Obesity, walking pace and risk of severe COVID-19 and mortality: analysis of UK Biobank
et al., International Journal of Obesity, doi:10.1038/s41366-021-00771-z, Feb 2021
Exercise for COVID-19
9th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 68 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
UK Biobank retrospective 412,596 people, showing severe COVID-19 and COVID-19 mortality inversely associated with self-reported walking pace.
Standard of Care (SOC) for COVID-19 in the study country,
the United Kingdom, is very poor with very low average efficacy for approved treatments1.
The United Kingdom focused on expensive high-profit treatments, approving only one low-cost early treatment, which required a prescription and had limited adoption. The high-cost prescription treatment strategy reduces the probability of early treatment due to access and cost barriers, and eliminates complementary and synergistic benefits seen with many low-cost treatments.
|
risk of death, 45.3% lower, RR 0.55, p = 0.001, high activity levels 72 of 163,912 (0.0%), low activity levels 62 of 30,119 (0.2%), adjusted per study, inverted to make RR<1 favor high activity levels, odds ratio converted to relative risk, multivariable.
|
|
risk of severe case, 46.7% lower, RR 0.53, p < 0.001, high activity levels 291 of 163,912 (0.2%), low activity levels 180 of 30,119 (0.6%), adjusted per study, inverted to make RR<1 favor high activity levels, odds ratio converted to relative risk, multivariable.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Yates et al., 26 Feb 2021, retrospective, United Kingdom, peer-reviewed, 7 authors.
Obesity, walking pace and risk of severe COVID-19 and mortality: analysis of UK Biobank
International Journal of Obesity, doi:10.1038/s41366-021-00771-z
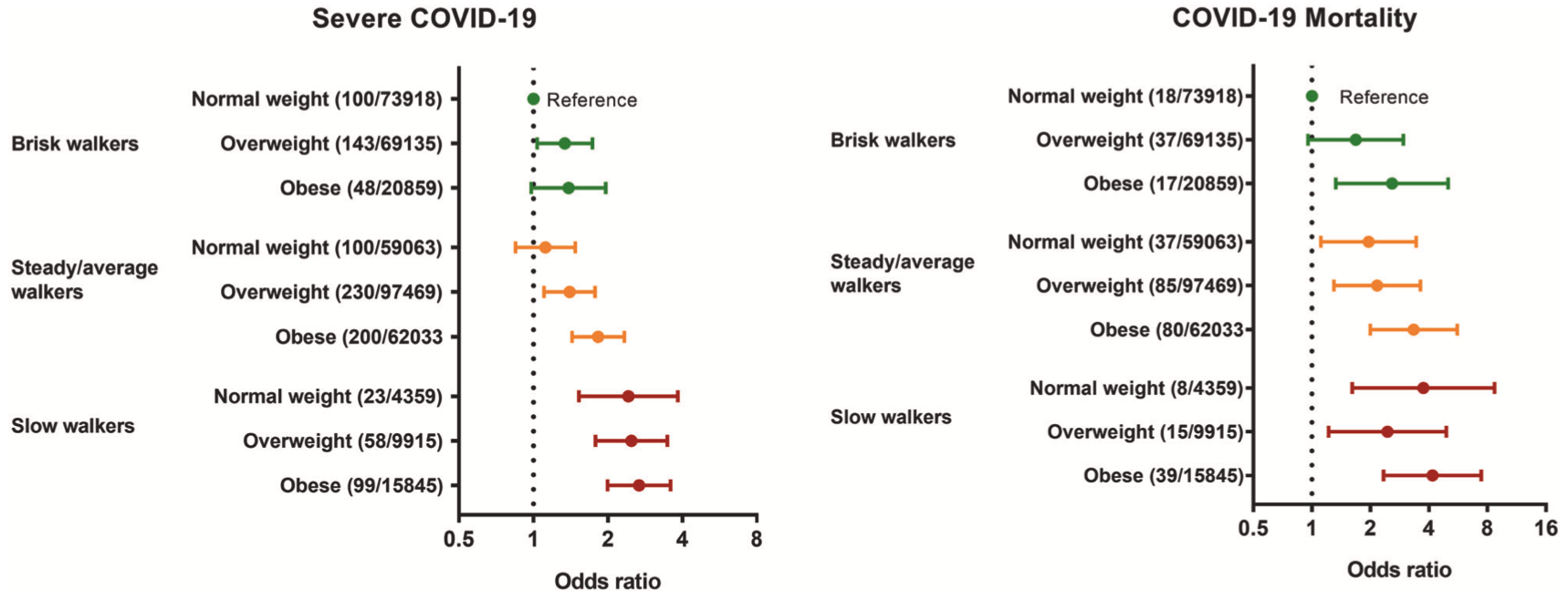
Obesity is an emerging risk factor for coronavirus disease-2019 (COVID-19). Simple measures of physical fitness, such as self-reported walking pace, may also be important risk markers. This analysis includes 412,596 UK Biobank participants with linked COVID-19 data (median age at linkage = 68 years, obese = 24%, median number of comorbidities = 1). As of August 24th 2020, there were 1001 cases of severe (in-hospital) disease and 336 COVID-19 deaths. Compared to normal weight individuals, the adjusted odds ratio (OR) of severe COVID-19 in overweight and obese individuals was 1.
Author contributions Concept and design: TY, CR, FZ, KK, Acquisition, analysis, or interpretation of data: All authors. Drafting of the manuscript: TY. Critical revision of the manuscript for important intellectual content: All authors. Statistical analysis: TY. Statistical support: FZ.
Compliance with ethical standards Conflict of interest Prof. Kamlesh Khunti is Chair of the UK SAGE subgroup on ethnicity and COVID-19. No other conflicts have been declared. Financial support This research was supported by the National Institute for Health Research (NIHR) Leicester Biomedical Research Centre, the NIHR Applied Research Collaboration -East Midlands, and a grant from the UKRI-DHSC COVID-19 Rapid Response Rolling Call (MR/V020536/1). The funder had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication. Publisher's note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Argyridou, Zaccardi, Davies, Khunti, Yates, Walking pace improves all-cause and cardiovascular mortality risk prediction: a UK Biobank prognostic study, Eur J Prev Cardiol
Armstrong, Rudkin, Allen, Crook, Wilson et al., Dynamic linkage of COVID-19 test results between Public Health England's Second Generation Surveillance System and UK Biobank, Microbial Genomics Online
Bayer, Krüger, Kries, Toschke, Factors associated with tracking of BMI: a meta-regression analysis on BMI tracking, Obesity
Hewitt, Carter, Vilches-Moraga, Quinn, Braude et al., The effect of frailty on survival in patients with COVID-19 (COPE): a multicentre, European, observational cohort study, Lancet Public Health
Kruglikov, Scherer, The role of adipocytes and adipocytelike cells in the severity of COVID-19 infections, Obesity
Lighter, Phillips, Hochman, Sterling, Johnson et al., Obesity in patients younger than 60 years is a risk factor for Covid-19 hospital admission, Clin Infect Dis
Maltese, Corsonello, Rosa, Soraci, Vitale et al., Frailty and COVID-19: a systematic scoping review, J Clin Med
Mertens, Clarys, Mullie, Lefevre, Charlier et al., Stability of physical activity, fitness components and diet quality indices, Eur J Clin Nutr
Michalakis, Ilias, SARS-CoV-2 infection and obesity: common inflammatory and metabolic aspects, Diabetes Metab Syndr
Seidu, Gillies, Zaccardi, Kunutsor, Hartmann-Boyce et al., The impact of obesity on severe disease and mortality in people with SARS-CoV-2: a systematic review and meta-analysis, Endocrinol Diabetes Metab
Simonnet, Chetboun, Poissy, Raverdy, Noulette et al., High prevalence of obesity in severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) requiring invasive mechanical ventilation, Obesity
Stamatakis, Kelly, Strain, Murtagh, Ding et al., Self-rated walking pace and all-cause, cardiovascular disease and cancer mortality: individual participant pooled analysis of 50,225 walkers from 11 population British cohorts, Br J Sports Med
Sudlow, Allen, Beral, Burton, UK Biobank: An Open Access Resource for Identifying the Causes of a Wide Range of Complex Diseases of Middle and Old Age, PLoS Med, doi:10.1371/journal.pmed.1001779
Williamson, Walker, Bhaskaran, Bacon, Bates et al., Factors associated with COVID-19-related death using OpenSAFELY, Nature
Yang, Zheng, Gou, Pu, Chen et al., Prevalence of comorbidities in the novel Wuhan coronavirus (COVID-19) infection: a systematic review and meta-analysis, Int J Infect Dis
Yates, Zaccardi, Dhalwani, Davies, Bakrania et al., Association of walking pace and handgrip strength with all-cause, cardiovascular, and cancer mortality: a UK Biobank observational study, Eur Heart J
Yates, Zaccardi, Razieh, Gillies, Rowlands et al., Framework to aid analysis and interpretation of ongoing COVID-19 research, Welcome Open Res
Zaccardi, Davies, Khunti, Yates, Comparative relevance of physical fitness and adiposity on life expectancy: a UK biobank observational study, Mayo Clin Proc
Zaccardi, Franks, Dudbridge, Davies, Khunti et al., Mortality risk comparing walking pace to handgrip strength and a healthy lifestyle: a UK Biobank study, Eur J Prev Cardiol
DOI record:
{
"DOI": "10.1038/s41366-021-00771-z",
"ISSN": [
"0307-0565",
"1476-5497"
],
"URL": "http://dx.doi.org/10.1038/s41366-021-00771-z",
"alternative-id": [
"771"
],
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "17 June 2020"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Revised",
"name": "revised",
"order": 2,
"value": "11 December 2020"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 3,
"value": "21 January 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 4,
"value": "26 February 2021"
},
{
"group": {
"label": "Compliance with ethical standards",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Conflict of interest",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "Prof. Kamlesh Khunti is Chair of the UK SAGE subgroup on ethnicity and COVID-19. No other conflicts have been declared."
},
{
"group": {
"label": "Financial support",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "This research was supported by the National Institute for Health Research (NIHR) Leicester Biomedical Research Centre, the NIHR Applied Research Collaboration – East Midlands, and a grant from the UKRI-DHSC COVID-19 Rapid Response Rolling Call (MR/V020536/1). The funder had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication."
},
{
"label": "Free to read",
"name": "free",
"value": "This content has been made available to all."
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-5724-5178",
"affiliation": [],
"authenticated-orcid": false,
"family": "Yates",
"given": "Thomas",
"sequence": "first"
},
{
"affiliation": [],
"family": "Razieh",
"given": "Cameron",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Zaccardi",
"given": "Francesco",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-1463-697X",
"affiliation": [],
"authenticated-orcid": false,
"family": "Rowlands",
"given": "Alex V.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Seidu",
"given": "Samuel",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Davies",
"given": "Melanie J.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-2343-7099",
"affiliation": [],
"authenticated-orcid": false,
"family": "Khunti",
"given": "Kamlesh",
"sequence": "additional"
}
],
"container-title": [
"International Journal of Obesity"
],
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2021,
2,
26
]
],
"date-time": "2021-02-26T18:05:15Z",
"timestamp": 1614362715000
},
"deposited": {
"date-parts": [
[
2021,
12,
2
]
],
"date-time": "2021-12-02T11:33:04Z",
"timestamp": 1638444784000
},
"indexed": {
"date-parts": [
[
2022,
3,
28
]
],
"date-time": "2022-03-28T22:52:20Z",
"timestamp": 1648507940544
},
"is-referenced-by-count": 20,
"issn-type": [
{
"type": "print",
"value": "0307-0565"
},
{
"type": "electronic",
"value": "1476-5497"
}
],
"issue": "5",
"issued": {
"date-parts": [
[
2021,
2,
26
]
]
},
"journal-issue": {
"issue": "5",
"published-print": {
"date-parts": [
[
2021,
5
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://www.springer.com/tdm",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
2,
26
]
],
"date-time": "2021-02-26T00:00:00Z",
"timestamp": 1614297600000
}
},
{
"URL": "https://www.springer.com/tdm",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
2,
26
]
],
"date-time": "2021-02-26T00:00:00Z",
"timestamp": 1614297600000
}
}
],
"link": [
{
"URL": "http://www.nature.com/articles/s41366-021-00771-z.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "http://www.nature.com/articles/s41366-021-00771-z",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "http://www.nature.com/articles/s41366-021-00771-z.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"page": "1155-1159",
"prefix": "10.1038",
"published": {
"date-parts": [
[
2021,
2,
26
]
]
},
"published-online": {
"date-parts": [
[
2021,
2,
26
]
]
},
"published-print": {
"date-parts": [
[
2021,
5
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.1016/j.ijid.2020.03.017",
"author": "J Yang",
"doi-asserted-by": "publisher",
"first-page": "91",
"journal-title": "Int J Infect Dis",
"key": "771_CR1",
"unstructured": "Yang J, Zheng Y, Gou X, Pu K, Chen Z, Guo Q, et al. Prevalence of comorbidities in the novel Wuhan coronavirus (COVID-19) infection: a systematic review and meta-analysis. Int J Infect Dis. 2020;94:91–95.",
"volume": "94",
"year": "2020"
},
{
"author": "S Seidu",
"journal-title": "Endocrinol Diabetes Metab",
"key": "771_CR2",
"unstructured": "Seidu S, Gillies C, Zaccardi F, Kunutsor SK, Hartmann‐Boyce J, Yates T, et al. The impact of obesity on severe disease and mortality in people with SARS‐CoV‐2: a systematic review and meta‐analysis. Endocrinol Diabetes Metab. 2020;14:e00176.",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2020.04.033",
"author": "K Michalakis",
"doi-asserted-by": "publisher",
"first-page": "469",
"journal-title": "Diabetes Metab Syndr",
"key": "771_CR3",
"unstructured": "Michalakis K, Ilias I. SARS-CoV-2 infection and obesity: common inflammatory and metabolic aspects. Diabetes Metab Syndr. 2020;14:469–71.",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.3390/jcm9072106",
"author": "G Maltese",
"doi-asserted-by": "publisher",
"first-page": "2106",
"journal-title": "J Clin Med",
"key": "771_CR4",
"unstructured": "Maltese G, Corsonello A, Di Rosa M, Soraci L, Vitale C, Corica F, et al. Frailty and COVID-19: a systematic scoping review. J Clin Med. 2020;9:2106.",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1016/S2468-2667(20)30146-8",
"author": "J Hewitt",
"doi-asserted-by": "publisher",
"first-page": "e444",
"journal-title": "Lancet Public Health",
"key": "771_CR5",
"unstructured": "Hewitt J, Carter B, Vilches-Moraga A, Quinn TJ, Braude P, Verduri A, et al. The effect of frailty on survival in patients with COVID-19 (COPE): a multicentre, European, observational cohort study. Lancet Public Health. 2020;5:e444–51.",
"volume": "5",
"year": "2020"
},
{
"DOI": "10.1093/eurheartj/ehx449",
"author": "T Yates",
"doi-asserted-by": "publisher",
"first-page": "3232",
"journal-title": "Eur Heart J",
"key": "771_CR6",
"unstructured": "Yates T, Zaccardi F, Dhalwani NN, Davies MJ, Bakrania K, Celis-Morales CA, et al. Association of walking pace and handgrip strength with all-cause, cardiovascular, and cancer mortality: a UK Biobank observational study. Eur Heart J. 2017;14:3232–40.",
"volume": "14",
"year": "2017"
},
{
"DOI": "10.1136/bjsports-2017-098677",
"author": "E Stamatakis",
"doi-asserted-by": "publisher",
"first-page": "761",
"journal-title": "Br J Sports Med",
"key": "771_CR7",
"unstructured": "Stamatakis E, Kelly P, Strain T, Murtagh EM, Ding D, Murphy MH. Self-rated walking pace and all-cause, cardiovascular disease and cancer mortality: individual participant pooled analysis of 50,225 walkers from 11 population British cohorts. Br J Sports Med. 2018;52:761–8.",
"volume": "52",
"year": "2018"
},
{
"DOI": "10.1016/j.mayocp.2018.10.029",
"author": "F Zaccardi",
"doi-asserted-by": "publisher",
"first-page": "985",
"journal-title": "Mayo Clin Proc",
"key": "771_CR8",
"unstructured": "Zaccardi F, Davies MJ, Khunti K, Yates T. Comparative relevance of physical fitness and adiposity on life expectancy: a UK biobank observational study. Mayo Clin Proc. 2019;94:985–94.",
"volume": "94",
"year": "2019"
},
{
"DOI": "10.1177/2047487319885041",
"author": "F Zaccardi",
"doi-asserted-by": "crossref",
"first-page": "204748731988504",
"journal-title": "Eur J Prev Cardiol",
"key": "771_CR9",
"unstructured": "Zaccardi F, Franks PW, Dudbridge F, Davies MJ, Khunti K, Yates T. Mortality risk comparing walking pace to handgrip strength and a healthy lifestyle: a UK Biobank study. Eur J Prev Cardiol. 2019;12:2047487319885041.",
"volume": "12",
"year": "2019"
},
{
"author": "S Argyridou",
"first-page": "204748731988728",
"journal-title": "Eur J Prev Cardiol",
"key": "771_CR10",
"unstructured": "Argyridou S, Zaccardi F, Davies MJ, Khunti K, Yates T. Walking pace improves all-cause and cardiovascular mortality risk prediction: a UK Biobank prognostic study. Eur J Prev Cardiol. 2019;7:2047487319887281.",
"volume": "7",
"year": "2019"
},
{
"DOI": "10.1371/journal.pmed.1001779",
"author": "C Sudlow",
"doi-asserted-by": "publisher",
"first-page": "e1001779",
"journal-title": "PLoS Med",
"key": "771_CR11",
"unstructured": "Sudlow C, Gallacher J, Allen N, Beral V, Burton P, Danesh J, et al. UK Biobank: An Open Access Resource for Identifying the Causes of a Wide Range of Complex Diseases of Middle and Old Age. PLoS Med. 2015;12:e1001779. https://doi.org/10.1371/journal.pmed.1001779.",
"volume": "12",
"year": "2015"
},
{
"author": "A Armstrong",
"first-page": "mgen000397",
"journal-title": "Microbial Genomics Online.",
"key": "771_CR12",
"unstructured": "Armstrong A, Rudkin JK, Allen N, Crook DW, Wilson DJ, Wyllie DH, et al. Dynamic linkage of COVID-19 test results between Public Health England’s Second Generation Surveillance System and UK Biobank. Microbial Genomics Online. 2020;6:mgen000397.",
"volume": "6",
"year": "2020"
},
{
"DOI": "10.12688/wellcomeopenres.16227.1",
"author": "T Yates",
"doi-asserted-by": "publisher",
"first-page": "208",
"journal-title": "Welcome Open Res.",
"key": "771_CR13",
"unstructured": "Yates T, Zaccardi F, Razieh C, Gillies CL, Rowlands A, Kloecker DE. et al. Framework to aid analysis and interpretation of ongoing COVID-19 research. Welcome Open Res.2020;5:208",
"volume": "5",
"year": "2020"
},
{
"DOI": "10.1038/s41586-020-2521-4",
"author": "EJ Williamson",
"doi-asserted-by": "publisher",
"first-page": "430",
"journal-title": "Nature.",
"key": "771_CR14",
"unstructured": "Williamson EJ, Walker AJ, Bhaskaran K, Bacon S, Bates C, Morton CE, et al. Factors associated with COVID-19-related death using OpenSAFELY. Nature. 2020;584:430–6.",
"volume": "584",
"year": "2020"
},
{
"DOI": "10.1002/oby.22856",
"author": "IL Kruglikov",
"doi-asserted-by": "publisher",
"first-page": "1187",
"journal-title": "Obesity.",
"key": "771_CR15",
"unstructured": "Kruglikov IL, Scherer PE. The role of adipocytes and adipocyte‐like cells in the severity of COVID‐19 infections. Obesity. 2020;28:1187–90.",
"volume": "28",
"year": "2020"
},
{
"DOI": "10.1093/cid/ciaa415",
"author": "J Lighter",
"doi-asserted-by": "publisher",
"first-page": "896",
"journal-title": "Clin Infect Dis",
"key": "771_CR16",
"unstructured": "Lighter J, Phillips M, Hochman S, Sterling S, Johnson D, Francois F, et al. Obesity in patients younger than 60 years is a risk factor for Covid-19 hospital admission. Clin Infect Dis. 2020;71:896–897.",
"volume": "71",
"year": "2020"
},
{
"DOI": "10.1002/oby.22831",
"author": "A Simonnet",
"doi-asserted-by": "publisher",
"first-page": "1195",
"journal-title": "Obesity.",
"key": "771_CR17",
"unstructured": "Simonnet A, Chetboun M, Poissy J, Raverdy V, Noulette J, Duhamel A, et al. High prevalence of obesity in severe acute respiratory syndrome coronavirus‐2 (SARS‐CoV‐2) requiring invasive mechanical ventilation. Obesity. 2020;28:1195–1199.",
"volume": "28",
"year": "2020"
},
{
"DOI": "10.1038/oby.2010.250",
"author": "O Bayer",
"doi-asserted-by": "publisher",
"first-page": "1069",
"journal-title": "Obesity.",
"key": "771_CR18",
"unstructured": "Bayer O, Krüger H, Von Kries R, Toschke AM. Factors associated with tracking of BMI: a meta‐regression analysis on BMI tracking. Obesity. 2011;19:1069–76.",
"volume": "19",
"year": "2011"
},
{
"DOI": "10.1038/ejcn.2016.172",
"author": "E Mertens",
"doi-asserted-by": "publisher",
"first-page": "519",
"journal-title": "Eur J Clin Nutr",
"key": "771_CR19",
"unstructured": "Mertens E, Clarys P, Mullie P, Lefevre J, Charlier R, Knaeps S, et al. Stability of physical activity, fitness components and diet quality indices. Eur J Clin Nutr. 2017;71:519–24.",
"volume": "71",
"year": "2017"
}
],
"reference-count": 19,
"references-count": 19,
"relation": {},
"resource": {
"primary": {
"URL": "http://www.nature.com/articles/s41366-021-00771-z"
}
},
"score": 1,
"short-container-title": [
"Int J Obes"
],
"short-title": [],
"source": "Crossref",
"subject": [
"Nutrition and Dietetics",
"Endocrinology, Diabetes and Metabolism",
"Medicine (miscellaneous)"
],
"subtitle": [],
"title": [
"Obesity, walking pace and risk of severe COVID-19 and mortality: analysis of UK Biobank"
],
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "45"
}
