Zinc reduces COVID-19 risk: real-time meta-analysis of 42 studies (Version 74)
, Mar 2026
Zinc for COVID-19
2nd treatment shown to reduce risk in
July 2020, now with p = 0.00000019 from 42 studies, recognized in 23 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,400+ studies for
210+ treatments. c19early.org
|
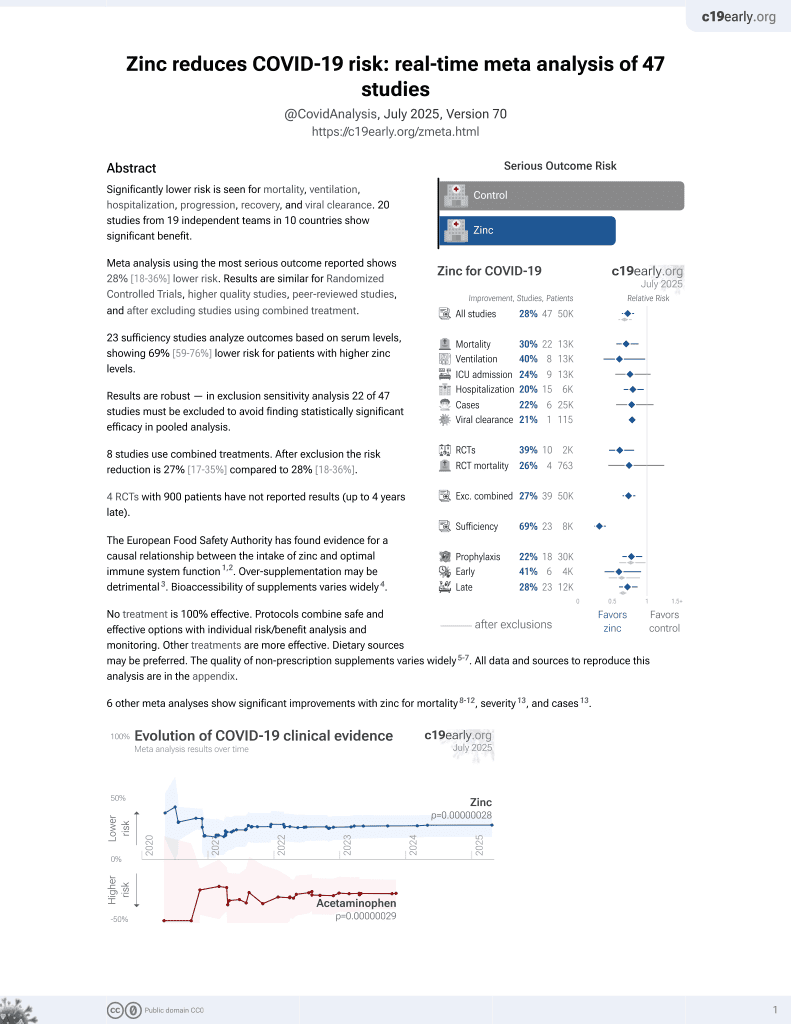
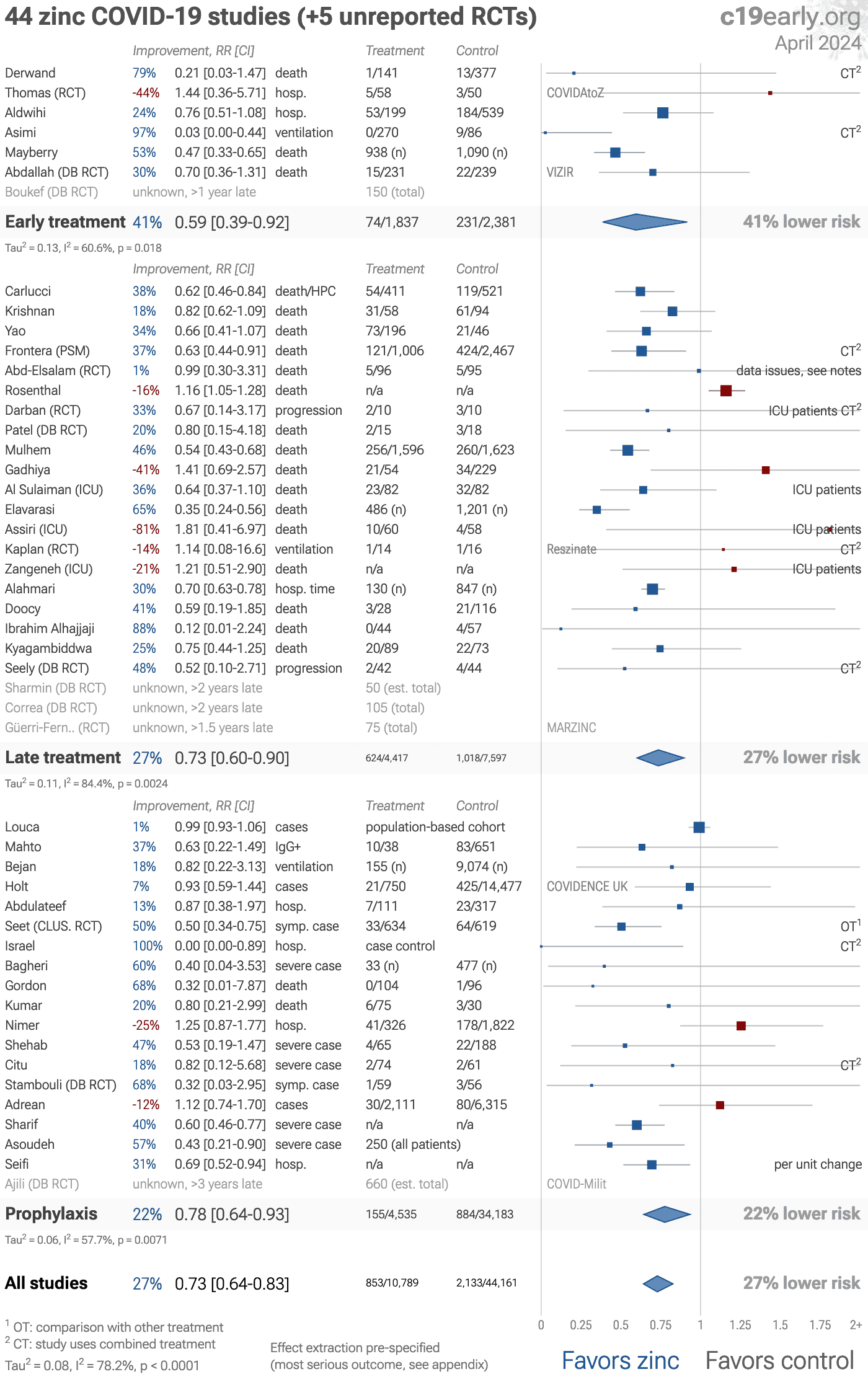
Significantly lower risk is seen for mortality, hospitalization, progression, recovery, and viral clearance. 20 studies from 19 independent teams in 10 countries show significant benefit.
Meta-analysis using the most serious outcome reported shows 29% [19‑37%] lower risk. Results are similar for Randomized Controlled Trials, higher quality studies, peer-reviewed studies, and after excluding studies using combined treatment.
24 sufficiency studies analyze outcomes based on serum levels, showing 69% [60‑76%] lower risk for patients with higher zinc levels.
Results are very robust—in worst case exclusion sensitivity analysis 22 of 42 studies must be excluded before statistical significance is lost. Emergent results matching biological mechanisms confirm efficacy: meta-regression of efficacy vs. treatment delay (p = 0.032) and efficacy gradient across outcomes (p = 0.028).
Control Zinc
6 studies use combined treatments. After exclusion the risk reduction is 28% [18‑36%] compared to 29% [19‑37%].
4 RCTs with 900 patients have not reported results (up to 5 years late).
The European Food Safety Authority has found evidence for a causal relationship between the intake of zinc and optimal immune system function1,2. Over-supplementation may be detrimental3. Bioaccessibility of supplements varies widely4. Dietary sources may be preferred, where other food-matrix components have been shown to enhance absorption. For non-diet sources, zinc picolinate may be the best form, with the highest and most diet-independent bioaccessibility5.
No treatment is 100% effective. Protocols combine safe and effective options with individual risk/benefit analysis and monitoring. Other treatments are more effective. Dietary sources may be preferred. The quality of non-prescription supplements varies widely6-8. All data and sources to reproduce this analysis are in the appendix.
7 other meta-analyses show significant improvements with zinc for mortality9-14, severity15, and cases15.
1.
Tabatabaeizadeh, S., Zinc supplementation and COVID-19 mortality: a meta-analysis, European Journal of Medical Research, doi:10.1186/s40001-022-00694-z.
2.
Olczak-Pruc et al., The effect of zinc supplementation on the course of COVID-19 – A systematic review and meta-analysis, Annals of Agricultural and Environmental Medicine, doi:10.26444/aaem/155846.
3.
Xie et al., Micronutrient perspective on COVID-19: Umbrella review and reanalysis of meta-analyses, Critical Reviews in Food Science and Nutrition, doi:10.1080/10408398.2023.2174948.
4.
Abuhelwa, Z., Do Zinc Supplements Reduce Mortality in Patients with COVID-19?, Translation: The University of Toledo Journal of Medical Sciences, doi:10.46570/utjms.vol11-2023-749.
5.
Rheingold et al., Zinc Supplementation Associated With a Decrease in Mortality in COVID-19 Patients: A Meta-Analysis, Cureus, doi:10.7759/cureus.40231.
Covid Analysis et al., Mar 2026, preprint, 1 author.
