Lifestyle risk factors and infectious disease mortality, including COVID-19, among middle aged and older adults: Evidence from a community-based cohort study in the United Kingdom
et al., Brain, Behavior, and Immunity, doi:10.1016/j.bbi.2021.04.022, Aug 2021
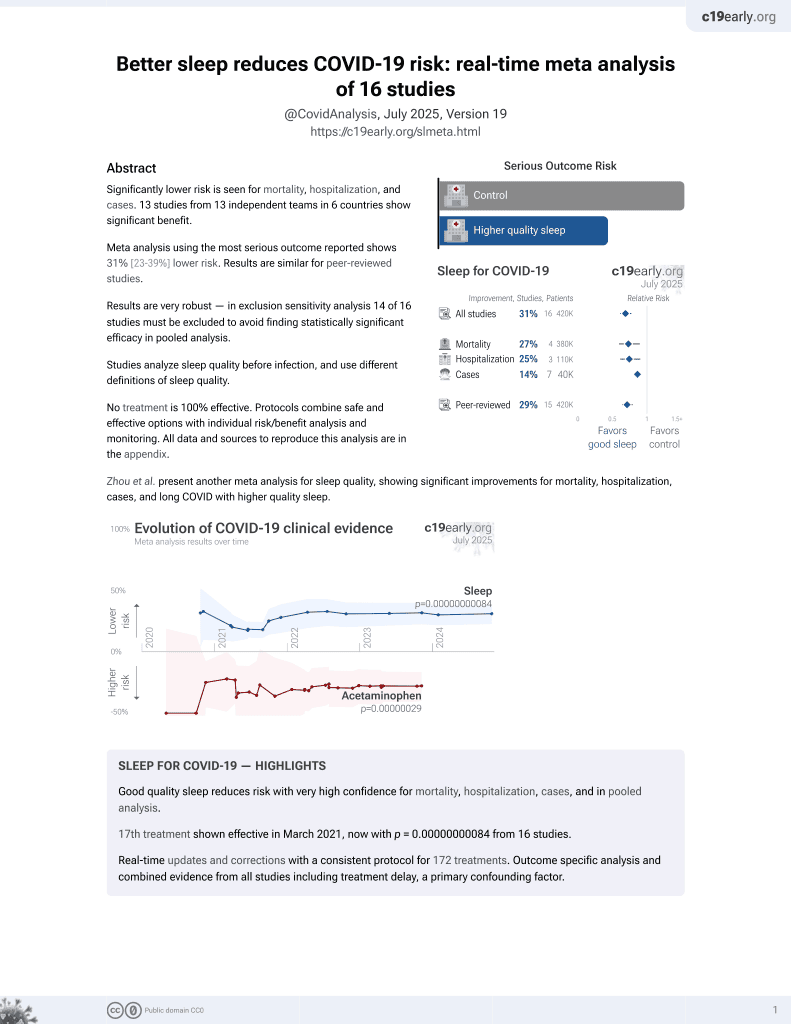
Sleep for COVID-19
17th treatment shown to reduce risk in
March 2021, now with p = 0.00000000084 from 16 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
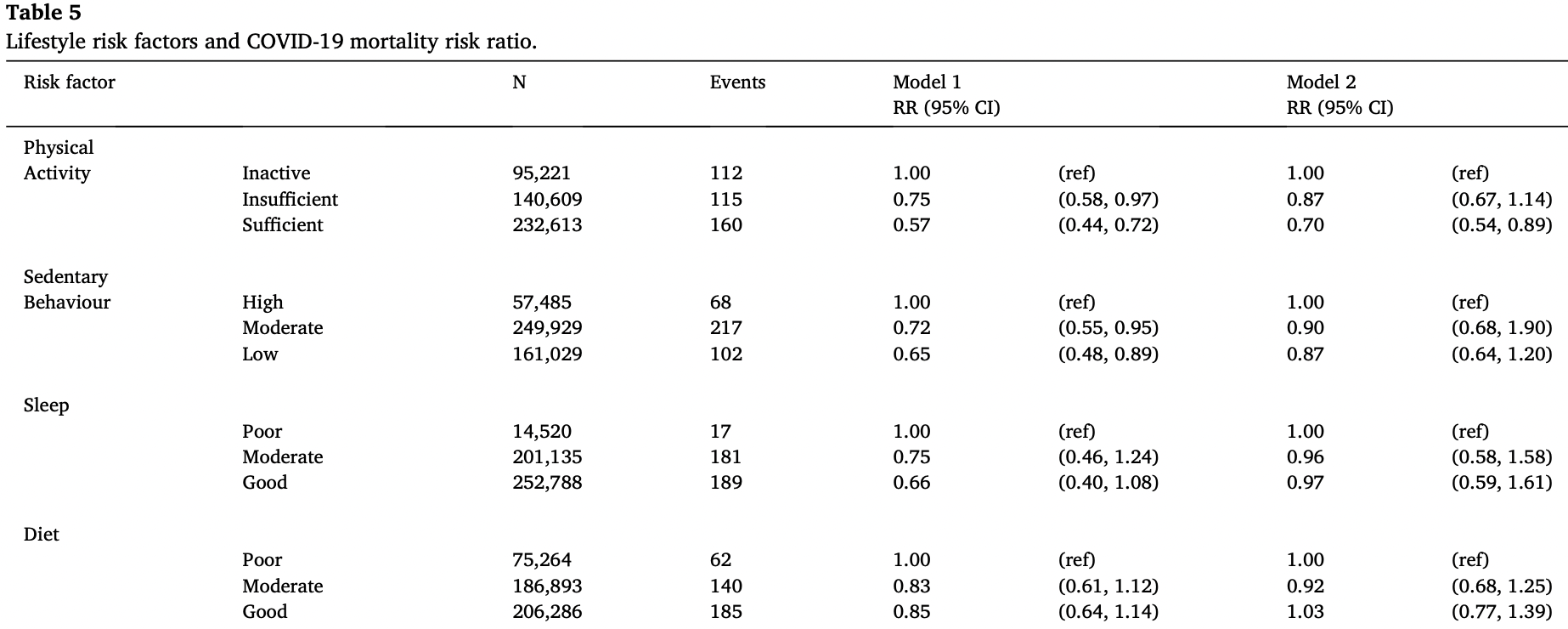
Retrospective 468,569 adults in the UK, showing no significant difference in COVID-19 mortality based on sleep quality.
Standard of Care (SOC) for COVID-19 in the study country,
the United Kingdom, is very poor with very low average efficacy for approved treatments1.
The United Kingdom focused on expensive high-profit treatments, approving only one low-cost early treatment, which required a prescription and had limited adoption. The high-cost prescription treatment strategy reduces the probability of early treatment due to access and cost barriers, and eliminates complementary and synergistic benefits seen with many low-cost treatments.
|
risk of death, 3.0% lower, RR 0.97, p = 0.91, adjusted per study, good vs. poor, model 2, multivariable.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Ahmadi et al., 31 Aug 2021, retrospective, United Kingdom, peer-reviewed, 5 authors.
Lifestyle risk factors and infectious disease mortality, including COVID-19, among middle aged and older adults: Evidence from a community-based cohort study in the United Kingdom
Brain, Behavior, and Immunity, doi:10.1016/j.bbi.2021.04.022
In this community-based cohort study, we investigated the relationship between combinations of modifiable lifestyle risk factors and infectious disease mortality. Participants were 468,569 men and women (56.5 ± 8.1, 54.6% women) residing in the United Kingdom. Lifestyle indexes included traditional and emerging lifestyle risk factors based on health guidelines and best practice recommendations for: physical activity, sedentary behaviour, sleep quality, diet quality, alcohol consumption, and smoking status. The main outcome was mortality from infectious diseases, including pneumonia, and coronavirus disease 2019 (COVID-19). Meeting public health guidelines or best practice recommendations among combinations of lifestyle risk factors was inversely associated with mortality. Hazard ratios ranged between 0.26 (0.23-0.30) to 0.69 (0.60-0.79) for infectious disease and pneumonia. Among participants with pre-existing cardiovascular disease or cancer, hazard ratios ranged between 0.30 (0.25-0.34) to 0.73 (0.60-0.89). COVID-19 mortality risk ranged between 0.42 (0.28-0.63) to 0.75 (0.49-1.13). We found a beneficial dose-response association with a higher lifestyle index against mortality that was consistent across sex, age, BMI, and socioeconomic status. There was limited evidence of synergistic interactions between most lifestyle behaviour pairs, suggesting that the dose-response relationship among different lifestyle behaviours is not greater than the sum of the risk induced by each behaviour. Improvements in lifestyle risk factors and meeting public health guidelines or best practice recommendations could be used as an ancillary measure to ameliorate infectious disease mortality.
References
Adan, Archer, Hidalgo, Di Milia, Natale et al., Circadian typology: A comprehensive review, Chronobiol. Int, doi:10.3109/07420528.2012.719971
Allen, Sudlow, Downey, Peakman, Danesh et al., UK Biobank: Current status and what it means for epidemiology, Heal. Policy Technol
Almirall, Bolíbar, Serra-Prat, Roig, Hospital et al., New evidence of risk factors for community-acquired pneumonia: A population-based study, Eur. Respir. J, doi:10.1183/09031936.00095807
Ambrus, Ambrus, Nutrition and infectious diseases in developing countries and problems of acquired immunodeficiency syndrome, Exp. Biol. Med, doi:10.1177/153537020422900603
Andersson, Alfredsson, Källberg, Zdravkovic, Ahlbom, Calculating measures of biological interaction, Eur. J. Epidemiol, doi:10.1007/s10654-005-7835-x
Baik, Curhan, Rimm, Bendich, Willett et al., A prospective study of age and lifestyle factors in relation to community-acquired pneumonia in US men and women, Arch. Intern. Med, doi:10.1001/archinte.160.20.3082
Bonaccio, Di Castelnuovo, Costanzo, De Curtis, Persichillo et al., Impact of combined healthy lifestyle factors on survival in an adult general population and in high-risk groups: prospective results from the Moli-sani study, J. Intern. Med, doi:10.1111/joim.12637
Bull, Saad Al-Ansari, Biddle, Borodulin, Buman et al., World Health Organization 2020 Guidelines on Physical Activity and Sedentary Behaviour, Br. J. Sports Med, doi:10.1136/bjsports-2020-102955
Buuren, Van, Groothuis-Oudshoorn, mice: Multivariate imputation by chained equations in R, J. Stat. Softw, doi:10.1080/10580530.2013.739883
Carter, Abnet, Feskanich, Freedman, Hartge et al., Smoking and Mortality -Beyond Established Causes, N. Engl. J. Med, doi:10.1056/nejmsa1407211
Cassini, Högberg, Plachouras, Quattrocchi, Hoxha et al., Attributable deaths and disability-adjusted life-years caused by infections with antibiotic-resistant bacteria in the EU and the European Economic Area in 2015: a population-level modelling analysis, Lancet Infect. Dis, doi:10.1016/S1473-3099(18)30605-4
Chau, Grunseit, Chey, Stamatakis, Brown et al., Daily sitting time and all-cause mortality: A meta-analysis, PLoS One, doi:10.1371/journal.pone.0080000
Chau, Grunseit, Midthjell, Holmen, Holmen et al., Sedentary behaviour and risk of mortality from all-causes and cardiometabolic diseases in adults: Evidence from the HUNT3 population cohort, Br. J. Sports Med, doi:10.1136/bjsports-2012-091974
Chiuve, Fung, Rimm, Hu, Mccullough et al., Alternative dietary indices both strongly predict risk of chronic disease, J. Nutr, doi:10.3945/jn.111.157222
Craig, Marshall, Sjöström, Bauman, Booth et al., International physical activity questionnaire: 12-Country reliability and validity, Med. Sci. Sports Exerc, doi:10.1249/01.MSS.0000078924.61453.FB
Ding, Rogers, Van Der Ploeg, Stamatakis, Bauman, Traditional and Emerging Lifestyle Risk Behaviors and All-Cause Mortality in Middle-Aged and Older Adults: Evidence from a Large Population-Based Australian Cohort, PLoS Med, doi:10.1371/journal.pmed.1001917
Dunstan, Howard, Healy, Owen, Too much sitting -A health hazard, Diabetes Res. Clin. Pract, doi:10.1016/j.diabres.2012.05.020
Fan, Sun, Zhou, Heianza, Lv et al., Sleep patterns, genetic susceptibility, and incident cardiovascular disease: A prospective study of 385 292 UK biobank participants, Eur. Heart J, doi:10.1093/eurheartj/ehz849
Ferkol, Schraufnagel, The global burden of respiratory disease, Ann. Am. Thorac. Soc, doi:10.1513/AnnalsATS.201311-405PS
Fletcher, Landolfo, Niebauer, Ozemek, Arena et al., Promoting Physical Activity and Exercise: JACC Health Promotion Series, J. Am. Coll. Cardiol, doi:10.1016/j.jacc.2018.08.2141
Friedman, Klatsky, Is alcohol good for your health?, N. Engl. J. Med
Fry, Littlejohns, Sudlow, Doherty, Adamska et al., Comparison of Sociodemographic and Health-Related Characteristics of UK Biobank Participants With Those of the General Population, Am. J. Epidemiol, doi:10.1093/aje/kwx246
Galea, Ph, Tracy, Participation Rates in Epidemiologic Studies, Ann. Epidemiol, doi:10.1016/j.annepidem.2007.03.013
Gelband, Miller-Petrie, Pant, Gandra, Levinson et al., The state of the world's antibiotics 2015, Wound Heal. South. Africa
Gordon, Weanling diarrhoea-a synergism of infection and nutrition, Interactions of Malnutrition and Infection
Hamer, Kivimäki, Gale, Batty, Lifestyle risk factors, inflammatory mechanisms, and COVID-19 hospitalization: A community-based cohort study of 387,109 adults in UK, Brain. Behav. Immun, doi:10.1016/j.bbi.2020.05.059
Hamer, O'donovan, Stamatakis, Lifestyle risk factors, obesity and infectious disease mortality in the general population: Linkage study of 97,844 adults from England and Scotland, Prev. Med. (Baltim), doi:10.1016/j.ypmed.2019.03.002
Hamer, Stamatakis, Steptoe, Effects of substituting sedentary time with physical activity on metabolic risk, Med. Sci. Sports Exerc, doi:10.1249/MSS.0000000000000317
Hamilton, Hamilton, Zderic, Role of low energy expenditure and sitting in obesity, metabolic syndrome, type 2 diabetes, and cardiovascular disease, Diabetes, doi:10.2337/db07-0882.CVD
Hersey, Prendergast, Edwards, Effects of cigarette smoking on the immune system Follow-up studies in normal subjects after cessation of smoking, Med. J. Aust, doi:10.5694/j.1326-5377.1983.tb122565.x
Hur, Bourchar, Lykken, Genetic and environmental influence on morningness-eveningness, Pers. Individ. Dif
Huttunen, Heikkinen, Syrjänen, Smoking and the outcome of infection, J. Intern. Med, doi:10.1111/j.1365-2796.2010.02332.x
Ibarra-Coronado, Pantaleón-Martínez, Velazquéz-Moctezuma, Prospéro-García, Méndez-Díaz et al., The Bidirectional Relationship between Sleep and Immunity against Infections, J. Immunol. Res, doi:10.1155/2015/678164
Inoue, Koizumi, Wada, Iso, Watanabe et al., Risk and protective factors related to mortality from pneumonia among middle-aged and elderly community residents: The JACC study, J. Epidemiol, doi:10.2188/jea.17.194
Irwin, Why sleep is important for health: A psychoneuroimmunology perspective, Annu. Rev. Psychol, doi:10.1146/annurev-psych-010213-115205
Kadri, Key Takeaways from the U.S. CDC's 2019 Antibiotic Resistance Threats Report for Frontline Providers, Crit. Care Med, doi:10.1097/CCM.0000000000004371
Katona, Katona-Apte, The interaction between nutrition and infection, Clin. Infect. Dis, doi:10.1086/587658
Knott, Coombs, Stamatakis, Biddulph, All cause mortality and the case for age specific alcohol consumption guidelines: Pooled analyses of up to 10 population based cohorts, BMJ, doi:10.1136/bmj.h384
Koskenvuo, Hublin, Partinen, Heikkilä, Kaprio, Heritability of diurnal type: A nationwide study of 8753 adult twin pairs, J. Sleep Res, doi:10.1111/j.1365-2869.2007.00580.x
Källberg, Ahlbom, Alfredsson, Calculating measures of biological interaction using R, Eur. J. Epidemiol, doi:10.1007/s10654-006-9037-6
Lee, Sui, Hooker, Ebert, Blair, Combined Impact of Lifestyle Factors on Cancer Mortality in Men, doi:10.1016/j.annepidem.2011.04.010
Mackinnon, Marston, Dixon, Knisely, Palmore et al., Advances in exercise immunology, JAMA -J. Am. Med. Assoc, doi:10.1001/jama.2016.11764
Matthews, Ockene, Freedson, Rosal, Merriam et al., Moderate to vigorous physical activity and risk of upper-respiratory tract infection, Med. Sci. Sport. Exerc
Mccullough, Feskanich, Stampfer, Giovannucci, Rimm et al., Diet quality and major chronic disease risk in men and women: Moving toward improved dietary guidance, Am. J. Clin. Nutr, doi:10.1093/ajcn/76.6.1261
Nair, Brooks, Katz, Roca, Berkley et al., Global burden of respiratory infections due to seasonal influenza in young children: A systematic review and meta-analysis, Lancet, doi:10.1016/S0140-6736(11)61051-9
Nieman, Exercise, Infection, and Immunity, Int. J. Sports Med, doi:10.1055/s-2007-1021128
Nieman, Henson, Austin, Sha, Upper respiratory tract infection is reduced in physically fit and active adults, Br. J. Sports Med, doi:10.1136/bjsm.2010.077875
Nieman, Nehlsen-Cannarella, Markoff, Balk-Lamberton, Yang et al., The effects of moderate exercise training on natural killer cells and acute upper respiratory tract infections, Int. J. Sports Med, doi:10.1055/s-2007-1024839
Opp, Krueger, Sleep and immunity: A growing field with clinical impact, Brain. Behav. Immun, doi:10.1016/j.bbi.2015.03.011
Paulsen, Mehl, Dewan, Solliga, Dama et al., Associations of obesity and lifestyle with the risk and mortality of bloodstream infection in a general population : a 15-year follow-up of 64 027 individuals in the HUNT Study, Int. J. Epidemiol, doi:10.1093/ije/dyx091
Perreault, Bauman, Johnson, Britton, Rangul et al., Does physical activity moderate the association between alcohol drinking and all-cause, cancer and cardiovascular diseases mortality? A pooled analysis of eight British population cohorts, Br. J. Sports Med, doi:10.1136/bjsports-2016-096194
Prather, Leung, Association of insufficient sleep with respiratory infection among adults in the United States, JAMA Intern. Med, doi:10.1001/jamainternmed.2016.0787
Rehm, Baliunas, Borges, Graham, Irving et al., The relation between different dimensions of alcohol consumption and burden of disease: An overview, Addiction, doi:10.1111/j.1360-0443.2010.02899.x
Rosenberg, Bauld, Hooper, Buykx, Holmes et al., New national alcohol guidelines in the UK: Public awareness, understanding and behavioural intentions, J. Public Heal, doi:10.1093/pubmed/fdx126
Rudd, Johnson, Agesa, Shackelford, Tsoi et al., Global, regional, and national sepsis incidence and mortality, 1990-2017: analysis for the Global Burden of Disease Study, Lancet, doi:10.1016/S0140-6736(19)32989-7
Sallis, Adlakha, Oyeyemi, Salvo, An international physical activity and public health research agenda to inform coronavirus disease-2019 policies and practices, J. Sport Heal. Sci, doi:10.1016/j.jshs.2020.05.005
Samokhvalov, Irving, Rehm, Alcohol consumption as a risk factor for pneumonia: A systematic review and meta-analysis, Epidemiol. Infect, doi:10.1017/S0950268810000774
Scrimshaw, Sangiovanni, Synergism of nutrition, infection, and immunity: An overview, Am. J. Clin. Nutr, doi:10.1093/ajcn/66.2.464S
Song, Thamlikitkul, Hsueh, Clinical and economic burden of community-acquired pneumonia amongst adults in the Asia-Pacific region, Int. J. Antimicrob. Agents, doi:10.1016/j.ijantimicag.2011.02.017
Sopori, Effects of cigarette smoke on the immune system, Nat. Rev. Immunol
Stamatakis, Rogers, Ding, Berrigan, Chau et al., All-cause mortality effects of replacing sedentary time with physical activity and sleeping using an isotemporal substitution model: A prospective study of 201,129 mid-aged and older adults, Int. J. Behav. Nutr. Phys. Act, doi:10.1186/s12966-015-0280-7
Sudlow, Gallacher, Allen, Beral, Burton et al., UK Biobank: An Open Access Resource for Identifying the Causes of a Wide Range of Complex Diseases of Middle and Old Age, PLoS Med, doi:10.1371/journal.pmed.1001779
Tacconelli, Sifakis, Harbarth, Schrijver, Van Mourik et al., Surveillance for control of antimicrobial resistance, Lancet Infect. Dis, doi:10.1016/S1473-3099(17)30485-1
Townsend, Phillimore, Beattie, Health and deprivation: inequality and the North
Uk Biobank, UK Biobank: Protocol for a large-scale prospective epidemiological resource
Wang, Baddley, Griffin, Judd, Howard et al., Physical inactivity and long-term rates of community-acquired sepsis, Prev. Med. (Baltim), doi:10.1016/j.ypmed.2014.04.017
Wang, Liu, Chen, Liu, Huang et al., The role of increased body mass index in outcomes of sepsis: A systematic review and meta-analysis, BMC Anesthesiol, doi:10.1186/s12871-017-0405-4
Welte, Torres, Nathwani, Clinical and economic burden of communityacquired pneumonia among adults in Europe, Thorax, doi:10.1136/thx.2009.129502
Weycker, Strutton, Edelsberg, Sato, Jackson, Clinical and economic burden of pneumococcal disease in older US adults, Vaccine, doi:10.1016/j.vaccine.2010.05.030
Xiao, Keadle, Hollenbeck, Matthews, Sleep duration and total and cause-specific mortality in a large US cohort: Interrelationships with physical activity, sedentary behavior, and body mass index, Am. J. Epidemiol, doi:10.1093/aje/kwu222
DOI record:
{
"DOI": "10.1016/j.bbi.2021.04.022",
"ISSN": [
"0889-1591"
],
"URL": "http://dx.doi.org/10.1016/j.bbi.2021.04.022",
"alternative-id": [
"S088915912100180X"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Lifestyle risk factors and infectious disease mortality, including COVID-19, among middle aged and older adults: Evidence from a community-based cohort study in the United Kingdom"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "Brain, Behavior, and Immunity"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.bbi.2021.04.022"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2021 Elsevier Inc. All rights reserved."
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-3115-338X",
"affiliation": [],
"authenticated-orcid": false,
"family": "Ahmadi",
"given": "Matthew N.",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0001-8543-3152",
"affiliation": [],
"authenticated-orcid": false,
"family": "Huang",
"given": "Bo-Huei",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Inan-Eroglu",
"given": "Elif",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Hamer",
"given": "Mark",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Stamatakis",
"given": "Emmanuel",
"sequence": "additional"
}
],
"container-title": [
"Brain, Behavior, and Immunity"
],
"content-domain": {
"crossmark-restriction": true,
"domain": [
"clinicalkey.jp",
"clinicalkey.com",
"clinicalkey.es",
"clinicalkey.com.au",
"clinicalkey.fr",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2021,
5,
1
]
],
"date-time": "2021-05-01T06:37:46Z",
"timestamp": 1619851066000
},
"deposited": {
"date-parts": [
[
2021,
11,
1
]
],
"date-time": "2021-11-01T12:51:27Z",
"timestamp": 1635771087000
},
"indexed": {
"date-parts": [
[
2022,
3,
11
]
],
"date-time": "2022-03-11T11:26:30Z",
"timestamp": 1646997990992
},
"is-referenced-by-count": 4,
"issn-type": [
{
"type": "print",
"value": "0889-1591"
}
],
"issued": {
"date-parts": [
[
2021,
8
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
8,
1
]
],
"date-time": "2021-08-01T00:00:00Z",
"timestamp": 1627776000000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S088915912100180X?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S088915912100180X?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "18-27",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2021,
8
]
]
},
"published-print": {
"date-parts": [
[
2021,
8
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.3109/07420528.2012.719971",
"article-title": "Circadian typology: A comprehensive review",
"author": "Adan",
"doi-asserted-by": "crossref",
"first-page": "1153",
"journal-title": "Chronobiol. Int.",
"key": "10.1016/j.bbi.2021.04.022_b0005",
"volume": "29",
"year": "2012"
},
{
"DOI": "10.1016/j.hlpt.2012.07.003",
"doi-asserted-by": "crossref",
"key": "10.1016/j.bbi.2021.04.022_b0010",
"unstructured": "Allen, N., Sudlow, C., Downey, P., Peakman, T., Danesh, J., Elliott, P., Gallacher, J., Green, J., Matthews, P., Pell, J., Sprosen, T., Collins, R., 2012. UK Biobank: Current status and what it means for epidemiology. Heal. Policy Technol. 10.1016/j.hlpt.2012.07.003."
},
{
"DOI": "10.1183/09031936.00095807",
"article-title": "New evidence of risk factors for community-acquired pneumonia: A population-based study",
"author": "Almirall",
"doi-asserted-by": "crossref",
"first-page": "1274",
"journal-title": "Eur. Respir. J.",
"key": "10.1016/j.bbi.2021.04.022_b0015",
"volume": "31",
"year": "2008"
},
{
"DOI": "10.1177/153537020422900603",
"article-title": "Nutrition and infectious diseases in developing countries and problems of acquired immunodeficiency syndrome",
"author": "Ambrus",
"doi-asserted-by": "crossref",
"first-page": "464",
"journal-title": "Exp. Biol. Med.",
"key": "10.1016/j.bbi.2021.04.022_b0020",
"volume": "229",
"year": "2004"
},
{
"DOI": "10.1007/s10654-005-7835-x",
"article-title": "Calculating measures of biological interaction",
"author": "Andersson",
"doi-asserted-by": "crossref",
"first-page": "575",
"journal-title": "Eur. J. Epidemiol.",
"key": "10.1016/j.bbi.2021.04.022_b0025",
"volume": "20",
"year": "2005"
},
{
"DOI": "10.1001/archinte.160.20.3082",
"article-title": "A prospective study of age and lifestyle factors in relation to community-acquired pneumonia in US men and women",
"author": "Baik",
"doi-asserted-by": "crossref",
"first-page": "3082",
"journal-title": "Arch. Intern. Med.",
"key": "10.1016/j.bbi.2021.04.022_b0030",
"volume": "160",
"year": "2000"
},
{
"article-title": "Impact of combined healthy lifestyle factors on survival in an adult general population and in high-risk groups: prospective results from the Moli-sani study",
"author": "Bonaccio",
"first-page": "207",
"journal-title": "J. Intern. Med.",
"key": "10.1016/j.bbi.2021.04.022_b0035",
"volume": "286",
"year": "2019"
},
{
"article-title": "World Health Organization 2020 Guidelines on Physical Activity and Sedentary Behaviour",
"author": "Bull",
"journal-title": "Br. J. Sports Med.",
"key": "10.1016/j.bbi.2021.04.022_b0040",
"volume": "1451–1462",
"year": "2020"
},
{
"article-title": "mice: Multivariate imputation by chained equations in R",
"author": "Buuren",
"journal-title": "J. Stat. Softw.",
"key": "10.1016/j.bbi.2021.04.022_b0045",
"volume": "1–68",
"year": "2010"
},
{
"DOI": "10.1056/NEJMsa1407211",
"article-title": "Smoking and Mortality — Beyond Established Causes",
"author": "Carter",
"doi-asserted-by": "crossref",
"first-page": "631",
"journal-title": "N. Engl. J. Med.",
"key": "10.1016/j.bbi.2021.04.022_b0050",
"volume": "372",
"year": "2015"
},
{
"DOI": "10.1016/S1473-3099(18)30605-4",
"article-title": "Attributable deaths and disability-adjusted life-years caused by infections with antibiotic-resistant bacteria in the EU and the European Economic Area in 2015: a population-level modelling analysis",
"author": "Cassini",
"doi-asserted-by": "crossref",
"first-page": "56",
"journal-title": "Lancet Infect. Dis.",
"key": "10.1016/j.bbi.2021.04.022_b0055",
"volume": "19",
"year": "2019"
},
{
"DOI": "10.1136/bjsports-2012-091974",
"article-title": "Sedentary behaviour and risk of mortality from all-causes and cardiometabolic diseases in adults: Evidence from the HUNT3 population cohort",
"author": "Chau",
"doi-asserted-by": "crossref",
"first-page": "737",
"journal-title": "Br. J. Sports Med.",
"key": "10.1016/j.bbi.2021.04.022_b0060",
"volume": "49",
"year": "2015"
},
{
"DOI": "10.1371/journal.pone.0080000",
"article-title": "Daily sitting time and all-cause mortality: A meta-analysis",
"author": "Chau",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "PLoS One",
"key": "10.1016/j.bbi.2021.04.022_b0065",
"volume": "8",
"year": "2013"
},
{
"DOI": "10.3945/jn.111.157222",
"article-title": "Alternative dietary indices both strongly predict risk of chronic disease",
"author": "Chiuve",
"doi-asserted-by": "crossref",
"first-page": "1009",
"journal-title": "J. Nutr.",
"key": "10.1016/j.bbi.2021.04.022_b0070",
"volume": "142",
"year": "2012"
},
{
"DOI": "10.1249/01.MSS.0000078924.61453.FB",
"article-title": "International physical activity questionnaire: 12-Country reliability and validity",
"author": "Craig",
"doi-asserted-by": "crossref",
"first-page": "1381",
"journal-title": "Med. Sci. Sports Exerc.",
"key": "10.1016/j.bbi.2021.04.022_b0075",
"volume": "35",
"year": "2003"
},
{
"DOI": "10.1371/journal.pmed.1001917",
"article-title": "Traditional and Emerging Lifestyle Risk Behaviors and All-Cause Mortality in Middle-Aged and Older Adults: Evidence from a Large Population-Based Australian Cohort",
"author": "Ding",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "PLoS Med.",
"key": "10.1016/j.bbi.2021.04.022_b0080",
"volume": "12",
"year": "2015"
},
{
"DOI": "10.1016/j.diabres.2012.05.020",
"article-title": "Too much sitting - A health hazard",
"author": "Dunstan",
"doi-asserted-by": "crossref",
"first-page": "368",
"journal-title": "Diabetes Res. Clin. Pract.",
"key": "10.1016/j.bbi.2021.04.022_b0085",
"volume": "97",
"year": "2012"
},
{
"DOI": "10.1093/eurheartj/ehz849",
"article-title": "Sleep patterns, genetic susceptibility, and incident cardiovascular disease: A prospective study of 385 292 UK biobank participants",
"author": "Fan",
"doi-asserted-by": "crossref",
"first-page": "1182",
"journal-title": "Eur. Heart J.",
"key": "10.1016/j.bbi.2021.04.022_b0090",
"volume": "41",
"year": "2020"
},
{
"DOI": "10.1513/AnnalsATS.201311-405PS",
"article-title": "The global burden of respiratory disease",
"author": "Ferkol",
"doi-asserted-by": "crossref",
"first-page": "404",
"journal-title": "Ann. Am. Thorac. Soc.",
"key": "10.1016/j.bbi.2021.04.022_b0095",
"volume": "11",
"year": "2014"
},
{
"DOI": "10.1016/j.jacc.2018.08.2141",
"article-title": "Promoting Physical Activity and Exercise: JACC Health Promotion Series",
"author": "Fletcher",
"doi-asserted-by": "crossref",
"first-page": "1622",
"journal-title": "J. Am. Coll. Cardiol.",
"key": "10.1016/j.bbi.2021.04.022_b0100",
"volume": "72",
"year": "2018"
},
{
"DOI": "10.1056/NEJM199312163292510",
"article-title": "Is alcohol good for your health?",
"author": "Friedman",
"doi-asserted-by": "crossref",
"first-page": "1882",
"journal-title": "N. Engl. J. Med.",
"key": "10.1016/j.bbi.2021.04.022_b0105",
"year": "1993"
},
{
"DOI": "10.1093/aje/kwx246",
"article-title": "Comparison of Sociodemographic and Health-Related Characteristics of UK Biobank Participants With Those of the General Population",
"author": "Fry",
"doi-asserted-by": "crossref",
"first-page": "1026",
"journal-title": "Am. J. Epidemiol.",
"key": "10.1016/j.bbi.2021.04.022_b0110",
"volume": "186",
"year": "2017"
},
{
"DOI": "10.1016/j.annepidem.2007.03.013",
"article-title": "Participation Rates in Epidemiologic Studies",
"author": "Galea",
"doi-asserted-by": "crossref",
"first-page": "643",
"journal-title": "Ann. Epidemiol.",
"key": "10.1016/j.bbi.2021.04.022_b0115",
"volume": "17",
"year": "2007"
},
{
"article-title": "The state of the world’s antibiotics 2015",
"author": "Gelband",
"first-page": "30",
"journal-title": "Wound Heal. South. Africa",
"key": "10.1016/j.bbi.2021.04.022_b0120",
"volume": "8",
"year": "2015"
},
{
"key": "10.1016/j.bbi.2021.04.022_b0125",
"unstructured": "Gordon, J.E., 1968. Weanling diarrhoea—a synergism of infection and nutrition, in: Interactions of Malnutrition and Infection. p. 216."
},
{
"DOI": "10.1016/j.bbi.2020.05.059",
"article-title": "Lifestyle risk factors, inflammatory mechanisms, and COVID-19 hospitalization: A community-based cohort study of 387,109 adults in UK",
"author": "Hamer",
"doi-asserted-by": "crossref",
"first-page": "184",
"journal-title": "Brain. Behav. Immun.",
"key": "10.1016/j.bbi.2021.04.022_b0130",
"volume": "87",
"year": "2020"
},
{
"DOI": "10.1016/j.ypmed.2019.03.002",
"article-title": "Lifestyle risk factors, obesity and infectious disease mortality in the general population: Linkage study of 97,844 adults from England and Scotland",
"author": "Hamer",
"doi-asserted-by": "crossref",
"first-page": "65",
"journal-title": "Prev. Med. (Baltim)",
"key": "10.1016/j.bbi.2021.04.022_b0135",
"volume": "123",
"year": "2019"
},
{
"DOI": "10.1249/MSS.0000000000000317",
"article-title": "Effects of substituting sedentary time with physical activity on metabolic risk",
"author": "Hamer",
"doi-asserted-by": "crossref",
"first-page": "1946",
"journal-title": "Med. Sci. Sports Exerc.",
"key": "10.1016/j.bbi.2021.04.022_b0140",
"volume": "46",
"year": "2014"
},
{
"DOI": "10.2337/db07-0882",
"article-title": "Role of low energy expenditure and sitting in obesity, metabolic syndrome, type 2 diabetes, and cardiovascular disease",
"author": "Hamilton",
"doi-asserted-by": "crossref",
"first-page": "2655",
"journal-title": "Diabetes",
"key": "10.1016/j.bbi.2021.04.022_b0145",
"volume": "56",
"year": "2007"
},
{
"key": "10.1016/j.bbi.2021.04.022_b0150",
"unstructured": "Alcohol guidelines review–Report from the Guidelines development group to the UK Chief Medical Officers."
},
{
"DOI": "10.5694/j.1326-5377.1983.tb122565.x",
"article-title": "Effects of cigarette smoking on the immune system Follow-up studies in normal subjects after cessation of smoking",
"author": "Hersey",
"doi-asserted-by": "crossref",
"first-page": "425",
"journal-title": "Med. J. Aust.",
"key": "10.1016/j.bbi.2021.04.022_b0155",
"volume": "2",
"year": "1983"
},
{
"DOI": "10.1016/S0191-8869(98)00089-0",
"article-title": "Genetic and environmental influence on morningness-eveningness",
"author": "Hur",
"doi-asserted-by": "crossref",
"first-page": "917",
"journal-title": "Pers. Individ. Dif.",
"key": "10.1016/j.bbi.2021.04.022_b0160",
"volume": "25",
"year": "1998"
},
{
"DOI": "10.1111/j.1365-2796.2010.02332.x",
"article-title": "Smoking and the outcome of infection",
"author": "Huttunen",
"doi-asserted-by": "crossref",
"first-page": "258",
"journal-title": "J. Intern. Med.",
"key": "10.1016/j.bbi.2021.04.022_b0165",
"volume": "269",
"year": "2011"
},
{
"DOI": "10.1155/2015/678164",
"article-title": "The Bidirectional Relationship between Sleep and Immunity against Infections",
"author": "Ibarra-Coronado",
"doi-asserted-by": "crossref",
"journal-title": "J. Immunol. Res.",
"key": "10.1016/j.bbi.2021.04.022_b0170",
"volume": "2015",
"year": "2015"
},
{
"DOI": "10.2188/jea.17.194",
"article-title": "Risk and protective factors related to mortality from pneumonia among middle-aged and elderly community residents: The JACC study",
"author": "Inoue",
"doi-asserted-by": "crossref",
"first-page": "194",
"journal-title": "J. Epidemiol.",
"key": "10.1016/j.bbi.2021.04.022_b0175",
"volume": "17",
"year": "2007"
},
{
"DOI": "10.1146/annurev-psych-010213-115205",
"article-title": "Why sleep is important for health: A psychoneuroimmunology perspective",
"author": "Irwin",
"doi-asserted-by": "crossref",
"first-page": "143",
"journal-title": "Annu. Rev. Psychol.",
"key": "10.1016/j.bbi.2021.04.022_b0180",
"volume": "66",
"year": "2015"
},
{
"article-title": "Key Takeaways from the U.S. CDC’s 2019 Antibiotic Resistance Threats Report for Frontline Providers",
"author": "Kadri",
"journal-title": "Crit. Care Med.",
"key": "10.1016/j.bbi.2021.04.022_b0185",
"volume": "939–945",
"year": "2020"
},
{
"DOI": "10.1007/s10654-006-9037-6",
"article-title": "Calculating measures of biological interaction using R",
"author": "Källberg",
"doi-asserted-by": "crossref",
"first-page": "571",
"journal-title": "Eur. J. Epidemiol.",
"key": "10.1016/j.bbi.2021.04.022_b0190",
"volume": "21",
"year": "2006"
},
{
"DOI": "10.1086/587658",
"article-title": "The interaction between nutrition and infection",
"author": "Katona",
"doi-asserted-by": "crossref",
"first-page": "1582",
"journal-title": "Clin. Infect. Dis.",
"key": "10.1016/j.bbi.2021.04.022_b0195",
"volume": "46",
"year": "2008"
},
{
"DOI": "10.1136/bmj.h384",
"article-title": "All cause mortality and the case for age specific alcohol consumption guidelines: Pooled analyses of up to 10 population based cohorts",
"author": "Knott",
"doi-asserted-by": "crossref",
"journal-title": "BMJ",
"key": "10.1016/j.bbi.2021.04.022_b0200",
"volume": "350",
"year": "2015"
},
{
"DOI": "10.1111/j.1365-2869.2007.00580.x",
"article-title": "Heritability of diurnal type: A nationwide study of 8753 adult twin pairs",
"author": "Koskenvuo",
"doi-asserted-by": "crossref",
"first-page": "156",
"journal-title": "J. Sleep Res.",
"key": "10.1016/j.bbi.2021.04.022_b0205",
"volume": "16",
"year": "2007"
},
{
"author": "Lee",
"journal-title": "Combined Impact of Lifestyle Factors on Cancer Mortality in Men.",
"key": "10.1016/j.bbi.2021.04.022_b0210",
"year": "2011"
},
{
"article-title": "Advances in exercise immunology",
"author": "Mackinnon",
"journal-title": "Human Kinetics.",
"key": "10.1016/j.bbi.2021.04.022_b0215",
"year": "1999"
},
{
"DOI": "10.1001/jama.2016.11764",
"article-title": "Antimicrobial resistance",
"author": "Marston",
"doi-asserted-by": "crossref",
"first-page": "1193",
"journal-title": "JAMA - J. Am. Med. Assoc.",
"key": "10.1016/j.bbi.2021.04.022_b0220",
"volume": "316",
"year": "2016"
},
{
"DOI": "10.1097/00005768-200208000-00003",
"article-title": "Moderate to vigorous physical activity and risk of upper-respiratory tract infection",
"author": "Matthews",
"doi-asserted-by": "crossref",
"first-page": "1242",
"journal-title": "Med. Sci. Sport. Exerc.",
"key": "10.1016/j.bbi.2021.04.022_b0225",
"volume": "34",
"year": "2002"
},
{
"DOI": "10.1093/ajcn/76.6.1261",
"article-title": "Diet quality and major chronic disease risk in men and women: Moving toward improved dietary guidance",
"author": "McCullough",
"doi-asserted-by": "crossref",
"first-page": "1261",
"journal-title": "Am. J. Clin. Nutr.",
"key": "10.1016/j.bbi.2021.04.022_b0230",
"volume": "76",
"year": "2002"
},
{
"DOI": "10.1016/S0140-6736(11)61051-9",
"article-title": "Global burden of respiratory infections due to seasonal influenza in young children: A systematic review and meta-analysis",
"author": "Nair",
"doi-asserted-by": "crossref",
"first-page": "1917",
"journal-title": "Lancet",
"key": "10.1016/j.bbi.2021.04.022_b0235",
"volume": "378",
"year": "2011"
},
{
"DOI": "10.1055/s-2007-1021128",
"article-title": "Exercise, Infection, and Immunity",
"author": "Nieman",
"doi-asserted-by": "crossref",
"first-page": "S131",
"journal-title": "Int. J. Sports Med.",
"key": "10.1016/j.bbi.2021.04.022_b0240",
"volume": "15",
"year": "1994"
},
{
"DOI": "10.1136/bjsm.2010.077875",
"article-title": "Upper respiratory tract infection is reduced in physically fit and active adults",
"author": "Nieman",
"doi-asserted-by": "crossref",
"first-page": "987",
"journal-title": "Br. J. Sports Med.",
"key": "10.1016/j.bbi.2021.04.022_b0245",
"volume": "45",
"year": "2011"
},
{
"DOI": "10.1055/s-2007-1024839",
"article-title": "The effects of moderate exercise training on natural killer cells and acute upper respiratory tract infections",
"author": "Nieman",
"doi-asserted-by": "crossref",
"first-page": "467",
"journal-title": "Int. J. Sports Med.",
"key": "10.1016/j.bbi.2021.04.022_b0250",
"volume": "11",
"year": "1990"
},
{
"DOI": "10.1016/j.bbi.2015.03.011",
"article-title": "Sleep and immunity: A growing field with clinical impact",
"author": "Opp",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Brain. Behav. Immun.",
"key": "10.1016/j.bbi.2021.04.022_b0255",
"volume": "47",
"year": "2015"
},
{
"DOI": "10.1093/ije/dyx091",
"article-title": "Associations of obesity and lifestyle with the risk and mortality of bloodstream infection in a general population : a 15-year follow-up of 64 027 individuals in the HUNT Study",
"author": "Paulsen",
"doi-asserted-by": "crossref",
"first-page": "1573",
"journal-title": "Int. J. Epidemiol.",
"key": "10.1016/j.bbi.2021.04.022_b0260",
"volume": "46",
"year": "2017"
},
{
"DOI": "10.1136/bjsports-2016-096194",
"article-title": "Does physical activity moderate the association between alcohol drinking and all-cause, cancer and cardiovascular diseases mortality? A pooled analysis of eight British population cohorts",
"author": "Perreault",
"doi-asserted-by": "crossref",
"first-page": "651",
"journal-title": "Br. J. Sports Med.",
"key": "10.1016/j.bbi.2021.04.022_b0265",
"volume": "51",
"year": "2017"
},
{
"DOI": "10.1001/jamainternmed.2016.0787",
"article-title": "Association of insufficient sleep with respiratory infection among adults in the United States",
"author": "Prather",
"doi-asserted-by": "crossref",
"first-page": "850",
"journal-title": "JAMA Intern. Med.",
"key": "10.1016/j.bbi.2021.04.022_b0270",
"volume": "176",
"year": "2016"
},
{
"DOI": "10.1111/j.1360-0443.2010.02899.x",
"article-title": "The relation between different dimensions of alcohol consumption and burden of disease: An overview",
"author": "Rehm",
"doi-asserted-by": "crossref",
"first-page": "817",
"journal-title": "Addiction",
"key": "10.1016/j.bbi.2021.04.022_b0275",
"volume": "105",
"year": "2010"
},
{
"article-title": "New national alcohol guidelines in the UK: Public awareness, understanding and behavioural intentions",
"author": "Rosenberg",
"first-page": "549",
"journal-title": "J. Public Heal. (United Kingdom)",
"key": "10.1016/j.bbi.2021.04.022_b0280",
"volume": "40",
"year": "2018"
},
{
"DOI": "10.1016/S0140-6736(19)32989-7",
"article-title": "Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the Global Burden of Disease Study",
"author": "Rudd",
"doi-asserted-by": "crossref",
"first-page": "200",
"journal-title": "Lancet",
"key": "10.1016/j.bbi.2021.04.022_b0285",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/j.jshs.2020.05.005",
"article-title": "An international physical activity and public health research agenda to inform coronavirus disease-2019 policies and practices",
"author": "Sallis",
"doi-asserted-by": "crossref",
"first-page": "328",
"journal-title": "J. Sport Heal. Sci.",
"key": "10.1016/j.bbi.2021.04.022_b0290",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1017/S0950268810000774",
"article-title": "Alcohol consumption as a risk factor for pneumonia: A systematic review and meta-analysis",
"author": "Samokhvalov",
"doi-asserted-by": "crossref",
"first-page": "1789",
"journal-title": "Epidemiol. Infect.",
"key": "10.1016/j.bbi.2021.04.022_b0295",
"volume": "138",
"year": "2010"
},
{
"DOI": "10.1093/ajcn/66.2.464S",
"article-title": "Synergism of nutrition, infection, and immunity: An overview",
"author": "Scrimshaw",
"doi-asserted-by": "crossref",
"journal-title": "Am. J. Clin. Nutr.",
"key": "10.1016/j.bbi.2021.04.022_b0300",
"volume": "66",
"year": "1997"
},
{
"article-title": "Clinical and economic burden of community-acquired pneumonia amongst adults in the Asia-Pacific region",
"author": "Song",
"first-page": "108",
"journal-title": "Int. J. Antimicrob. Agents",
"key": "10.1016/j.bbi.2021.04.022_b0305",
"volume": "38",
"year": "2011"
},
{
"DOI": "10.1038/nri803",
"article-title": "Effects of cigarette smoke on the immune system",
"author": "Sopori",
"doi-asserted-by": "crossref",
"first-page": "372",
"journal-title": "Nat. Rev. Immunol.",
"key": "10.1016/j.bbi.2021.04.022_b0310",
"volume": "2",
"year": "2002"
},
{
"DOI": "10.1186/s12966-015-0280-7",
"article-title": "All-cause mortality effects of replacing sedentary time with physical activity and sleeping using an isotemporal substitution model: A prospective study of 201,129 mid-aged and older adults",
"author": "Stamatakis",
"doi-asserted-by": "crossref",
"journal-title": "Int. J. Behav. Nutr. Phys. Act.",
"key": "10.1016/j.bbi.2021.04.022_b0315",
"volume": "12",
"year": "2015"
},
{
"DOI": "10.1371/journal.pmed.1001779",
"article-title": "UK Biobank: An Open Access Resource for Identifying the Causes of a Wide Range of Complex Diseases of Middle and Old Age",
"author": "Sudlow",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "PLoS Med.",
"key": "10.1016/j.bbi.2021.04.022_b0320",
"volume": "12",
"year": "2015"
},
{
"DOI": "10.1016/S1473-3099(17)30485-1",
"article-title": "Surveillance for control of antimicrobial resistance",
"author": "Tacconelli",
"doi-asserted-by": "crossref",
"first-page": "e99",
"journal-title": "Lancet Infect. Dis.",
"key": "10.1016/j.bbi.2021.04.022_b0325",
"volume": "18",
"year": "2018"
},
{
"author": "Townsend",
"key": "10.1016/j.bbi.2021.04.022_b0330",
"series-title": "Health and deprivation: inequality and the North",
"year": "1988"
},
{
"key": "10.1016/j.bbi.2021.04.022_b0335",
"unstructured": "UK Biobank, 2007. UK Biobank: Protocol for a large-scale prospective epidemiological resource. UKBB-PROT-09-06 (Main Phase)."
},
{
"DOI": "10.1016/j.ypmed.2014.04.017",
"article-title": "Physical inactivity and long-term rates of community-acquired sepsis",
"author": "Wang",
"doi-asserted-by": "crossref",
"first-page": "58",
"journal-title": "Prev. Med. (Baltim)",
"key": "10.1016/j.bbi.2021.04.022_b0340",
"volume": "65",
"year": "2014"
},
{
"DOI": "10.1186/s12871-017-0405-4",
"article-title": "The role of increased body mass index in outcomes of sepsis: A systematic review and meta-analysis",
"author": "Wang",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "BMC Anesthesiol.",
"key": "10.1016/j.bbi.2021.04.022_b0345",
"volume": "17",
"year": "2017"
},
{
"DOI": "10.1136/thx.2009.129502",
"article-title": "Clinical and economic burden of community-acquired pneumonia among adults in Europe",
"author": "Welte",
"doi-asserted-by": "crossref",
"first-page": "71",
"journal-title": "Thorax",
"key": "10.1016/j.bbi.2021.04.022_b0350",
"volume": "67",
"year": "2012"
},
{
"DOI": "10.1016/j.vaccine.2010.05.030",
"article-title": "Clinical and economic burden of pneumococcal disease in older US adults",
"author": "Weycker",
"doi-asserted-by": "crossref",
"first-page": "4955",
"journal-title": "Vaccine",
"key": "10.1016/j.bbi.2021.04.022_b0355",
"volume": "28",
"year": "2010"
},
{
"DOI": "10.1093/aje/kwu222",
"article-title": "Sleep duration and total and cause-specific mortality in a large US cohort: Interrelationships with physical activity, sedentary behavior, and body mass index",
"author": "Xiao",
"doi-asserted-by": "crossref",
"first-page": "997",
"journal-title": "Am. J. Epidemiol.",
"key": "10.1016/j.bbi.2021.04.022_b0360",
"volume": "180",
"year": "2014"
}
],
"reference-count": 72,
"references-count": 72,
"relation": {},
"score": 1,
"short-container-title": [
"Brain, Behavior, and Immunity"
],
"short-title": [],
"source": "Crossref",
"subject": [
"Behavioral Neuroscience",
"Endocrine and Autonomic Systems",
"Immunology"
],
"subtitle": [],
"title": [
"Lifestyle risk factors and infectious disease mortality, including COVID-19, among middle aged and older adults: Evidence from a community-based cohort study in the United Kingdom"
],
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "96"
}
ahmadi2
