Vitamin D deficiency is associated with increased risk of delirium and mortality among critically Ill, elderly covid-19 patients
et al., Complementary Therapies in Medicine, doi:10.1016/j.ctim.2022.102855, Jul 2022
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 310 COVID-19 ICU patients in Iran, showing higher mortality for patients with vitamin D deficiency.
This is the 141st of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
|
risk of death, 74.7% lower, HR 0.25, p < 0.001, high D levels 157, low D levels 38, inverted to make HR<1 favor high D levels, >30ng/mL vs. <20ng/mL, model 2, day 45.
|
|
risk of death, 39.8% lower, HR 0.60, p = 0.05, high D levels 157, low D levels 38, inverted to make HR<1 favor high D levels, >30ng/mL vs. <20ng/mL, ICU mortality, model 2.
|
|
risk of mechanical ventilation, 44.9% higher, HR 1.45, p = 0.27, high D levels 157, low D levels 38, inverted to make HR<1 favor high D levels, >30ng/mL vs. <20ng/mL, model 2, day 45.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Gholi et al., 19 Jul 2022, prospective, Iran, peer-reviewed, 4 authors.
Contact: zahra.gholi@sbmu.ac.ir, hassan.eini@gmail.com, nutritiondata@yahoo.com.
Vitamin D deficiency is Associated with Increased Risk of Delirium and Mortality among Critically Ill, Elderly Covid-19 Patients
Complementary Therapies in Medicine, doi:10.1016/j.ctim.2022.102855
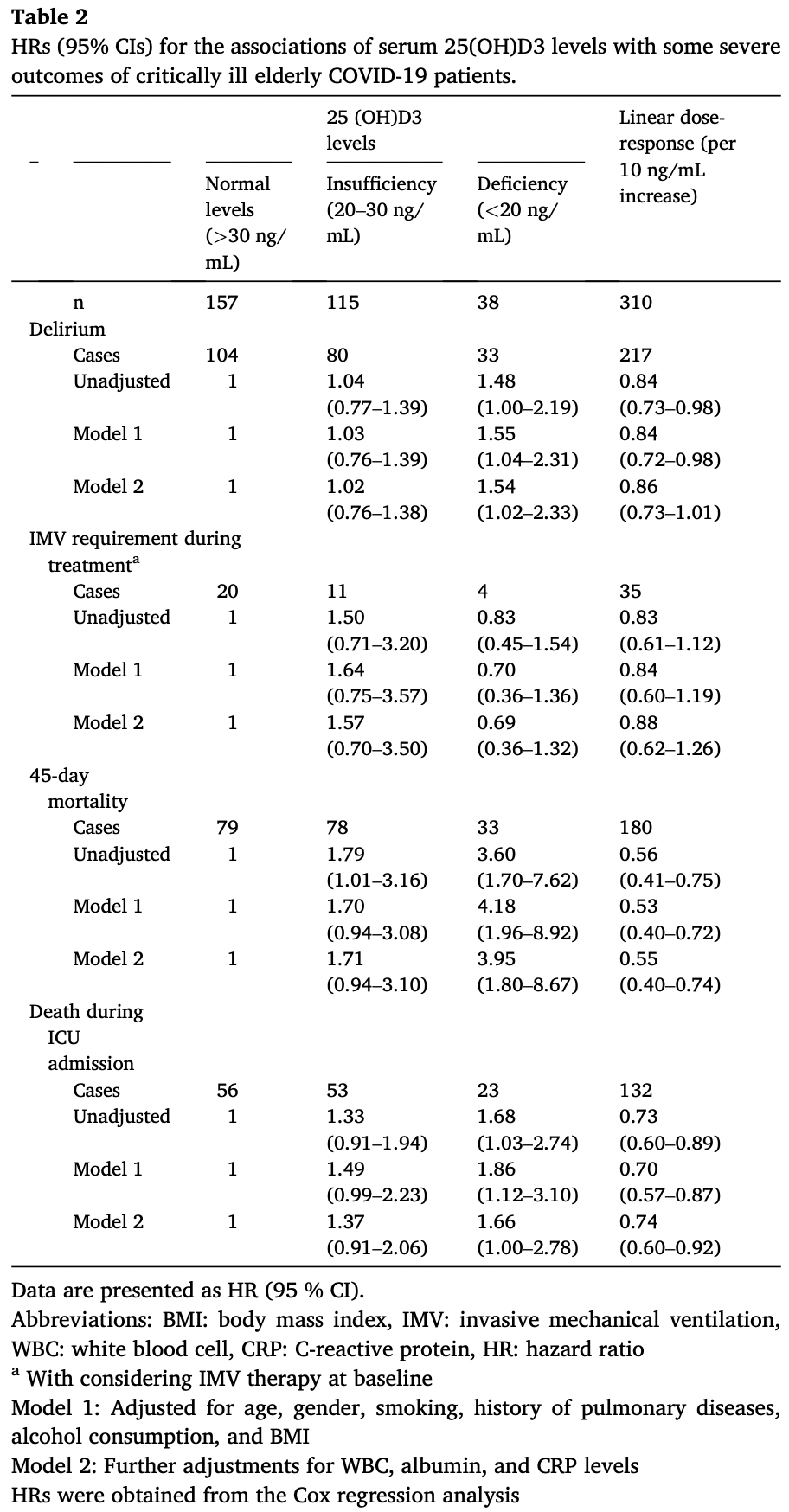
Background and aim: Data on the associations of vitamin D levels with severe outcomes of coronavirus disease 2019 (COVID-19) among critically ill elderly patients are not conclusive and also no information is available about some outcomes such as delirium. Therefore, the current study was done to assess these associations in critically ill elderly COVID-19 patients. Methods: In total, 310 critically ill COVID-19 patients, aged ≥ 65 years, were included in the current single center prospective study. All patients were hospitalized in the intensive care unit (ICU). We collected data on demographic characteristics, laboratory parameters, blood pressure, comorbidities, medications, and types of mechanical ventilation at baseline (the first day of ICU admission). Patients were categorized based on serum 25 (OH)D3 levels at the baseline [normal levels (>30 ng/mL), insufficiency (20-30 ng/mL), deficiency (<20 ng/ mL)]. Data on delirium incidence, mortality, invasive mechanical ventilation (IMV) requirement during treatment, length of ICU and hospital admission, and re-hospitalization were recorded until 45 days after the baseline. Results: Vitamin D deficiency and insufficiency were prevalent among 12 % and 37 % of study participants, respectively. In terms of baseline differences, patients with vitamin D deficiency were more likely to be older, have organ failure, take propofol, need IMV, and were less likely to need face mask compared to patients with normal levels of vitamin D. A significant positive association was found between vitamin D deficiency and risk of delirium. After controlling for potential confounders, patients with vitamin D deficiency had a 54 % higher risk of delirium compared to those with vitamin D sufficiency (HR: 1.54, 95 % CI: 1.02-2.33). Such a positive association was also seen for 45-day COVID-19 mortality (HR: 3.95, 95 % CI: 1.80-8.67). Also, each 10 ng/mL increase in vitamin D levels was associated with a 45 % and 26 % lower risk of 45-day mortality (HR: 0.55, 95 % CI: 0.40-0.74) and ICU mortality due to COVID-19 (HR: 0.74, 95 % CI: 0.60-0.92), respectively. In terms of other COVID-19 outcomes including IMV requirement during treatment, prolonged hospitalization, and rehospitalization, we found no significant association in relation to serum 25(OH)D3 levels either in crude or fully adjusted models. Conclusion: Vitamin D deficiency was associated with an increased risk of delirium and mortality among critically ill elderly COVID-19 patients.
Normal levels (>30 ng/mL) Insufficiency (20-30
Ethical approval All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Furthermore, we took written informed consent from each participant. The study was approved by the Ethics Committee of Shahid Beheshti University of Medical Sciences, Tehran, Iran.
CRediT authorship contribution statement ZGh, DY, HEZ, and ZVS designed the research project. ZGh and ZVS conducted the research; ZGh analyzed data; ZGh and ZVS wrote the paper; ZGh and ZVS had primary responsibility for final content. All authors read and approved the final manuscript.
Declaration of Competing Interest The authors report no declarations of interest.
Conflicts of interest Authors declared no personal or financial conflicts of interest.
Appendix A. Supporting information Supplementary data associated with this article can be found in the online version at doi:10.1016/j.ctim.2022.102855.
References
Alguwaihes, Al-Sofiani, Megdad, Diabetes and Covid-19 among hospitalized patients in Saudi Arabia: a single-centre retrospective study, Cardiovasc Diabetol
Alguwaihes, Sabico, Hasanato, Severe vitamin D deficiency is not related to SARS-CoV-2 infection but may increase mortality risk in hospitalized adults: a retrospective case-control study in an Arab Gulf country, Aging Clin Exp Res
Allard, Ouedraogo, Molleville, Malnutrition: percentage and association with prognosis in patients hospitalized for coronavirus disease 2019, Nutrients
Alsafar, Grant, Hijazi, COVID-19 disease severity and death in relation to vitamin D status among SARS-CoV-2-positive UAE residents, Nutrients
Amer, Alotaibi, Vitamin D status of Arab Gulf residents screened for SARS-CoV-2 and its association with COVID-19 infection: a multi-centre case-control study, J Transl Med
Amin, Drenos, No evidence that vitamin D is able to prevent or affect the severity of COVID-19 in individuals with European ancestry: a Mendelian randomisation study of open data, BMJ Nutr, Prev Health
Angelidi, Belanger, Lorinsky, Vitamin D status is associated with inhospital mortality and mechanical ventilation: a cohort of COVID-19 hospitalized patients, Mayo Clin Proc
Baeke, Takiishi, Korf, Gysemans, Mathieu, Vitamin D: modulator of the immune system, Curr Opin Pharmacol
Bilezikian, Bikle, Hewison, Mechanisms in endocrinology: vitamin D and COVID-19, Eur J Endocrinol
Bishop, Ismailova, Dimeloe, Hewison, White, Vitamin D and immune regulation: antibacterial, antiviral, anti-inflammatory, J Bone Miner Res
Bulca-Acar, Nur-Eke, Tas ¸kin, Köksal-Yasin, 25 (OH) vitamin D levels of patients with COVID-19 are not associated with the length of hospital stay, Clin Lab
Chai, Gao, Wu, Vitamin D deficiency as a risk factor for dementia and Alzheimer's disease: an updated meta-analysis, BMC Neurol
Chen, Mei, Xie, Low vitamin D levels do not aggravate COVID-19 risk or death, and vitamin D supplementation does not improve outcomes in hospitalized patients with COVID-19: a meta-analysis and GRADE assessment of cohort studies and RCTs, Nutr J
Ciotti, Ciccozzi, Pieri, Bernardini, The COVID-19 pandemic: viral variants and vaccine efficacy, Crit Rev Clin Lab Sci
Cole, Too many digits: the presentation of numerical data, Arch Dis Child
De Carvalho, Ribeiro, Aging, low-grade systemic inflammation and vitamin D: a mini-review, Eur J Clin Nutr
Evans, Lippman, Shining light on the COVID-19 pandemic: a vitamin D receptor checkpoint in defense of unregulated wound healing, Cell Metab
Fang, Li, Yu, Epidemiological, comorbidity factors with severity and prognosis of COVID-19: a systematic review and meta-analysis, Aging
Fedele, Francesco, Riso, Collo, Obesity, malnutrition, and trace element deficiency in the coronavirus disease (COVID-19) pandemic: an overview, Nutrition
Gold, Sehayek, Gabrielli, Zhang, Mccusker et al., COVID-19 and comorbidities: a systematic review and meta-analysis, Postgrad Med
Gusmao-Flores, Salluh, Chalhub, Quarantini, The confusion assessment method for the intensive care unit (CAM-ICU) and intensive care delirium screening checklist (ICDSC) for the diagnosis of delirium: a systematic review and metaanalysis of clinical studies, Crit Care
Hadizadeh, Supplementation with vitamin D in the COVID-19 pandemic?, Nutr Rev
Hariyanto, Intan, Hananto, Harapan, Kurniawan, Vitamin D supplementation and Covid-19 outcomes: a systematic review, meta-analysis and meta-regression, Rev Med Virol
Henry, Aggarwal, Wong, Lactate dehydrogenase levels predict coronavirus disease 2019 (COVID-19) severity and mortality: a pooled analysis, Am J Emerg Med
Hu, Kung, Cave, Banh, Effects of vitamin D serum level on morbidity and mortality in patients with COVID-19: a systematic review and meta-analysis, J Pharm Pharm Sci
Jeffery, Burke, Mura, Zheng, Qureshi et al., 1,25-Dihydroxyvitamin D3 and IL-2 combine to inhibit T cell production of inflammatory cytokines and promote development of regulatory T cells expressing CTLA-4 and FoxP3, J Immunol
Jenei, Jenei, Tamás, COVID-19 mortality is associated with low vitamin D levels in patients with risk factors and/or advanced age, Clin Nutr ESPEN
Kalueff, Eremin, Tuohimaa, Mechanisms of neuroprotective action of vitamin D(3), Biochem Biokhimiia
Kulkarni, Rajput, Dawre, Severe malnutrition and anemia are associated with severe COVID in infants, J Trop Pediatr
Kuo, Pilling, Atkins, Fortinsky, Kuchel et al., APOE e4 genotypes increase risk of delirium during COVID-19-related hospitalizations: evidence from a large UK Cohort, J Gerontol: Ser A
Lohia, Nguyen, Patel, Kapur, Exploring the link between vitamin D and clinical outcomes in COVID-19, Am J Physiol Endocrinol Metab
Luetz, Grunow, Mörgeli, Innovative ICU solutions to prevent and reduce delirium and post-intensive care unit syndrome, Semin Respir Crit Care Med
Menéndez, Giménez, Holick, Barrantes, Manucha, COVID-19 and neurological sequelae: vitamin D as a possible neuroprotective and/or neuroreparative agent, Life Sci
Mercola, Grant, Wagner, Evidence regarding vitamin D and risk of COVID-19 and its severity, Nutrients
Notz, Herrmann, Schlesinger, Vitamin D deficiency in critically ill COVID-19 ARDS patients, Clin Nutr
Oristrell, Oliva, Casado, Vitamin D supplementation and COVID-19 risk: a population-based, cohort study, J Endocrinol Investig
Patchen, Clark, Gaddis, Hancock, Cassano, Genetically predicted serum vitamin D and COVID-19: a Mendelian randomization study, Curr Dev Nutr
Pereira, Damascena, Azevedo, De Almeida Oliveira, Da Mota et al., Vitamin D deficiency aggravates COVID-19: systematic review and meta-analysis, Crit Rev Food Sci Nutr
Pilling, Jones, Masoli, Low vitamin D levels and risk of incident delirium in 351,000 older UK biobank participants, J Am Geriatr Soc
Pimentel, Vega, Pichard, Low vitamin D levels and increased neutrophil in patients admitted at ICU with COVID-19, Clin Nutr ESPEN
Qiu, Sessler, Chen, Preoperative vitamin D deficiency is associated with postoperative delirium in critically Ill patients, J Intensive care Med
Radujkovic, Hippchen, Tiwari-Heckler, Dreher, Boxberger, Vitamin D deficiency and outcome of COVID-19 patients, Nutrients
Rajpal, Rahimi, Ismail-Beigi, Factors leading to high morbidity and mortality of COVID-19 in patients with type 2 diabetes, J Diabetes
Reis, Fernandes, Sales, Influence of vitamin D status on hospital length of stay and prognosis in hospitalized patients with moderate to severe COVID-19: a multicenter prospective cohort study, Am J Clin Nutr
Richardson, Hirsch, Narasimhan, Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York city area, JAMA
Seal, Bertenthal, Carey, Grunfeld, Bikle et al., Association of vitamin D status and COVID-19-related hospitalization and mortality, J Gen Intern Med
Silverio, Gonçalves, Andrade, Seelaender, Coronavirus disease 2019 (COVID-19) and nutritional status: the missing link?, Adv Nutr
Subramanian, Rhodes, Taylor, Vitamin D, vitamin D -binding protein, free vitamin D and COVID-19 mortality in hospitalized patients, Am J Clin Nutr
Vanegas-Cedillo, Bello-Chavolla, Ramírez-Pedraza, Serum vitamin D levels are associated with increased COVID-19 severity and mortality independent of whole-body and visceral adiposity, Front Nutr
Velayati, Vahdat Shariatpanahi, Dehghan, Zayeri, Vahdat et al., Vitamin D and postoperative delirium after coronary artery bypass grafting: a prospective cohort study, J Cardiothorac Vasc Anesth
Villasis-Keever, López-Alarcón, Miranda-Novales, Efficacy and safety of vitamin D supplementation to prevent COVID-19 in frontline healthcare workers. A randomized clinical trial, Arch Med Res
Wiersinga, Rhodes, Cheng, Peacock, Prescott, Pathophysiology, transmission, diagnosis, and treatment of coronavirus disease 2019 (COVID-19): a review, JAMA
Wirth, Becker, Djukic, COVID-19 in old age-The geriatric perspective, Z fur Gerontol und Geriatr
Wrzosek, Łukaszkiewicz, Wrzosek, Vitamin D and the central nervous system, Pharmacol Rep: PR
Xu, Chen, Tang, Guidelines for the diagnosis and treatment of coronavirus disease 2019 (COVID-19) in China, Glob Health Med
Zhou, Chi, Lv, Wang, Obesity and diabetes as high-risk factors for severe coronavirus disease 2019 (Covid-19), Diabetes/Metab Res Rev
Zhou, Yang, Chi, Comorbidities and the risk of severe or fatal outcomes associated with coronavirus disease 2019: A systematic review and meta-analysis, Int J Infect Dis
DOI record:
{
"DOI": "10.1016/j.ctim.2022.102855",
"ISSN": [
"0965-2299"
],
"URL": "http://dx.doi.org/10.1016/j.ctim.2022.102855",
"alternative-id": [
"S0965229922000577"
],
"article-number": "102855",
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Vitamin D deficiency is associated with increased risk of delirium and mortality among critically Ill, elderly covid-19 patients"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "Complementary Therapies in Medicine"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.ctim.2022.102855"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2022 Published by Elsevier Ltd."
}
],
"author": [
{
"affiliation": [],
"family": "Gholi",
"given": "Zahra",
"sequence": "first"
},
{
"affiliation": [],
"family": "Yadegarynia",
"given": "Davood",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Eini-Zinab",
"given": "Hassan",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Vahdat Shariatpanahi",
"given": "Zahra",
"sequence": "additional"
}
],
"container-title": "Complementary Therapies in Medicine",
"container-title-short": "Complementary Therapies in Medicine",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"clinicalkey.fr",
"clinicalkey.jp",
"clinicalkey.es",
"clinicalkey.com.au",
"clinicalkey.com",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2022,
7,
19
]
],
"date-time": "2022-07-19T06:21:40Z",
"timestamp": 1658211700000
},
"deposited": {
"date-parts": [
[
2022,
7,
23
]
],
"date-time": "2022-07-23T03:03:29Z",
"timestamp": 1658545409000
},
"indexed": {
"date-parts": [
[
2022,
7,
23
]
],
"date-time": "2022-07-23T03:41:33Z",
"timestamp": 1658547693254
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2022,
11
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
11,
1
]
],
"date-time": "2022-11-01T00:00:00Z",
"timestamp": 1667260800000
}
},
{
"URL": "http://creativecommons.org/licenses/by-nc-nd/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
7,
12
]
],
"date-time": "2022-07-12T00:00:00Z",
"timestamp": 1657584000000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S0965229922000577?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S0965229922000577?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "102855",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2022,
11
]
]
},
"published-print": {
"date-parts": [
[
2022,
11
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1080/10408363.2021.1979462",
"article-title": "The COVID-19 pandemic: viral variants and vaccine efficacy",
"author": "Ciotti",
"doi-asserted-by": "crossref",
"first-page": "66",
"issue": "1",
"journal-title": "Crit Rev Clin Lab Sci",
"key": "10.1016/j.ctim.2022.102855_bib1",
"volume": "59",
"year": "2022"
},
{
"DOI": "10.1001/jama.2020.12839",
"article-title": "Pathophysiology, transmission, diagnosis, and treatment of coronavirus disease 2019 (COVID-19): a review",
"author": "Wiersinga",
"doi-asserted-by": "crossref",
"first-page": "782",
"issue": "8",
"journal-title": "JAMA",
"key": "10.1016/j.ctim.2022.102855_bib2",
"volume": "324",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.6775",
"article-title": "Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York city area",
"author": "Richardson",
"doi-asserted-by": "crossref",
"first-page": "2052",
"issue": "20",
"journal-title": "JAMA",
"key": "10.1016/j.ctim.2022.102855_bib3",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1016/j.ijid.2020.07.029",
"article-title": "Comorbidities and the risk of severe or fatal outcomes associated with coronavirus disease 2019: A systematic review and meta-analysis",
"author": "Zhou",
"doi-asserted-by": "crossref",
"first-page": "47",
"journal-title": "Int J Infect Dis",
"key": "10.1016/j.ctim.2022.102855_bib4",
"volume": "99",
"year": "2020"
},
{
"DOI": "10.1007/s00391-021-01864-0",
"article-title": "COVID-19 in old age-The geriatric perspective",
"author": "Wirth",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "Z fur Gerontol und Geriatr",
"key": "10.1016/j.ctim.2022.102855_bib5",
"volume": "54",
"year": "2021"
},
{
"DOI": "10.1016/j.nut.2020.111016",
"article-title": "Obesity, malnutrition, and trace element deficiency in the coronavirus disease (COVID-19) pandemic: an overview",
"author": "Fedele",
"doi-asserted-by": "crossref",
"journal-title": "Nutrition",
"key": "10.1016/j.ctim.2022.102855_bib6",
"volume": "81",
"year": "2021"
},
{
"DOI": "10.1093/tropej/fmaa084",
"article-title": "Severe malnutrition and anemia are associated with severe COVID in infants",
"author": "Kulkarni",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "J Trop Pediatr",
"key": "10.1016/j.ctim.2022.102855_bib7",
"volume": "67",
"year": "2021"
},
{
"DOI": "10.1080/00325481.2020.1786964",
"article-title": "COVID-19 and comorbidities: a systematic review and meta-analysis",
"author": "Gold",
"doi-asserted-by": "crossref",
"issue": "8",
"journal-title": "Postgrad Med",
"key": "10.1016/j.ctim.2022.102855_bib8",
"volume": "132",
"year": "2020"
},
{
"DOI": "10.1002/dmrr.3377",
"article-title": "Obesity and diabetes as high-risk factors for severe coronavirus disease 2019 (Covid-19)",
"author": "Zhou",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "Diabetes/Metab Res Rev",
"key": "10.1016/j.ctim.2022.102855_bib9",
"volume": "37",
"year": "2021"
},
{
"DOI": "10.1016/j.clnesp.2021.05.021",
"article-title": "Low vitamin D levels and increased neutrophil in patients admitted at ICU with COVID-19",
"author": "Pimentel",
"doi-asserted-by": "crossref",
"first-page": "466",
"journal-title": "Clin Nutr ESPEN",
"key": "10.1016/j.ctim.2022.102855_bib10",
"volume": "44",
"year": "2021"
},
{
"DOI": "10.1093/nutrit/nuaa081",
"article-title": "Supplementation with vitamin D in the COVID-19 pandemic?",
"author": "Hadizadeh",
"doi-asserted-by": "crossref",
"first-page": "200",
"issue": "2",
"journal-title": "Nutr Rev",
"key": "10.1016/j.ctim.2022.102855_bib11",
"volume": "79",
"year": "2021"
},
{
"article-title": "Association of vitamin D status and COVID-19-related hospitalization and mortality",
"author": "Seal",
"first-page": "1",
"journal-title": "J Gen Intern Med",
"key": "10.1016/j.ctim.2022.102855_bib12",
"year": "2022"
},
{
"DOI": "10.1007/s40618-021-01639-9",
"article-title": "Vitamin D supplementation and COVID-19 risk: a population-based, cohort study",
"author": "Oristrell",
"doi-asserted-by": "crossref",
"issue": "1",
"journal-title": "J Endocrinol Investig",
"key": "10.1016/j.ctim.2022.102855_bib13",
"volume": "45",
"year": "2022"
},
{
"DOI": "10.1016/j.arcmed.2022.04.003",
"article-title": "Efficacy and safety of vitamin D supplementation to prevent COVID-19 in frontline healthcare workers. A randomized clinical trial",
"author": "Villasis-Keever",
"doi-asserted-by": "crossref",
"journal-title": "Arch Med Res",
"key": "10.1016/j.ctim.2022.102855_bib14",
"year": "2022"
},
{
"article-title": "Vitamin D and immune regulation: antibacterial, antiviral, anti-inflammatory",
"author": "Bishop",
"first-page": "1",
"journal-title": "J Bone Miner Res",
"key": "10.1016/j.ctim.2022.102855_bib15",
"volume": "5",
"year": "2020"
},
{
"DOI": "10.3390/nu12113361",
"article-title": "Evidence regarding vitamin D and risk of COVID-19 and its severity",
"author": "Mercola",
"doi-asserted-by": "crossref",
"first-page": "11",
"journal-title": "Nutrients",
"key": "10.1016/j.ctim.2022.102855_bib16",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.18433/jpps32590",
"article-title": "Effects of vitamin D serum level on morbidity and mortality in patients with COVID-19: a systematic review and meta-analysis",
"author": "Hu",
"doi-asserted-by": "crossref",
"first-page": "84",
"journal-title": "J Pharm Pharm Sci",
"key": "10.1016/j.ctim.2022.102855_bib17",
"volume": "25",
"year": "2022"
},
{
"DOI": "10.1093/ajcn/nqac027",
"article-title": "Vitamin D, vitamin D – binding protein, free vitamin D and COVID-19 mortality in hospitalized patients",
"author": "Subramanian",
"doi-asserted-by": "crossref",
"issue": "5",
"journal-title": "Am J Clin Nutr",
"key": "10.1016/j.ctim.2022.102855_bib18",
"volume": "115",
"year": "2022"
},
{
"DOI": "10.1080/10408398.2020.1841090",
"article-title": "Vitamin D deficiency aggravates COVID-19: systematic review and meta-analysis",
"author": "Pereira",
"doi-asserted-by": "crossref",
"issue": "5",
"journal-title": "Crit Rev Food Sci Nutr",
"key": "10.1016/j.ctim.2022.102855_bib19",
"volume": "62",
"year": "2022"
},
{
"article-title": "Vitamin D supplementation and Covid‐19 outcomes: a systematic review, meta‐analysis and meta‐regression",
"author": "Hariyanto",
"issue": "2",
"journal-title": "Rev Med Virol",
"key": "10.1016/j.ctim.2022.102855_bib20",
"volume": "32",
"year": "2022"
},
{
"DOI": "10.1093/cdn/nzab053_073",
"article-title": "Genetically predicted serum vitamin D and COVID-19: a Mendelian randomization study",
"author": "Patchen",
"doi-asserted-by": "crossref",
"first-page": "1080",
"issue": "2",
"journal-title": "Curr Dev Nutr",
"key": "10.1016/j.ctim.2022.102855_bib21",
"volume": "5",
"year": "2021"
},
{
"DOI": "10.1136/bmjnph-2020-000151",
"article-title": "No evidence that vitamin D is able to prevent or affect the severity of COVID-19 in individuals with European ancestry: a Mendelian randomisation study of open data",
"author": "Amin",
"doi-asserted-by": "crossref",
"first-page": "42",
"issue": "1",
"journal-title": "BMJ Nutr, Prev Health",
"key": "10.1016/j.ctim.2022.102855_bib22",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.7754/Clin.Lab.2021.210543",
"article-title": "25 (OH) vitamin D levels of patients with COVID-19 are not associated with the length of hospital stay",
"author": "Bulca-Acar",
"doi-asserted-by": "crossref",
"first-page": "3",
"journal-title": "Clin Lab",
"key": "10.1016/j.ctim.2022.102855_bib23",
"volume": "68",
"year": "2022"
},
{
"DOI": "10.1186/s12937-021-00744-y",
"article-title": "Low vitamin D levels do not aggravate COVID-19 risk or death, and vitamin D supplementation does not improve outcomes in hospitalized patients with COVID-19: a meta-analysis and GRADE assessment of cohort studies and RCTs",
"author": "Chen",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "Nutr J",
"key": "10.1016/j.ctim.2022.102855_bib24",
"volume": "20",
"year": "2021"
},
{
"DOI": "10.1016/j.mayocp.2021.01.001",
"article-title": "Vitamin D status is associated with in-hospital mortality and mechanical ventilation: a cohort of COVID-19 hospitalized patients",
"author": "Angelidi",
"doi-asserted-by": "crossref",
"issue": "4",
"journal-title": "Mayo Clin Proc",
"key": "10.1016/j.ctim.2022.102855_bib25",
"volume": "96",
"year": "2021"
},
{
"DOI": "10.1152/ajpendo.00517.2020",
"article-title": "Exploring the link between vitamin D and clinical outcomes in COVID-19",
"author": "Lohia",
"doi-asserted-by": "crossref",
"first-page": "E520",
"issue": "3",
"journal-title": "Am J Physiol Endocrinol Metab",
"key": "10.1016/j.ctim.2022.102855_bib26",
"volume": "320",
"year": "2021"
},
{
"DOI": "10.3390/nu12092757",
"article-title": "Vitamin D deficiency and outcome of COVID-19 patients",
"author": "Radujkovic",
"doi-asserted-by": "crossref",
"first-page": "9",
"journal-title": "Nutrients",
"key": "10.1016/j.ctim.2022.102855_bib27",
"volume": "12",
"year": "2020"
},
{
"article-title": "Innovative ICU solutions to prevent and reduce delirium and post-intensive care unit syndrome",
"author": "Luetz",
"issue": "5",
"journal-title": "Semin Respir Crit Care Med",
"key": "10.1016/j.ctim.2022.102855_bib28",
"volume": "40",
"year": "2019"
},
{
"DOI": "10.35772/ghm.2020.01015",
"article-title": "Guidelines for the diagnosis and treatment of coronavirus disease 2019 (COVID-19) in China",
"author": "Xu",
"doi-asserted-by": "crossref",
"first-page": "66",
"issue": "2",
"journal-title": "Glob Health Med",
"key": "10.1016/j.ctim.2022.102855_bib29",
"volume": "2",
"year": "2020"
},
{
"DOI": "10.1016/j.ajem.2020.05.073",
"article-title": "Lactate dehydrogenase levels predict coronavirus disease 2019 (COVID-19) severity and mortality: a pooled analysis",
"author": "Henry",
"doi-asserted-by": "crossref",
"issue": "9",
"journal-title": "Am J Emerg Med",
"key": "10.1016/j.ctim.2022.102855_bib30",
"volume": "38",
"year": "2020"
},
{
"DOI": "10.1186/cc11407",
"article-title": "The confusion assessment method for the intensive care unit (CAM-ICU) and intensive care delirium screening checklist (ICDSC) for the diagnosis of delirium: a systematic review and meta-analysis of clinical studies",
"author": "Gusmao-Flores",
"doi-asserted-by": "crossref",
"first-page": "R115",
"issue": "4",
"journal-title": "Crit Care",
"key": "10.1016/j.ctim.2022.102855_bib31",
"volume": "16",
"year": "2012"
},
{
"DOI": "10.1186/s12933-020-01184-4",
"article-title": "Diabetes and Covid-19 among hospitalized patients in Saudi Arabia: a single-centre retrospective study",
"author": "Alguwaihes",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "Cardiovasc Diabetol",
"key": "10.1016/j.ctim.2022.102855_bib32",
"volume": "19",
"year": "2020"
},
{
"DOI": "10.1007/s40520-021-01831-0",
"article-title": "Severe vitamin D deficiency is not related to SARS-CoV-2 infection but may increase mortality risk in hospitalized adults: a retrospective case–control study in an Arab Gulf country",
"author": "Alguwaihes",
"doi-asserted-by": "crossref",
"issue": "5",
"journal-title": "Aging Clin Exp Res",
"key": "10.1016/j.ctim.2022.102855_bib33",
"volume": "33",
"year": "2021"
},
{
"DOI": "10.1186/s12967-021-02838-x",
"article-title": "Vitamin D status of Arab Gulf residents screened for SARS-CoV-2 and its association with COVID-19 infection: a multi-centre case–control study",
"author": "Al-Daghri",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "J Transl Med",
"key": "10.1016/j.ctim.2022.102855_bib34",
"volume": "19",
"year": "2021"
},
{
"DOI": "10.3390/nu13051714",
"article-title": "COVID-19 disease severity and death in relation to vitamin D status among SARS-CoV-2-positive UAE residents",
"author": "AlSafar",
"doi-asserted-by": "crossref",
"first-page": "1714",
"issue": "5",
"journal-title": "Nutrients",
"key": "10.1016/j.ctim.2022.102855_bib35",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.18632/aging.103579",
"article-title": "Epidemiological, comorbidity factors with severity and prognosis of COVID-19: a systematic review and meta-analysis",
"author": "Fang",
"doi-asserted-by": "crossref",
"issue": "13",
"journal-title": "Aging",
"key": "10.1016/j.ctim.2022.102855_bib36",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3390/nu12123679",
"article-title": "Malnutrition: percentage and association with prognosis in patients hospitalized for coronavirus disease 2019",
"author": "Allard",
"doi-asserted-by": "crossref",
"first-page": "12",
"journal-title": "Nutrients",
"key": "10.1016/j.ctim.2022.102855_bib37",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1093/advances/nmaa125",
"article-title": "Coronavirus disease 2019 (COVID-19) and nutritional status: the missing link?",
"author": "Silverio",
"doi-asserted-by": "crossref",
"first-page": "682",
"issue": "3",
"journal-title": "Adv Nutr",
"key": "10.1016/j.ctim.2022.102855_bib38",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.3389/fnut.2022.813485",
"article-title": "Serum vitamin D levels are associated with increased COVID-19 severity and mortality independent of whole-body and visceral adiposity",
"author": "Vanegas-Cedillo",
"doi-asserted-by": "crossref",
"journal-title": "Front Nutr",
"key": "10.1016/j.ctim.2022.102855_bib39",
"volume": "9",
"year": "2022"
},
{
"DOI": "10.1016/j.clnesp.2021.11.025",
"article-title": "COVID-19 mortality is associated with low vitamin D levels in patients with risk factors and/or advanced age",
"author": "Jenei",
"doi-asserted-by": "crossref",
"first-page": "410",
"journal-title": "Clin Nutr ESPEN",
"key": "10.1016/j.ctim.2022.102855_bib40",
"volume": "47",
"year": "2022"
},
{
"DOI": "10.1016/j.clnu.2021.03.001",
"article-title": "Vitamin D deficiency in critically ill COVID-19 ARDS patients",
"author": "Notz",
"doi-asserted-by": "crossref",
"journal-title": "Clin Nutr",
"key": "10.1016/j.ctim.2022.102855_bib41",
"year": "2021"
},
{
"DOI": "10.1016/j.coph.2010.04.001",
"article-title": "Vitamin D: modulator of the immune system",
"author": "Baeke",
"doi-asserted-by": "crossref",
"first-page": "482",
"issue": "4",
"journal-title": "Curr Opin Pharmacol",
"key": "10.1016/j.ctim.2022.102855_bib42",
"volume": "10",
"year": "2010"
},
{
"DOI": "10.4049/jimmunol.0803217",
"article-title": "1,25-Dihydroxyvitamin D3 and IL-2 combine to inhibit T cell production of inflammatory cytokines and promote development of regulatory T cells expressing CTLA-4 and FoxP3",
"author": "Jeffery",
"doi-asserted-by": "crossref",
"first-page": "5458",
"issue": "9",
"journal-title": "J Immunol",
"key": "10.1016/j.ctim.2022.102855_bib43",
"volume": "183",
"year": "2009"
},
{
"DOI": "10.1111/1753-0407.13085",
"article-title": "Factors leading to high morbidity and mortality of COVID-19 in patients with type 2 diabetes",
"author": "Rajpal",
"doi-asserted-by": "crossref",
"first-page": "895",
"issue": "12",
"journal-title": "J Diabetes",
"key": "10.1016/j.ctim.2022.102855_bib44",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1016/j.cmet.2020.09.007",
"article-title": "Shining light on the COVID-19 pandemic: a vitamin D receptor checkpoint in defense of unregulated wound healing",
"author": "Evans",
"doi-asserted-by": "crossref",
"first-page": "704",
"issue": "5",
"journal-title": "Cell Metab",
"key": "10.1016/j.ctim.2022.102855_bib45",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.1530/EJE-20-0665",
"article-title": "Mechanisms in endocrinology: vitamin D and COVID-19",
"author": "Bilezikian",
"doi-asserted-by": "crossref",
"first-page": "R133",
"issue": "5",
"journal-title": "Eur J Endocrinol",
"key": "10.1016/j.ctim.2022.102855_bib46",
"volume": "183",
"year": "2020"
},
{
"DOI": "10.1016/j.lfs.2022.120464",
"article-title": "COVID-19 and neurological sequelae: vitamin D as a possible neuroprotective and/or neuroreparative agent",
"author": "Menéndez",
"doi-asserted-by": "crossref",
"journal-title": "Life Sci",
"key": "10.1016/j.ctim.2022.102855_bib47",
"year": "2022"
},
{
"DOI": "10.1093/gerona/glab184",
"article-title": "APOE e4 genotypes increase risk of delirium during COVID-19-related hospitalizations: evidence from a large UK Cohort",
"author": "Kuo",
"doi-asserted-by": "crossref",
"issue": "4",
"journal-title": "J Gerontol: Ser A",
"key": "10.1016/j.ctim.2022.102855_bib48",
"volume": "77",
"year": "2022"
},
{
"DOI": "10.1186/s12883-019-1500-6",
"article-title": "Vitamin D deficiency as a risk factor for dementia and Alzheimer’s disease: an updated meta-analysis",
"author": "Chai",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "BMC Neurol",
"key": "10.1016/j.ctim.2022.102855_bib49",
"volume": "19",
"year": "2019"
},
{
"article-title": "Preoperative vitamin D deficiency is associated with postoperative delirium in critically Ill patients",
"author": "Qiu",
"journal-title": "J Intensive care Med",
"key": "10.1016/j.ctim.2022.102855_bib50",
"year": "2021"
},
{
"DOI": "10.1111/jgs.16853",
"article-title": "Low vitamin D levels and risk of incident delirium in 351,000 older UK biobank participants",
"author": "Pilling",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "J Am Geriatr Soc",
"key": "10.1016/j.ctim.2022.102855_bib51",
"volume": "69",
"year": "2021"
},
{
"DOI": "10.1053/j.jvca.2020.02.008",
"article-title": "Vitamin D and postoperative delirium after coronary artery bypass grafting: a prospective cohort study",
"author": "Velayati",
"doi-asserted-by": "crossref",
"first-page": "1774",
"issue": "7",
"journal-title": "J Cardiothorac Vasc Anesth",
"key": "10.1016/j.ctim.2022.102855_bib52",
"volume": "34",
"year": "2020"
},
{
"DOI": "10.1016/S1734-1140(13)71003-X",
"article-title": "Vitamin D and the central nervous system",
"author": "Wrzosek",
"doi-asserted-by": "crossref",
"first-page": "271",
"issue": "2",
"journal-title": "Pharmacol Rep: PR",
"key": "10.1016/j.ctim.2022.102855_bib53",
"volume": "65",
"year": "2013"
},
{
"DOI": "10.1023/B:BIRY.0000040196.65686.2f",
"article-title": "Mechanisms of neuroprotective action of vitamin D(3)",
"author": "Kalueff",
"doi-asserted-by": "crossref",
"first-page": "738",
"issue": "7",
"journal-title": "Biochem Biokhimiia",
"key": "10.1016/j.ctim.2022.102855_bib54",
"volume": "69",
"year": "2004"
},
{
"DOI": "10.1038/ejcn.2016.177",
"article-title": "Aging, low-grade systemic inflammation and vitamin D: a mini-review",
"author": "Gonçalves de Carvalho",
"doi-asserted-by": "crossref",
"issue": "4",
"journal-title": "Eur J Clin Nutr",
"key": "10.1016/j.ctim.2022.102855_bib55",
"volume": "71",
"year": "2017"
},
{
"DOI": "10.1093/ajcn/nqab151",
"article-title": "Influence of vitamin D status on hospital length of stay and prognosis in hospitalized patients with moderate to severe COVID-19: a multicenter prospective cohort study",
"author": "Reis",
"doi-asserted-by": "crossref",
"first-page": "598",
"issue": "2",
"journal-title": "Am J Clin Nutr",
"key": "10.1016/j.ctim.2022.102855_bib56",
"volume": "114",
"year": "2021"
},
{
"DOI": "10.1136/archdischild-2014-307149",
"article-title": "Too many digits: the presentation of numerical data",
"author": "Cole",
"doi-asserted-by": "crossref",
"first-page": "608",
"issue": "7",
"journal-title": "Arch Dis Child",
"key": "10.1016/j.ctim.2022.102855_bib57",
"volume": "100",
"year": "2015"
}
],
"reference-count": 57,
"references-count": 57,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S0965229922000577"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Advanced and Specialized Nursing",
"Complementary and alternative medicine",
"Complementary and Manual Therapy"
],
"subtitle": [],
"title": "Vitamin D deficiency is associated with increased risk of delirium and mortality among critically Ill, elderly covid-19 patients",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "70"
}
