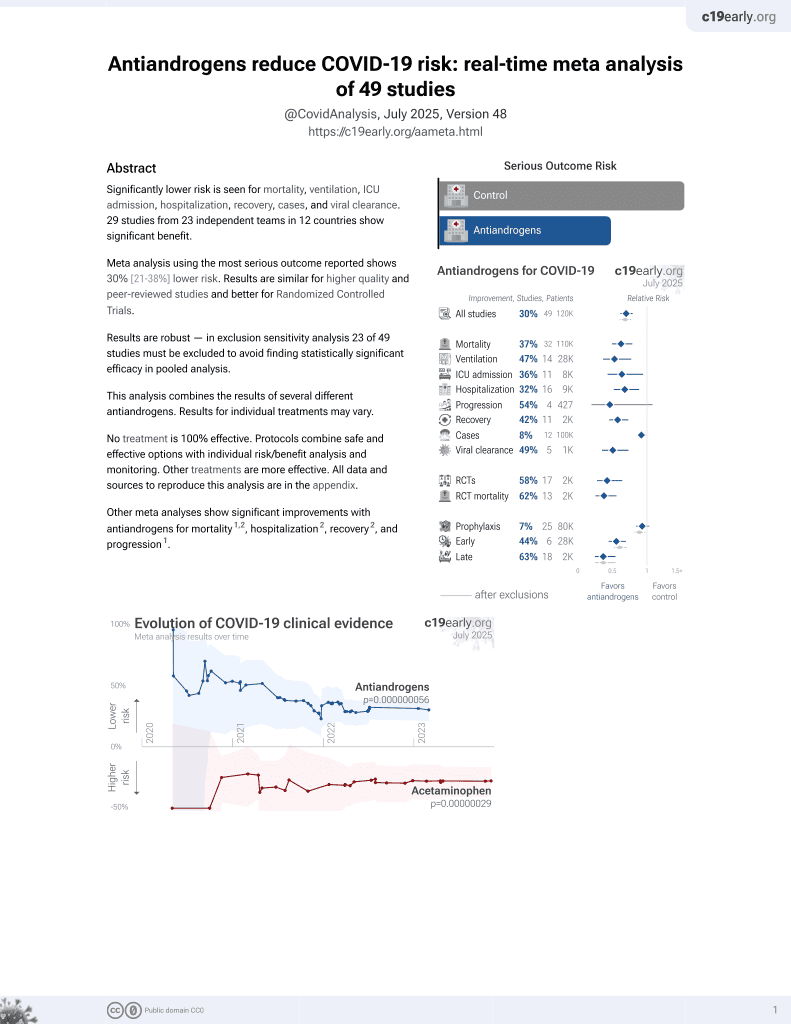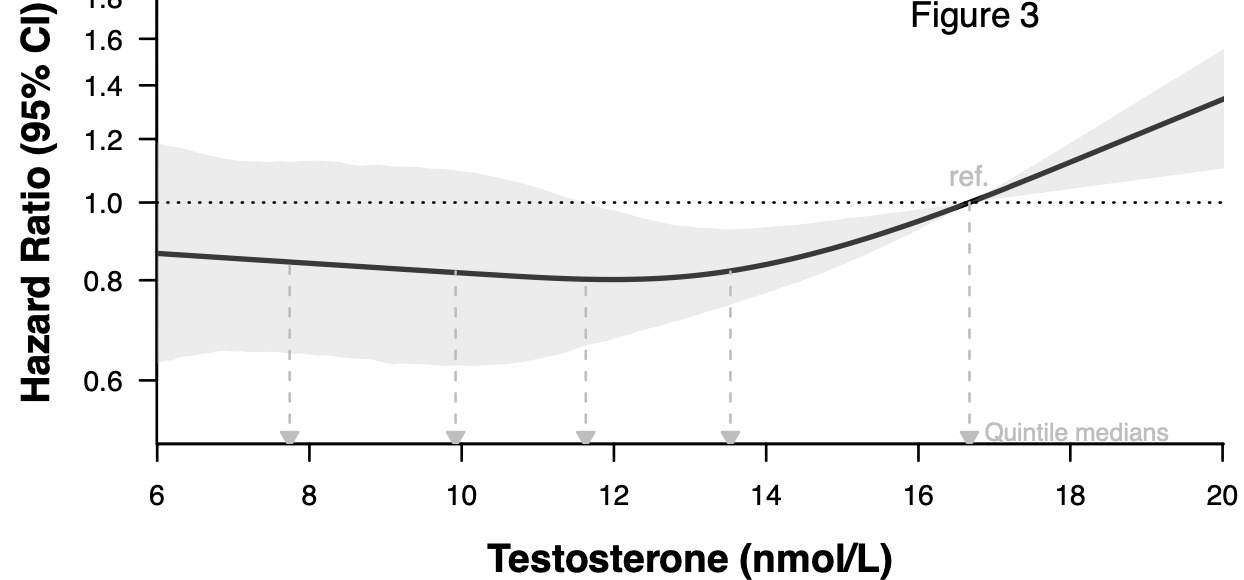
Higher premorbid serum testosterone predicts COVID-19-related mortality risk in men.
et al., European Journal of Endocrinology, doi:10.1530/EJE-22-0104, May 2022
7th treatment shown to reduce risk in
September 2020, now with p = 0.000000056 from 49 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective UK Biobank study showing higher premorbid testosterone levels associated with higher COVID-19 mortality.
Yeap et al., 10 May 2022, prospective, United Kingdom, peer-reviewed, 8 authors, study period 16 March, 2020 - 31 January, 2021.
Contact: bu.yeap@uwa.edu.au, j.nicholson@imperial.ac.uk.
Higher premorbid serum testosterone predicts COVID-19-related mortality risk in men. Authors
Objective Men are at greater risk from COVID-19 than women. Older, overweight men, and those with type 2 diabetes, have lower testosterone concentrations, and poorer COVID-19-related outcomes. We analysed associations of premorbid serum testosterone concentrations, not confounded by effects of acute SARS-CoV-2 infection, with COVID-19-related mortality risk in men.
Design UK Biobank prospective cohort study of community-dwelling men aged 40-69 years.
Methods
Supplemental data Higher premorbid serum testosterone predicts COVID-19-related mortality risk in men. Authors: Bu B. Yeap, Ross J. Marriott, Laurens Manning, Girish Dwivedi, Graeme J. Hankey, Frederick C.W. Wu, Jeremy K. Nicholson, Kevin Murray
Supplemental Methods
Variables of interest
Social, demographic, and lifestyle variables Educational attainment (qualifications) was categorised as below A-levels (high school), completed A-levels, completed college/university, or completed other professional qualification (not school/college/university). Townsend Deprivation Index scores were grouped into quintile categories, with Quintile 5 being the most disadvantaged. 1 Alcohol consumption was categorised using a simplification of categories used by Topiwala et al.: "low" (<14 units/week) including abstainers and men with safe levels of consumption, consistent with UK guidelines; "medium" (14-<30 units/week); "high" ≥30 units/week (1 unit=8 g pure alcohol). 2, 3 Diet categories were high red meat (beef, lamb and pork >3 times/week), low red meat (≤3/week), no red meat, which is a simplification of Bradbury et al. 4 Ethnicity categories were White or Not white (includes Asian, Black, Chinese, Mixed, Other). Vigorous and moderate physical activity undertaken per week was categorised to World Health Organization recommendations as sufficient: ≥75 minutes vigorous or ≥150 minutes moderate, or equivalent combination; insufficient: less..
References
Armstrong, Rudkin, Allen, Crook, Wilson et al., Dynamic linkage of COVID-19 test results between Public Health England's Second Generation Surveillance System and UK Biobank, Microb Genom
Baldassarri, Pichiotti, Fava, Fallerini, Benetti et al., Shorter androgen receptor polyQ alleles protect against life-threatening COVID-19 disease in European males, EBioMedicine
Bohan, Van Ert, Ruggio, Rogers, Badreddine et al., Phosphatidylserine receptors enhance SARS-CoV-2 infection, PLoS Pathog
Bradbury, Tong, Key, Dietary intake of high-protein foods and other major foods in meat-eaters, poultry-eaters, fish-eaters, vegetarians, and vegans in UK Biobank, Nutrients
Bunders, Altfeld, Implications of sex differences in immunity for SARS-CoV-2 pathogenesis and design of therapeutic interventions, Immunity
Cadegiani, Zimerman, Fonseca, Correia, Muller et al., Final results of a randomized, placebocontrolled, two-arm, parallel clinical trial of proxalutamide for hospitalized COVID-19 patients: a multiregional, joint analysis of the Proxa-Rescue AndroCoV Trial, Cureus
Camacho, Huhtaniemi, Neill, Finn, Pye et al., Age-associated changes in hypothalamic-pituitarytesticular function in middle-aged and older men are modified by weight change and lifestyle factors: longitudinal results from the European Male Ageing Study, Eur J Endocrinol
Camici, Zuppi, Lorenzini, Scarnecchia, Pinnetti et al., Group. Role of testosterone in SARS-CoV-2 infection: A key pathogenic factor and a biomarker for severe pneumonia, Int J Infect Dis
Cayan, Uguz, Saylam, Akbay, Effect of serum total testosterone and its relationship with other laboratory parameters on the prognosis of coronavirus disease 2019 (COVID-19) in SARS-CoV-2 infected male patients: a cohort study, Aging Male
Chanana, Palmo, Sharma, Kumar, Graham et al., Sex-derived attributes contributing to SARS-CoV-2 mortality, Am J Physiol Endocrinol Metab
Cinislioglu, Cinislioglu, Demirdogen, Sam, Akkas et al., The relationship of serum testosterone levels with the clinical course and prognosis of COVID-19 disease in male patients: A prospective study, Andrology
Corona, Pizzocaro, Vena, Rastrelli, Semeraro et al., Diabetes is most important cause for mortality in COVID-19 hospitalized patients: Systematic review and meta-analysis, Rev Endocr Metab Dis
Dittadi, Matteucci, Meneghetti, Ndreu, Reassessment of the Access Testosterone chemiluminescence assay and comparison with the LC-MS method, J Clin Lab Anal
Feldman, Longcope, Derby, Johannes, Araujo et al., Age trends in the level of serum testosterone and other hormones in middle-aged men: longitudinal results from the Massachusetts Male Aging Study, J Clin Endocrinol Metab
Fortunato, Martinelli, Caputo, Santantonio, Dattoli et al., Sex and gender differences in COVID-19: an Italian local register-based study, BMJ Open
Fry, Almond, Moffat, Gordon, Singh, UK Biobank Biomarker Project. Companion document to accompany serum biomarker data, Version
Fry, Almond, Moffat, Gordon, Singh, UK Biobank Biomarker Project. Companion document to accompany serum biomarker data, Version
Grambsch, Therneau, Proportional hazards tests and diagnostics based on weighted residuals, Biometrika
Grasselli, Greco, Zanella, Albano, Antonelli et al., Risk factors associated with mortality among patients with COVID-19 in intensive care units in Lombardy, Italy, JAMA Intern Med
Harrell, Regression modelling strategies with applications to linear models, logistic and ordinal regression, and survival analysis
Hastie, Pell, Sattar, Vitamin D and COVID-19 infection and mortality in UK Biobank, Eur J Nutr
Hoffmann, Kleine-Weber, Schroeder, Kruger, Herrier et al., SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor, Cell
Hyde, Flicker, Almeida, Hankey, Mccaul et al., Low free testosterone predicts frailty in older men. The Health in Men Study, J Clin Endocrinol Metab
Kim, Garg, 'halloran, Whitaker, Pham et al., Risk factors for intensive care unit admission and in-hospital mortality among hospitalized adults identified through the US Coronavirus Disease 2019 (COVID-19)-associated hospitalization surveillance network (COVID-NET), Clin Infect Dis
Lanser, Burkert, Thommes, Egger, Hoermann et al., Testosterone deficiency is a risk factor for severe COVID-19, Front Endocrinol
Lenoir, Fuertes, Gomez-Real, Leynaert, Van Der Plaat, Lung function changes over 8 years and testosterone markers in both sexes: UK Biobank, ERJ Open Res
Lin, Smeeth, Langan, Distribution of vitamin D status in the UK: a crosssectional analysis of UK Biobank, BMJ Open
Ly, Sartorius, Hull, Leung, Swerdloff et al., Accuracy of calculated free testosterone formulae in men, Clin Endocrinol
Marriott, Murray, Flicker, Hankey, Matsumoto et al., Lower serum testosterone concentrations are associated with a higher incidence of dementia in men: The UK Biobank prospective cohort study, Alzheimers Dement, doi:10.1002/alz.12529
Mccoy, Goren, Cadegiani, Vano-Galvin, Kovacevic et al., Proxalutamide reduces the rate of hospitalization for COVID-19 male outpatients: a randomized double-blinded placebocontrolled trial, Front Med
Mccoy, Wambier, Herrera, Vano-Galvan, Gioia et al., Androgen receptor genetic variant predicts COVID-19 disease severity: a prospective longitudinal study of hospitalized COVID-19 male patients, J Eur Acad Dermatol Venereol
Mohan, Knuiman, Divitini, James, Musk et al., Higher serum testosterone and dihydrotestosterone, but not oestradiol, are independently associated with favourable indices of lung function in community-dwelling men, Clin Endocrinol
Moody, Mindell, Faulding, Health Survey for England
Moreno-Perez, Merino, Alfayate, Torregrosa, Andres et al., Male pituitary-gonadal axis dysfunction in post-acute COVID-19 syndrome -Prevalence and associated factors: a Mediterranean case series, Clin Endocrinol
Pivonello, Auriemma, Pivonello, Isidori, Corona et al., Sex disparities in COVID-19 severity and outcome: are men weaker or women stronger?, Neuroendocrinology
Qiao, Wang, Mannan, Pitchiaya, Zhang et al., Targeting transcriptional regulation of SARS-CoV-2 entry factors ACE2 and TMPRSS2, Proc Natl Acad Sci
Rastrelli, Stasi, Inglese, Beccaria, Garuti et al., Low testosterone levels predict clinical adverse outcomes in SARS-CoV-2 pneumonia patients, Andrology
Rottoli, Bernante, Belvedere, Balsamo, Garelli et al., How important is obesity as a risk factor for respiratory failure, intensive care admission and death in hospitalised COVID-19 patients? Results from a single Italian centre, Eur J Endocrinol
Salonia, Pontillo, Capogrosso, Gregori, Carenzi et al., Testosterone in males with COVID-19: a 7-month cohort study, Andrology
Samuel, Majd, Richter, Ghazizadeh, Zekevat et al., androgen signalling regulates SARS-CoV-2 receptor levels and is associated with severe COVID-19 symptoms in men, Cell Stem Cell
Simanainen, Brogley, Gao, Jimenez, Harwood et al., Length of the human androgen receptor glutamine tract determines androgen sensitivity in vivo, Mol Cell Endocrinol
Sudlow, Gallacher, Allen, Beral, Burton et al., UK Biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age, PLoS Med
Tenforde, Self, Adams, Gaglani, Ginde et al., Association between mRNA vaccination and COVID-19 hospitalization and disease severity, JAMA
Therneau, Grambsch, Modeling survival data: extending the Cox model
Topiwala, Allan, Valkanova, Moderate alcohol consumption as risk factor for adverse brain outcomes and cognitive decline: longitudinal cohort study, BMJ
Tramunt, Smati, Coudol, Wargny, Pichelin et al., Sex disparities in COVID-19 outcomes of inpatients with diabetes: insights from the CORONADO study, Eur J Endocrinol
Uk Biobank, Biomarker assay quality procedures: approaches used to minimise systematic and random errors (and the wider epidemiological implications), Version
Van Zeggeren, Boelen, Van De Beek, Heijboer, Vlaar et al., Sex steroid hormones are associated with mortality in COVID-19 patients: Level of sex hormones in severe COVID-19, Medicine
Wambier, Goren, Vano-Galvan, Ramos, Ossimetha et al., Androgen sensitivity gateway to COVID-19 disease severity, Drug Develop Res
Wang, Qiu, Hou, Deng, Xu et al., AXL is a candidate receptor for SARS-CoV-2 that promotes infection of pulmonary and bronchial epithelial cells, Cell Res
Welen, Rosendal, Gisslen, Lenman, Freyhult et al., A phase 2 trial of the effect of antiandrogen therapy on COVID-19 outcome: no evidence of benefit, supported by epidemiology and in vitro data, Eur Urol
Williamson, Walker, Bhaskaran, Bacon, Bates et al., OpenSAFELY: factors associated with COVID-19 death in 17 million patients, Nature
Wittert, Bracken, Robledo, Grossmann, Yeap et al., Testosterone treatment to prevent or revert type 2 diabetes in men enrolled in a lifestyle programme (T4DM): a randomised, doubleblind, placebo-controlled, 2-year phase 3b trial, Lancet Diabetes Endocrinol
Wray, Arrowsmith, The physiological mechanisms of the sex-based difference in outcomes of COVID19 infection, Front Physiol
Xu, Wang, Feng, Yu, Chen et al., Effects of SARS-CoV-2 infection on male sex hormones in recovering patients, Andrology
Yeap, Marriott, Antonio, Bhasin, Dobs et al., Sociodemographic, lifestyle and medical influences on serum testosterone and sex hormone-binding globulin in men from UK Biobank, Clin Endocrinol
Yeap, Marriott, Antonio, Chan, Raj et al., Serum testosterone is inversely, and sex hormone-binding globulin directly, associated with all-cause mortality in men, J Clin Endocrinol Metab
Zanetti, Bergman, Burgess, Assimes, Bhalla et al., Urinary albumin, sodium, and potassium and cardiovascular outcomes in the UK Biobank: Observation and Mendelian Randomization analyses, Hypertension
Zarehoseinzade, Allami, Ahmadi, Bijani, Mohammadi, Finasteride in hospitalized adult males with COVID-19: a risk factor for severity of the disease or an adjunct treatment: a randomized controlled clinical trial, Med J Islam Repub Iran
DOI record:
{
"DOI": "10.1530/eje-22-0104",
"ISSN": [
"0804-4643",
"1479-683X"
],
"URL": "http://dx.doi.org/10.1530/EJE-22-0104",
"abstract": "<jats:p><jats:underline>Objective</jats:underline>\n</jats:p>\n<jats:p>Men are at greater risk from COVID-19 than women. Older, overweight men, and those with type 2 diabetes, have lower testosterone concentrations, and poorer COVID-19-related outcomes. We analysed associations of premorbid serum testosterone concentrations, not confounded by effects of acute SARS-CoV-2 infection, with COVID-19-related mortality risk in men.\n</jats:p>\n<jats:p><jats:underline>Design</jats:underline>\n</jats:p>\n<jats:p>UK Biobank prospective cohort study of community-dwelling men aged 40-69 years.\n</jats:p>\n<jats:p><jats:underline>Methods</jats:underline>\n</jats:p>\n<jats:p>Serum total testosterone and sex hormone-binding globulin (SHBG) were measured at baseline (2006-2010). Free testosterone values were calculated (cFT). Incidence of SARS-CoV-2 infections and deaths related to COVID-19 were ascertained from 16 March 2020-31 January 2021, and modelled using time-stratified Cox regression.\n</jats:p>\n<jats:p><jats:underline>Results</jats:underline>\n</jats:p>\n<jats:p>In 159,964 men there were 5,558 SARS-CoV-2 infections and 438 COVID-19 deaths. Younger age, higher body mass index, non-white ethnicity, lower educational attainment, and socio-economic deprivation were associated with incidence of SARS-CoV-2 infections, but total testosterone, SHBG, and cFT were not. Adjusting for potential confounders, higher total testosterone was associated with COVID-19-related mortality risk (overall trend P=0.008; hazard ratios, HR [95% confidence intervals] quintile 1, Q1 vs Q5 [reference]: 0.84 [0.65-1.12], Q2:Q5 0.82 [0.63-1.10], Q3:Q5 0.80 [0.66-1.00], Q4:Q5 0.82 [0.75-0.93]). Higher SHBG was also associated with COVID-19 mortality risk (P=0.008), but cFT was not (P=0.248).\n</jats:p>\n<jats:p><jats:underline>Conclusions</jats:underline>\n</jats:p>\n<jats:p>Middle-aged to older men with the highest premorbid serum total testosterone and SHBG concentrations are at greater risk of COVID-19-related mortality. Men could be advised that having relatively high serum testosterone concentrations does not protect against future COVID-19-related mortality. Further investigation of causality and potential underlying mechanisms is warranted.</jats:p>",
"author": [
{
"affiliation": [
{
"name": "B Yeap, Medical School, The University of Western Australia, Perth, Australia"
}
],
"family": "Yeap",
"given": "Bu B",
"sequence": "first"
},
{
"affiliation": [
{
"name": "R Marriott, School of Population and Global Health, The University of Western Australia, Perth, Australia"
}
],
"family": "Marriott",
"given": "Ross J",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "L Manning, Medical School, The University of Western Australia, Perth, Australia"
}
],
"family": "Manning",
"given": "Laurens",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "G Dwivedi, Medical School, The University of Western Australia, Perth, Australia"
}
],
"family": "Dwivedi",
"given": "Girish",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "G Hankey, Medical School, The University of Western Australia, Perth, Australia"
}
],
"family": "Hankey",
"given": "Graeme J",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "F Wu, Andrology Research Unit, The University of Manchester, Manchester, United Kingdom of Great Britain and Northern Ireland"
}
],
"family": "Wu",
"given": "Frederick C. W.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "J Nicholson, Medical School, The University of Western Australia, Perth, Australia"
}
],
"family": "Nicholson",
"given": "Jeremy K",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "K Murray, School of Population and Global Health, The University of Western Australia, Perth, Australia"
}
],
"family": "Murray",
"given": "Kevin",
"sequence": "additional"
}
],
"container-title": "European Journal of Endocrinology",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"eje.bioscientifica.com"
]
},
"created": {
"date-parts": [
[
2022,
5,
10
]
],
"date-time": "2022-05-10T17:56:28Z",
"timestamp": 1652205388000
},
"deposited": {
"date-parts": [
[
2022,
5,
10
]
],
"date-time": "2022-05-10T17:57:17Z",
"timestamp": 1652205437000
},
"indexed": {
"date-parts": [
[
2022,
5,
10
]
],
"date-time": "2022-05-10T18:11:35Z",
"timestamp": 1652206295557
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2022,
5
]
]
},
"license": [
{
"URL": "http://creativecommons.org/licenses/by/4.0/deed.en_GB",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
5,
1
]
],
"date-time": "2022-05-01T00:00:00Z",
"timestamp": 1651363200000
}
}
],
"link": [
{
"URL": "https://eje.bioscientifica.com/view/journals/eje/aop/eje-22-0104/eje-22-0104.xml",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://eje.bioscientifica.com/downloadpdf/journals/eje/aop/eje-22-0104/eje-22-0104.xml",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "416",
"original-title": [],
"prefix": "10.1530",
"published": {
"date-parts": [
[
2022,
5
]
]
},
"published-print": {
"date-parts": [
[
2022,
5
]
]
},
"publisher": "Bioscientifica",
"reference-count": 0,
"references-count": 0,
"relation": {},
"resource": {
"primary": {
"URL": "https://eje.bioscientifica.com/view/journals/eje/aop/eje-22-0104/eje-22-0104.xml"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Endocrinology",
"General Medicine",
"Endocrinology, Diabetes and Metabolism"
],
"subtitle": [],
"title": "Higher premorbid serum testosterone predicts COVID-19-related mortality risk in men.",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1530/crossmarkpolicy-7"
}
