022090112402186000_2022.08.29.22279355v1.40",
"unstructured": "Casiraghi E , Wong R , Hall M , et al. A Methodological Framework for the Comparative Evaluation of Multiple Imputation Methods: Multiple Imputation of Race, Ethnicity and Body Mass Index in the U.S. National COVID Cohort Collaborative [Internet]. arXiv [cs.AI]. 2022;Available from: http://arxiv.org/abs/2206.06444"
},
{
"DOI": "10.32614/RJ-2021-073",
"article-title": "MatchThem:: Matching and weighting after multiple imputation",
"doi-asserted-by": "crossref",
"first-page": "228",
"issue": "2",
"journal-title": "R J",
"key": "2022090112402186000_2022.08.29.22279355v1.41",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1002/9780470316696",
"doi-asserted-by": "crossref",
"key": "2022090112402186000_2022.08.29.22279355v1.42",
"unstructured": "Rubin DB . Multiple imputation for nonresponse in surveys. New York: Wiley; 1987."
},
{
"key": "2022090112402186000_2022.08.29.22279355v1.43",
"unstructured": "The R Stats Package [Internet]. [cited 2022 Jun 14];Available from: https://stat.ethz.ch/R-manual/R-devel/library/stats/html/00Index.html"
},
{
"DOI": "10.7326/M16-2607",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.44"
},
{
"DOI": "10.1177/1536867X1301300407",
"article-title": "Little’s Test of Missing Completely at Random",
"doi-asserted-by": "crossref",
"first-page": "795",
"issue": "4",
"journal-title": "Stata J",
"key": "2022090112402186000_2022.08.29.22279355v1.45",
"volume": "13",
"year": "2013"
},
{
"DOI": "10.1016/S1473-3099(20)30483-7",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.46"
},
{
"DOI": "10.1089/thy.2020.0515",
"article-title": "New Formulations of Levothyroxine in the Treatment of Hypothyroidism: Trick or Treat?",
"doi-asserted-by": "crossref",
"first-page": "193",
"issue": "2",
"journal-title": "Thyroid",
"key": "2022090112402186000_2022.08.29.22279355v1.47",
"volume": "31",
"year": "2021"
},
{
"DOI": "10.1007/s40471-018-0155-y",
"article-title": "The importance and implications of comparator selection in pharmacoepidemiologic research",
"doi-asserted-by": "crossref",
"first-page": "272",
"issue": "3",
"journal-title": "Curr Epidemiol Rep",
"key": "2022090112402186000_2022.08.29.22279355v1.48",
"volume": "5",
"year": "2018"
},
{
"DOI": "10.1002/bimj.201900297",
"article-title": "Making apples from oranges: Comparing noncollapsible effect estimators and their standard errors after adjustment for different covariate sets",
"doi-asserted-by": "crossref",
"first-page": "528",
"issue": "3",
"journal-title": "Biom J",
"key": "2022090112402186000_2022.08.29.22279355v1.49",
"volume": "63",
"year": "2021"
},
{
"DOI": "10.1186/s12874-021-01316-8",
"article-title": "Noncollapsibility and its role in quantifying confounding bias in logistic regression",
"doi-asserted-by": "crossref",
"first-page": "136",
"issue": "1",
"journal-title": "BMC Med Res Methodol",
"key": "2022090112402186000_2022.08.29.22279355v1.50",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.1016/j.obmed.2020.100290",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.51"
},
{
"DOI": "10.1186/s12916-020-01697-5",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.52"
},
{
"DOI": "10.1007/s11154-022-09715-y",
"article-title": "Polycystic ovary syndrome and risks for COVID-19 infection: A comprehensive review",
"doi-asserted-by": "crossref",
"first-page": "251",
"issue": "2",
"journal-title": "Rev Endocr Metab Disord",
"key": "2022090112402186000_2022.08.29.22279355v1.53",
"volume": "23",
"year": "2022"
},
{
"DOI": "10.1530/EJE-20-1163",
"doi-asserted-by": "publisher",
"key": "2022090112402186000_2022.08.29.22279355v1.54"
},
{
"DOI": "10.1177/1535370220973451",
"article-title": "Pre-diabetes and COVID-19, could we be missing the silent killer?",
"doi-asserted-by": "crossref",
"first-page": "369",
"issue": "4",
"journal-title": "Exp Biol Med",
"key": "2022090112402186000_2022.08.29.22279355v1.55",
"volume": "246",
"year": "2021"
},
{
"DOI": "10.1136/bmjdrc-2019-001061",
"doi-asserted-by": "crossref",
"key": "2022090112402186000_2022.08.29.22279355v1.56",
"unstructured": "Palladino R , Tabak AG , Khunti K , et al. Association between pre-diabetes and microvascular and macrovascular disease in newly diagnosed type 2 diabetes. BMJ Open Diabetes Res Care [Internet] 2020;8(1). Available from: http://dx.doi.org/10.1136/bmjdrc-2019-001061"
},
{
"key": "2022090112402186000_2022.08.29.22279355v1.57",
"unstructured": "Eghtedari B , Correa R. Levothyroxine. StatPearls Publishing; 2021."
},
{
"DOI": "10.1016/j.dsx.2020.07.044",
"article-title": "Thyroid disease is associated with severe coronavirus disease 2019 (COVID-19) infection",
"doi-asserted-by": "crossref",
"first-page": "1429",
"issue": "5",
"journal-title": "Diabetes Metab Syndr",
"key": "2022090112402186000_2022.08.29.22279355v1.58",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2022.102464",
"article-title": "The prognostic values of thyroid disorders in predicting COVID-19 composite poor outcomes: A systematic review and meta-analysis",
"doi-asserted-by": "crossref",
"first-page": "102464",
"issue": "5",
"journal-title": "Diabetes Metab Syndr",
"key": "2022090112402186000_2022.08.29.22279355v1.59",
"volume": "16",
"year": "2022"
},
{
"DOI": "10.1530/EJE-20-0445",
"article-title": "ENDOCRINOLOGY IN THE TIME OF COVID-19: Management of hyperthyroidism and hypothyroidism",
"doi-asserted-by": "crossref",
"first-page": "G33",
"issue": "1",
"journal-title": "Eur J Endocrinol",
"key": "2022090112402186000_2022.08.29.22279355v1.60",
"volume": "183",
"year": "2020"
},
{
"DOI": "10.3390/jcm10163522",
"doi-asserted-by": "crossref",
"key": "2022090112402186000_2022.08.29.22279355v1.61",
"unstructured": "Kim S-Y , Yoo D-M , Min C-Y , Choi H-G. The Effects of Previous Thyroid Disease on the Susceptibility to, Morbidity of, and Mortality Due to COVID-19: A Nationwide Cohort Study in South Korea. J Clin Med Res [Internet] 2021;10(16). Available from: http://dx.doi.org/10.3390/jcm10163522"
}
],
"reference-count": 61,
"references-count": 61,
"relation": {},
"resource": {
"primary": {
"URL": "http://medrxiv.org/lookup/doi/10.1101/2022.08.29.22279355"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subtitle": [],
"subtype": "preprint",
"title": "Metformin is Associated with Reduced COVID-19 Severity in Patients with Prediabetes",
"type": "posted-content"
}
