Efficacy of Colchicine and Budesonide in Improvement Outcomes of Patients with Coronavirus Infection 2019 in Damascus, Syria: A Randomized Control Trial
et al., Interdisciplinary Perspectives on Infectious Diseases, doi:10.1155/2021/2129006, Dec 2021
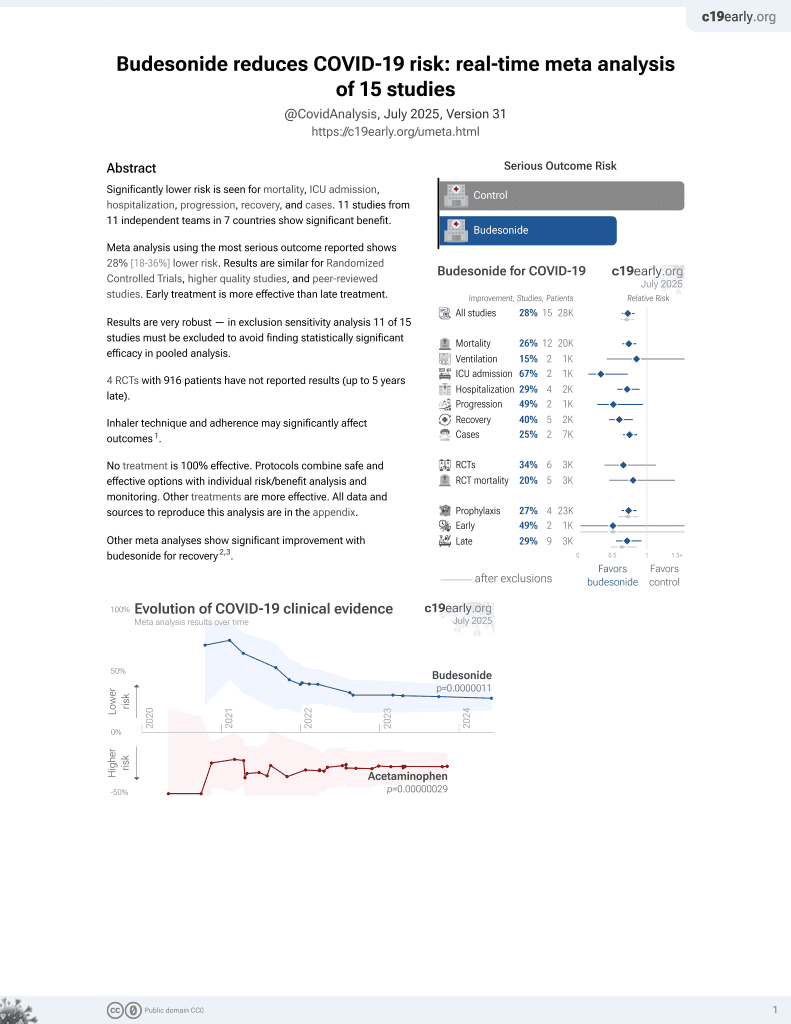
Budesonide for COVID-19
27th treatment shown to reduce risk in
September 2021, now with p = 0.000003 from 15 studies, recognized in 10 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
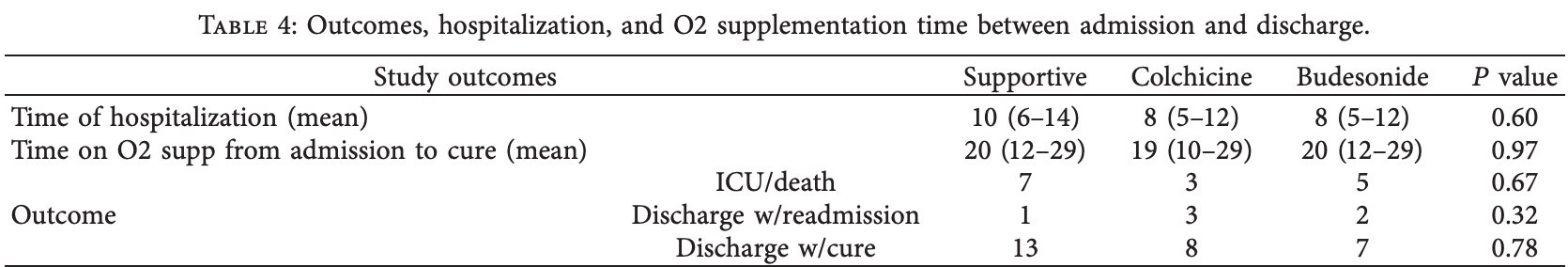
Small RCT 49 severe condition hospitalized patients in Syria, showing lower mortality with colchicine and shorter hospitalization time with both colchicine and budesonide (all of these are not statistically significant).
Study covers colchicine and budesonide.
|
risk of death, 7.1% higher, RR 1.07, p = 1.00, treatment 5 of 14 (35.7%), control 7 of 21 (33.3%).
|
|
hospitalization time, 20.0% lower, relative time 0.80, treatment 14, control 21.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Alsultan et al., 31 Dec 2021, Randomized Controlled Trial, Syria, peer-reviewed, 11 authors.
Efficacy of Colchicine and Budesonide in Improvement Outcomes of Patients with Coronavirus Infection 2019 in Damascus, Syria: A Randomized Control Trial
Interdisciplinary Perspectives on Infectious Diseases, doi:10.1155/2021/2129006
COVID-19 was reported in China in 2019 and has spread worldwide. Transmission occurs through respiratory secretions and, less commonly, through contaminated surfaces. e severity of the disease can range from asymptomatic to acute respiratory distress syndrome (ARDS). In this study, we aim to investigate the efficacy of two agents (oral colchicine and budesonide inhaler) in COVID-19 infection management, compared with supportive care alone. 77 patients were admitted to the isolation section of Al Assad University Hospital, between the 1 st of August and the 30 th of August. A total of 49 patients were included in this randomized control trial, after excluding ineligible patients. e random sample was divided into three groups; the first group was supportive care plus colchicine, the second group was supportive care plus budesonide inhaler, and the control group was supportive care alone. PaO2/FiO2 was improved in the budesonide group, higher than the supportive and colchicine groups. e median hospitalization days were shorter when using colchicine or budesonide, opposed to supportive care alone (8 vs 10 days, respectively). 34 patients (69.3%) were discharged, and 27 patients (55.1%) were followed up until they were weaned from oxygen and made a complete recovery. ere was a significant decrease in mortality with colchicine (3 patients; 21.4%) compared with supportive care (7 patients; 33.3%) and the budesonide group (5 patients; 35.7%).
Conflicts of Interest e authors declare that they have no conflicts of interest.
References
Anthony, Dennis, Kasper, Dan, Longo, Harrison's Pulmonary and Critical Care Medicine
Atta, El-Rehany, Abdel Raheim, Fouad, Galal, Colchicine inhibits intimal hyperplasia and leukocyte VEGF expression in dogs, Journal of Surgical Research
Ben-Chetrit, Levy, Colchicine: 1998 update, Seminars in Arthritis and Rheumatism
Bhattacharyya, Panda, Gupta, Banerjee, Antimitotic activity of colchicine and the structural basis for its interaction with tubulin, Medicinal Research Reviews
Bitterman, Pathogenesis of fibrosis in acute lung injury, e American Journal of Medicine
Coronavirus, Disease 2019 (COVID-19) treatment guidelines
Deftereos, Giannopoulos, Vrachatis, Effect of colchicine vs standard care on cardiac and inflammatory biomarkers and clinical outcomes in patients hospitalized with coronavirus disease 2019, Journal of the American Medical Association Network Open
Flynn Makic, Prone position of patients with COVID-19 and acute respiratory distress syndrome, Journal of PeriAnesthesia Nursing
Gao, Hu, Dai, Xiao, Wang et al., e epidemiological characteristics of 2019 novel coronavirus diseases (COVID-19) in jingmen, China, SSRN Electronic Journal
Grassin-Delyle, Roquencourt, Moine, Saffroy, Carn et al., Metabolomics of exhaled breath in critically ill COVID-19 patients: a pilot study, EBioMedicine
Guideline, CG10393-COVID-romboprophylaxis-and-Anticoagulation-in-COVID-19-infections
Gust, Schuster, Cardiocirculatory management in acute lung injury and ARDS, Timing, sleep, and respiration in health and disease
Ju, Gao, Huang, erapeutic effect of inhaled budesonide (PulmicortTurbuhaler) on the inflammatory response to one-lung ventilation, Anaesthesia
Ju, Yu, Wang, Budesonide ameliorates lung injury induced by large volume ventilation, BMC Pulmonary Medicine
Lee, Lu, Zhen, Benefit of combined therapy with nicorandil and colchicine in preventing monocrotaline-induced rat pulmonary arterial hypertension, European Journal of Pharmaceutical Sciences: Official Journal of the European Federation for Pharmaceutical Sciences
Li, Liao, Lee, Huang, Quinn, Involvement of Akt and endothelial nitric oxide synthase in ventilation-induced neutrophil infiltration: a prospective, controlled animal experiment, Critical Care
Lopes, Bonjorno, Giannini, Amaral, Benatti et al., double-blinded, placebo controlled clinical trial
Matthay, Folkesson, Clerici, Lung epithelial fluid transport and the resolution of pulmonary edema, Physiological Reviews
Miyao, Suzuki, Takeshita, Various adhesion molecules impair microvascular leukocyte kinetics in ventilator-induced lung injury, American Journal of Physiology. Lung Cellular and Molecular Physiology
Mohamed, Meguid, Effect of nebulized budesonide on respiratory mechanics and oxygenation in acute lung injury/ acute respiratory distress syndrome: randomized controlled study, Saudi Journal of Anaesthesia
Moraes, Zurawska, Downey, Neutrophil granule contents in the pathogenesis of lung injury, Current Opinion in Hematology
Nathan, Secretory products of macrophages, Journal of Clinical Investigation
Opal, Depalo, Anti-inflammatory cytokines, Chest
Pittet, Mackersie, Martin, Matthay, Biological markers of acute lung injury: prognostic and pathogenetic significance, American Journal of Respiratory and Critical Care Medicine
Ramakrishnan, Nicolau, Inhaled budesonide in the treatment of early COVID-19 illness: a randomised controlled trial, British Medical Journal
Ramanathan, Antognini, Combes, Paden, Zakhary et al., Since january 2020
Rüdiger, Gencay, Yang, Bihl, Tamm et al., Fast beneficial systemic anti-inflammatory effects of inhaled budesonide and formoterol on circulating lymphocytes in asthma, Respirology
Sandbo, Ngam, Torr, Kregel, Kach et al., Control of myofibroblast differentiation by microtubule dynamics through a regulated localization of mDia2, Journal of Biological Chemistry
Scarsi, Piantoni, Colombo, Association between treatment with colchicine and improved survival in a singlecentre cohort of adult hospitalised patients with COVID-19 pneumonia and acute respiratory distress syndrome, Annals of the Rheumatic Diseases
Schlesinger, Firestein, Brunetti, Colchicine in COVID-19: an old drug, new use, Current Pharmacology Reports
Stokes, Zambrano, Anderson, Coronavirus disease 2019 case surveillance-United States, january 22-may, MMWR. Morbidity and Mortality Weekly Report
Straumann, Conus, Degen, Budesonide is effective in adolescent and adult patients with active eosinophilic esophagitis, Gastroenterology
Wu, Mcgoogan, Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China, Journal of the American Medical Association
Xu, Huang, Fan, Arbidol/IFN-α2b therapy for patients with corona virus disease 2019: a retrospective multicenter cohort study, Microbes and Infection
DOI record:
{
"DOI": "10.1155/2021/2129006",
"ISSN": [
"1687-7098",
"1687-708X"
],
"URL": "http://dx.doi.org/10.1155/2021/2129006",
"abstract": "<jats:p>COVID-19 was reported in China in 2019 and has spread worldwide. Transmission occurs through respiratory secretions and, less commonly, through contaminated surfaces. The severity of the disease can range from asymptomatic to acute respiratory distress syndrome (ARDS). In this study, we aim to investigate the efficacy of two agents (oral colchicine and budesonide inhaler) in COVID-19 infection management, compared with supportive care alone. 77 patients were admitted to the isolation section of Al Assad University Hospital, between the 1st of August and the 30th of August. A total of 49 patients were included in this randomized control trial, after excluding ineligible patients. The random sample was divided into three groups; the first group was supportive care plus colchicine, the second group was supportive care plus budesonide inhaler, and the control group was supportive care alone. PaO2/FiO2 was improved in the budesonide group, higher than the supportive and colchicine groups. The median hospitalization days were shorter when using colchicine or budesonide, opposed to supportive care alone (8 vs 10 days, respectively). 34 patients (69.3%) were discharged, and 27 patients (55.1%) were followed up until they were weaned from oxygen and made a complete recovery. There was a significant decrease in mortality with colchicine (3 patients; 21.4%) compared with supportive care (7 patients; 33.3%) and the budesonide group (5 patients; 35.7%).</jats:p>",
"alternative-id": [
"2129006",
"2129006"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0001-9113-5338",
"affiliation": [
{
"name": "Department of Nephrology, Al Assad and Al Mouwasat University Hospitals, Damascus, Syria"
}
],
"authenticated-orcid": true,
"family": "Alsultan",
"given": "Mohammad",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Department of Infectious Diseases, Al Assad and Al Mouwasat University Hospitals, Damascus, Syria"
}
],
"family": "Obeid",
"given": "Ameer",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Neurology, Al Assad and Al Mouwasat University Hospitals, Damascus, Syria"
}
],
"family": "Alsamarrai",
"given": "Omar",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Professor, Statics Department, Aleppo University, Aleppo, Syria"
}
],
"family": "Anan",
"given": "Mohamed Taher",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Oncology, Al Biruni University Hospital, Damascus, Syria"
}
],
"family": "Bakr",
"given": "Aliaa",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Internal Medicine, Al Assad and Al Mouwasat University Hospitals, Damascus, Syria"
}
],
"family": "Soliman",
"given": "Nawwar",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Oncology, Al Biruni University Hospital, Damascus, Syria"
}
],
"family": "Kurdy",
"given": "Mamdoh",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Internal Medicine, Al Assad and Al Mouwasat University Hospitals, Damascus, Syria"
}
],
"family": "Mosa",
"given": "Muhannad Hag",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Neurology, Al Assad and Al Mouwasat University Hospitals, Damascus, Syria"
}
],
"family": "Saleh",
"given": "Zain",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Internal Medicine, Al Assad and Al Mouwasat University Hospitals, Damascus, Syria"
}
],
"family": "Hujij",
"given": "Fatima",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Rheumatology, Al Assad and Al Mouwasat University Hospitals, Damascus, Syria"
}
],
"family": "Barhoum",
"given": "Jafar",
"sequence": "additional"
}
],
"container-title": [
"Interdisciplinary Perspectives on Infectious Diseases"
],
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2021,
12,
31
]
],
"date-time": "2021-12-31T16:50:07Z",
"timestamp": 1640969407000
},
"deposited": {
"date-parts": [
[
2021,
12,
31
]
],
"date-time": "2021-12-31T16:50:14Z",
"timestamp": 1640969414000
},
"editor": [
{
"affiliation": [],
"family": "Lanzafame",
"given": "Massimiliano",
"sequence": "additional"
}
],
"indexed": {
"date-parts": [
[
2022,
1,
1
]
],
"date-time": "2022-01-01T05:55:40Z",
"timestamp": 1641016540493
},
"is-referenced-by-count": 0,
"issn-type": [
{
"type": "electronic",
"value": "1687-7098"
},
{
"type": "print",
"value": "1687-708X"
}
],
"issued": {
"date-parts": [
[
2021,
12,
31
]
]
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
12,
31
]
],
"date-time": "2021-12-31T00:00:00Z",
"timestamp": 1640908800000
}
}
],
"link": [
{
"URL": "http://downloads.hindawi.com/journals/ipid/2021/2129006.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "http://downloads.hindawi.com/journals/ipid/2021/2129006.xml",
"content-type": "application/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "http://downloads.hindawi.com/journals/ipid/2021/2129006.pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "98",
"original-title": [],
"page": "1-7",
"prefix": "10.1155",
"published": {
"date-parts": [
[
2021,
12,
31
]
]
},
"published-print": {
"date-parts": [
[
2021,
12,
31
]
]
},
"publisher": "Hindawi Limited",
"reference": [
{
"article-title": "Disease 2019 (COVID-19) treatment guidelines",
"author": "N. H. Coronavirus",
"key": "1",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.2648",
"doi-asserted-by": "publisher",
"key": "2"
},
{
"DOI": "10.15585/mmwr.mm6924e2",
"doi-asserted-by": "publisher",
"key": "3"
},
{
"article-title": "The epidemiological characteristics of 2019 novel coronavirus diseases (COVID-19) in jingmen, China",
"author": "Q. Gao",
"first-page": "113",
"issue": "8",
"journal-title": "SSRN Electronic Journal",
"key": "4",
"volume": "2",
"year": "2020"
},
{
"author": "S. Anthony",
"key": "5",
"volume-title": "Harrison’s Pulmonary and Critical Care Medicine",
"year": "2010"
},
{
"DOI": "10.1152/physrev.00003.2002",
"doi-asserted-by": "publisher",
"key": "6"
},
{
"DOI": "10.1172/jci112815",
"doi-asserted-by": "publisher",
"key": "7"
},
{
"DOI": "10.1097/01.moh.0000190113.31027.d5",
"doi-asserted-by": "publisher",
"key": "8"
},
{
"DOI": "10.1164/ajrccm.155.4.9105054",
"doi-asserted-by": "publisher",
"key": "9"
},
{
"DOI": "10.1016/0002-9343(92)90606-c",
"doi-asserted-by": "publisher",
"key": "10"
},
{
"DOI": "10.1002/med.20097",
"doi-asserted-by": "publisher",
"key": "11"
},
{
"DOI": "10.1016/s0049-0172(98)80028-0",
"doi-asserted-by": "publisher",
"key": "12"
},
{
"DOI": "10.1007/s40495-020-00225-6",
"doi-asserted-by": "publisher",
"key": "13"
},
{
"DOI": "10.1016/j.jss.2007.04.029",
"doi-asserted-by": "publisher",
"key": "14"
},
{
"DOI": "10.1074/jbc.m113.464461",
"doi-asserted-by": "publisher",
"key": "15"
},
{
"DOI": "10.1016/j.ejps.2013.08.004",
"doi-asserted-by": "publisher",
"key": "16"
},
{
"DOI": "10.1186/cc6101",
"doi-asserted-by": "publisher",
"key": "17"
},
{
"DOI": "10.1152/ajplung.00365.2005",
"doi-asserted-by": "publisher",
"key": "18"
},
{
"DOI": "10.1111/resp.12104",
"doi-asserted-by": "publisher",
"key": "19"
},
{
"DOI": "10.1111/anae.12479",
"doi-asserted-by": "publisher",
"key": "20"
},
{
"DOI": "10.1378/chest.117.4.1162",
"doi-asserted-by": "publisher",
"key": "21"
},
{
"DOI": "10.1053/j.gastro.2010.07.048",
"doi-asserted-by": "publisher",
"key": "22"
},
{
"DOI": "10.1186/s12890-016-0251-z",
"doi-asserted-by": "publisher",
"key": "23"
},
{
"DOI": "10.1016/j.micinf.2020.05.012",
"doi-asserted-by": "publisher",
"key": "24"
},
{
"article-title": "Beneficial effects of colchicine for moderate to severe COVID-19: an interim analysis of a randomized, double-blinded, placebo controlled clinical trial",
"author": "M. I. F. Lopes",
"key": "25",
"year": "2020"
},
{
"DOI": "10.1016/j.ebiom.2020.103154",
"doi-asserted-by": "publisher",
"key": "26"
},
{
"DOI": "10.1001/jamanetworkopen.2020.13136",
"doi-asserted-by": "publisher",
"key": "27"
},
{
"DOI": "10.4103/1658-354x.197369",
"doi-asserted-by": "publisher",
"key": "28"
},
{
"article-title": "CG10393-COVID-Thromboprophylaxis-and-Anticoagulation-in-COVID-19-infections.pdf",
"author": "C. Guideline",
"key": "29",
"year": "2021"
},
{
"article-title": "Cardiocirculatory management in acute lung injury and ARDS",
"author": "R. Gust",
"first-page": "837",
"issue": "1",
"journal-title": "Timing, sleep, and respiration in health and disease [Internet",
"key": "30",
"volume": "1",
"year": "2001"
},
{
"DOI": "10.1016/j.jopan.2020.05.008",
"doi-asserted-by": "publisher",
"key": "31"
},
{
"article-title": "Since january 2020 elsevier has created a COVID-19 resource centre with free information in english and mandarin on the novel coronavirus COVID- research that is available on the COVID-19 resource centre - including this for unrestricted research re-use a",
"author": "K. Ramanathan",
"key": "32",
"year": "2020"
},
{
"DOI": "10.1183/13993003.congress-2021.rct4270",
"doi-asserted-by": "publisher",
"key": "33"
},
{
"DOI": "10.1136/annrheumdis-2020-217712",
"doi-asserted-by": "publisher",
"key": "34"
}
],
"reference-count": 34,
"references-count": 34,
"relation": {},
"score": 1,
"short-container-title": [
"Interdisciplinary Perspectives on Infectious Diseases"
],
"short-title": [],
"source": "Crossref",
"subject": [
"Virology",
"Infectious Diseases",
"Microbiology (medical)",
"Microbiology",
"Parasitology"
],
"subtitle": [],
"title": [
"Efficacy of Colchicine and Budesonide in Improvement Outcomes of Patients with Coronavirus Infection 2019 in Damascus, Syria: A Randomized Control Trial"
],
"type": "journal-article",
"volume": "2021"
}
