Hydroxychloroquine reduces COVID-19 risk: real-time meta analysis of 424 studies (c19hcq hcqmeta)
, Nov 2025
HCQ for COVID-19
1st treatment shown to reduce risk in
March 2020, now with p < 0.00000000001 from 424 studies, used in 59 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,300+ studies for
210+ treatments. c19early.org
|
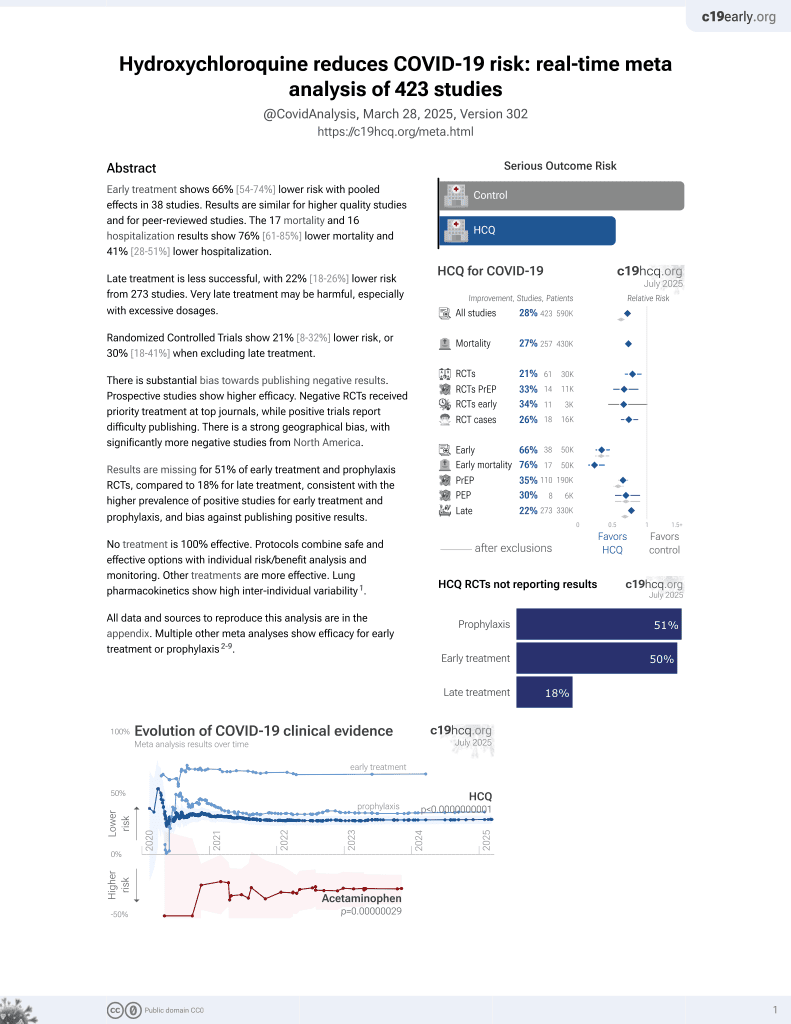
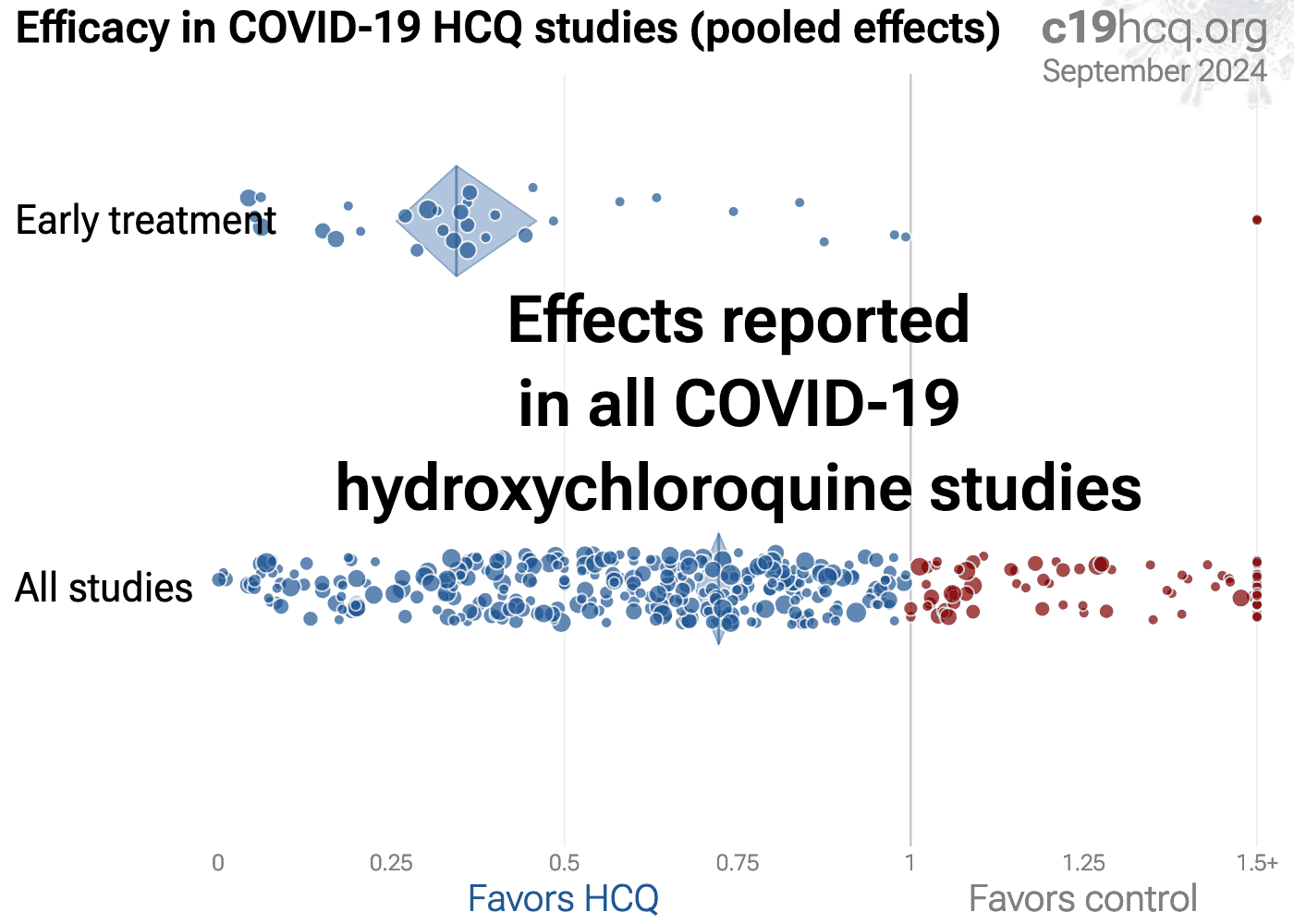
Early treatment shows 66% [54‑74%] lower risk with pooled effects in 38 studies. Results are similar for higher quality studies and for peer-reviewed studies. The 17 mortality and 16 hospitalization results show 76% [61‑85%] lower mortality and 41% [28‑51%] lower hospitalization.
Late treatment is less successful, with 22% [18‑26%] lower risk from 274 studies. Very late treatment may be harmful, especially with excessive dosages.
Randomized Controlled Trials show 20% [8‑32%] lower risk, or 30% [18‑41%] when excluding late treatment.
Control HCQ
There is substantial bias towards publishing negative results. Prospective studies show higher efficacy. Negative RCTs received priority treatment at top journals, while positive trials report difficulty publishing. There is a strong geographical bias, with significantly more negative studies from North America.
Results are missing for 51% of early treatment and prophylaxis RCTs, compared to 17% for late treatment, consistent with the higher prevalence of positive studies for early treatment and prophylaxis, and bias against publishing positive results.
No treatment is 100% effective. Protocols combine safe and effective options with individual risk/benefit analysis and monitoring. Other treatments are more effective. Lung pharmacokinetics show high inter-individual variability1.
All data and sources to reproduce this analysis are in the appendix.
Multiple other meta analyses show efficacy for early treatment or prophylaxis2-9.
9 meta analyses show significant improvements with hydroxychloroquine for mortality1-4,
hospitalization1,
recovery5,
combined death/hospitalization/cases6,
cases7,8, and
viral clearance9.
1.
Landsteiner de Sampaio Amêndola et al., COVID-19 Infection in Rheumatic Patients on Chronic Antimalarial Drugs: A Systematic Review and Meta-Analysis, Journal of Clinical Medicine, doi:10.3390/jcm11226865.
2.
Risch, H., Early Outpatient Treatment of Symptomatic, High-Risk Covid-19 Patients that Should be Ramped-Up Immediately as Key to the Pandemic Crisis, American Journal of Epidemiology, kwaa093, 27 May 2020, doi:10.1093/aje/kwaa093.
3.
Risch (B), H., Response to: “Early Outpatient Treatment of Symptomatic, High-Risk Covid-19 Patients” and “Re: Early Outpatient Treatment of Symptomatic, High-Risk Covid-19 Patients that Should be Ramped-Up Immediately as Key to the Pandemic Crisis”, American Journal of Epidemiology, July 20, 2020, doi:10.1093/aje/kwaa152.
4.
Stricker et al., Hydroxychloroquine Pre-Exposure Prophylaxis for COVID-19 in Healthcare Workers from India: A Meta-Analysis, Journal of Infection and Public Health, doi:10.1016/j.jiph.2021.08.001.
5.
Prodromos et al., Hydroxychloroquine is effective, and consistently so used early, for Covid-19: A systematic review, New Microbes and New Infections, doi:10.1016/j.nmni.2020.100776.
6.
Ladapo et al., Randomized Controlled Trials of Early Ambulatory Hydroxychloroquine in the Prevention of COVID-19 Infection, Hospitalization, and Death: Meta-Analysis, medRxiv, doi:10.1101/2020.09.30.20204693.
7.
García-Albéniz et al., Systematic review and meta-analysis of randomized trials of hydroxychloroquine for the prevention of COVID-19, European Journal of Epidemiology, doi:10.1007/s10654-022-00891-4.
