Cetylpyridinium chloride and chlorhexidine show antiviral activity against Influenza A virus and Respiratory Syncytial virus in vitro
et al., PLOS ONE, doi:10.1371/journal.pone.0297291, Feb 2024
58th treatment shown to reduce risk in
September 2025, now with p = 0.0035 from 4 studies.
Lower risk for recovery and viral clearance.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
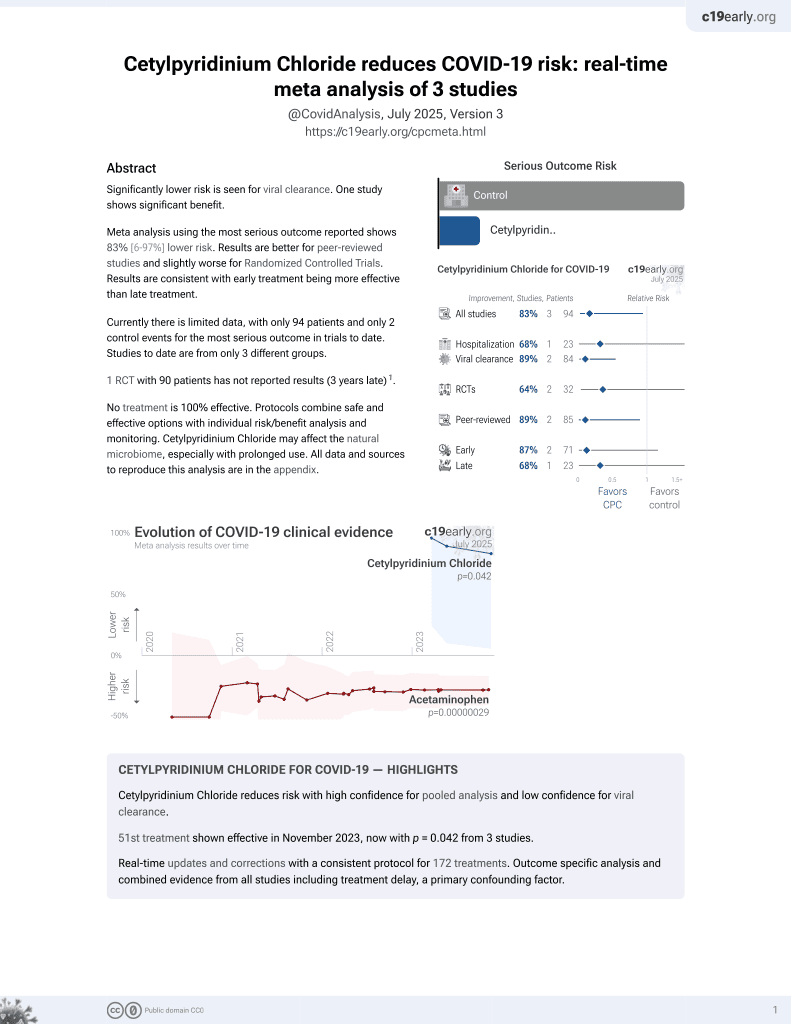
In vitro study showing antiviral activity against influenza A virus and respiratory syncytial virus with cetylpyridinium chloride (CPC) and chlorhexidine (CHX). Authors found CPC and CHX decreased infectivity of both viruses by 90-99.9% depending on concentration. Commercial CPC and CHX-containing mouthwash preparations also reduced viral viability up to 99.99%. The use of mouthwashes with CPC or CHX may help limit infection and spread of enveloped respiratory viruses in the oral cavity.
2 preclinical studies support the efficacy of cetylpyridinium chloride for COVID-19:
Study covers cetylpyridinium chloride and chlorhexidine.
Rius-Salvador et al., 16 Feb 2024, peer-reviewed, 8 authors.
Contact: luis.martinez-gil@uv.es.
In vitro studies are an important part of preclinical research, however results may be very different in vivo.
Cetylpyridinium chloride and chlorhexidine show antiviral activity against Influenza A virus and Respiratory Syncytial virus in vitro
PLOS ONE, doi:10.1371/journal.pone.0297291
Background The oral cavity is the site of entry and replication for many respiratory viruses. Furthermore, it is the source of droplets and aerosols that facilitate viral transmission. It is thought that appropriate oral hygiene that alters viral infectivity might reduce the spread of respiratory viruses and contribute to infection control.
Materials and methods Here, we analyzed the antiviral activity of cetylpyridinium chloride (CPC), chlorhexidine (CHX), and three commercial CPC and CHX-containing mouthwash preparations against the Influenza A virus and the Respiratory syncytial virus. To do so the aforementioned compounds and preparations were incubated with the Influenza A virus or with the Respiratory syncytial virus. Next, we analyzed the viability of the treated viral particles.
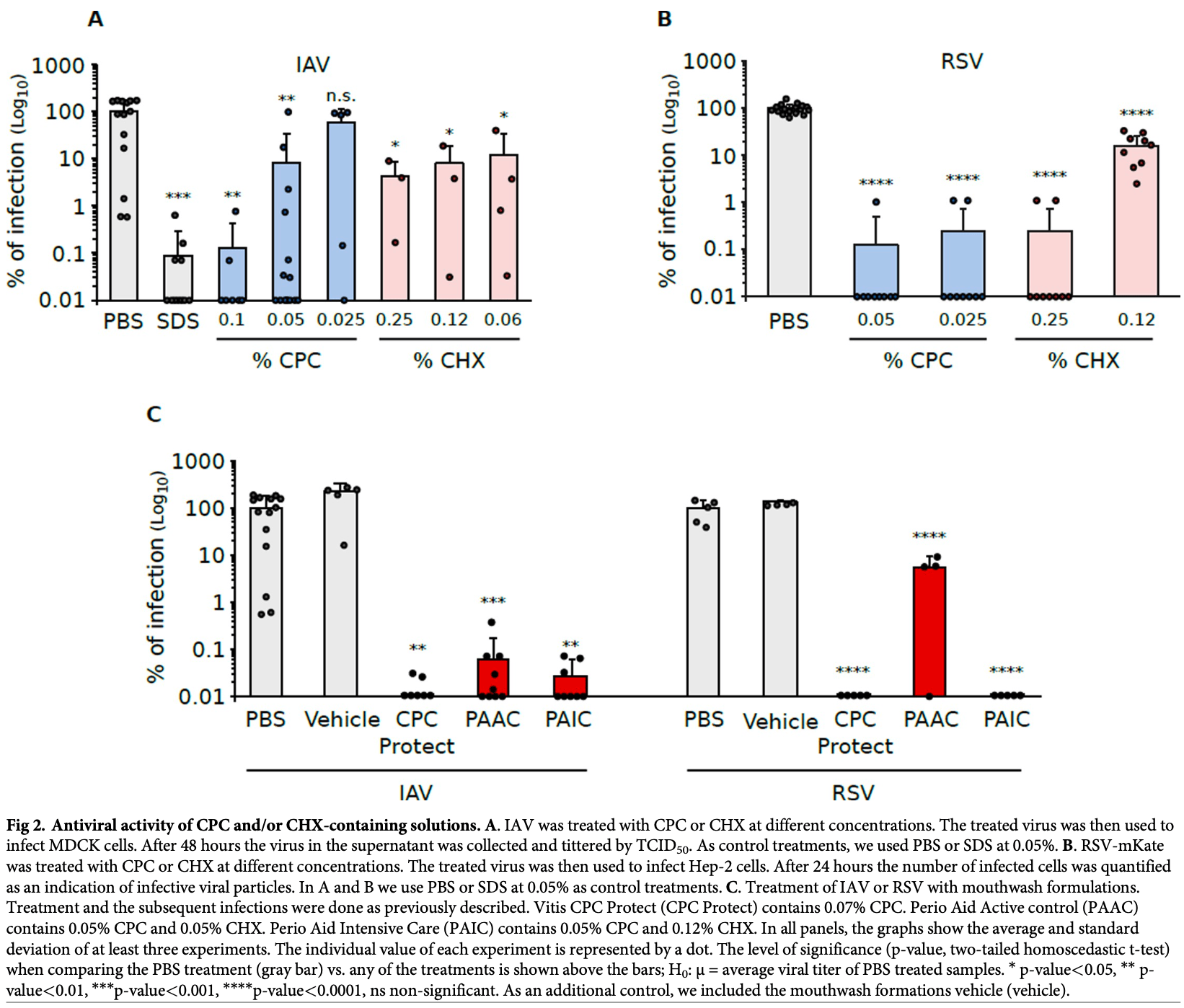
Results Our results indicate that CPC and CHX decrease the infectivity of both the Influenza A virus and the Respiratory Syncytial virus in vitro between 90 and 99.9% depending on the concentration. Likewise, CPC and CHX-containing mouthwash preparations were up to 99.99% effective in decreasing the viral viability of both the Influenza A virus and the Respiratory syncytial virus in vitro.
Conclusion The use of a mouthwash containing CPC or CHX alone or in combination might represent a cost-effective measure to limit infection and spread of enveloped respiratory viruses infecting the oral cavity, aiding in reducing viral transmission. Our findings may stimulate future
Supporting information S1 Fig. Time of exposure. We tested the effect of the exposure time to CPC. To do so, IAV/ WSN/33 was incubated with CPC at 0.1% for 2 minutes, 1 minute, or 30 seconds. Next, the virus was diluted and used to infect MDCK cells as previously described. After 48 hours of infection, the viral load was assessed by TCID50. We used a 2-minute treatment with SDS at 0.05% as a positive control and PBS solution as a negative control. No differences in the viral load were observed between the 2 minutes, 1 minute, or 30 seconds exposure. (PDF)
Author Contributions Conceptualization: Maria Jesu ´s Garcı ´a-Mu ´rria, Ron Geller, Ismael Mingarro, Luis Martinez-Gil. Data curation: Luis Martinez-Gil. Formal analysis: Luis Martinez-Gil. Investigation: Marina Rius-Salvador, Maria Jesu ´s Garcı ´a-Mu ´rria, Luciana Rusu, Luis Martinez-Gil. Project administration: Maria Jesu ´s Garcı ´a-Mu ´rria, Ismael Mingarro, Luis Martinez-Gil. Resources: Manuel Baño ´-Polo, Rube ´n Leo ´n, Ron Geller, Ismael Mingarro. Supervision: Ismael Mingarro, Luis Martinez-Gil. Validation: Ron Geller. Writing -original draft: Luis Martinez-Gil.
References
Alqarni, Jamleh, Chamber, Chlorhexidine as a Disinfectant in the Prosthodontic Practice: A Comprehensive Review, Cureus, doi:10.7759/cureus.30566
Baño, -Polo, ´nez-Gil, Pino, Massoli et al., Cetylpyridinium chloride promotes disaggregation of SARS-CoV-2 virus-like particles, J Oral Microbiol, doi:10.1080/20002297.2022.2030094
Bernstein, Schiff, Echler, Prince, Feller et al., In vitro Virucidal Effectiveness of a 0.12%-Chlorhexidine Gluconate Mouthrinse, J Dent Res, doi:10.1177/00220345900690030901
Bonn, Rohrhofer, Audebert, Lang, Auer et al., Efficacy of a Mouthwash Containing CHX and CPC in SARS-CoV-2-Positive Patients: A Randomized Controlled Clinical Trial, J Dent Res, doi:10.1177/00220345231156415
Brookes, Mcgrath, Mccullough, Antimicrobial Mouthwashes: An Overview of Mechanisms-What Do We Still Need to Know, Int Dent J, doi:10.1016/j.identj.2023.08.009
Brookes, Teoh, Cieplik, Kumar, Mouthwash Effects on the Oral Microbiome: Are They Good, Bad, or Balanced, Int Dent J, doi:10.1016/j.identj.2023.08.010
Busscher, White, Atema-Smit, Geertsema-Doornbusch, De Vries et al., Surfactive and antibacterial activity of cetylpyridinium chloride formulations in vitro and in vivo, J Clin Periodontol, doi:10.1111/j.1600-051X.2008.01230.x
Carrouel, Gonc ¸alves, Conte, Campus, Fisher et al., Antiviral Activity of Reagents in Mouth Rinses against SARS-CoV-2, J Dent Res, doi:10.1177/0022034520967933
D'amico, Moro, Saracino, Marmiere, Cilona et al., Efficacy of Cetylpyridinium Chloride mouthwash against SARS-CoV-2: A systematic review of randomized controlled trials, Mol Oral Microbiol, doi:10.1111/omi.12408
Deus, Ouanounou, Chlorhexidine in Dentistry: Pharmacology, Uses, and Adverse Effects, Int Dent J, doi:10.1016/j.identj.2022.01.005
He, Liu, Jia, Richardson, Huang, Viral respiratory infections in a rapidly changing climate: the need to prepare for the next pandemic, EBioMedicine, doi:10.1016/j.ebiom.2023.104593
Herrera, Serrano, Rolda ´n, Sanz, Is the oral cavity relevant in SARS-CoV-2 pandemic?, Clin Oral Investig, doi:10.1007/s00784-020-03413-2
Hirose, Bandou, Ikegaya, Watanabe, Yoshida et al., Disinfectant effectiveness against SARS-CoV-2 and influenza viruses present on human skin: model-based evaluation, Clin Microbiol Infect, doi:10.1016/j.cmi.2021.04.009
Hoffmann, The role of the oral cavity in SARS-CoV-2-and other viral infections, Clin Oral Investig, doi:10.1007/s00784-023-05078-z
Hotard, Shaikh, Lee, Yan, Teng et al., A stabilized respiratory syncytial virus reverse genetics system amenable to recombination-mediated mutagenesis, Virology, doi:10.1016/j.virol.2012.09.022
Howley, Knipe, Mahan, Enquist, Fields Virology: Fundamentals
Huang, Pe ´rez, Kato, Mikami, Okuda et al., SARS-CoV-2 infection of the oral cavity and saliva, Nat Med, doi:10.1038/s41591-021-01296-8
Imran, Khurshid, Adanir, Ashi, Almarzouki et al., Dental Practitioners' Knowledge, Attitude and Practices for Mouthwash Use Amidst the COVID-19 Pandemic, Risk Manag Healthc Policy, doi:10.2147/RMHP.S287547
Koletsi, Belibasakis, Eliades, Interventions to Reduce Aerosolized Microbes in Dental Practice: A Systematic Review with Network Meta-analysis of Randomized Controlled Trials, J Dent Res, doi:10.1177/0022034520943574
Langedijk, Bont, Respiratory syncytial virus infection and novel interventions, Nat Rev Microbiol, doi:10.1038/s41579-023-00919-w
Latorre, Geller, Identification of Cytoplasmic Chaperone Networks Relevant for Respiratory Syncytial Virus Replication, Front Microbiol, doi:10.3389/fmicb.2022.880394
Lin, Sun, Hung, Chang, Effectiveness of mouth rinses against COVID-19: a systematic review and network meta-analysis, J Hosp Infect, doi:10.1016/j.jhin.2023.06.022
Lowry, Wolfe, Boehm, Respiratory virus concentrations in human excretions that contribute to wastewater: a systematic review and meta-analysis, J Water Health, doi:10.2166/wh.2023.057
Mao, Auer, Buchalla, Hiller, Maisch et al., Cetylpyridinium Chloride: Mechanism of Action, Antimicrobial Efficacy in Biofilms, and Potential Risks of Resistance, Antimicrob Agents Chemother, doi:10.1128/AAC.00576-20
Meyers, Robison, Milici, Alam, Quillen et al., Lowering the transmission and spread of human coronavirus, J Med Virol, doi:10.1002/jmv.26514
Mukherjee, Esper, Buchheit, Arters, Adkins et al., Randomized, doubleblind, placebo-controlled clinical trial to assess the safety and effectiveness of a novel dual-action oral topical formulation against upper respiratory infections, BMC Infect Dis, doi:10.1186/s12879-016-2177-8
Muñoz-Basagoiti, Perez-Zsolt, Leo ´n R, Blanc, Raïch-Regue et al., Mouthwashes with CPC Reduce the Infectivity of SARS-CoV-2 Variants In Vitro, J Dent Res, doi:10.1177/00220345211029269
Okunishi, Nishihara, Maeda, Ikeda, In vitro evaluation of the antimicrobial activity of HM-242, a novel antiseptic compound, J Antibiot, doi:10.1038/ja.2009.56
Pannuti, Reis, Souza, Souto, Silva et al., Efficacy of mouthrinses in reducing oral SARS-COV-2 load: a review, Braz Oral Res, doi:10.1590/1807-3107BOR-2023.vol37.0038
Peng, Xu, Li, Cheng, Zhou et al., Transmission routes of 2019-nCoV and controls in dental practice, Int J Oral Sci, doi:10.1038/s41368-020-0075-9
Pitten, Kramer, Efficacy of cetylpyridinium chloride used as oropharyngeal antiseptic, Arzneimittelforschung, doi:10.1055/s-0031-1300084
Platt, Bucknall, The disinfection of respiratory syncytial virus by isopropanol and a chlorhexidinedetergent handwash, J Hosp Infect, doi:10.1016/s0195-6701(85)80023-2
Popkin, Zilka, Dimaano, Fujioka, Rackley et al., Cetylpyridinium Chloride (CPC) Exhibits Potent, Rapid Activity Against Influenza Viruses in vitro and in vivo, Pathog Immun, doi:10.20411/pai.v2i2.200
Riveira-Muñoz, Vidal, Baño, -Polo, Leo ´n R et al., Cetylpyridinium Chloride-Containing Mouthwashes Show Virucidal Activity against Herpes Simplex Virus Type 1, Viruses, doi:10.3390/v15071433
Schanzer, Saboui, Lee, Nwosu, Bancej, Burden of influenza, respiratory syncytial virus, and other respiratory viruses and the completeness of respiratory viral identification among respiratory inpatients, Canada, 2003-2014, Influenza Other Respir Viruses, doi:10.1111/irv.12497
Shen, Niu, Wang, Huang, Wang et al., High-Throughput Screening and Identification of Potent Broad-Spectrum Inhibitors of Coronaviruses, J Virol, doi:10.1128/JVI.00023-19
Tarrago, Gil, Mj, Salcedo, Alvarez et al., Randomized clinical trial to assess the impact of oral intervention with cetylpyridinium chloride to reduce salivary SARS-CoV-2 viral load, J Clin Periodontol, doi:10.1111/jcpe.13746
Weber, Bonn, Auer, Kirschneck, Buchalla et al., Preprocedural mouthwashes for infection control in dentistry-an update, Clin Oral Investig, doi:10.1007/s00784-023-04953-z
DOI record:
{
"DOI": "10.1371/journal.pone.0297291",
"ISSN": [
"1932-6203"
],
"URL": "http://dx.doi.org/10.1371/journal.pone.0297291",
"abstract": "<jats:sec id=\"sec001\">\n<jats:title>Background</jats:title>\n<jats:p>The oral cavity is the site of entry and replication for many respiratory viruses. Furthermore, it is the source of droplets and aerosols that facilitate viral transmission. It is thought that appropriate oral hygiene that alters viral infectivity might reduce the spread of respiratory viruses and contribute to infection control.</jats:p>\n</jats:sec>\n<jats:sec id=\"sec002\">\n<jats:title>Materials and methods</jats:title>\n<jats:p>Here, we analyzed the antiviral activity of cetylpyridinium chloride (CPC), chlorhexidine (CHX), and three commercial CPC and CHX-containing mouthwash preparations against the Influenza A virus and the Respiratory syncytial virus. To do so the aforementioned compounds and preparations were incubated with the Influenza A virus or with the Respiratory syncytial virus. Next, we analyzed the viability of the treated viral particles.</jats:p>\n</jats:sec>\n<jats:sec id=\"sec003\">\n<jats:title>Results</jats:title>\n<jats:p>Our results indicate that CPC and CHX decrease the infectivity of both the Influenza A virus and the Respiratory Syncytial virus <jats:italic>in vitro</jats:italic> between 90 and 99.9% depending on the concentration. Likewise, CPC and CHX-containing mouthwash preparations were up to 99.99% effective in decreasing the viral viability of both the Influenza A virus and the Respiratory syncytial virus <jats:italic>in vitro</jats:italic>.</jats:p>\n</jats:sec>\n<jats:sec id=\"sec004\">\n<jats:title>Conclusion</jats:title>\n<jats:p>The use of a mouthwash containing CPC or CHX alone or in combination might represent a cost-effective measure to limit infection and spread of enveloped respiratory viruses infecting the oral cavity, aiding in reducing viral transmission. Our findings may stimulate future clinical studies to evaluate the effects of CPC and CHX in reducing viral respiratory transmissions.</jats:p>\n</jats:sec>",
"author": [
{
"affiliation": [],
"family": "Rius-Salvador",
"given": "Marina",
"sequence": "first"
},
{
"affiliation": [],
"family": "García-Múrria",
"given": "Maria Jesús",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Rusu",
"given": "Luciana",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bañó-Polo",
"given": "Manuel",
"sequence": "additional"
},
{
"affiliation": [],
"family": "León",
"given": "Rubén",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-7612-4611",
"affiliation": [],
"authenticated-orcid": true,
"family": "Geller",
"given": "Ron",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mingarro",
"given": "Ismael",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-9076-7760",
"affiliation": [],
"authenticated-orcid": true,
"family": "Martinez-Gil",
"given": "Luis",
"sequence": "additional"
}
],
"container-title": "PLOS ONE",
"container-title-short": "PLoS ONE",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"www.plosone.org"
]
},
"created": {
"date-parts": [
[
2024,
2,
16
]
],
"date-time": "2024-02-16T18:25:18Z",
"timestamp": 1708107918000
},
"deposited": {
"date-parts": [
[
2024,
2,
16
]
],
"date-time": "2024-02-16T18:25:49Z",
"timestamp": 1708107949000
},
"editor": [
{
"affiliation": [],
"family": "Bhattarai",
"given": "Ajaya",
"sequence": "first"
}
],
"indexed": {
"date-parts": [
[
2024,
2,
17
]
],
"date-time": "2024-02-17T00:24:16Z",
"timestamp": 1708129456977
},
"is-referenced-by-count": 0,
"issue": "2",
"issued": {
"date-parts": [
[
2024,
2,
16
]
]
},
"journal-issue": {
"issue": "2",
"published-online": {
"date-parts": [
[
2024,
2,
16
]
]
}
},
"language": "en",
"license": [
{
"URL": "http://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2024,
2,
16
]
],
"date-time": "2024-02-16T00:00:00Z",
"timestamp": 1708041600000
}
}
],
"link": [
{
"URL": "https://dx.plos.org/10.1371/journal.pone.0297291",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "340",
"original-title": [],
"page": "e0297291",
"prefix": "10.1371",
"published": {
"date-parts": [
[
2024,
2,
16
]
]
},
"published-online": {
"date-parts": [
[
2024,
2,
16
]
]
},
"publisher": "Public Library of Science (PLoS)",
"reference": [
{
"DOI": "10.1111/irv.12497",
"article-title": "Burden of influenza, respiratory syncytial virus, and other respiratory viruses and the completeness of respiratory viral identification among respiratory inpatients, Canada, 2003–2014",
"author": "DL Schanzer",
"doi-asserted-by": "crossref",
"first-page": "113",
"journal-title": "Influenza Other Respir Viruses",
"key": "pone.0297291.ref001",
"volume": "12",
"year": "2018"
},
{
"key": "pone.0297291.ref002",
"unstructured": "Influenza (Seasonal). [cited 27 Jul 2023]. Available: https://www.who.int/news-room/fact-sheets/detail/influenza-(seasonal)."
},
{
"article-title": "Respiratory syncytial virus infection and novel interventions",
"author": "AC Langedijk",
"first-page": "1",
"journal-title": "Nat Rev Microbiol",
"key": "pone.0297291.ref003",
"year": "2023"
},
{
"DOI": "10.1016/j.ebiom.2023.104593",
"article-title": "Viral respiratory infections in a rapidly changing climate: the need to prepare for the next pandemic",
"author": "Y He",
"doi-asserted-by": "crossref",
"first-page": "104593",
"journal-title": "EBioMedicine",
"key": "pone.0297291.ref004",
"volume": "93",
"year": "2023"
},
{
"DOI": "10.1007/s00784-023-05078-z",
"article-title": "The role of the oral cavity in SARS-CoV-2- and other viral infections",
"author": "D. Hoffmann",
"doi-asserted-by": "crossref",
"first-page": "15",
"journal-title": "Clin Oral Investig",
"key": "pone.0297291.ref005",
"volume": "27",
"year": "2023"
},
{
"DOI": "10.2166/wh.2023.057",
"article-title": "Respiratory virus concentrations in human excretions that contribute to wastewater: a systematic review and meta-analysis",
"author": "SA Lowry",
"doi-asserted-by": "crossref",
"first-page": "831",
"journal-title": "J Water Health",
"key": "pone.0297291.ref006",
"volume": "21",
"year": "2023"
},
{
"DOI": "10.1038/s41591-021-01296-8",
"article-title": "SARS-CoV-2 infection of the oral cavity and saliva",
"author": "N Huang",
"doi-asserted-by": "crossref",
"first-page": "892",
"journal-title": "Nat Med",
"key": "pone.0297291.ref007",
"volume": "27",
"year": "2021"
},
{
"DOI": "10.1007/s00784-023-04953-z",
"article-title": "Preprocedural mouthwashes for infection control in dentistry—an update",
"author": "J Weber",
"doi-asserted-by": "crossref",
"first-page": "33",
"journal-title": "Clin Oral Investig",
"key": "pone.0297291.ref008",
"volume": "27",
"year": "2023"
},
{
"DOI": "10.1177/0022034520967933",
"article-title": "Antiviral Activity of Reagents in Mouth Rinses against SARS-CoV-2",
"author": "F Carrouel",
"doi-asserted-by": "crossref",
"first-page": "124",
"journal-title": "J Dent Res",
"key": "pone.0297291.ref009",
"volume": "100",
"year": "2021"
},
{
"DOI": "10.1111/j.1600-051X.2008.01230.x",
"article-title": "Surfactive and antibacterial activity of cetylpyridinium chloride formulations in vitro and in vivo",
"author": "HJ Busscher",
"doi-asserted-by": "crossref",
"first-page": "547",
"journal-title": "J Clin Periodontol",
"key": "pone.0297291.ref010",
"volume": "35",
"year": "2008"
},
{
"article-title": "Efficacy of cetylpyridinium chloride used as oropharyngeal antiseptic",
"author": "FA Pitten",
"first-page": "588",
"journal-title": "Arzneimittelforschung",
"key": "pone.0297291.ref011",
"volume": "51",
"year": "2001"
},
{
"DOI": "10.1002/jmv.26514",
"article-title": "Lowering the transmission and spread of human coronavirus",
"author": "C Meyers",
"doi-asserted-by": "crossref",
"first-page": "1605",
"journal-title": "J Med Virol",
"key": "pone.0297291.ref012",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.1080/20002297.2022.2030094",
"article-title": "Cetylpyridinium chloride promotes disaggregation of SARS-CoV-2 virus-like particles",
"author": "M Bañó-Polo",
"doi-asserted-by": "crossref",
"first-page": "2030094",
"journal-title": "J Oral Microbiol",
"key": "pone.0297291.ref013",
"volume": "14",
"year": "2022"
},
{
"DOI": "10.1111/jcpe.13746",
"article-title": "Randomized clinical trial to assess the impact of oral intervention with cetylpyridinium chloride to reduce salivary SARS-CoV-2 viral load",
"author": "R Tarragó-Gil",
"doi-asserted-by": "crossref",
"first-page": "288",
"journal-title": "J Clin Periodontol",
"key": "pone.0297291.ref014",
"volume": "50",
"year": "2023"
},
{
"DOI": "10.1177/00220345231156415",
"article-title": "Efficacy of a Mouthwash Containing CHX and CPC in SARS-CoV-2-Positive Patients: A Randomized Controlled Clinical Trial",
"author": "EL Bonn",
"doi-asserted-by": "crossref",
"first-page": "608",
"journal-title": "J Dent Res",
"key": "pone.0297291.ref015",
"volume": "102",
"year": "2023"
},
{
"DOI": "10.1177/00220345211029269",
"article-title": "Mouthwashes with CPC Reduce the Infectivity of SARS-CoV-2 Variants In Vitro",
"author": "J Muñoz-Basagoiti",
"doi-asserted-by": "crossref",
"first-page": "1265",
"journal-title": "J Dent Res",
"key": "pone.0297291.ref016",
"volume": "100",
"year": "2021"
},
{
"DOI": "10.2147/RMHP.S287547",
"article-title": "Dental Practitioners’ Knowledge, Attitude and Practices for Mouthwash Use Amidst the COVID-19 Pandemic",
"author": "E Imran",
"doi-asserted-by": "crossref",
"first-page": "605",
"journal-title": "Risk Manag Healthc Policy",
"key": "pone.0297291.ref017",
"volume": "14",
"year": "2021"
},
{
"DOI": "10.1128/JVI.00023-19",
"article-title": "High-Throughput Screening and Identification of Potent Broad-Spectrum Inhibitors of Coronaviruses",
"author": "L Shen",
"doi-asserted-by": "crossref",
"first-page": "e00023",
"journal-title": "J Virol",
"key": "pone.0297291.ref018",
"volume": "93",
"year": "2019"
},
{
"DOI": "10.20411/pai.v2i2.200",
"article-title": "Cetylpyridinium Chloride (CPC) Exhibits Potent, Rapid Activity Against Influenza Viruses in vitro and in vivo",
"author": "DL Popkin",
"doi-asserted-by": "crossref",
"first-page": "253",
"journal-title": "Pathog Immun",
"key": "pone.0297291.ref019",
"volume": "2",
"year": "2017"
},
{
"DOI": "10.1111/omi.12408",
"article-title": "Efficacy of Cetylpyridinium Chloride mouthwash against SARS-CoV-2: A systematic review of randomized controlled trials",
"author": "F D’Amico",
"doi-asserted-by": "crossref",
"first-page": "171",
"journal-title": "Mol Oral Microbiol",
"key": "pone.0297291.ref020",
"volume": "38",
"year": "2023"
},
{
"DOI": "10.1186/s12879-016-2177-8",
"article-title": "Randomized, double-blind, placebo-controlled clinical trial to assess the safety and effectiveness of a novel dual-action oral topical formulation against upper respiratory infections",
"author": "PK Mukherjee",
"doi-asserted-by": "crossref",
"first-page": "74",
"journal-title": "BMC Infect Dis",
"key": "pone.0297291.ref021",
"volume": "17",
"year": "2017"
},
{
"article-title": "Cetylpyridinium Chloride: Mechanism of Action, Antimicrobial Efficacy in Biofilms, and Potential Risks of Resistance",
"author": "X Mao",
"first-page": "e00576",
"journal-title": "Antimicrob Agents Chemother",
"key": "pone.0297291.ref022",
"volume": "64",
"year": "2020"
},
{
"DOI": "10.1177/0022034520943574",
"article-title": "Interventions to Reduce Aerosolized Microbes in Dental Practice: A Systematic Review with Network Meta-analysis of Randomized Controlled Trials",
"author": "D Koletsi",
"doi-asserted-by": "crossref",
"first-page": "1228",
"journal-title": "J Dent Res",
"key": "pone.0297291.ref023",
"volume": "99",
"year": "2020"
},
{
"DOI": "10.1177/00220345900690030901",
"article-title": "In vitro Virucidal Effectiveness of a 0.12%-Chlorhexidine Gluconate Mouthrinse",
"author": "D Bernstein",
"doi-asserted-by": "crossref",
"first-page": "874",
"journal-title": "J Dent Res",
"key": "pone.0297291.ref024",
"volume": "69",
"year": "1990"
},
{
"DOI": "10.1007/s00784-020-03413-2",
"article-title": "Is the oral cavity relevant in SARS-CoV-2 pandemic?",
"author": "D Herrera",
"doi-asserted-by": "crossref",
"first-page": "2925",
"journal-title": "Clin Oral Investig",
"key": "pone.0297291.ref025",
"volume": "24",
"year": "2020"
},
{
"DOI": "10.1038/s41368-020-0075-9",
"article-title": "Transmission routes of 2019-nCoV and controls in dental practice",
"author": "X Peng",
"doi-asserted-by": "crossref",
"first-page": "9",
"journal-title": "Int J Oral Sci",
"key": "pone.0297291.ref026",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3389/fmicb.2022.880394",
"article-title": "Identification of Cytoplasmic Chaperone Networks Relevant for Respiratory Syncytial Virus Replication",
"author": "V Latorre",
"doi-asserted-by": "crossref",
"first-page": "880394",
"journal-title": "Front Microbiol",
"key": "pone.0297291.ref027",
"volume": "13",
"year": "2022"
},
{
"DOI": "10.1016/j.virol.2012.09.022",
"article-title": "A stabilized respiratory syncytial virus reverse genetics system amenable to recombination-mediated mutagenesis",
"author": "AL Hotard",
"doi-asserted-by": "crossref",
"first-page": "129",
"journal-title": "Virology",
"key": "pone.0297291.ref028",
"volume": "434",
"year": "2012"
},
{
"DOI": "10.1016/j.jhin.2023.06.022",
"article-title": "Effectiveness of mouth rinses against COVID-19: a systematic review and network meta-analysis",
"author": "S-Y Lin",
"doi-asserted-by": "crossref",
"first-page": "175",
"journal-title": "J Hosp Infect",
"key": "pone.0297291.ref029",
"volume": "139",
"year": "2023"
},
{
"DOI": "10.1590/1807-3107bor-2023.vol37.0038",
"article-title": "Efficacy of mouthrinses in reducing oral SARS-COV-2 load: a review",
"author": "CM Pannuti",
"doi-asserted-by": "crossref",
"first-page": "e038",
"journal-title": "Braz Oral Res",
"key": "pone.0297291.ref030",
"volume": "37",
"year": "2023"
},
{
"DOI": "10.1038/ja.2009.56",
"article-title": "In vitro evaluation of the antimicrobial activity of HM-242, a novel antiseptic compound",
"author": "J Okunishi",
"doi-asserted-by": "crossref",
"first-page": "489",
"journal-title": "J Antibiot (Tokyo)",
"key": "pone.0297291.ref031",
"volume": "62",
"year": "2009"
},
{
"DOI": "10.1016/j.cmi.2021.04.009",
"article-title": "Disinfectant effectiveness against SARS-CoV-2 and influenza viruses present on human skin: model-based evaluation",
"author": "R Hirose",
"doi-asserted-by": "crossref",
"first-page": "1042",
"journal-title": "Clin Microbiol Infect",
"key": "pone.0297291.ref032",
"volume": "27",
"year": "2021"
},
{
"DOI": "10.1016/S0195-6701(85)80023-2",
"article-title": "The disinfection of respiratory syncytial virus by isopropanol and a chlorhexidine-detergent handwash",
"author": "J Platt",
"doi-asserted-by": "crossref",
"first-page": "89",
"journal-title": "J Hosp Infect",
"key": "pone.0297291.ref033",
"volume": "6",
"year": "1985"
},
{
"DOI": "10.3390/v15071433",
"article-title": "Cetylpyridinium Chloride-Containing Mouthwashes Show Virucidal Activity against Herpes Simplex Virus Type 1",
"author": "E Riveira-Muñoz",
"doi-asserted-by": "crossref",
"first-page": "1433",
"journal-title": "Viruses",
"key": "pone.0297291.ref034",
"volume": "15",
"year": "2023"
},
{
"DOI": "10.1016/j.identj.2023.08.009",
"article-title": "Antimicrobial Mouthwashes: An Overview of Mechanisms-What Do We Still Need to Know?",
"author": "Z Brookes",
"doi-asserted-by": "crossref",
"first-page": "S64",
"issue": "2",
"journal-title": "Int Dent J",
"key": "pone.0297291.ref035",
"volume": "73",
"year": "2023"
},
{
"DOI": "10.1016/j.identj.2023.08.010",
"article-title": "Mouthwash Effects on the Oral Microbiome: Are They Good, Bad, or Balanced?",
"author": "Z Brookes",
"doi-asserted-by": "crossref",
"first-page": "S74",
"issue": "2",
"journal-title": "Int Dent J",
"key": "pone.0297291.ref036",
"volume": "73",
"year": "2023"
},
{
"article-title": "Chlorhexidine as a Disinfectant in the Prosthodontic Practice: A Comprehensive Review",
"author": "H Alqarni",
"first-page": "e30566",
"journal-title": "Cureus",
"key": "pone.0297291.ref037",
"volume": "14",
"year": "2022"
},
{
"DOI": "10.1016/j.identj.2022.01.005",
"article-title": "Chlorhexidine in Dentistry: Pharmacology, Uses, and Adverse Effects",
"author": "F Poppolo Deus",
"doi-asserted-by": "crossref",
"first-page": "269",
"journal-title": "Int Dent J",
"key": "pone.0297291.ref038",
"volume": "72",
"year": "2022"
},
{
"article-title": "Fields Virology: Fundamentals",
"author": "Howley",
"journal-title": "Wolters Kluwer",
"key": "pone.0297291.ref039",
"year": "2023"
}
],
"reference-count": 39,
"references-count": 39,
"relation": {},
"resource": {
"primary": {
"URL": "https://dx.plos.org/10.1371/journal.pone.0297291"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Multidisciplinary"
],
"subtitle": [],
"title": "Cetylpyridinium chloride and chlorhexidine show antiviral activity against Influenza A virus and Respiratory Syncytial virus in vitro",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1371/journal.pone.corrections_policy",
"volume": "19"
}
