Lactoferrin reduces the risk of respiratory tract infections: A meta-analysis of randomized controlled trials
et al., Clinical Nutrition ESPEN, doi:10.1016/j.clnesp.2021.08.019, Sep 2021
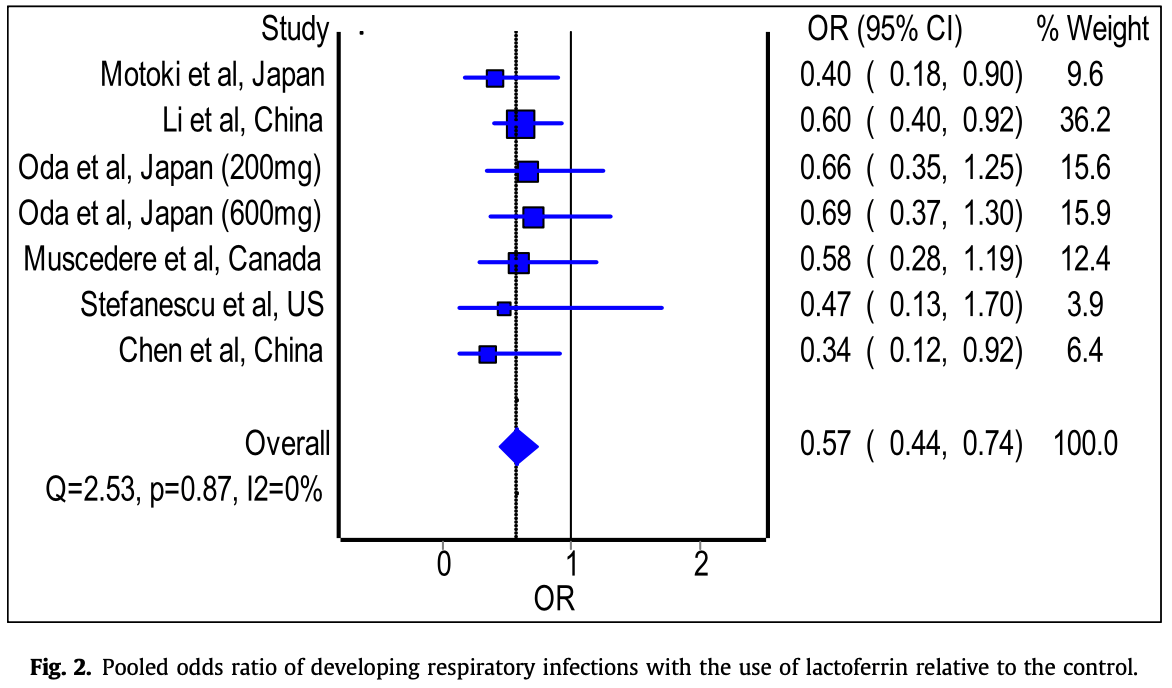
Meta analysis of 6 RCTs, showing significantly lower risk of respiratory tract infections with lactoferrin.
Currently there are 8 lactoferrin studies and meta-analysis shows:
| Outcome | Improvement |
|---|---|
| Mortality | 17% lower [-161‑73%] |
| Ventilation | 45% higher [-35‑220%] |
| Hospitalization | 61% lower [-164‑94%] |
| Cases | 36% more [-42‑218%] |
Ali et al., 3 Sep 2021, peer-reviewed, 4 authors.
Lactoferrin reduces the risk of respiratory tract infections: A meta-analysis of randomized controlled trials
Clinical Nutrition ESPEN, doi:10.1016/j.clnesp.2021.08.019
Background: Lactoferrin (Lf) is one of the key immunomodulatory substances found naturally in various body fluids, such as saliva, tears, and breast milk, and forms a vital part of the innate defense against invading pathogens. Various studies have demonstrated antibacterial, antifungal, and antiviral properties of Lf and its protective role against respiratory tract infections (RTIs). The present meta-analysis aims to elucidate the association of Lf administration in reducing the risk of RTIs by systematically reviewing the data from randomized controlled trials (RCTs). Methods: We systematically searched PubMed, Cochrane Library, Medline & CINAHL, Turning Research into Practice (TRIP), ProQuest Theses & Dissertations Databases, and China National Knowledge Infrastructure (CNKI) from inception till March 15, 2021. The primary outcome measure was a reduction in respiratory illness; decrease in frequency, symptoms, and duration. Random-effects model was used to estimate the odds ratio (OR) and 95% confidence interval (CI). We used Cochrane's RoB-2 to appraise the risk of bias of included RCTs. Results: A total of nine RCTs were eligible for this review, of which six were included in the metaanalysis. Overall, two studies demonstrated a high risk of bias. The meta-analysis revealed a significantly reduced odds of developing respiratory infections with the use of Lf relative to the control (pooled odds ratio ¼ 0.57; 95% confidence interval 0.44 to 0.74, n ¼ 1,194), with sufficient evidence against the hypothesis of 'no significant difference' at the current sample size. Conclusions: The administration of Lf shows promising efficacy in reducing the risk of RTIs. Current evidence also favours Lf fortification of infant formula. Lf may also have a beneficial role in managing symptoms and recovery of patients suffering from RTIs and may have potential for use as an adjunct in COVID-19, however this warrants further evidence from a large well-designed RCT.
Authors contributions HAM conceptualized and designed the study, SSH, CSK ASA, HAM extracted and analysed the data and drafted the manuscript. All authors read and approved the final version of the manuscript.
Declaration of competing interest HAM is on a scientific advisory board for a lactoferrin supplement product but does not have any financial or other affiliation with the company and has neither received any funding or financial reimbursements. HAM is committed to promote the science behind Lf and its immunomodulatory role in the prevention and management of infections.
References
Actor, Hwang, Kruzel, Lactoferrin as a natural immune modulator, Curr Pharmaceut Des
Ammendolia, Agamennone, Pietrantoni, Lannutti, Siciliano et al., Bovine lactoferrin-derived peptides as novel broad-spectrum inhibitors of influenza virus, Pathog Glob Health
Chang, Ng, Sun, Lactoferrin as potential preventative and adjunct treatment for COVID-19, Int J Antimicrob Agents
Chen, Chai, Li, Zhang, Xie et al., Effect of bovine lactoferrin from iron-fortified formulas on diarrhea and respiratory tract infections of weaned infants in a randomized controlled trial, Nutrition
Chen, Jiang, Effect of lactoferrin on anemia and recurrent respiratory tract infection in preterm infants born between 34 to 36 weeks, Chin J Woman Child Health Res
Christianson, Belting, Heparan sulfate proteoglycan as a cell-surface endocytosis receptor, Matrix Biol
Drago-Serrano, Campos-Rodríguez, Carrero, De, Garza, Lactoferrin: balancing ups and downs of inflammation due to microbial infections, Int J Mol Sci
Fernandes, Weeks, Carter, Lactoferrin is broadly active against yeasts and highly synergistic with amphotericin B, Antimicrob Agents Chemother
García-Montoya, Cend On, Ts, Evalo-Gallegos, Rasc On-Cruz, Lactoferrin a multiple bioactive protein: an overview, Biochim Biophys Acta
Hu, Meng, Zhang, Xiang, Wang, The in vitro antiviral activity of lactoferrin against common human coronaviruses and SARS-CoV-2 is mediated by targeting the heparan sulfate co-receptor, Emerg Microb Infect
Hwang, Kruzel, Actor, CHO expressed recombinant human lactoferrin as an adjuvant for BCG, Int J Immunopathol Pharmacol
Iglesias-Figueroa, Espinoza, Ea, Ts, Qjidj, Lactoferrin as a nutraceutical protein from milk, an overview
Jr, Cummings, Guo, Trivedi, Readmond et al., A double-blind, placebo-controlled, pilot study of bovine lactoferrin supplementation in bottle-fed infants, J Pediatr Gastroenterol Nutr
Kell, Heyden, Pretorius, The biology of lactoferrin, an iron-binding protein that can help defend against viruses and bacteria, Front Immunol
Kruzel, Zimecki, Actor, Lactoferrin in a context of inflammationinduced pathology, Front Immunol
Latorre, Puddu, Valenti, Gessani, Reciprocal interactions between lactoferrin and bacterial endotoxins and their role in the regulation of the immune response, Toxins
Legrand, Overview of lactoferrin as a natural immune modulator, J Pediatr
Li, Wu, Berseth, Harris, Richards et al., Improved neurodevelopmental outcomes associated with bovine milk fat globule membrane and lactoferrin in infant formula: a randomized, controlled trial, J Pediatr
Liberati, Altman, Tetzlaff, Mulrow, Gøtzsche et al., The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration, BMJ
Lu, Francis, Guevara, Moore, Chambers et al., Antibacterial and anti-biofilm activity of the human breast milk glycoprotein lactoferrin against group B Streptococcus, Chembiochem
Machnicki, Zimecki, Zagulski, Lactoferrin regulates the release of tumour necrosis factor alpha and interleukin 6 in vivo, Int J Exp Pathol
Milewska, Nowak, Owczarek, Szczepanski, Zarebski et al., Entry of human coronavirus NL63 into the cell, J Virol
Motoki, Mizuki, Tsukahara, Miyakawa, Kubo et al., Effects of lactoferrin-fortified formula on acute gastrointestinal symptoms in children aged 12e32 Months: a randomized, double-blind, Placebo-Contr Trial
Muscedere, Maslove, Boyd, 'callaghan, Sibley et al., Prevention of nosocomial infections in critically ill patients with lactoferrin: a randomized, double-blind, placebo-controlled study, Crit Care Med
Naghavi, Abajobir, Abbafati, Abbas, Abd-Allah et al., Global, regional, and national age-sex specific mortality for 264 causes of death, Lancet
Najmafshar, Rostami, Varshosaz, Norouzian, Shariat, Enhanced antitumor activity of bovine lactoferrin through immobilization onto functionalized nano graphene oxide: an in vitro/in vivo study, Drug Deliv
Oda, Wakabayashi, Tanaka, Yamauchi, Sugita et al., Effects of lactoferrin on infectious diseases in Japanese summer: a randomized, double-blinded, placebo-controlled trial, J Microbiol Immunol Infect
Pietrantoni, Ammendolia, Superti, Bovine lactoferrin: involvement of metal saturation and carbohydrates in the inhibition of influenza virus infection, Biochem Cell Biol
Rasc On-Cruz, Espinoza, Ea, Ts, Nakamura-Bencomo et al., Lactoferrin: a glycoprotein involved in immunomodulation, anticancer, and antimicrobial processes, Molecules
Shin, Wakabayashi, Yamauchi, Teraguchi, Tamura et al., Effects of orally administered bovine lactoferrin and lactoperoxidase on influenza virus infection in mice, J Med Microbiol
Siqueiros-Cend On, Evalo-Gallegos, Iglesias-Figueroa, García-Montoya, Salazar-Martínez et al., Immunomodulatory effects of lactoferrin, Acta Pharmacol Sin
Stefanescu, Etu, Slaughter, Shea, Shetty, A pilot study of Biotene OralBalance® gel for oral care in mechanically ventilated preterm neonates, Contemp Clin Trials
Vitetta, Coulson, Beck, Gramotnev, Du et al., The clinical efficacy of a bovine lactoferrin/whey protein Ig-rich fraction (Lf/IgF) for the common cold: a double blind randomized study, Compl Ther Med
Wakabayashi, Oda, Yamauchi, Abe, Lactoferrin for prevention of common viral infections, J Infect Chemother
Xu, Olson, Cole, Van Wijk, Brinkmann et al., Heparan sulfate modulates neutrophil and endothelial function in antibacterial innate immunity, Infect Immun
Zimecki, Actor, Kruzel, The potential for Lactoferrin to reduce SARS-CoV-2 induced cytokine storm, Int Immunopharm
DOI record:
{
"DOI": "10.1016/j.clnesp.2021.08.019",
"ISSN": [
"2405-4577"
],
"URL": "http://dx.doi.org/10.1016/j.clnesp.2021.08.019",
"alternative-id": [
"S2405457721003077"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Lactoferrin reduces the risk of respiratory tract infections: A meta-analysis of randomized controlled trials"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "Clinical Nutrition ESPEN"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.clnesp.2021.08.019"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2021 European Society for Clinical Nutrition and Metabolism. Published by Elsevier Ltd. All rights reserved."
}
],
"author": [
{
"affiliation": [],
"family": "Ali",
"given": "Akbar Shoukat",
"sequence": "first"
},
{
"affiliation": [],
"family": "Hasan",
"given": "Syed Shahzad",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kow",
"given": "Chia Siang",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Merchant",
"given": "Hamid A.",
"sequence": "additional"
}
],
"container-title": "Clinical Nutrition ESPEN",
"container-title-short": "Clinical Nutrition ESPEN",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"clinicalkey.jp",
"clinicalkey.com",
"clinicalnutritionespen.com",
"clinicalkey.es",
"clinicalkey.com.au",
"clinicalkey.fr",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2021,
9,
3
]
],
"date-time": "2021-09-03T08:09:37Z",
"timestamp": 1630656577000
},
"deposited": {
"date-parts": [
[
2021,
11,
6
]
],
"date-time": "2021-11-06T16:54:39Z",
"timestamp": 1636217679000
},
"indexed": {
"date-parts": [
[
2022,
8,
9
]
],
"date-time": "2022-08-09T04:16:09Z",
"timestamp": 1660018569686
},
"is-referenced-by-count": 6,
"issued": {
"date-parts": [
[
2021,
10
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
10,
1
]
],
"date-time": "2021-10-01T00:00:00Z",
"timestamp": 1633046400000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S2405457721003077?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S2405457721003077?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "26-32",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2021,
10
]
]
},
"published-print": {
"date-parts": [
[
2021,
10
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.3390/ijms18030501",
"article-title": "Lactoferrin: balancing ups and downs of inflammation due to microbial infections",
"author": "Drago-Serrano",
"doi-asserted-by": "crossref",
"first-page": "501",
"journal-title": "Int J Mol Sci",
"key": "10.1016/j.clnesp.2021.08.019_bib1",
"volume": "18",
"year": "2017"
},
{
"DOI": "10.1016/S0140-6736(17)32152-9",
"article-title": "Global, regional, and national age-sex specific mortality for 264 causes of death, 1980–2016: a systematic analysis for the Global Burden of Disease Study 2016",
"author": "Naghavi",
"doi-asserted-by": "crossref",
"first-page": "1151",
"journal-title": "Lancet",
"key": "10.1016/j.clnesp.2021.08.019_bib2",
"volume": "390",
"year": "2017"
},
{
"DOI": "10.3390/molecules26010205",
"article-title": "Lactoferrin: a glycoprotein involved in immunomodulation, anticancer, and antimicrobial processes",
"author": "Rascón-Cruz",
"doi-asserted-by": "crossref",
"first-page": "205",
"journal-title": "Molecules",
"key": "10.1016/j.clnesp.2021.08.019_bib3",
"volume": "26",
"year": "2021"
},
{
"DOI": "10.1016/j.intimp.2021.107571",
"article-title": "The potential for Lactoferrin to reduce SARS-CoV-2 induced cytokine storm",
"author": "Zimecki",
"doi-asserted-by": "crossref",
"first-page": "107571",
"journal-title": "Int Immunopharm",
"key": "10.1016/j.clnesp.2021.08.019_bib4",
"volume": "95",
"year": "2021"
},
{
"DOI": "10.1016/j.bbagen.2011.06.018",
"article-title": "Lactoferrin a multiple bioactive protein: an overview",
"author": "García-Montoya",
"doi-asserted-by": "crossref",
"first-page": "226",
"journal-title": "Biochim Biophys Acta",
"key": "10.1016/j.clnesp.2021.08.019_bib5",
"volume": "1820",
"year": "2012"
},
{
"article-title": "Antibacterial and anti-biofilm activity of the human breast milk glycoprotein lactoferrin against group B Streptococcus",
"author": "Lu",
"journal-title": "Chembiochem",
"key": "10.1016/j.clnesp.2021.08.019_bib6",
"volume": "22",
"year": "2021"
},
{
"DOI": "10.1080/22221751.2021.1888660",
"article-title": "The in vitro antiviral activity of lactoferrin against common human coronaviruses and SARS-CoV-2 is mediated by targeting the heparan sulfate co-receptor",
"author": "Hu",
"doi-asserted-by": "crossref",
"first-page": "317",
"journal-title": "Emerg Microb Infect",
"key": "10.1016/j.clnesp.2021.08.019_bib7",
"volume": "10",
"year": "2021"
},
{
"article-title": "Lactoferrin is broadly active against yeasts and highly synergistic with amphotericin B",
"author": "Fernandes",
"journal-title": "Antimicrob Agents Chemother",
"key": "10.1016/j.clnesp.2021.08.019_bib8",
"volume": "64",
"year": "2020"
},
{
"DOI": "10.1080/10717544.2020.1809558",
"article-title": "Enhanced antitumor activity of bovine lactoferrin through immobilization onto functionalized nano graphene oxide: an in vitro/in vivo study",
"author": "Najmafshar",
"doi-asserted-by": "crossref",
"first-page": "1236",
"journal-title": "Drug Deliv",
"key": "10.1016/j.clnesp.2021.08.019_bib9",
"volume": "27",
"year": "2020"
},
{
"article-title": "Lactoferrin as a nutraceutical protein from milk",
"author": "Iglesias-Figueroa",
"first-page": "37",
"journal-title": "an overview",
"key": "10.1016/j.clnesp.2021.08.019_bib10",
"volume": "89",
"year": "2019"
},
{
"article-title": "Effects of lactoferrin on infectious diseases in Japanese summer: a randomized, double-blinded, placebo-controlled trial",
"author": "Oda",
"journal-title": "J Microbiol Immunol Infect",
"key": "10.1016/j.clnesp.2021.08.019_bib11",
"volume": "54",
"year": "2020"
},
{
"article-title": "Effects of lactoferrin-fortified formula on acute gastrointestinal symptoms in children aged 12–32 Months: a randomized, double-blind",
"author": "Motoki",
"journal-title": "Placebo-Contr Trial",
"key": "10.1016/j.clnesp.2021.08.019_bib12",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/j.jpeds.2019.08.030",
"article-title": "Improved neurodevelopmental outcomes associated with bovine milk fat globule membrane and lactoferrin in infant formula: a randomized, controlled trial",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "24",
"journal-title": "J Pediatr",
"key": "10.1016/j.clnesp.2021.08.019_bib13",
"volume": "215",
"year": "2019"
},
{
"DOI": "10.1097/CCM.0000000000003294",
"article-title": "Prevention of nosocomial infections in critically ill patients with lactoferrin: a randomized, double-blind, placebo-controlled study",
"author": "Muscedere",
"doi-asserted-by": "crossref",
"first-page": "1450",
"journal-title": "Crit Care Med",
"key": "10.1016/j.clnesp.2021.08.019_bib14",
"volume": "46",
"year": "2018"
},
{
"DOI": "10.1016/j.cct.2013.03.010",
"article-title": "A pilot study of Biotene OralBalance® gel for oral care in mechanically ventilated preterm neonates",
"author": "Stefanescu",
"doi-asserted-by": "crossref",
"first-page": "33",
"journal-title": "Contemp Clin Trials",
"key": "10.1016/j.clnesp.2021.08.019_bib15",
"volume": "35",
"year": "2013"
},
{
"DOI": "10.1136/bmj.b2700",
"article-title": "The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration",
"author": "Liberati",
"doi-asserted-by": "crossref",
"first-page": "b2700",
"journal-title": "BMJ",
"key": "10.1016/j.clnesp.2021.08.019_bib16",
"volume": "339",
"year": "2009"
},
{
"DOI": "10.1016/j.nut.2015.08.010",
"article-title": "Effect of bovine lactoferrin from iron-fortified formulas on diarrhea and respiratory tract infections of weaned infants in a randomized controlled trial",
"author": "Chen",
"doi-asserted-by": "crossref",
"first-page": "222",
"journal-title": "Nutrition",
"key": "10.1016/j.clnesp.2021.08.019_bib17",
"volume": "32",
"year": "2016"
},
{
"DOI": "10.1016/j.ctim.2012.12.006",
"article-title": "The clinical efficacy of a bovine lactoferrin/whey protein Ig-rich fraction (Lf/IgF) for the common cold: a double blind randomized study",
"author": "Vitetta",
"doi-asserted-by": "crossref",
"first-page": "164",
"journal-title": "Compl Ther Med",
"key": "10.1016/j.clnesp.2021.08.019_bib18",
"volume": "21",
"year": "2013"
},
{
"DOI": "10.1097/01.mpg.0000243435.54958.68",
"article-title": "A double-blind, placebo-controlled, pilot study of bovine lactoferrin supplementation in bottle-fed infants",
"author": "King",
"doi-asserted-by": "crossref",
"first-page": "245",
"journal-title": "J Pediatr Gastroenterol Nutr",
"key": "10.1016/j.clnesp.2021.08.019_bib19",
"volume": "44",
"year": "2007"
},
{
"article-title": "Effect of lactoferrin on anemia and recurrent respiratory tract infection in preterm infants born between 34 to 36 weeks",
"author": "Chen",
"first-page": "424",
"journal-title": "Chin J Woman Child Health Res",
"key": "10.1016/j.clnesp.2021.08.019_bib20",
"volume": "27",
"year": "2016"
},
{
"DOI": "10.3389/fimmu.2020.01221",
"article-title": "The biology of lactoferrin, an iron-binding protein that can help defend against viruses and bacteria",
"author": "Kell",
"doi-asserted-by": "crossref",
"journal-title": "Front Immunol",
"key": "10.1016/j.clnesp.2021.08.019_bib21",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.3390/toxins2010054",
"article-title": "Reciprocal interactions between lactoferrin and bacterial endotoxins and their role in the regulation of the immune response",
"author": "Latorre",
"doi-asserted-by": "crossref",
"first-page": "54",
"journal-title": "Toxins",
"key": "10.1016/j.clnesp.2021.08.019_bib22",
"volume": "2",
"year": "2010"
},
{
"DOI": "10.1128/IAI.00545-15",
"article-title": "Heparan sulfate modulates neutrophil and endothelial function in antibacterial innate immunity",
"author": "Xu",
"doi-asserted-by": "crossref",
"first-page": "3648",
"journal-title": "Infect Immun",
"key": "10.1016/j.clnesp.2021.08.019_bib23",
"volume": "83",
"year": "2015"
},
{
"DOI": "10.1016/j.matbio.2013.10.004",
"article-title": "Heparan sulfate proteoglycan as a cell-surface endocytosis receptor",
"author": "Christianson",
"doi-asserted-by": "crossref",
"first-page": "51",
"journal-title": "Matrix Biol",
"key": "10.1016/j.clnesp.2021.08.019_bib24",
"volume": "35",
"year": "2014"
},
{
"DOI": "10.1128/JVI.01933-17",
"article-title": "Entry of human coronavirus NL63 into the cell",
"author": "Milewska",
"doi-asserted-by": "crossref",
"journal-title": "J Virol",
"key": "10.1016/j.clnesp.2021.08.019_bib25",
"volume": "92",
"year": "2018"
},
{
"DOI": "10.1016/j.ijantimicag.2020.106118",
"article-title": "Lactoferrin as potential preventative and adjunct treatment for COVID-19",
"author": "Chang",
"doi-asserted-by": "crossref",
"first-page": "106118",
"journal-title": "Int J Antimicrob Agents",
"key": "10.1016/j.clnesp.2021.08.019_bib26",
"volume": "56",
"year": "2020"
},
{
"DOI": "10.2174/138161209788453202",
"article-title": "Lactoferrin as a natural immune modulator",
"author": "Actor",
"doi-asserted-by": "crossref",
"first-page": "1956",
"journal-title": "Curr Pharmaceut Des",
"key": "10.1016/j.clnesp.2021.08.019_bib27",
"volume": "15",
"year": "2009"
},
{
"DOI": "10.3389/fimmu.2017.01438",
"article-title": "Lactoferrin in a context of inflammation-induced pathology",
"author": "Kruzel",
"doi-asserted-by": "crossref",
"first-page": "1438",
"journal-title": "Front Immunol",
"key": "10.1016/j.clnesp.2021.08.019_bib28",
"volume": "8",
"year": "2017"
},
{
"DOI": "10.1177/0394632015599832",
"article-title": "CHO expressed recombinant human lactoferrin as an adjuvant for BCG",
"author": "Hwang",
"doi-asserted-by": "crossref",
"first-page": "452",
"journal-title": "Int J Immunopathol Pharmacol",
"key": "10.1016/j.clnesp.2021.08.019_bib29",
"volume": "28",
"year": "2015"
},
{
"DOI": "10.1016/j.jpeds.2016.02.071",
"article-title": "Overview of lactoferrin as a natural immune modulator",
"author": "Legrand",
"doi-asserted-by": "crossref",
"first-page": "S10",
"journal-title": "J Pediatr",
"key": "10.1016/j.clnesp.2021.08.019_bib30",
"volume": "173",
"year": "2016"
},
{
"article-title": "Lactoferrin regulates the release of tumour necrosis factor alpha and interleukin 6 in vivo",
"author": "Machnicki",
"first-page": "433",
"journal-title": "Int J Exp Pathol",
"key": "10.1016/j.clnesp.2021.08.019_bib31",
"volume": "74",
"year": "1993"
},
{
"DOI": "10.1016/j.jiac.2014.08.003",
"article-title": "Lactoferrin for prevention of common viral infections",
"author": "Wakabayashi",
"doi-asserted-by": "crossref",
"first-page": "666",
"journal-title": "J Infect Chemother",
"key": "10.1016/j.clnesp.2021.08.019_bib32",
"volume": "20",
"year": "2014"
},
{
"DOI": "10.1038/aps.2013.200",
"article-title": "Immunomodulatory effects of lactoferrin",
"author": "Siqueiros-Cendón",
"doi-asserted-by": "crossref",
"first-page": "557",
"journal-title": "Acta Pharmacol Sin",
"key": "10.1016/j.clnesp.2021.08.019_bib33",
"volume": "35",
"year": "2014"
},
{
"DOI": "10.1099/jmm.0.46018-0",
"article-title": "Effects of orally administered bovine lactoferrin and lactoperoxidase on influenza virus infection in mice",
"author": "Shin",
"doi-asserted-by": "crossref",
"first-page": "717",
"journal-title": "J Med Microbiol",
"key": "10.1016/j.clnesp.2021.08.019_bib34",
"volume": "54",
"year": "2005"
},
{
"DOI": "10.1139/o11-072",
"article-title": "Bovine lactoferrin: involvement of metal saturation and carbohydrates in the inhibition of influenza virus infection",
"author": "Pietrantoni",
"doi-asserted-by": "crossref",
"first-page": "442",
"journal-title": "Biochem Cell Biol",
"key": "10.1016/j.clnesp.2021.08.019_bib35",
"volume": "90",
"year": "2012"
},
{
"DOI": "10.1179/2047773212Y.0000000004",
"article-title": "Bovine lactoferrin-derived peptides as novel broad-spectrum inhibitors of influenza virus",
"author": "Ammendolia",
"doi-asserted-by": "crossref",
"first-page": "12",
"journal-title": "Pathog Glob Health",
"key": "10.1016/j.clnesp.2021.08.019_bib36",
"volume": "106",
"year": "2012"
}
],
"reference-count": 36,
"references-count": 36,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S2405457721003077"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Nutrition and Dietetics",
"Endocrinology, Diabetes and Metabolism"
],
"subtitle": [],
"title": "Lactoferrin reduces the risk of respiratory tract infections: A meta-analysis of randomized controlled trials",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "45"
}