Nutritional Immunity, Zinc Sufficiency, and COVID-19 Mortality in Socially Similar European Populations
et al., Frontiers in Immunology, doi:10.3389/fimmu.2021.699389, Sep 2021
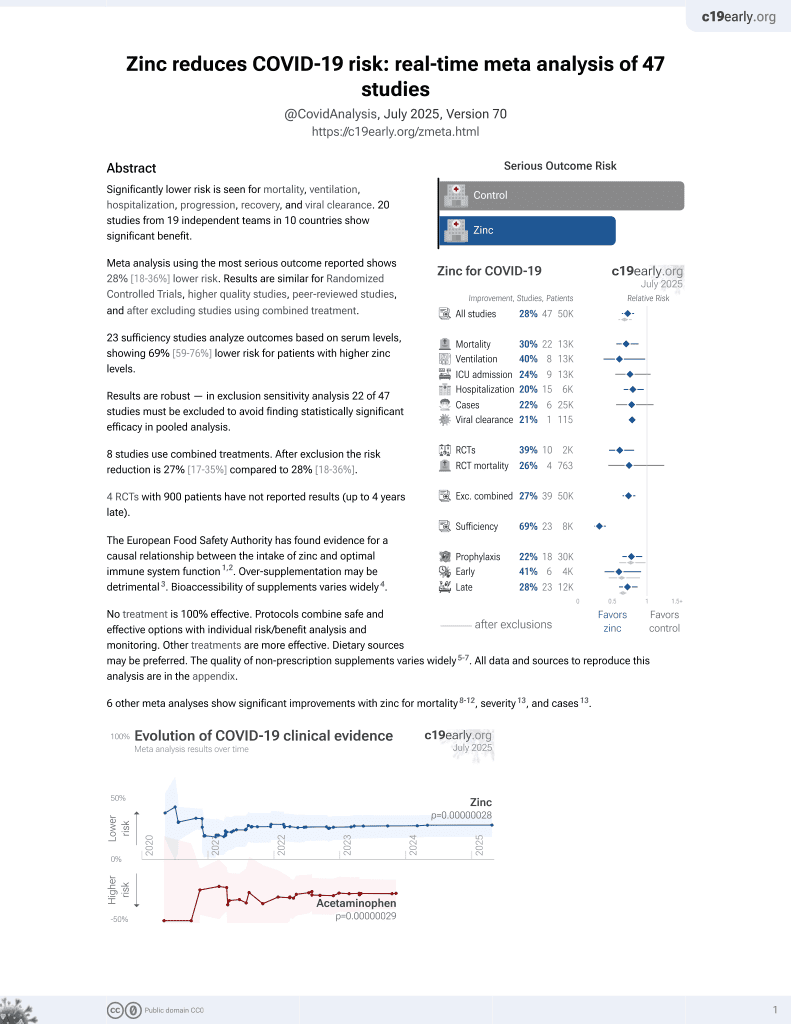
Zinc for COVID-19
2nd treatment shown to reduce risk in
July 2020, now with p = 0.00000012 from 41 studies, recognized in 23 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
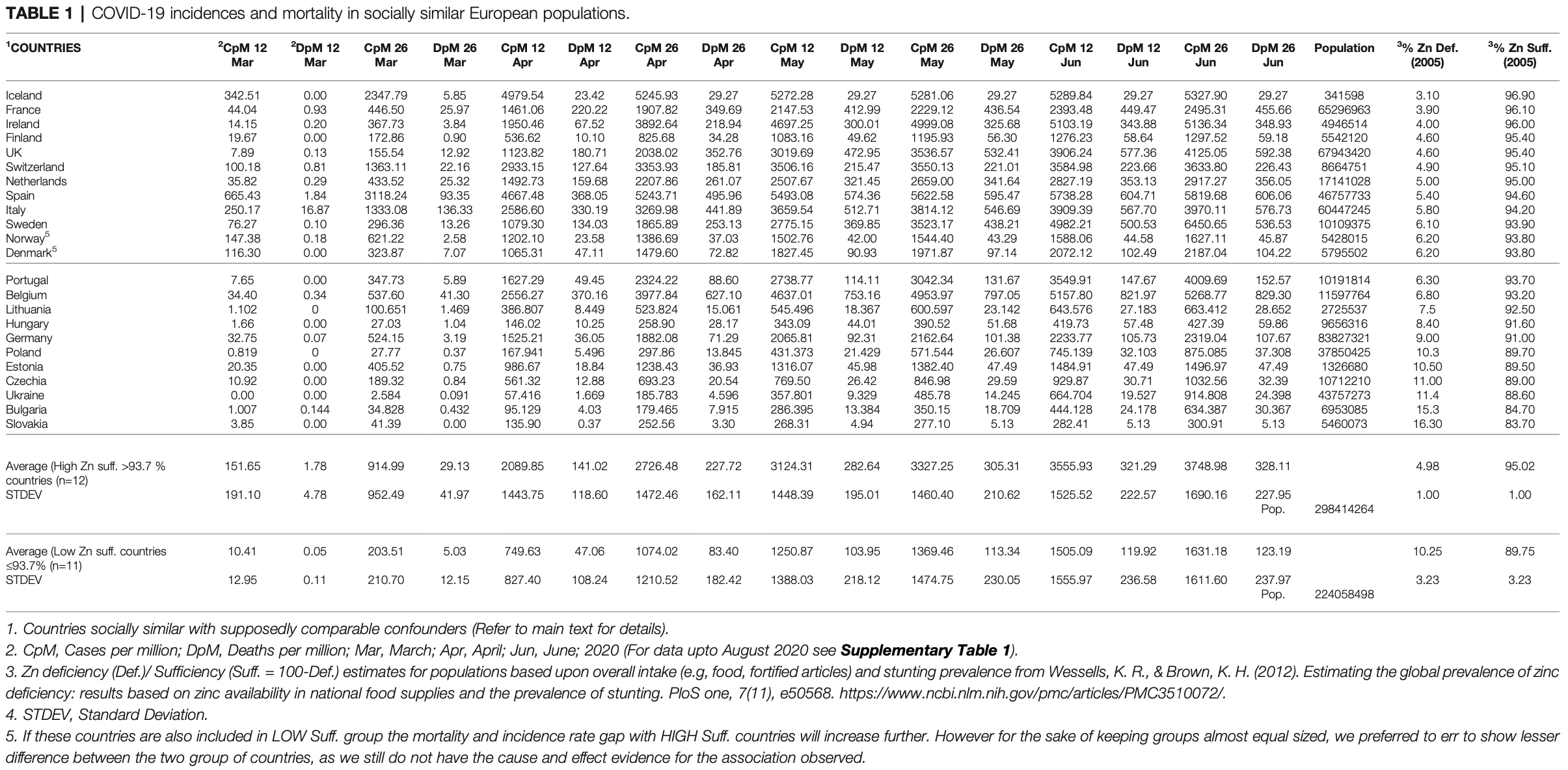
Analysis of zinc sufficiency showing a positive correlation between sufficiency and COVID-19 within European countries.
Unmeasured confounders are likely to be significant, for example the higher sufficiency countries also have significantly higher tourism and international travel on average. This confounder is not mentioned and could more than account for the observation.
Sufficiency levels were relatively high in all countries. Zinc sufficiency estimates were from 2005.
Higher sufficiency countries: Iceland France Ireland Finland UK Switzerland Netherlands Spain Italy Sweden Norway Denmark
Lower sufficiency countries: Portugal Belgium Lithuania Hungary Germany Poland Estonia Czechia Ukraine Bulgaria Slovakia
Lower sufficiency countries: Portugal Belgium Lithuania Hungary Germany Poland Estonia Czechia Ukraine Bulgaria Slovakia
Singh et al., 17 Sep 2021, peer-reviewed, 4 authors.
Contact: samer.singh10@bhu.ac.in.
Nutritional Immunity, Zinc Sufficiency, and COVID-19 Mortality in Socially Similar European Populations
Frontiers in Immunology, doi:10.3389/fimmu.2021.699389
The impact of zinc (Zn) sufficiency/supplementation on COVID-19-associated mortality and incidence (SARS-CoV-2 infections) remains unknown. During an infection, the levels of free Zn are reduced as part of "nutritional immunity" to limit the growth and replication of pathogen and the ensuing inflammatory damage. Considering its key role in immune competency and frequently recorded deficiency in large sections of different populations, Zn has been prescribed for both prophylactic and therapeutic purposes in COVID-19 without any corroborating evidence for its protective role. Multiple trials are underway evaluating the effect of Zn supplementation on COVID-19 outcome in patients getting standard of care treatment. However, the trial designs presumably lack the power to identify negative effects of Zn supplementation, especially in the vulnerable groups of elderly and patients with comorbidities (contributing 9 out of 10 deaths; up to >8,000-fold higher mortality). In this study, we have analyzed COVID-19 mortality and incidence (case) data from 23 socially similar European populations with comparable confounders (population: 522.47 million; experiencing up to >150-fold difference in death rates) and at the matching stage of the pandemic (March 12 to June 26, 2020; first wave of COVID-19 incidence and mortality). Our results suggest a positive correlation between populations' Zn-sufficiency status and COVID-19 mortality [r (23): 0.7893-0.6849, pvalue < 0.0003] as well as incidence [r (23):0.8084-0.5658; p-value < 0.005]. The observed association is contrary to what would be expected if Zn sufficiency was protective in COVID-19. Thus, controlled trials or retrospective analyses of the adverse event patients' data should be undertaken to correctly guide the practice of Zn supplementation in COVID-19.
ETHICS STATEMENT Ethical review and approval were not required for the study on human participants in accordance with the local legislation and institutional requirements. Written informed consent for participation was not required for this study in accordance with the national legislation and the institutional requirements.
AUTHOR CONTRIBUTIONS SS conceived the idea, collected the data, and wrote the manuscript. AD, BPS and RKS provided the necessary inputs and helped in data analysis and writing. All authors contributed to the article and approved the submitted version.
SUPPLEMENTARY MATERIAL The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fimmu.2021.
699389/full#supplementary-material Supplementary Table 1 | COVID-19 incidences and mortality in socially similar European populations up to 26 August 2020.
Conflict of Interest: The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. Publisher's Note: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
Agnew, Slesinger, Zinc Toxicity
Arlehamna, Settea, Peters, Lack of Evidence for BCG Vaccine Protection From Severe COVID-19, PNAS, doi:10.1073/pnas.2016733117
Aydemir, Chang, Guthrie, Maki, Ryu et al., Zinc Transporter ZIP14 Functions in Hepatic Zinc, Iron and Glucose Homeostasis During the Innate Immune Response (Endotoxemia), PloS One, doi:10.1371/journal.pone.0048679
Bao, Knoell, Zinc Modulates Airway Epithelium Susceptibility to Death Receptor-Mediated Apoptosis, Am J Physiol -Lung Cell Mol Physiol, doi:10.1152/ajplung.00341.2005
Besold, Gilston, Radin, Ramsoomair, Culbertson et al., Role of Calprotectin in Withholding Zinc and Copper From Candida Albicans, Infect Immun, doi:10.1128/IAI.00779-17
Bonaventura, Benedetti, Albarède, Miossec, Zinc and Its Role in Immunity and Inflammation, Autoimmun Rev, doi:10.1016/j.autrev.2014.11.008
Briggs, Briggs, Austin, Effects of Steroid Pharmaceuticals on Plasma Zinc, Nature, doi:10.1038/232480a0
Brown, Effect of Infections on Plasma Zinc Concentration and Implications for Zinc Status Assessment in Low-Income Countries, Am J Clin Nutr, doi:10.1093/ajcn/68.2.425S
Cabrera, Zinc, Aging, and Immunosenescence: An Overview, Pathobiol Aging Age-Relat Dis, doi:10.3402/pba.v5.25592
Calder, Carr, Gombart, Eggersdorfer, Optimal Nutritional Status for a Well-Functioning Immune System Is an Important Factor to Protect Against Viral Infections, Nutrients, doi:10.3390/nu12041181
Corbin, Seeley, Raab, Feldmann, Miller et al., Metal Chelation and Inhibition of Bacterial Growth in Tissue Abscesses, Science, doi:10.1126/science.1152449
De Faria Coelho-Ravagnani, Corgosinho, Sanches, Prado, Laviano et al., Dietary Recommendations During the COVID-19 Pandemic, Nutr Rev, doi:10.1093/nutrit/nuaa067
Ellul-Micallef, Galdes, Fenech, Serum Zinc Levels in Corticosteroid-Treated Asthmatic Patients, Postgrad Med J, doi:10.1136/pgmj.52.605.148
Escobara, Molina-Cruzb, Barillas-Mury, BCG Vaccine Protection From Severe Coronavirus Disease 2019 (COVID-19), Proc Natl Acad, doi:10.1073/pnas.2008410117
Freiberg, Cheng, Gnatienko, Blokhina, Coleman et al., Effect of Zinc Supplementation vs Placebo on Mortality Risk and HIV Disease Progression Among HIV-Positive Adults With Heavy Alcohol Use: A Randomized Clinical Trial, JAMA Netw Open, doi:10.1001/jamanetworkopen.2020.4330
Gombart, Pierre, Maggini, A Review of Micronutrients and the Immune System-Working in Harmony to Reduce the Risk of Infection, Nutrients, doi:10.3390/nu12010236
Grobler, Nagpal, Sudarsanam, Sinclair, Nutritional Supplements for People Being Treated for Active Tuberculosis, Cochrane Database Systematic Rev, doi:10.1002/14651858.CD006086.pub4
Hanada, Sawamura, Nakano, Hashimoto, Possible Role of 1,25-Dihydroxyvitamin D3-Induced Metallothionein in Photoprotection Against UVB Injury in Mouse Skin and Cultured Rat Keratinocytes, J Dermatol Sci, doi:10.1016/0923-1811(94)00378-r
Hess, Peerson, King, Brown, Use of Serum Zinc Concentration as an Indicator of Population Zinc Status, Food Nutr Bull, doi:10.1177/15648265070283S303
Hood, Skaar, Nutritional Immunity: Transition Metals at the Pathogen-Host Interface, Nat Rev Microbiol, doi:10.1038/nrmicro2836
Hunter, Chazin, High Level Expression and Dimer Characterization of the S100 EF-Hand Proteins, Migration Inhibitory Factor-Related Proteins 8 and 14, J Biol Chem, doi:10.1074/jbc.273.20.12427
Karin, Herschman, Induction of Metallothionein in HeLa Cells by Dexamethasone and Zinc, Eur J Biochem, doi:10.1111/j.1432-1033.1981.tb05062.x
Khawaja, Mohan, Jabbour, Bampouri, Bowsher et al., COVID-19 and Its Impact on the Cardiovascular System, Open Heart, doi:10.1136/openhrt-2020-001472
Kimura, Kambe, The Functions of Metallothionein and ZIP and ZnT Transporters: An Overview and Perspective, Int J Mol Sci, doi:10.3390/ijms17030336
Kobayashi, Okada, Kimura, Effects of Dexamethasone on Metallothionein Induction by Zn, Cu, and Cd in Chang Liver Cells, Chem Biol Interact, doi:10.1016/s0009-2797(85)80141-1
Lonergan, Skaar, Nutrient Zinc at the Host-Pathogen Interface, Trends Biochem Sci, doi:10.1016/j.tibs.2019.06.010
Maret, The Redox Biology of Redox-Inert Zinc Ions, Free Radical Biol Med, doi:10.1016/j.freeradbiomed.2019.01.006
Mayo-Wilson, Junior, Imdad, Dean, Chan et al., Zinc Supplementation for Preventing Mortality, Morbidity, and Growth Failure in Children Aged 6 Months to 12 Years of Age, Cochrane Database Syst Rev, doi:10.1002/14651858.CD009384.pub2
Milton, Vashum, Mcevoy, Hussain, Mcelduff et al., Prospective Study of Dietary Zinc Intake and Risk of Cardiovascular Disease in Women, Nutrients, doi:10.3390/nu10010038
Nishime, Kondo, Saito, Miyawaki, Nakagawa, Zinc Burden Evokes Copper Deficiency in the Hypoalbuminemic Hemodialysis Patients, Nutrients, doi:10.3390/nu12020577
Palmer, Skaar, Transition Metals and Virulence in Bacteria, Annu Rev Genet, doi:10.1146/annurev-genet-120215-035146
Prasad, Brewer, Schoomaker, Rabbani, Hypocupremia Induced by Zinc Therapy in Adults, JAMA, doi:10.1001/jama.1978.03290200044019
Prasad, Discovery of Human Zinc Deficiency: Its Impact on Human Health and Disease, Adv Nutr, doi:10.3945/an.112.003210
Pyle, Azad, Papp, Sadee, Knoell et al., Elemental Ingredients in the Macrophage Cocktail: Role of ZIP8 in Host Response to Mycobacterium Tuberculosis, Int J Mol Sci, doi:10.3390/ijms18112375
Qu, Yang, Yu, Jia, Qiao et al., Serum Zinc Levels and Multiple Health Outcomes: Implications for Zinc-Based Biomaterials, Bioact Mater, doi:10.1016/j.bioactmat.2020.03.006
Read, Obeid, Ahlenstiel, Ahlenstiel, The Role of Zinc in Antiviral Immunity, Adv Nutr, doi:10.1093/advances/nmz013
Rink, Haase, Zinc Homeostasis and Immunity, Trends Immunol, doi:10.1016/j.it.2006.11.005
Rochwerg, Siemieniuk, Agoritsas, Lamontagne, Askie et al., A Living WHO Guideline on Drugs for Covid-19, BMJ, doi:10.1136/bmj.m3379
Siemieniuk, Bartoszko, Ge, Zeraatkar, Izcovich et al., Drug Treatments for Covid-19: Living Systematic Review and Network Meta-Analysis, BMJ, doi:10.1136/bmj.m2980
Singh, BCG Vaccines May Not Reduce Covid-19 Mortality Rates, medRxiv, doi:10.1101/2020.04.11.20062232
Singh, Covariation of Zinc Deficiency With COVID-19 Infections and Mortality in European Countries: Is Zinc Deficiency a Risk Factor for COVID-19? medRxiv, Journal of Scientific Research, doi:10.37398/JSR.2020.640222
Singh, Kaur, Singh, Revisiting the Role of Vitamin D Levels in the Prevention of COVID-19 Infection and Mortality in European Countries Post Infections Peak, Aging Clin Exp Res, doi:10.1007/s40520-020-01619-8
Singh, Maurya, Singh, Trained Immunity" From Mycobacterium Spp. Exposure or BCG Vaccination and COVID-19 Outcomes, PloS Pathog, doi:10.1371/journal.ppat.1008969
Velthuis, Van Den Worm, Sims, Baric, Snijder et al., Zn(2+) Inhibits Coronavirus and Arterivirus RNA Polymerase Activity In Vitro and Zinc Ionophores Block the Replication of These Viruses in Cell Culture, PloS Pathog, doi:10.1371/journal.ppat.1001176
Vogl, Tenbrock, Ludwig, Leukert, Ehrhardt et al., Mrp8 and Mrp14 Are Endogenous Activators of Toll-Like Receptor 4, Promoting Lethal, Endotoxin-Induced Shock, Nat Med, doi:10.1038/nm1638
Wang, Lonergan, Gonzalez-Gutierrez, Nairn, Maxwell et al., Multi-Metal Restriction by Calprotectin Impacts De Novo Flavin Biosynthesis in Acinetobacter Baumannii, Cell Chem Biol, doi:10.1016/j.chembiol.2019.02.011
Wessells, Brown, Estimating the Global Prevalence of Zinc Deficiency: Results Based on Zinc Availability in National Food Supplies and the Prevalence of Stunting, PloS One, doi:10.1371/journal.pone.0050568
Wessels, Rolles, Rink, The Potential Impact of Zinc Supplementation on COVID-19 Pathogenesis, Front Immunol, doi:10.3389/fimmu.2020.01712
Worldometer, Life Expectancy of the World Population
Yui, Nakatani, Mikami, Calprotectin (S100A8/S100A9), an Inflammatory Protein Complex From Neutrophils With a Broad Apoptosis-Inducing Activity, Biol Pharm Bull, doi:10.1248/bpb.26.753
Yunice, Czerwinski, Lindeman, Influence of Synthetic Corticosteroids on Plasma Zinc and Copper Levels in Humans, Am J Med Sci, doi:10.1097/00000441-198109000-00003
DOI record:
{
"DOI": "10.3389/fimmu.2021.699389",
"ISSN": [
"1664-3224"
],
"URL": "http://dx.doi.org/10.3389/fimmu.2021.699389",
"abstract": "<jats:p>The impact of zinc (Zn) sufficiency/supplementation on COVID-19-associated mortality and incidence (SARS-CoV-2 infections) remains unknown. During an infection, the levels of free Zn are reduced as part of “nutritional immunity” to limit the growth and replication of pathogen and the ensuing inflammatory damage. Considering its key role in immune competency and frequently recorded deficiency in large sections of different populations, Zn has been prescribed for both prophylactic and therapeutic purposes in COVID-19 without any corroborating evidence for its protective role. Multiple trials are underway evaluating the effect of Zn supplementation on COVID-19 outcome in patients getting standard of care treatment. However, the trial designs presumably lack the power to identify negative effects of Zn supplementation, especially in the vulnerable groups of elderly and patients with comorbidities (contributing 9 out of 10 deaths; up to &gt;8,000-fold higher mortality). In this study, we have analyzed COVID-19 mortality and incidence (case) data from 23 socially similar European populations with comparable confounders (population: 522.47 million; experiencing up to &gt;150-fold difference in death rates) and at the matching stage of the pandemic (March 12 to June 26, 2020; first wave of COVID-19 incidence and mortality). Our results suggest a positive correlation between populations’ Zn-sufficiency status and COVID-19 mortality [<jats:italic>r</jats:italic> (23): 0.7893–0.6849, p-value &lt; 0.0003] as well as incidence [<jats:italic>r</jats:italic> (23):0.8084–0.5658; p-value &lt; 0.005]. The observed association is contrary to what would be expected if Zn sufficiency was protective in COVID-19. Thus, controlled trials or retrospective analyses of the adverse event patients’ data should be undertaken to correctly guide the practice of Zn supplementation in COVID-19.</jats:p>",
"alternative-id": [
"10.3389/fimmu.2021.699389"
],
"author": [
{
"affiliation": [],
"family": "Singh",
"given": "Samer",
"sequence": "first"
},
{
"affiliation": [],
"family": "Diwaker",
"given": "Amita",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Singh",
"given": "Brijesh P.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Singh",
"given": "Rakesh K.",
"sequence": "additional"
}
],
"container-title": "Frontiers in Immunology",
"container-title-short": "Front. Immunol.",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"frontiersin.org"
]
},
"created": {
"date-parts": [
[
2021,
9,
17
]
],
"date-time": "2021-09-17T04:28:53Z",
"timestamp": 1631852933000
},
"deposited": {
"date-parts": [
[
2021,
9,
17
]
],
"date-time": "2021-09-17T04:29:24Z",
"timestamp": 1631852964000
},
"indexed": {
"date-parts": [
[
2024,
4,
27
]
],
"date-time": "2024-04-27T15:13:04Z",
"timestamp": 1714230784808
},
"is-referenced-by-count": 15,
"issued": {
"date-parts": [
[
2021,
9,
17
]
]
},
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
9,
17
]
],
"date-time": "2021-09-17T00:00:00Z",
"timestamp": 1631836800000
}
}
],
"link": [
{
"URL": "https://www.frontiersin.org/articles/10.3389/fimmu.2021.699389/full",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1965",
"original-title": [],
"prefix": "10.3389",
"published": {
"date-parts": [
[
2021,
9,
17
]
]
},
"published-online": {
"date-parts": [
[
2021,
9,
17
]
]
},
"publisher": "Frontiers Media SA",
"reference": [
{
"DOI": "10.1016/j.tibs.2019.06.010",
"article-title": "Nutrient Zinc at the Host–Pathogen Interface",
"author": "Lonergan",
"doi-asserted-by": "publisher",
"journal-title": "Trends Biochem Sci",
"key": "B1",
"volume": "44",
"year": "2019"
},
{
"DOI": "10.1016/j.freeradbiomed.2019.01.006",
"article-title": "The Redox Biology of Redox-Inert Zinc Ions",
"author": "Maret",
"doi-asserted-by": "publisher",
"journal-title": "Free Radical Biol Med",
"key": "B2",
"volume": "134",
"year": "2019"
},
{
"DOI": "10.3945/an.112.003210",
"article-title": "Discovery of Human Zinc Deficiency: Its Impact on Human Health and Disease",
"author": "Prasad",
"doi-asserted-by": "publisher",
"journal-title": "Adv Nutr",
"key": "B3",
"volume": "4",
"year": "2013"
},
{
"DOI": "10.1093/nutrit/nuaa067",
"article-title": "Dietary Recommendations During the COVID-19 Pandemic",
"author": "de Faria Coelho-Ravagnani",
"doi-asserted-by": "publisher",
"journal-title": "Nutr Rev",
"key": "B4",
"volume": "79",
"year": "2021"
},
{
"DOI": "10.3390/nu12041181",
"article-title": "Optimal Nutritional Status for a Well-Functioning Immune System Is an Important Factor to Protect Against Viral Infections",
"author": "Calder",
"doi-asserted-by": "publisher",
"first-page": "1181",
"journal-title": "Nutrients",
"key": "B5",
"volume": "12",
"year": "2020"
},
{
"key": "B6",
"unstructured": "National Institutes of HealthCOVID-19 Treatment Guidelines Panel. Coronavirus Disease 2019 (COVID-19) Treatment Guidelines"
},
{
"DOI": "10.3389/fimmu.2020.01712",
"article-title": "The Potential Impact of Zinc Supplementation on COVID-19 Pathogenesis",
"author": "Wessels",
"doi-asserted-by": "publisher",
"journal-title": "Front Immunol",
"key": "B7",
"volume": "11",
"year": "2020"
},
{
"key": "B8",
"unstructured": ""
},
{
"key": "B9",
"unstructured": ""
},
{
"key": "B10",
"unstructured": ""
},
{
"key": "B11",
"unstructured": ""
},
{
"DOI": "10.1093/advances/nmz013",
"article-title": "The Role of Zinc in Antiviral Immunity",
"author": "Read",
"doi-asserted-by": "publisher",
"first-page": "696",
"journal-title": "Adv Nutr",
"key": "B12",
"volume": "10",
"year": "2019"
},
{
"DOI": "10.1371/journal.ppat.1001176",
"article-title": "Zn(2+) Inhibits Coronavirus and Arterivirus RNA Polymerase Activity In Vitro and Zinc Ionophores Block the Replication of These Viruses in Cell Culture",
"author": "te Velthuis",
"doi-asserted-by": "publisher",
"first-page": "e1001176",
"journal-title": "PloS Pathog",
"key": "B13",
"volume": "6",
"year": "2010"
},
{
"DOI": "10.1371/journal.pone.0050568",
"article-title": "Estimating the Global Prevalence of Zinc Deficiency: Results Based on Zinc Availability in National Food Supplies and the Prevalence of Stunting",
"author": "Wessells",
"doi-asserted-by": "publisher",
"first-page": "e50568",
"journal-title": "PloS One",
"key": "B14",
"volume": "7",
"year": "2012"
},
{
"DOI": "10.1001/jama.1978.03290200044019",
"article-title": "Hypocupremia Induced by Zinc Therapy in Adults",
"author": "Prasad",
"doi-asserted-by": "publisher",
"journal-title": "JAMA",
"key": "B15",
"volume": "240",
"year": "1978"
},
{
"DOI": "10.1016/j.autrev.2014.11.008",
"article-title": "Zinc and Its Role in Immunity and Inflammation",
"author": "Bonaventura",
"doi-asserted-by": "publisher",
"journal-title": "Autoimmun Rev",
"key": "B16",
"volume": "14",
"year": "2015"
},
{
"DOI": "10.3390/ijms17030336",
"article-title": "The Functions of Metallothionein and ZIP and ZnT Transporters: An Overview and Perspective",
"author": "Kimura",
"doi-asserted-by": "publisher",
"first-page": "336",
"journal-title": "Int J Mol Sci",
"key": "B17",
"volume": "17",
"year": "2016"
},
{
"DOI": "10.1016/j.it.2006.11.005",
"article-title": "Zinc Homeostasis and Immunity",
"author": "Rink",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Trends Immunol",
"key": "B18",
"volume": "28",
"year": "2007"
},
{
"DOI": "10.1038/nrmicro2836",
"article-title": "Nutritional Immunity: Transition Metals at the Pathogen–Host Interface",
"author": "Hood",
"doi-asserted-by": "publisher",
"journal-title": "Nat Rev Microbiol",
"key": "B19",
"volume": "10",
"year": "2012"
},
{
"DOI": "10.3390/nu12020577",
"article-title": "Zinc Burden Evokes Copper Deficiency in the Hypoalbuminemic Hemodialysis Patients",
"author": "Nishime",
"doi-asserted-by": "publisher",
"journal-title": "Nutrients",
"key": "B20",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3390/nu10010038",
"article-title": "Prospective Study of Dietary Zinc Intake and Risk of Cardiovascular Disease in Women",
"author": "Milton",
"doi-asserted-by": "publisher",
"journal-title": "Nutrients",
"key": "B21",
"volume": "10",
"year": "2018"
},
{
"DOI": "10.1016/j.bioactmat.2020.03.006",
"article-title": "Serum Zinc Levels and Multiple Health Outcomes: Implications for Zinc-Based Biomaterials",
"author": "Qu",
"doi-asserted-by": "publisher",
"journal-title": "Bioact Mater",
"key": "B22",
"volume": "5",
"year": "2020"
},
{
"key": "B23",
"volume-title": "Your Health: People With Certain Medical Conditions",
"year": "2020"
},
{
"key": "B24",
"unstructured": "COVID-19 Coronavirus Pandemic"
},
{
"key": "B25",
"unstructured": "Coronavirus Pandemic (COVID-19). Healthcare Access and Quality Index. Life ExpectancyMedian Age2020"
},
{
"DOI": "10.1371/journal.ppat.1008969",
"article-title": "“Trained Immunity” From Mycobacterium Spp. Exposure or BCG Vaccination and COVID-19 Outcomes",
"author": "Singh",
"doi-asserted-by": "publisher",
"first-page": "e1008969",
"journal-title": "PloS Pathog",
"key": "B26",
"volume": "16",
"year": "2020"
},
{
"DOI": "10.1101/2020.04.11.20062232",
"article-title": "BCG Vaccines May Not Reduce Covid-19 Mortality Rates",
"author": "Singh",
"doi-asserted-by": "publisher",
"journal-title": "medRxiv",
"key": "B27",
"year": "2020"
},
{
"DOI": "10.1073/pnas.2008410117",
"article-title": "BCG Vaccine Protection From Severe Coronavirus Disease 2019 (COVID-19)",
"author": "Escobara",
"doi-asserted-by": "publisher",
"journal-title": "Proc Natl Acad USA",
"key": "B28",
"volume": "117",
"year": "2020"
},
{
"DOI": "10.1007/s40520-020-01619-8",
"article-title": "Revisiting the Role of Vitamin D Levels in the Prevention of COVID-19 Infection and Mortality in European Countries Post Infections Peak",
"author": "Singh",
"doi-asserted-by": "publisher",
"journal-title": "Aging Clin Exp Res",
"key": "B29",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.1101/2020.06.12.20105676",
"article-title": "Covariation of Zinc Deficiency With COVID-19 Infections and Mortality in European Countries: Is Zinc Deficiency a Risk Factor for COVID-19",
"author": "Singh",
"doi-asserted-by": "publisher",
"journal-title": "medRxiv",
"key": "B30",
"year": "2020"
},
{
"DOI": "10.1073/pnas.2016733117",
"article-title": "Lack of Evidence for BCG Vaccine Protection From Severe COVID-19",
"author": "Arlehamna",
"doi-asserted-by": "publisher",
"journal-title": "PNAS",
"key": "B31",
"volume": "117",
"year": "2020"
},
{
"DOI": "10.1146/annurev-genet-120215-035146",
"article-title": "Transition Metals and Virulence in Bacteria",
"author": "Palmer",
"doi-asserted-by": "publisher",
"first-page": "67",
"journal-title": "Annu Rev Genet",
"key": "B32",
"volume": "50",
"year": "2016"
},
{
"DOI": "10.1371/journal.pone.0048679",
"article-title": "Zinc Transporter ZIP14 Functions in Hepatic Zinc, Iron and Glucose Homeostasis During the Innate Immune Response (Endotoxemia)",
"author": "Aydemir",
"doi-asserted-by": "publisher",
"first-page": "e48679",
"journal-title": "PloS One",
"key": "B33",
"volume": "7",
"year": "2012"
},
{
"DOI": "10.3390/ijms18112375",
"article-title": "Elemental Ingredients in the Macrophage Cocktail: Role of ZIP8 in Host Response to Mycobacterium Tuberculosis",
"author": "Pyle",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "B34",
"volume": "18",
"year": "2017"
},
{
"DOI": "10.1074/jbc.273.20.12427",
"article-title": "High Level Expression and Dimer Characterization of the S100 EF-Hand Proteins, Migration Inhibitory Factor-Related Proteins 8 and 14",
"author": "Hunter",
"doi-asserted-by": "publisher",
"journal-title": "J Biol Chem",
"key": "B35",
"volume": "273",
"year": "1998"
},
{
"DOI": "10.1038/nm1638",
"article-title": "Mrp8 and Mrp14 Are Endogenous Activators of Toll-Like Receptor 4, Promoting Lethal, Endotoxin-Induced Shock",
"author": "Vogl",
"doi-asserted-by": "publisher",
"journal-title": "Nat Med",
"key": "B36",
"volume": "13",
"year": "2007"
},
{
"DOI": "10.1248/bpb.26.753",
"article-title": "Calprotectin (S100A8/S100A9), an Inflammatory Protein Complex From Neutrophils With a Broad Apoptosis-Inducing Activity",
"author": "Yui",
"doi-asserted-by": "publisher",
"journal-title": "Biol Pharm Bull",
"key": "B37",
"volume": "26",
"year": "2003"
},
{
"DOI": "10.1126/science.1152449",
"article-title": "Metal Chelation and Inhibition of Bacterial Growth in Tissue Abscesses",
"author": "Corbin",
"doi-asserted-by": "publisher",
"journal-title": "Science",
"key": "B38",
"volume": "319",
"year": "2008"
},
{
"DOI": "10.1128/IAI.00779-17",
"article-title": "Role of Calprotectin in Withholding Zinc and Copper From Candida Albicans",
"author": "Besold",
"doi-asserted-by": "publisher",
"journal-title": "Infect Immun",
"key": "B39",
"volume": "86",
"year": "2018"
},
{
"DOI": "10.1016/j.chembiol.2019.02.011",
"article-title": "Multi-Metal Restriction by Calprotectin Impacts De Novo Flavin Biosynthesis in Acinetobacter Baumannii",
"author": "Wang",
"doi-asserted-by": "publisher",
"first-page": "745",
"journal-title": "Cell Chem Biol",
"key": "B40",
"volume": "26",
"year": "2019"
},
{
"DOI": "10.3390/nu12010236",
"article-title": "A Review of Micronutrients and the Immune System-Working in Harmony to Reduce the Risk of Infection",
"author": "Gombart",
"doi-asserted-by": "publisher",
"journal-title": "Nutrients",
"key": "B41",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1002/14651858.CD009384.pub2",
"article-title": "Zinc Supplementation for Preventing Mortality, Morbidity, and Growth Failure in Children Aged 6 Months to 12 Years of Age",
"author": "Mayo–Wilson",
"doi-asserted-by": "publisher",
"first-page": "Cd009384",
"journal-title": "Cochrane Database Syst Rev",
"key": "B42",
"volume": "5",
"year": "2014"
},
{
"key": "B43",
"unstructured": "World Health OrganizationZinc Supplementation in Children With Respiratory Infections E-Library of Evidence for Nutrition Actions (eLENA)"
},
{
"DOI": "10.1152/ajplung.00341.2005",
"article-title": "Zinc Modulates Airway Epithelium Susceptibility to Death Receptor- Mediated Apoptosis",
"author": "Bao",
"doi-asserted-by": "publisher",
"journal-title": "Am J Physiol – Lung Cell Mol Physiol",
"key": "B44",
"volume": "290",
"year": "2006"
},
{
"key": "B45",
"volume-title": "Guideline: Nutritional Care and Support for Patients With Tuberculosis",
"year": "2013"
},
{
"DOI": "10.1002/14651858.CD006086.pub4",
"article-title": "Nutritional Supplements for People Being Treated for Active Tuberculosis",
"author": "Grobler",
"doi-asserted-by": "publisher",
"journal-title": "Cochrane Database Systematic Rev",
"key": "B46",
"volume": "2016",
"year": "2016"
},
{
"DOI": "10.1001/jamanetworkopen.2020.4330",
"article-title": "Effect of Zinc Supplementation vs Placebo on Mortality Risk and HIV Disease Progression Among HIV-Positive Adults With Heavy Alcohol Use: A Randomized Clinical Trial",
"author": "Freiberg",
"doi-asserted-by": "publisher",
"first-page": "e204330",
"journal-title": "JAMA Netw Open",
"key": "B47",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1093/ajcn/68.2.425S",
"article-title": "Effect of Infections on Plasma Zinc Concentration and Implications for Zinc Status Assessment in Low-Income Countries",
"author": "Brown",
"doi-asserted-by": "publisher",
"journal-title": "Am J Clin Nutr",
"key": "B48",
"volume": "68",
"year": "1998"
},
{
"DOI": "10.1177/15648265070283S303",
"article-title": "Use of Serum Zinc Concentration as an Indicator of Population Zinc Status",
"author": "Hess",
"doi-asserted-by": "publisher",
"journal-title": "Food Nutr Bull",
"key": "B49",
"volume": "28",
"year": "2007"
},
{
"DOI": "10.3402/pba.v5.25592",
"article-title": "Zinc, Aging, and Immunosenescence: An Overview",
"author": "Cabrera",
"doi-asserted-by": "publisher",
"journal-title": "Pathobiol Aging Age-Relat Dis",
"key": "B50",
"volume": "5",
"year": "2015"
},
{
"DOI": "10.1136/openhrt-2020-001472",
"article-title": "COVID-19 and Its Impact on the Cardiovascular System",
"author": "Khawaja",
"doi-asserted-by": "publisher",
"first-page": "e001472",
"journal-title": "Open Heart",
"key": "B51",
"volume": "8",
"year": "2021"
},
{
"key": "B52",
"unstructured": "Zinc Toxicity\n AgnewUM\n SlesingerTL\n Treasure Island (FLStatPearls PublishingStatPearls2020"
},
{
"DOI": "10.1136/bmj.m3379",
"article-title": "A Living WHO Guideline on Drugs for Covid-19",
"author": "Rochwerg",
"doi-asserted-by": "publisher",
"journal-title": "BMJ",
"key": "B53",
"volume": "370",
"year": "2020"
},
{
"DOI": "10.1136/bmj.m2980",
"article-title": "Drug Treatments for Covid-19: Living Systematic Review and Network Meta-Analysis",
"author": "Siemieniuk",
"doi-asserted-by": "publisher",
"journal-title": "BMJ",
"key": "B54",
"volume": "370",
"year": "2020"
},
{
"DOI": "10.1038/232480a0",
"article-title": "Effects of Steroid Pharmaceuticals on Plasma Zinc",
"author": "Briggs",
"doi-asserted-by": "publisher",
"journal-title": "Nature",
"key": "B55",
"volume": "232",
"year": "1971"
},
{
"DOI": "10.1097/00000441-198109000-00003",
"article-title": "Influence of Synthetic Corticosteroids on Plasma Zinc and Copper Levels in Humans",
"author": "Yunice",
"doi-asserted-by": "publisher",
"first-page": "68",
"journal-title": "Am J Med Sci",
"key": "B56",
"volume": "282",
"year": "1981"
},
{
"DOI": "10.1136/pgmj.52.605.148",
"article-title": "Serum Zinc Levels in Corticosteroid-Treated Asthmatic Patients",
"author": "Ellul-Micallef",
"doi-asserted-by": "publisher",
"journal-title": "Postgrad Med J",
"key": "B57",
"volume": "52",
"year": "1976"
},
{
"DOI": "10.1111/j.1432-1033.1981.tb05062.x",
"article-title": "Induction of Metallothionein in HeLa Cells by Dexamethasone and Zinc",
"author": "Karin",
"doi-asserted-by": "publisher",
"journal-title": "Eur J Biochem",
"key": "B58",
"volume": "113",
"year": "1981"
},
{
"DOI": "10.1016/s0009-2797(85)80141-1",
"article-title": "Effects of Dexamethasone on Metallothionein Induction by Zn, Cu, and Cd in Chang Liver Cells",
"author": "Kobayashi",
"doi-asserted-by": "publisher",
"journal-title": "Chem Biol Interact",
"key": "B59",
"volume": "55",
"year": "1985"
},
{
"DOI": "10.1016/0923-1811(94)00378-r",
"article-title": "Possible Role of 1,25-Dihydroxyvitamin D3-Induced Metallothionein in Photoprotection Against UVB Injury in Mouse Skin and Cultured Rat Keratinocytes",
"author": "Hanada",
"doi-asserted-by": "publisher",
"journal-title": "J Dermatol Sci",
"key": "B60",
"volume": "9",
"year": "1995"
}
],
"reference-count": 60,
"references-count": 60,
"relation": {
"has-preprint": [
{
"asserted-by": "object",
"id": "10.1101/2020.11.04.20151290",
"id-type": "doi"
}
]
},
"resource": {
"primary": {
"URL": "https://www.frontiersin.org/articles/10.3389/fimmu.2021.699389/full"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "Nutritional Immunity, Zinc Sufficiency, and COVID-19 Mortality in Socially Similar European Populations",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.3389/crossmark-policy",
"volume": "12"
}
