COVID-19: Poor outcomes in patients with zinc deficiency
et al., International Journal of Infectious Diseases, doi:10.1016/j.ijid.2020.09.014, Sep 2020
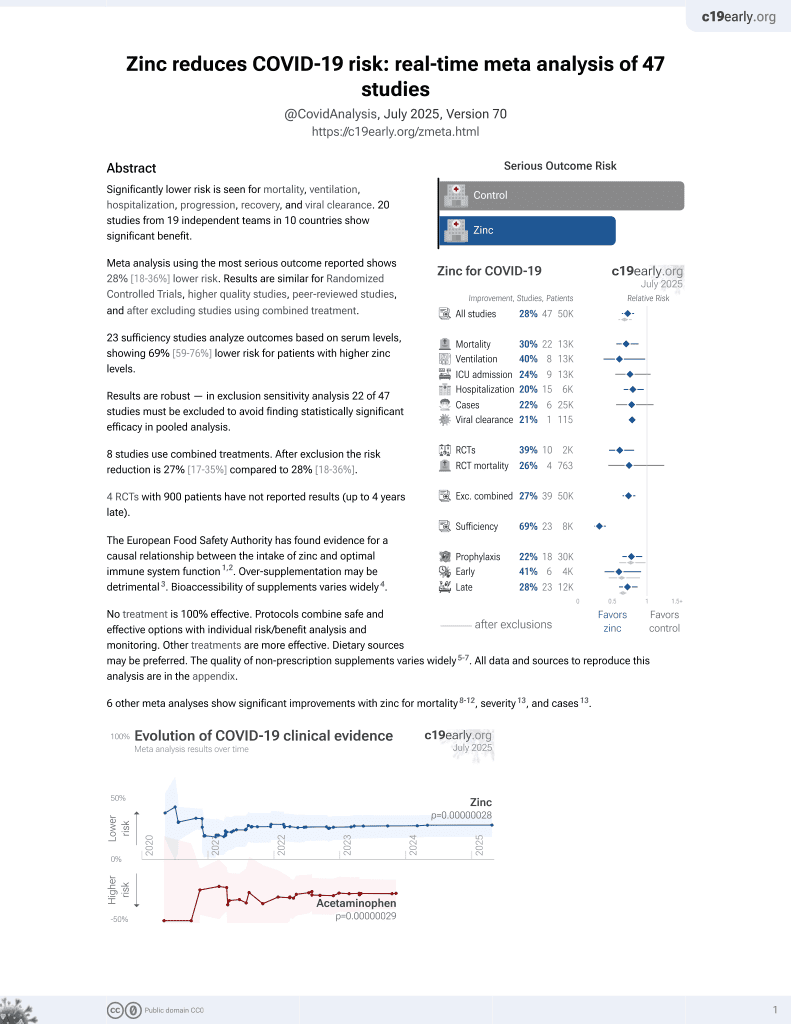
Zinc for COVID-19
2nd treatment shown to reduce risk in
July 2020, now with p = 0.00000012 from 41 studies, recognized in 23 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
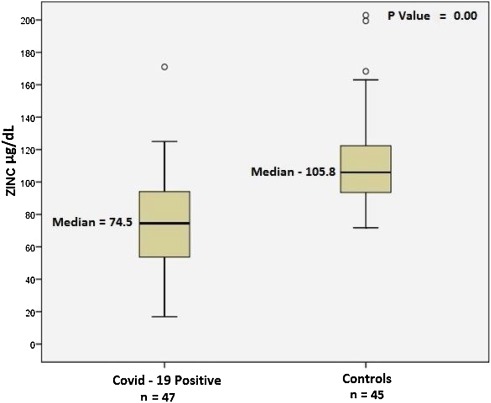
Prospective study of zinc levels in 47 hospitalized COVID-19 patients and 45 healthy controls. COVID-19 patients had significantly lower zinc levels (74.5 vs. 105.8 median μg/dl, p < 0.001). 57.4% of COVID-19 patients were zinc deficient, and they had higher rates of complications, ARDS, prolonged hospital stay, and increased mortality.
|
risk of death, 89.7% lower, RR 0.10, p = 0.06, high zinc levels 0 of 20 (0.0%), low zinc levels 5 of 27 (18.5%), NNT 5.4, relative risk is not 0 because of continuity correction due to zero events (with reciprocal of the contrasting arm).
|
|
risk of ICU admission, 92.4% lower, RR 0.08, p = 0.02, high zinc levels 0 of 20 (0.0%), low zinc levels 7 of 27 (25.9%), NNT 3.9, relative risk is not 0 because of continuity correction due to zero events (with reciprocal of the contrasting arm).
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Jothimani et al., 10 Sep 2020, prospective, India, peer-reviewed, 11 authors.
COVID-19: Poor outcomes in patients with zinc deficiency
International Journal of Infectious Diseases, doi:10.1016/j.ijid.2020.09.014
Background: Zinc is a trace element with potent immunoregulatory and antiviral properties, and is utilized in the treatment of coronavirus disease 2019 . However, we do not know the clinical significance of serum Zinc levels in COVID-19 patients. The aim of this study was to determine the clinical significance of serum zinc in COVID-19 patients and to establish a correlation with disease severity. Methods: This was a prospective study of fasting zinc levels in COVID-19 patients at the time of hospitalization. An initial comparative analysis was conducted between COVID-19 patients and healthy controls. COVID-19 patients with zinc deficiency were compared to those with normal zinc levels. Results: COVID-19 patients (n = 47) showed significantly lower zinc levels when compared to healthy controls (n = 45): median 74.5 (interquartile range 53.4-94.6) mg/dl vs 105.8 (interquartile range 95.65-120.90) mg/dl (p < 0.001). Amongst the COVID-19 patients, 27 (57.4%) were found to be zinc deficient. These patients were found to have higher rates of complications (p = 0.009), acute respiratory distress syndrome (18.5% vs 0%, p = 0.06), corticosteroid therapy (p = 0.02), prolonged hospital stay (p = 0.05), and increased mortality (18.5% vs 0%, p = 0.06). The odds ratio (OR) of developing complications was 5.54 for zinc deficient COVID-19 patients. Conclusions: The study data clearly show that a significant number of COVID-19 patients were zinc deficient. These zinc deficient patients developed more complications, and the deficiency was associated with a prolonged hospital stay and increased mortality.
Conflict of interest
References
Adhikari, Meng, Wu, Epidemiology, causes, clinical manifestation and diagnosis, prevention and control of coronavirus disease (COVID-19) during the early outbreak period: a scoping review, Infect Dis Poverty, doi:10.1186/s40249-020-00646-x
Alexander, Tinkov, Strand, Alehagen, Skalny et al., Early nutritional interventions with zinc, selenium and vitamin D for raising anti-viral resistance against progressive COVID-19, Nutrients, doi:10.3390/nu12082358
Barocas, So-Armah, Cheng, Zinc deficiency and advanced liver fibrosis among HIV and hepatitis C co-infected anti-retroviral naïve persons with alcohol use in Russia, PLoS One, doi:10.1371/journal.pone.0218852
Devaux, Rolain, Raoult, ACE2 receptor polymorphism: susceptibility to SARS-CoV-2, hypertension, multi-organ failure, and COVID-19 disease outcome, J Microbiol Immunol Infect, doi:10.1016/j.jmii.2020.04.015
Ferrari, Wright-Minogue, Fang, Baroudy, Lau et al., Characterization of soluble hepatitis C virus RNA-dependent RNA polymerase expressed in Escherichia coli, J Virol, doi:10.1128/JVI.73.2.1649-1654.1999
Galimberti, Baldini, Baratè, The CoV-2 outbreak: how hematologists could help to fight Covid-19, Pharmacol Res, doi:10.1016/j.phrs.2020.104866
Ghaffari, Tavakoli, Moradi, Inhibition of H1N1 influenza virus infection by zinc oxide nanoparticles: another emerging application of nanomedicine, J Biomed Sci, doi:10.1186/s12929-019-0563-4
Haraguchi, Sakurai, Hussain, Anner, Hoshino, Inhibition of HIV-1 infection by zinc group metal compounds, Antiviral Res, doi:10.1016/s0166-3542(99)00040-6
Henry, Aggarwal, Wong, Lactate dehydrogenase levels predict coronavirus disease
Henry, Aggarwal, Wong, Lactate dehydrogenase levels predict coronavirus disease 2019 (COVID-19) severity and mortality: a pooled analysis, Am J Emerg Med, doi:10.1016/j.ajem.2020.05.073Epubaheadofprint
Iddir, Brito, Dingeo, International Zinc Nutrition Consultative Group (IZiNCG) technical document #1. Assessment of the risk of zinc deficiency in populations and options for its control, Food Nutr Bull, doi:10.3390/nu12061562
Kato, Mcgowan, Machado, Lactate dehydrogenase as a biomarker of hemolysis-associated nitric oxide resistance, priapism, leg ulceration, pulmonary hypertension, and death in patients with sickle cell disease, Blood, doi:10.1182/blood-2005-06-2373
Ko, Morihara, Shibata, Factors attenuating zinc deficiency improvement in direct-acting antiviral agent-treated chronic hepatitis C virus infection, Nutrients, doi:10.3390/nu10111620Pub-lished2018November2
Kumar, Kubota, Chernov, Kasuya, Potential role of zinc supplementation in prophylaxis and treatment of COVID-19
Li, Li, Zhang, Wang, Expression of the SARS-CoV-2 cell receptor gene ACE2 in a wide variety of human tissues, Infect Dis Poverty, doi:10.1186/s40249-020-00662-x
Prasad, Bao, Beck, Sarkar, Zinc activates NF-kappaB in HUT-78 cells, J Lab Clin Med, doi:10.1067/mlc.2001.118108
Prasad, Zinc in human health: effect of zinc on immune cells, Mol Med, doi:10.2119/2008-00033.Prasad
Rahman, Idid, Can Zn Be a critical element in COVID-19 treatment?
Read, Obeid, Ahlenstiel, Ahlenstiel, The role of zinc in antiviral immunity, Adv Nutr, doi:10.1093/advances/
Reeves, Dell, An experimental study of the effect of zinc on the activity of angiotensin converting enzyme in serum, Clin Chem, doi:10.1093/advances/nmz013
Shankar, Prasad, Zinc and immune function: the biological basis of altered resistance to infection, Am J Clin Nutr, doi:10.1093/ajcn/68.2.447S
Shi, Li, Zhou, Lactate dehydrogenase and susceptibility to deterioration of mild COVID-19 patients: a multicenter nested case-control study, BMC Med, doi:10.1186/s12916-020-01633-7
Skalny, Rink, Ajsuvakova, Zinc and respiratory tract infections: perspectives for COVID-19 (Review), Int J Mol Med, doi:10.3892/ijmm.2020.4575
Towler, Staker, Prasad, ACE2 X-ray structures reveal a large hingebending motion important for inhibitor binding and catalysis, J Biol Chem, doi:10.1074/jbc.M311191200
Velthuis, Van Den Worm, Sims, Baric, Snijder et al., Zn(2 +) inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture, PLoS Pathog, doi:10.1371/journal.ppat.1001176Pub-lished2010
Wessels, Rolles, Rink, The potential impact of zinc supplementation on COVID-19 pathogenesis, Front Immunol, doi:10.3389/fimmu.2020.01712
Wintergerst, Maggini, Hornig, Immune-enhancing role of vitamin C and zinc and effect on clinical conditions, Ann Nutr Metab, doi:10.1159/000090495
Xue, Moyer, Peng, Wu, Hannafon et al., Chloroquine is a zinc ionophore, PLoS One, doi:10.1371/journal.pone.0109180
Yang, Zheng, Gou, Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis, Int J Infect Dis, doi:10.1016/j.ijid.2020.03.017
Yazdanpanah, Hamblin, Rezaei, The immune system and COVID-19: Friend or foe?
DOI record:
{
"DOI": "10.1016/j.ijid.2020.09.014",
"ISSN": [
"1201-9712"
],
"URL": "http://dx.doi.org/10.1016/j.ijid.2020.09.014",
"alternative-id": [
"S120197122030730X"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "COVID-19: Poor outcomes in patients with zinc deficiency"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "International Journal of Infectious Diseases"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.ijid.2020.09.014"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2020 Published by Elsevier Ltd on behalf of International Society for Infectious Diseases."
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0003-4189-690X",
"affiliation": [],
"authenticated-orcid": false,
"family": "Jothimani",
"given": "Dinesh",
"sequence": "first"
},
{
"affiliation": [],
"family": "Kailasam",
"given": "Ezhilarasan",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-6468-5641",
"affiliation": [],
"authenticated-orcid": false,
"family": "Danielraj",
"given": "Silas",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Nallathambi",
"given": "Balaji",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ramachandran",
"given": "Hemalatha",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sekar",
"given": "Padmini",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Manoharan",
"given": "Shruthi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ramani",
"given": "Vidyalakshmi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Narasimhan",
"given": "Gomathy",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kaliamoorthy",
"given": "Ilankumaran",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Rela",
"given": "Mohamed",
"sequence": "additional"
}
],
"container-title": "International Journal of Infectious Diseases",
"container-title-short": "International Journal of Infectious Diseases",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"ijidonline.com",
"clinicalkey.jp",
"clinicalkey.com",
"clinicalkey.es",
"clinicalkey.fr",
"clinicalkey.com.au",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2020,
9,
10
]
],
"date-time": "2020-09-10T15:43:09Z",
"timestamp": 1599752589000
},
"deposited": {
"date-parts": [
[
2021,
6,
10
]
],
"date-time": "2021-06-10T06:34:42Z",
"timestamp": 1623306882000
},
"indexed": {
"date-parts": [
[
2022,
9,
28
]
],
"date-time": "2022-09-28T23:07:36Z",
"timestamp": 1664406456041
},
"is-referenced-by-count": 145,
"issued": {
"date-parts": [
[
2020,
11
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2020,
11,
1
]
],
"date-time": "2020-11-01T00:00:00Z",
"timestamp": 1604188800000
}
},
{
"URL": "http://creativecommons.org/licenses/by-nc-nd/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2020,
9,
7
]
],
"date-time": "2020-09-07T00:00:00Z",
"timestamp": 1599436800000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S120197122030730X?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S120197122030730X?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "343-349",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2020,
11
]
]
},
"published-print": {
"date-parts": [
[
2020,
11
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1186/s40249-020-00646-x",
"article-title": "Epidemiology, causes, clinical manifestation and diagnosis, prevention and control of coronavirus disease (COVID-19) during the early outbreak period: a scoping review",
"author": "Adhikari",
"doi-asserted-by": "crossref",
"first-page": "29",
"issue": "1",
"journal-title": "Infect Dis Poverty",
"key": "10.1016/j.ijid.2020.09.014_bib0005",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.3390/nu12082358",
"article-title": "Early nutritional interventions with zinc, selenium and vitamin D for raising anti-viral resistance against progressive COVID-19",
"author": "Alexander",
"doi-asserted-by": "crossref",
"first-page": "E2358",
"issue": "8",
"journal-title": "Nutrients",
"key": "10.1016/j.ijid.2020.09.014_bib0010",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0218852",
"article-title": "Zinc deficiency and advanced liver fibrosis among HIV and hepatitis C co-infected anti-retroviral naïve persons with alcohol use in Russia",
"author": "Barocas",
"doi-asserted-by": "crossref",
"issue": "6",
"journal-title": "PLoS One",
"key": "10.1016/j.ijid.2020.09.014_bib0015",
"volume": "14",
"year": "2019"
},
{
"DOI": "10.1016/j.jmii.2020.04.015",
"article-title": "ACE2 receptor polymorphism: susceptibility to SARS-CoV-2, hypertension, multi-organ failure, and COVID-19 disease outcome",
"author": "Devaux",
"doi-asserted-by": "crossref",
"first-page": "425",
"issue": "3",
"journal-title": "J Microbiol Immunol Infect",
"key": "10.1016/j.ijid.2020.09.014_bib0020",
"volume": "53",
"year": "2020"
},
{
"DOI": "10.1128/JVI.73.2.1649-1654.1999",
"article-title": "Characterization of soluble hepatitis C virus RNA-dependent RNA polymerase expressed in Escherichia coli",
"author": "Ferrari",
"doi-asserted-by": "crossref",
"first-page": "1649",
"issue": "2",
"journal-title": "J Virol",
"key": "10.1016/j.ijid.2020.09.014_bib0025",
"volume": "73",
"year": "1999"
},
{
"DOI": "10.1016/j.phrs.2020.104866",
"article-title": "The CoV-2 outbreak: how hematologists could help to fight Covid-19",
"author": "Galimberti",
"doi-asserted-by": "crossref",
"first-page": "104866",
"journal-title": "Pharmacol Res",
"key": "10.1016/j.ijid.2020.09.014_bib0030",
"volume": "157",
"year": "2020"
},
{
"DOI": "10.1186/s12929-019-0563-4",
"article-title": "Inhibition of H1N1 influenza virus infection by zinc oxide nanoparticles: another emerging application of nanomedicine",
"author": "Ghaffari",
"doi-asserted-by": "crossref",
"first-page": "70",
"issue": "1",
"journal-title": "J Biomed Sci",
"key": "10.1016/j.ijid.2020.09.014_bib0035",
"volume": "26",
"year": "2019"
},
{
"DOI": "10.1016/S0166-3542(99)00040-6",
"article-title": "Inhibition of HIV-1 infection by zinc group metal compounds",
"author": "Haraguchi",
"doi-asserted-by": "crossref",
"first-page": "123",
"issue": "2",
"journal-title": "Antiviral Res",
"key": "10.1016/j.ijid.2020.09.014_bib0040",
"volume": "43",
"year": "1999"
},
{
"DOI": "10.1016/j.ajem.2020.05.073",
"article-title": "Lactate dehydrogenase levels predict coronavirus disease 2019 (COVID-19) severity and mortality: a pooled analysis [published online ahead of print, 2020 May 27]",
"author": "Henry",
"doi-asserted-by": "crossref",
"first-page": "1722",
"journal-title": "Am J Emerg Med",
"key": "10.1016/j.ijid.2020.09.014_bib0045",
"volume": "38",
"year": "2020"
},
{
"DOI": "10.1016/j.ajem.2020.05.073",
"article-title": "Lactate dehydrogenase levels predict coronavirus disease 2019 (COVID-19) severity and mortality: a pooled analysis",
"author": "Henry",
"doi-asserted-by": "crossref",
"journal-title": "Am J Emerg Med",
"key": "10.1016/j.ijid.2020.09.014_bib0050",
"year": "2020"
},
{
"DOI": "10.3390/nu12061562",
"article-title": "Strengthening the immune system and reducing inflammation and oxidative stress through diet and nutrition: considerations during the COVID-19 crisis",
"author": "Iddir",
"doi-asserted-by": "crossref",
"first-page": "E1562",
"issue": "6",
"journal-title": "Nutrients",
"key": "10.1016/j.ijid.2020.09.014_bib0055",
"volume": "12",
"year": "2020"
},
{
"article-title": "International Zinc Nutrition Consultative Group (IZiNCG) technical document #1. Assessment of the risk of zinc deficiency in populations and options for its control",
"author": "International Zinc Nutrition Consultative Group (IZiNCG)",
"first-page": "S99",
"issue": "1 Suppl 2",
"journal-title": "Food Nutr Bull",
"key": "10.1016/j.ijid.2020.09.014_bib0060",
"volume": "25",
"year": "2004"
},
{
"DOI": "10.1182/blood-2005-06-2373",
"article-title": "Lactate dehydrogenase as a biomarker of hemolysis-associated nitric oxide resistance, priapism, leg ulceration, pulmonary hypertension, and death in patients with sickle cell disease",
"author": "Kato",
"doi-asserted-by": "crossref",
"first-page": "2279",
"issue": "6",
"journal-title": "Blood",
"key": "10.1016/j.ijid.2020.09.014_bib0065",
"volume": "107",
"year": "2006"
},
{
"DOI": "10.3390/nu10111620",
"article-title": "Factors attenuating zinc deficiency improvement in direct-acting antiviral agent-treated chronic hepatitis C virus infection",
"author": "Ko",
"doi-asserted-by": "crossref",
"first-page": "1620",
"issue": "11",
"journal-title": "Nutrients",
"key": "10.1016/j.ijid.2020.09.014_bib0070",
"volume": "10",
"year": "2018"
},
{
"DOI": "10.1016/j.mehy.2020.109848",
"article-title": "Potential role of zinc supplementation in prophylaxis and treatment of COVID-19 [published online ahead of print, 2020 May 25]",
"author": "Kumar",
"doi-asserted-by": "crossref",
"first-page": "109848",
"journal-title": "Med Hypotheses",
"key": "10.1016/j.ijid.2020.09.014_bib0075",
"volume": "144",
"year": "2020"
},
{
"DOI": "10.1186/s40249-020-00662-x",
"article-title": "Expression of the SARS-CoV-2 cell receptor gene ACE2 in a wide variety of human tissues",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "45",
"issue": "1",
"journal-title": "Infect Dis Poverty",
"key": "10.1016/j.ijid.2020.09.014_bib0080",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.2119/2008-00033.Prasad",
"article-title": "Zinc in human health: effect of zinc on immune cells",
"author": "Prasad",
"doi-asserted-by": "crossref",
"first-page": "353",
"issue": "5–6",
"journal-title": "Mol Med",
"key": "10.1016/j.ijid.2020.09.014_bib0085",
"volume": "14",
"year": "2008"
},
{
"DOI": "10.1067/mlc.2001.118108",
"article-title": "Zinc activates NF-kappaB in HUT-78 cells",
"author": "Prasad",
"doi-asserted-by": "crossref",
"first-page": "250",
"issue": "4",
"journal-title": "J Lab Clin Med",
"key": "10.1016/j.ijid.2020.09.014_bib0090",
"volume": "138",
"year": "2001"
},
{
"article-title": "Can Zn Be a critical element in COVID-19 treatment? [published online ahead of print, 2020 May 26]",
"author": "Rahman",
"first-page": "1",
"journal-title": "Biol Trace Elem Res",
"key": "10.1016/j.ijid.2020.09.014_bib0095",
"year": "2020"
},
{
"DOI": "10.1093/advances/nmz013",
"article-title": "The role of zinc in antiviral immunity",
"author": "Read",
"doi-asserted-by": "crossref",
"first-page": "696",
"issue": "4",
"journal-title": "Adv Nutr",
"key": "10.1016/j.ijid.2020.09.014_bib0100",
"volume": "10",
"year": "2019"
},
{
"DOI": "10.1093/clinchem/31.4.581",
"article-title": "An experimental study of the effect of zinc on the activity of angiotensin converting enzyme in serum",
"author": "Reeves",
"doi-asserted-by": "crossref",
"first-page": "581",
"issue": "4",
"journal-title": "Clin Chem",
"key": "10.1016/j.ijid.2020.09.014_bib0105",
"volume": "31",
"year": "1985"
},
{
"DOI": "10.1093/ajcn/68.2.447S",
"article-title": "Zinc and immune function: the biological basis of altered resistance to infection",
"author": "Shankar",
"doi-asserted-by": "crossref",
"first-page": "447S",
"issue": "2 Suppl",
"journal-title": "Am J Clin Nutr",
"key": "10.1016/j.ijid.2020.09.014_bib0110",
"volume": "68",
"year": "1998"
},
{
"DOI": "10.1186/s12916-020-01633-7",
"article-title": "Lactate dehydrogenase and susceptibility to deterioration of mild COVID-19 patients: a multicenter nested case-control study",
"author": "Shi",
"doi-asserted-by": "crossref",
"first-page": "168",
"issue": "1",
"journal-title": "BMC Med",
"key": "10.1016/j.ijid.2020.09.014_bib0115",
"volume": "18",
"year": "2020"
},
{
"article-title": "Zinc and respiratory tract infections: perspectives for COVID-19 (Review)",
"author": "Skalny",
"first-page": "17",
"issue": "1",
"journal-title": "Int J Mol Med",
"key": "10.1016/j.ijid.2020.09.014_bib0120",
"volume": "46",
"year": "2020"
},
{
"DOI": "10.1371/journal.ppat.1001176",
"article-title": "Zn(2+) inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture",
"author": "te Velthuis",
"doi-asserted-by": "crossref",
"issue": "11",
"journal-title": "PLoS Pathog",
"key": "10.1016/j.ijid.2020.09.014_bib0125",
"volume": "6",
"year": "2010"
},
{
"DOI": "10.1074/jbc.M311191200",
"article-title": "ACE2 X-ray structures reveal a large hinge-bending motion important for inhibitor binding and catalysis",
"author": "Towler",
"doi-asserted-by": "crossref",
"first-page": "17996",
"issue": "17",
"journal-title": "J Biol Chem",
"key": "10.1016/j.ijid.2020.09.014_bib0130",
"volume": "279",
"year": "2004"
},
{
"DOI": "10.3389/fimmu.2020.01712",
"article-title": "The potential impact of zinc supplementation on COVID-19 pathogenesis",
"author": "Wessels",
"doi-asserted-by": "crossref",
"first-page": "1712",
"journal-title": "Front Immunol",
"key": "10.1016/j.ijid.2020.09.014_bib0135",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1159/000090495",
"article-title": "Immune-enhancing role of vitamin C and zinc and effect on clinical conditions",
"author": "Wintergerst",
"doi-asserted-by": "crossref",
"first-page": "85",
"issue": "2",
"journal-title": "Ann Nutr Metab",
"key": "10.1016/j.ijid.2020.09.014_bib0140",
"volume": "50",
"year": "2006"
},
{
"DOI": "10.1371/journal.pone.0109180",
"article-title": "Chloroquine is a zinc ionophore",
"author": "Xue",
"doi-asserted-by": "crossref",
"issue": "10",
"journal-title": "PLoS One",
"key": "10.1016/j.ijid.2020.09.014_bib0145",
"volume": "9",
"year": "2014"
},
{
"DOI": "10.1016/j.ijid.2020.03.017",
"article-title": "Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis",
"author": "Yang",
"doi-asserted-by": "crossref",
"first-page": "91",
"journal-title": "Int J Infect Dis",
"key": "10.1016/j.ijid.2020.09.014_bib0150",
"volume": "94",
"year": "2020"
},
{
"DOI": "10.1016/j.lfs.2020.117900",
"article-title": "The immune system and COVID-19: Friend or foe? [published online ahead of print, 2020 June 2]",
"author": "Yazdanpanah",
"doi-asserted-by": "crossref",
"first-page": "117900",
"journal-title": "Life Sci",
"key": "10.1016/j.ijid.2020.09.014_bib0155",
"volume": "256",
"year": "2020"
}
],
"reference-count": 31,
"references-count": 31,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S120197122030730X"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Infectious Diseases",
"Microbiology (medical)",
"General Medicine"
],
"subtitle": [],
"title": "COVID-19: Poor outcomes in patients with zinc deficiency",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "100"
}
