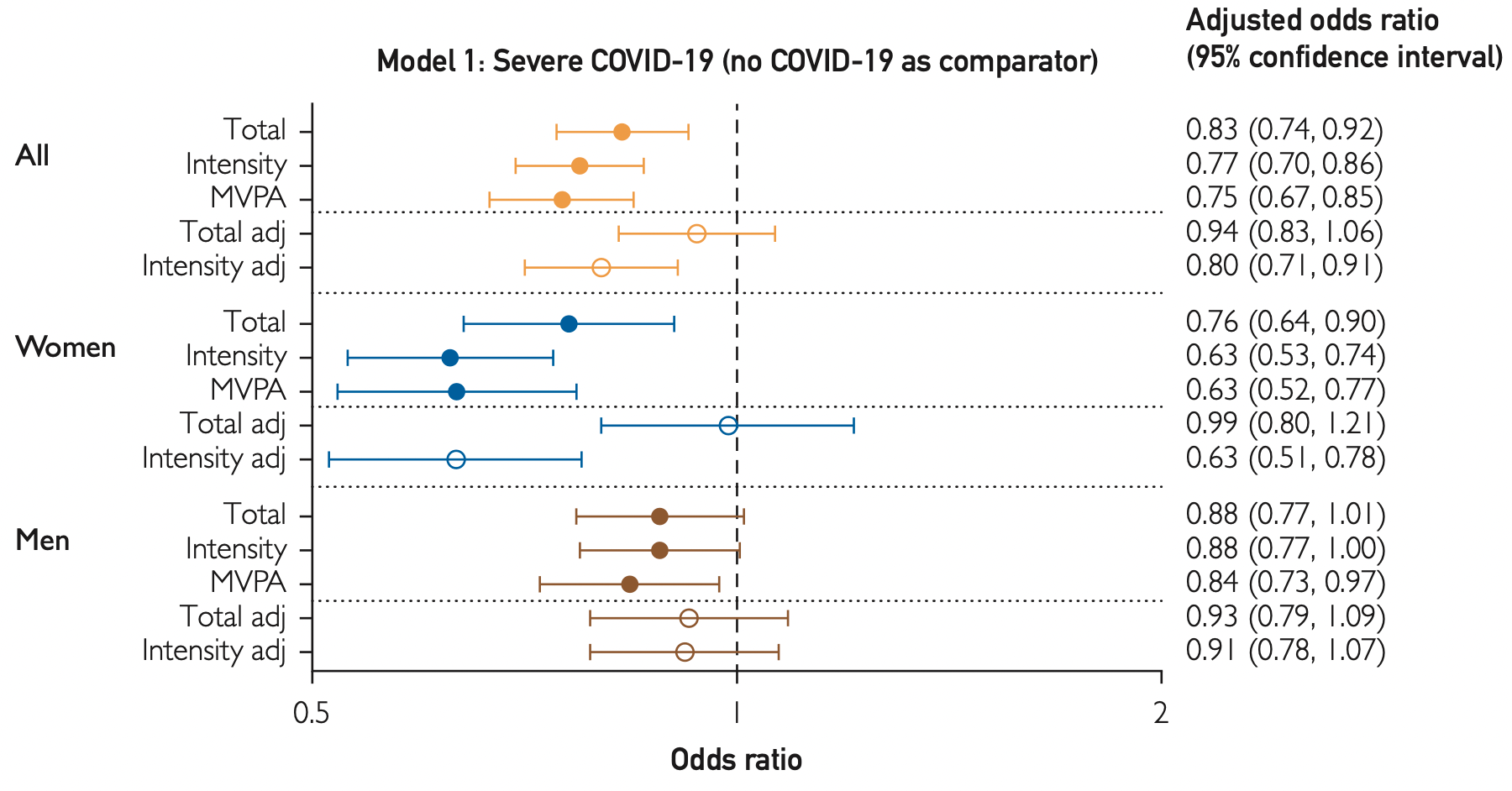
Association Between Accelerometer-Assessed Physical Activity and Severity of COVID-19 in UK Biobank
et al., Mayo Clinic Proceedings: Innovations, Quality & Outcomes, doi:10.1016/j.mayocpiqo.2021.08.011, Dec 2021
Exercise for COVID-19
9th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 68 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
UK Biobank retrospective showing lower risk of severe COVID-19 with higher moderate to vigorous physical activity. Results are only provided for physical activity as a continuous variable.
Rowlands et al., 31 Dec 2021, retrospective, United Kingdom, peer-reviewed, 13 authors, study period 16 March, 2020 - 16 March, 2021.
Association Between Accelerometer-Assessed Physical Activity and Severity of COVID-19 in UK Biobank
Mayo Clinic Proceedings: Innovations, Quality & Outcomes, doi:10.1016/j.mayocpiqo.2021.08.011
Objective: To quantify the association between accelerometer-assessed physical activity and coronavirus disease 2019 (COVID-19) outcomes.
Research and InnovationeDepartment of Health and Social Care COVID-19 Rapid Response Rolling Call (MR/ V020536/1) and Health Data Research UK (HDRUK2020.138). The funders had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication. Potential Competing Interests: K.K. is a member of the UK Scientific Advisory Group for Emergencies (SAGE), Chair of the SAGE subgroup on ethnicity and COVID-19, and member of Independent SAGE. All other authors declare that they have no competing interests.
References
Anderson, Heesterbeek, Klinkenberg, Hollingsworth, How will country-based mitigation . How will country-based mitigation measures influence the course of the COVID-19 epidemic?, Lancet
Armstrong, Rudkin, Allen, Dynamic linkage of COVID-19 test results between Public Health England's Second Generation Surveillance System and UK Biobank, Microb Genom
Arvidsson, Fridolfsson, Börjesson, Measurement of physical activity in clinical practice using accelerometers, J Intern Med
Batty, Gale, Kivimäki, Deary, Bell, Comparison of risk factor associations in UK Biobank against representative, general population-based studies with conventional response rates: prospective cohort study and individual participant meta-analysis, BMJ
Brawner, Ehman, Bole, Inverse relationship of maximal exercise capacity to hospitalization secondary to coronavirus disease 2019, Mayo Clin Proc
Bull, Al-Ansari, Biddle, World Health Organization 2020 guidelines on physical activity and sedentary behaviour, Br J Sports Med
Chastin, Abaraogu, Bourgois, Effects of regular physical activity on the immune system, vaccination and risk of community-acquired infectious disease in the general population: systematic review and meta-analysis, Sports Med
Doherty, Jackson, Hammerla, Large scale population assessment of physical activity using wrist worn accelerometers: the UK Biobank Study, PLoS One
Gao, Piernas, Astbury, Associations between body-mass index and COVID-19 severity in 6.9 million people in England: a prospective, community-based, cohort study. Lan, cet Diabetes Endocrinol
Griffith, Morrus, Tudball, Collider bias undermines our understanding of COVID-19 disease risk and severity, Nat Comm
Hildebrand, Van Hees, Hansen, Ekelund, Age group comparability of raw accelerometer output from wrist-and hipworn monitors, Med Sci Sports Exerc
Lavie, Sanchis-Gomar, Arena, Fit is it in COVID-19, future pandemics, and overall healthy living, Mayo Clin Proc
Mathur, Rentsch, Morton, Ethnic differences in SARS-CoV-2 infection and COVID-19erelated hospitalisation, intensive care unit admission, and death in 17 million adults in England: an observational cohort study using the OpenSAFELY platform, Lancet
Migueles, Rowlands, Huber, Sabia, Van Hees et al., GGIR: a research community-driven open-source R-package for generating physical activity and sleep outcomes from multi-day raw accelerometer data, J Measure Phys Behav
Mutambudzi, Niedwiedz, Macdonald, Occupation and risk of severe COVID-19: prospective cohort study of 120, 075 UK Biobank participants, Occup Environ Med
Razieh, Zaccardi, Islam, Ethnic minorities and COVID-19: examining whether excess risk is mediated through deprivation, Eur J Public Health
Rowlands, Edwardson, Davies, Khunti, Harrington et al., Beyond cut points: accelerometer metrics that capture the physical activity profile, Med Sci Sports Exerc
Rowlands, Edwardson, Dawkins, Maylor, Metcalf et al., Physical activity for bone health: how much and/or how hard?, Med Sci Sports Exerc
Rowlands, Gillies, Chudasama, Association of working shifts, inside and outside of healthcare, with severe COVID-19: an observational study, BMC Public Health
Rowlands, Kloecker, Chudasama, Association of balance and timing of physical activity and rest with risk of COVID-19 in UK Biobank, Mayo Clin Proc
Rowlands, Yates, Edwardson, Activity intensity, volume and norms: utility and interpretation of accelerometer metrics, Med Sci Sports Exerc
Sallis, Adlakha, Oyeyemi, An international physical activity and public health research agenda to inform coronavirus disease-2019 policies and practices, J Sport Health Sci
Sallis, Young, Tartof, Physical inactivity is associated with a higher risk for severe COVID-19 outcomes: a study in 48 440 adult patients, Br J Sports Med
Smith, Gardner, Fisher, Hamer, Patterns and correlates of physical activity behaviour over 10 years in older adults: prospective analyses from the English Longitudinal Study of Ageing, BMJ Open
Strain, Wijendaele, Dempsey, Wearable-devicemeasured physical activity and future health risk, Nat Med
Sudlow, Gallacher, Allen, UK Biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age, PLoS Med
Vepa, Bae, Ahmed, Pareek, Khunti, COVID-19 and ethnicity: a novel pathophysiological role for inflammation, Diabetes Metab Syndr
Warburton, Nicol, Bredin, Health benefits of physical activity: the evidence, CMAJ
Yang, Zheng, Gou, Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis, Int J Infect Dis
Yates, Razieh, Zaccardi, Davies, Khunti, Obesity and risk of COVID-19: analysis of UK Biobank, Prim Care Diabetes
Yates, Razieh, Zaccardi, Obesity, walking pace and risk of severe COVID-19: analysis of UK Biobank, Int J Obes (Lond)
DOI record:
{
"DOI": "10.1016/j.mayocpiqo.2021.08.011",
"ISSN": [
"2542-4548"
],
"URL": "http://dx.doi.org/10.1016/j.mayocpiqo.2021.08.011",
"alternative-id": [
"S2542454821001302"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-1463-697X",
"affiliation": [],
"authenticated-orcid": false,
"family": "Rowlands",
"given": "Alex V.",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-1714-6087",
"affiliation": [],
"authenticated-orcid": false,
"family": "Dempsey",
"given": "Paddy C.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-8417-9700",
"affiliation": [],
"authenticated-orcid": false,
"family": "Gillies",
"given": "Clare",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-8910-2091",
"affiliation": [],
"authenticated-orcid": false,
"family": "Kloecker",
"given": "David E.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-3597-2945",
"affiliation": [],
"authenticated-orcid": false,
"family": "Razieh",
"given": "Cameron",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-6777-0064",
"affiliation": [],
"authenticated-orcid": false,
"family": "Chudasama",
"given": "Yogini",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-3982-4325",
"affiliation": [],
"authenticated-orcid": false,
"family": "Islam",
"given": "Nazrul",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-2636-6487",
"affiliation": [],
"authenticated-orcid": false,
"family": "Zaccardi",
"given": "Francesco",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-0127-5236",
"affiliation": [],
"authenticated-orcid": false,
"family": "Lawson",
"given": "Claire",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-9140-0776",
"affiliation": [],
"authenticated-orcid": false,
"family": "Norris",
"given": "Tom",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-9987-9371",
"affiliation": [],
"authenticated-orcid": false,
"family": "Davies",
"given": "Melanie J.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-2343-7099",
"affiliation": [],
"authenticated-orcid": false,
"family": "Khunti",
"given": "Kamlesh",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-5724-5178",
"affiliation": [],
"authenticated-orcid": false,
"family": "Yates",
"given": "Tom",
"sequence": "additional"
}
],
"container-title": "Mayo Clinic Proceedings: Innovations, Quality & Outcomes",
"container-title-short": "Mayo Clinic Proceedings: Innovations, Quality & Outcomes",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2021,
8,
20
]
],
"date-time": "2021-08-20T05:36:03Z",
"timestamp": 1629437763000
},
"deposited": {
"date-parts": [
[
2021,
12,
26
]
],
"date-time": "2021-12-26T04:06:39Z",
"timestamp": 1640491599000
},
"funder": [
{
"DOI": "10.13039/501100000271",
"doi-asserted-by": "publisher",
"name": "UKRI Science and Technology Facilities Council"
}
],
"indexed": {
"date-parts": [
[
2022,
4,
1
]
],
"date-time": "2022-04-01T15:50:57Z",
"timestamp": 1648828257796
},
"is-referenced-by-count": 3,
"issue": "6",
"issued": {
"date-parts": [
[
2021,
12
]
]
},
"journal-issue": {
"issue": "6",
"published-print": {
"date-parts": [
[
2021,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
12,
1
]
],
"date-time": "2021-12-01T00:00:00Z",
"timestamp": 1638316800000
}
},
{
"URL": "http://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
8,
14
]
],
"date-time": "2021-08-14T00:00:00Z",
"timestamp": 1628899200000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S2542454821001302?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S2542454821001302?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "997-1007",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2021,
12
]
]
},
"published-print": {
"date-parts": [
[
2021,
12
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1093/eurpub/ckab041",
"article-title": "Ethnic minorities and COVID-19: examining whether excess risk is mediated through deprivation",
"author": "Razieh",
"doi-asserted-by": "crossref",
"first-page": "630",
"issue": "3",
"journal-title": "Eur J Public Health",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib2",
"volume": "31",
"year": "2021"
},
{
"DOI": "10.1016/S0140-6736(20)30567-5",
"article-title": "How will country-based mitigation . How will country-based mitigation measures influence the course of the COVID-19 epidemic?",
"author": "Anderson",
"doi-asserted-by": "crossref",
"first-page": "931",
"issue": "10228",
"journal-title": "Lancet",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib3",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(21)00634-6",
"author": "Mathur",
"doi-asserted-by": "crossref",
"first-page": "1711",
"issue": "10286",
"journal-title": "Lancet",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib4",
"volume": "397",
"year": "2021"
},
{
"DOI": "10.1016/j.pcd.2020.05.011",
"article-title": "Obesity and risk of COVID-19: analysis of UK Biobank",
"author": "Yates",
"doi-asserted-by": "crossref",
"first-page": "566",
"issue": "5",
"journal-title": "Prim Care Diabetes",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib5",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1038/s41366-021-00771-z",
"article-title": "Obesity, walking pace and risk of severe COVID-19: analysis of UK Biobank",
"author": "Yates",
"doi-asserted-by": "crossref",
"first-page": "115",
"issue": "5",
"journal-title": "Int J Obes (Lond)",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib6",
"volume": "45",
"year": "2021"
},
{
"DOI": "10.1007/s40279-021-01466-1",
"article-title": "Effects of regular physical activity on the immune system, vaccination and risk of community-acquired infectious disease in the general population: systematic review and meta-analysis",
"author": "Chastin",
"doi-asserted-by": "crossref",
"first-page": "1673",
"issue": "8",
"journal-title": "Sports Med",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib7",
"volume": "51",
"year": "2021"
},
{
"article-title": "An international physical activity and public health research agenda to inform coronavirus disease-2019 policies and practices",
"author": "Sallis",
"first-page": "328",
"issue": "4",
"journal-title": "J Sport Health Sci",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib8",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2020.06.056",
"article-title": "COVID-19 and ethnicity: a novel pathophysiological role for inflammation",
"author": "Vepa",
"doi-asserted-by": "crossref",
"first-page": "1043",
"issue": "5",
"journal-title": "Diabetes Metab Syndr",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib9",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1503/cmaj.051351",
"article-title": "Health benefits of physical activity: the evidence",
"author": "Warburton",
"doi-asserted-by": "crossref",
"first-page": "801",
"issue": "6",
"journal-title": "CMAJ",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib10",
"volume": "174",
"year": "2006"
},
{
"DOI": "10.1016/j.ijid.2020.03.017",
"article-title": "Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis",
"author": "Yang",
"doi-asserted-by": "crossref",
"first-page": "91",
"journal-title": "Int J Infect Dis",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib11",
"volume": "94",
"year": "2020"
},
{
"DOI": "10.1016/j.mayocp.2020.10.032",
"article-title": "Association of balance and timing of physical activity and rest with risk of COVID-19 in UK Biobank",
"author": "Rowlands",
"doi-asserted-by": "crossref",
"first-page": "156",
"issue": "1",
"journal-title": "Mayo Clin Proc",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib12",
"volume": "96",
"year": "2020"
},
{
"DOI": "10.1136/bjsports-2021-104080",
"article-title": "Physical inactivity is associated with a higher risk for severe COVID-19 outcomes: a study in 48 440 adult patients",
"author": "Sallis",
"doi-asserted-by": "crossref",
"journal-title": "Br J Sports Med",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib13",
"year": "2021"
},
{
"article-title": "Measurement of physical activity in clinical practice using accelerometers",
"author": "Arvidsson",
"first-page": "137",
"issue": "2",
"journal-title": "J Intern Med",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib14",
"volume": "286",
"year": "2019"
},
{
"DOI": "10.1249/MSS.0000000000002047",
"article-title": "Activity intensity, volume and norms: utility and interpretation of accelerometer metrics",
"author": "Rowlands",
"doi-asserted-by": "crossref",
"first-page": "2410",
"issue": "11",
"journal-title": "Med Sci Sports Exerc",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib15",
"volume": "51",
"year": "2019"
},
{
"DOI": "10.1038/s41591-020-1012-3",
"article-title": "Wearable-device-measured physical activity and future health risk",
"author": "Strain",
"doi-asserted-by": "crossref",
"first-page": "1385",
"issue": "9",
"journal-title": "Nat Med",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib16",
"volume": "26",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0169649",
"article-title": "Large scale population assessment of physical activity using wrist worn accelerometers: the UK Biobank Study",
"author": "Doherty",
"doi-asserted-by": "crossref",
"first-page": "e0169649",
"issue": "2",
"journal-title": "PLoS One",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib17",
"volume": "12",
"year": "2017"
},
{
"DOI": "10.1371/journal.pmed.1001779",
"article-title": "UK Biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age",
"author": "Sudlow",
"doi-asserted-by": "crossref",
"first-page": "e1001779",
"issue": "3",
"journal-title": "PLoS Med",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib18",
"volume": "12",
"year": "2015"
},
{
"article-title": "Dynamic linkage of COVID-19 test results between Public Health England’s Second Generation Surveillance System and UK Biobank",
"author": "Armstrong",
"first-page": "mgen000397",
"issue": "7",
"journal-title": "Microb Genom",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib19",
"volume": "6",
"year": "2020"
},
{
"DOI": "10.1123/jmpb.2018-0063",
"article-title": "GGIR: a research community-driven open-source R-package for generating physical activity and sleep outcomes from multi-day raw accelerometer data",
"author": "Migueles",
"doi-asserted-by": "crossref",
"first-page": "188",
"issue": "3",
"journal-title": "J Measure Phys Behav",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib20",
"volume": "2",
"year": "2019"
},
{
"DOI": "10.1249/MSS.0000000000001561",
"article-title": "Beyond cut points: accelerometer metrics that capture the physical activity profile",
"author": "Rowlands",
"doi-asserted-by": "crossref",
"first-page": "1323",
"issue": "6",
"journal-title": "Med Sci Sports Exerc",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib21",
"volume": "50",
"year": "2018"
},
{
"DOI": "10.1249/MSS.0000000000000289",
"article-title": "Age group comparability of raw accelerometer output from wrist- and hip-worn monitors",
"author": "Hildebrand",
"doi-asserted-by": "crossref",
"first-page": "1816",
"issue": "9",
"journal-title": "Med Sci Sports Exerc",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib22",
"volume": "46",
"year": "2014"
},
{
"DOI": "10.1249/MSS.0000000000002380",
"article-title": "Physical activity for bone health: how much and/or how hard?",
"author": "Rowlands",
"doi-asserted-by": "crossref",
"first-page": "2331",
"issue": "11",
"journal-title": "Med Sci Sports Exerc",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib23",
"volume": "52",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(21)00089-9",
"article-title": "Associations between body-mass index and COVID-19 severity in 6.9 million people in England: a prospective, community-based, cohort study",
"author": "Gao",
"doi-asserted-by": "crossref",
"first-page": "350",
"issue": "6",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib24",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1186/s12889-021-10839-0",
"article-title": "Association of working shifts, inside and outside of healthcare, with severe COVID-19: an observational study",
"author": "Rowlands",
"doi-asserted-by": "crossref",
"first-page": "773",
"issue": "1",
"journal-title": "BMC Public Health",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib25",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.1136/bjsports-2020-102955",
"article-title": "World Health Organization 2020 guidelines on physical activity and sedentary behaviour",
"author": "Bull",
"doi-asserted-by": "crossref",
"first-page": "1451",
"issue": "24",
"journal-title": "Br J Sports Med",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib26",
"volume": "54",
"year": "2020"
},
{
"DOI": "10.1016/j.mayocp.2020.10.003",
"article-title": "Inverse relationship of maximal exercise capacity to hospitalization secondary to coronavirus disease 2019",
"author": "Brawner",
"doi-asserted-by": "crossref",
"first-page": "32",
"issue": "1",
"journal-title": "Mayo Clin Proc",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib27",
"volume": "96",
"year": "2021"
},
{
"DOI": "10.1016/j.mayocp.2020.11.013",
"article-title": "Fit is it in COVID-19, future pandemics, and overall healthy living",
"author": "Lavie",
"doi-asserted-by": "crossref",
"first-page": "7",
"issue": "1",
"journal-title": "Mayo Clin Proc",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib28",
"volume": "96",
"year": "2021"
},
{
"DOI": "10.1038/s41467-020-19478-2",
"article-title": "Collider bias undermines our understanding of COVID-19 disease risk and severity",
"author": "Griffith",
"doi-asserted-by": "crossref",
"first-page": "5749",
"issue": "1",
"journal-title": "Nat Comm",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib29",
"volume": "11",
"year": "2020"
},
{
"article-title": "Occupation and risk of severe COVID-19: prospective cohort study of 120,075 UK Biobank participants",
"author": "Mutambudzi",
"journal-title": "Occup Environ Med",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib30",
"year": "2020"
},
{
"DOI": "10.1136/bmjopen-2014-007423",
"article-title": "Patterns and correlates of physical activity behaviour over 10 years in older adults: prospective analyses from the English Longitudinal Study of Ageing",
"author": "Smith",
"doi-asserted-by": "crossref",
"first-page": "e007423",
"issue": "4",
"journal-title": "BMJ Open",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib31",
"volume": "5",
"year": "2015"
},
{
"DOI": "10.1136/bmj.m131",
"article-title": "Comparison of risk factor associations in UK Biobank against representative, general population-based studies with conventional response rates: prospective cohort study and individual participant meta-analysis",
"author": "Batty",
"doi-asserted-by": "crossref",
"first-page": "m131",
"journal-title": "BMJ",
"key": "10.1016/j.mayocpiqo.2021.08.011_bib32",
"volume": "368",
"year": "2020"
}
],
"reference-count": 31,
"references-count": 31,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S2542454821001302"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine"
],
"subtitle": [],
"title": "Association Between Accelerometer-Assessed Physical Activity and Severity of COVID-19 in UK Biobank",
"type": "journal-article",
"volume": "5"
}
